Abstract
Background
Anastomotic surgical recurrence after bowel resection in Crohn’s disease patients is problematic. This study was performed to evaluate the increased risk of anastomotic surgical recurrence.
Methods
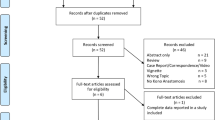
From 2006 to 2016, we performed anastomoses in 215 consecutive Crohn’s disease patients. The cohort was divided into two groups: Kono-S anastomosis (n = 117) and end-to-end anastomosis (n = 98). Multivariate analysis of predictors of anastomotic surgical recurrence and Kaplan–Meier analysis for the 5-year anastomotic surgical recurrence rate were evaluated.
Results
The two groups showed no statistically significant differences in patient backgrounds. During a median follow-up of 54 months, 28 patients required anastomotic surgical recurrence [4 (3.4%) in the Kono-S group and 24 (24.4%) in the end-to-end group]. Six leaks (5.1%) were detected in the Kono-S group and 17 leaks (17.3%) in the end-to-end group; all were successfully treated conservatively. End-to-end anastomosis, leakage, age < 45 years, and body mass index of ≥ 18 kg/m2 at the first surgery had a higher risk of anastomotic surgical recurrence. Kono-S anastomosis significantly reduced the risk of anastomotic surgical recurrence after 1 year (odds ratio, 0.14). Anastomotic leakage influenced anastomotic surgical recurrence within 1 year (odds ratio, 4.84). The 5-year surgery-free survival rate at the anastomosis site with Kono-S anastomosis (95.0%) was significantly higher than that with end-to-end anastomosis (81.3%; P < 0.001).
Conclusions
Anastomotic leakage after bowel resection in Crohn’s disease patients increased anastomotic surgical recurrence within 1 year, and Kono-S anastomosis is associated with a low risk of anastomotic surgical recurrence after > 1 year.



Similar content being viewed by others
References
Bernell O, Lapidus A, Hellers G. Risk factors for surgery and postoperative recurrence in Crohn’s disease. Annals of surgery. 2000;231(1):38–45.
Lewis RT, Maron DJ. Efficacy and complications of surgery for Crohn’s disease. Gastroenterology & hepatology. 2010;6(9):587–96.
Michelassi F. Crohn’s recurrence after intestinal resection and anastomosis. Digestive diseases and sciences. 2014;59(7):1352–3. https://doi.org/10.1007/s10620-014-3096-4.
Olaison G, Smedh K, Sjodahl R. Natural course of Crohn’s disease after ileocolic resection: endoscopically visualised ileal ulcers preceding symptoms. Gut. 1992;33(3):331–5.
Peyrin-Biroulet L, Harmsen WS, Tremaine WJ, Zinsmeister AR, Sandborn WJ, Loftus EV, Jr. Surgery in a population-based cohort of Crohn’s disease from Olmsted County, Minnesota (1970-2004). Am J Gastroenterol. 2012;107(11):1693–701. https://doi.org/10.1038/ajg.2012.298.
Cho SM, Cho SW, Regueiro M. Postoperative management of crohn disease. Gastroenterol Clin North Am. 2009;38(4):753–62.
Peyrin-Biroulet L, Loftus EV, Jr., Colombel JF, Sandborn WJ. The natural history of adult Crohn’s disease in population-based cohorts. The American journal of gastroenterology. 2010;105(2):289–97. https://doi.org/10.1038/ajg.2009.579.
He X, Chen Z, Huang J, Lian L, Rouniyar S, Wu X et al. Stapled side-to-side anastomosis might be better than handsewn end-to-end anastomosis in ileocolic resection for Crohn’s disease: a meta-analysis. Digestive diseases and sciences. 2014;59(7):1544–51. https://doi.org/10.1007/s10620-014-3039-0.
McLeod RS, Wolff BG, Ross S, Parkes R, McKenzie M. Recurrence of Crohn’s disease after ileocolic resection is not affected by anastomotic type: results of a multicenter, randomized, controlled trial. Dis Colon Rectum. 2009;52(5):919–27.
