Abstract
Purpose
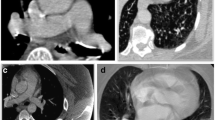
The purpose of this study was to investigate the prevalence of incidental pulmonary embolism (IPE) in suspected stroke patients receiving carotid computed tomography angiography (CTA) and its characteristics.
Materials and methods
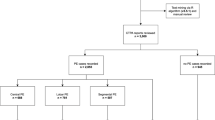
A total of 4873 cases receiving carotid CTA between January 2013 and December 2016 were retrospectively reassessed by one radiologist. Patients with previous or suspected PE were excluded. The remaining prior contrast-enhanced carotid CTA studies were regarded as a “potentially incidental” IPE when a filling defect was found in one or more pulmonary arteries and subjected to the other two thoracic radiologists independently for reviewing and assessing for characteristics of the IPE and the image quality of the PE. The differences were noted between inpatients and outpatients in prevalence of IPE. Characteristics of the patients with IPE were also studied in terms of gender, age, as well as clinical indication.
Results
The prevalence of IPE among these suspected stroke patients was 0.8% on carotid CT angiography, and 24 (96%) of all IPEs had not been previously diagnosed by the original reporting radiologists. Most of the IPEs were at the lobar or segmental levels, single and in right upper lobe of pulmonary arteries. In most of the cases, the reviewing radiologists judged the contrast bolus as good. The outpatient group had a lower percentage of patients with IPE when compared with the inpatient counterpart (p = 0.024). The prevalence of IPE in patients with suspected stroke was higher with the increasing of age (p = 0.013).
Conclusions
IPE can occur in suspected stroke patients on carotid CT angiography, and most of them have been previously neglected in clinical practice. Radiologists should check the higher pulmonary arterial vasculature carefully on the contrast-enhanced carotid CTA scans.



Similar content being viewed by others
References
Amato B, Compagna R, Rocca A et al (2016) Fondaparinux vs warfarin for the treatment of unsuspected pulmonary embolism in cancer patients. Drug Des Dev Ther 10:2041–2046
Cheuk BL, Cheung GC, Cheng SW (2004) Epidemiology of venous thromboembolism in a Chinese population. Br J Surg 91:424–428
Choi WI, Jo JY, Kwon YS et al (2012) Incidence of pulmonary embolism among hospitalized patients. Thromb Res 129:523–525
Cohen AT, Dobromirski M, Gurwith MM (2014) Managing pulmonary embolism from presentation to extended treatment. Thromb Res 133:139–148
Den Exter PL, Kroft LJ, Van Der Hulle T et al (2013) Embolic burden of incidental pulmonary embolism diagnosed on routinely performed contrast-enhanced computed tomography imaging in cancer patients. J Thromb Haemost 11:1620–1622
Deniz MA, Deniz ZT, Adin ME et al (2017) Detection of incidental pulmonary embolism with multi-slice computed tomography in cancer patients. Clin Imaging 41:106–111
Dentali F, Ageno W, Becattini C et al (2010) Prevalence and clinical history of incidental, asymptomatic pulmonary embolism: a meta-analysis. Thromb Res 125:518–522
Easton JD, Saver JL, Albers GW et al (2009) Definition and evaluation of transient ischemic attack. Stroke 40:2276–2293
Epstein NE, Staszewski H, Garrison M et al (2011) Pulmonary embolism diagnosed on computed tomography contrast angiography despite negative venous Doppler ultrasound after spinal surgery. J Spinal Disord Tech 24:358–362
Garcia-Fuster MJ, Fabia MJ, Furio E et al (2014) Should we look for silent pulmonary embolism in patients with deep venous thrombosis? BMC Cardiovasc Disord 14:178
Heit JA, Cohen AT, Anderson FA (2005) Estimated annual number of incident and recurrent, non-fatal and fatal venous thromboembolism (VTE) events in the US. Blood 106:910
Hughes MJ, Stein PD, Matta F (2014) Silent pulmonary embolism in patients with distal deep venous thrombosis: systematic review. Thromb Res 134:1182–1185
Keller K, Beule J, Coldewey M et al (2014) Effect of age on pulmonary embolism. Phlebologie 43:69–76
Khorana AA, O’connell C, Agnelli G et al (2012) Incidental venous thromboembolism in oncology patients. J Thromb Haemost 10:2602–2604
Kligerman SJ, Lahiji K, Galvin JR et al (2014) Missed pulmonary emboli on CT angiography: assessment with pulmonary embolism-computer-aided detection. AJR Am J Roentgenol 202:65–73
Li F, Wang X, Huang W et al (2014) Risk factors associated with the occurrence of silent pulmonary embolism in patients with deep venous thrombosis of the lower limb. Phlebology 29:442–446
Lim KY, Kligerman SJ, Lin CT et al (2014) Missed pulmonary embolism on abdominal CT. AJR Am J Roentgenol 202:738–743
O’connell C (2015) How I treat incidental pulmonary embolism. Blood 125:1877–1882 quiz 2009
Palacio D, Benveniste MF, Betancourt-Cuellar SL et al (2015) Multidetector computed tomography pulmonary angiography pitfalls in the evaluation of pulmonary embolism with emphasis in technique. Semin Roentgenol 50:217–225
Pongmoragot J, Rabinstein AA, Nilanont Y et al (2013) Pulmonary embolism in ischemic stroke: clinical presentation, risk factors, and outcome. J Am Heart Assoc 2:e000372
Refaat R, El-Shinnawy MA (2013) Does the anatomic distribution of acute pulmonary emboli at MDCT pulmonary angiography in oncology-population differ from that in non-oncology counterpart? Egypt J Radiol Nucl Med 44:463–474
Ritchie G, Mcgurk S, Mccreath C et al (2007) Prospective evaluation of unsuspected pulmonary embolism on contrast enhanced multidetector CT (MDCT) scanning. Thorax 62:536–540
Sahut D’izarn M, Caumont Prim A, Planquette B et al (2012) Risk factors and clinical outcome of unsuspected pulmonary embolism in cancer patients: a case-control study. J Thromb Haemost 10:2032–2038
Shteinberg M, Segal-Trabelsy M, Adir Y et al (2012) Clinical characteristics and outcomes of patients with clinically unsuspected pulmonary embolism versus patients with clinically suspected pulmonary embolism. Respiration 84:492–500
Stein PD, Matta F, Musani MH et al (2010) Silent pulmonary embolism in patients with deep venous thrombosis: a systematic review. Am J Med 123:426–431
Storto ML, Di Credico A, Guido F et al (2005) Incidental detection of pulmonary emboli on routine MDCT of the chest. AJR Am J Roentgenol 184:264–267
Tanislav C, Puille M, Pabst W et al (2011) High frequency of silent pulmonary embolism in patients with cryptogenic stroke and patent foramen ovale. Stroke 42:822–824
Torbicki A, Perrier A, Konstantinides S et al (2008) Guidelines on the diagnosis and management of acute pulmonary embolism: the task force for the diagnosis and management of acute pulmonary embolism of the European Society of Cardiology (ESC). Eur Heart J 29:2276–2315
Wargo JJ, Berg A, Gudjonsson JE (2016) Ongoing Pleuritic Chest Pain and a Guinea Pig: missed Pulmonary Embolism and Majocchi’s Granuloma. Am J Med 129:e165–e167
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflict of interest
The authors declare no conflict of interest.
Ethical standards
This article does not contain any studies with human