Kono T, Ashida T, Ebisawa Y, Chisato N, Okamoto K, Katsuno H et al. A new antimesenteric functional end-to-end handsewn anastomosis: surgical prevention of anastomotic recurrence in Crohn’s disease. Dis Colon Rectum. 2011;54(5):586–92. https://doi.org/10.1007/DCR.0b013e318208b90f.
Kono T, Fichera A, Maeda K, Sakai Y, Ohge H, Krane M et al. Kono-S Anastomosis for Surgical Prophylaxis of Anastomotic Recurrence in Crohn’s Disease: an International Multicenter Study. Journal of gastrointestinal surgery : official journal of the Society for Surgery of the Alimentary Tract. 2016;20(4):783–90. https://doi.org/10.1007/s11605-015-3061-3.
Fichera A, Zoccali M, Kono T. Antimesenteric functional end-to-end handsewn (Kono-S) anastomosis. Journal of gastrointestinal surgery : official journal of the Society for Surgery of the Alimentary Tract. 2012;16(7):1412–6. https://doi.org/10.1007/s11605-012-1905-7.
Katsuno H, Maeda K, Hanai T, Masumori K, Koide Y, Kono T. Novel antimesenteric functional end-to-end handsewn (Kono-S) anastomoses for Crohn’s disease: a report of surgical procedure and short-term outcomes. Digestive surgery. 2015;32(1):39–44. https://doi.org/10.1159/000371857.
Luglio G, Rispo A, Castiglione F, Imperatore N, Giglio MC, De Palma GD et al. Kono-type anastomosis in a patient with severe multi-recurrent Crohn’s disease. Int J Colorectal Dis. 2016;31(8):1565–6. https://doi.org/10.1007/s00384-016-2567-9.
Fornaro R, Caratto E, Caratto M, Fornaro F, Caristo G, Frascio M et al. Post-operative recurrence in Crohn’s disease. Critical analysis of potential risk factors. An update. The surgeon : journal of the Royal Colleges of Surgeons of Edinburgh and Ireland. 2015;13(6):330–47. https://doi.org/10.1016/j.surge.2015.04.002.
De Cruz P, Kamm MA, Prideaux L, Allen PB, Desmond PV. Postoperative recurrent luminal Crohn’s disease: a systematic review. Inflammatory bowel diseases. 2012;18(4):758–77. https://doi.org/10.1002/ibd.21825.
de Barcelos IF, Kotze PG, Spinelli A, Suzuki Y, Teixeira FV, de Albuquerque IC et al. Factors affecting the incidence of early endoscopic recurrence after ileocolonic resection for Crohn’s disease: a multicentre observational study. Colorectal disease : the official journal of the Association of Coloproctology of Great Britain and Ireland. 2017;19(1):O39-O45. https://doi.org/10.1111/codi.13581.
Iesalnieks I, Kilger A, Glass H, Muller-Wille R, Klebl F, Ott C et al. Intraabdominal septic complications following bowel resection for Crohn’s disease: detrimental influence on long-term outcome. International journal of colorectal disease. 2008;23(12):1167–74. https://doi.org/10.1007/s00384-008-0534-9.
Resegotti A, Astegiano M, Farina EC, Ciccone G, Avagnina G, Giustetto A et al. Side-to-side stapled anastomosis strongly reduces anastomotic leak rates in Crohn’s disease surgery. Dis Colon Rectum. 2005;48(3):464–8. https://doi.org/10.1007/s10350-004-0786-6.
Widmar M, Cummings DR, Steinhagen E, Samson A, Barth AR, Greenstein AJ et al. Oversewing staple lines to prevent anastomotic complications in primary ileocolic resections for Crohn’s disease. J Gastrointest Surg. 2015;19(5):911–6. https://doi.org/10.1007/s11605-015-2792-5.
Kusunoki M, Ikeuchi H, Yanagi H, Shoji Y, Yamamura T. A comparison of stapled and hand-sewn anastomoses in Crohn’s disease. Digestive surgery. 1998;15(6):679–82.
Smedh K, Andersson M, Johansson H, Hagberg T. Preoperative management is more important than choice of sutured or stapled anastomosis in Crohn’s disease. The European journal of surgery = Acta chirurgica. 2002;168(3):154–7. https://doi.org/10.1080/110241502320127766.
Yamamoto T, Allan RN, Keighley MR. Risk factors for intra-abdominal sepsis after surgery in Crohn’s disease. Dis Colon Rectum. 2000;43(8):1141–5.
D’Haens GR, Geboes K, Peeters M, Baert F, Penninckx F, Rutgeerts P. Early lesions of recurrent Crohn’s disease caused by infusion of intestinal contents in excluded ileum. Gastroenterology. 1998;114(2):262–7.
de Buck van Overstraeten A, Vermeire S, Vanbeckevoort D, Rimola J, Ferrante M, Van Assche G et al. Modified Side-To-Side Isoperistaltic Strictureplasty over the Ileocaecal Valve: An Alternative to Ileocaecal Resection in Extensive Terminal Ileal Crohn’s Disease. Journal of Crohn’s & colitis. 2016;10(4):437–42. https://doi.org/10.1093/ecco-jcc/jjv230.
Blonski W, Buchner AM, Lichtenstein GR. Clinical predictors of aggressive/disabling disease: ulcerative colitis and crohn disease. Gastroenterol Clin North Am. 2012;41(2):443–62. https://doi.org/10.1016/j.gtc.2012.01.008.
Gklavas A, Dellaportas D, Papaconstantinou I. Risk factors for postoperative recurrence of Crohn’s disease with emphasis on surgical predictors. Annals of gastroenterology. 2017;30(6):598–612. https://doi.org/10.20524/aog.2017.0195.
De Cruz P, Kamm MA, Hamilton AL, Ritchie KJ, Krejany EO, Gorelik A et al. Crohn’s disease management after intestinal resection: a randomised trial. Lancet (London, England). 2015;385(9976):1406–17. https://doi.org/10.1016/s0140-6736(14)61908-5.
Reese GE, Nanidis T, Borysiewicz C, Yamamoto T, Orchard T, Tekkis PP. The effect of smoking after surgery for Crohn’s disease: a meta-analysis of observational studies. Int J Colorectal Dis. 2008;23(12):1213–21. https://doi.org/10.1007/s00384-008-0542-9.
Manser CN, Frei P, Grandinetti T, Biedermann L, Mwinyi J, Vavricka SR et al. Risk factors for repetitive ileocolic resection in patients with Crohn’s disease: results of an observational cohort study. Inflammatory bowel diseases. 2014;20(9):1548–54. https://doi.org/10.1097/MIB.0000000000000123.
Author information
Authors and Affiliations
Contributions
Study conception: Norimitsu Shimada, Hiroki Ohge, Toru Kono, Taijiro Sueda
Study design: Norimitsu Shimada, Hiroki Ohge, Toru Kono
Data acquisition: Norimitsu Shimada, Raita Yano, Yusuke Watadani
Quality control of data and algorithms: Yusuke Watadani, Kenichiro Uemura, Yoshiaki Murakami
Data analysis and interpretation: Norimitsu Shimada, Ayumu Sugitani, Raita Yano
Statistical analysis: Ayumu Sugitani
Manuscript preparation: Norimitsu Shimada
Manuscript editing: Hiroki Ohge, Yoshiaki Murakami, Kenichiro Uemura
Manuscript review: Toru Kono, Taijiro Sueda
Corresponding author
Ethics declarations
Conflict of Interest
The authors declare that they have no conflicts of interest
Additional information
Conference presentation: This study was presented as a poster at the 2017 meeting of The American Society of Colon and Rectal Surgeons in Seattle, Washington (10–14 June 2017).
Rights and permissions
About this article
Cite this article
Shimada, N., Ohge, H., Kono, T. et al. Surgical Recurrence at Anastomotic Site After Bowel Resection in Crohn’s Disease: Comparison of Kono-S and End-to-end Anastomosis. J Gastrointest Surg 23, 312–319 (2019). https://doi.org/10.1007/s11605-018-4012-6
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s11605-018-4012-6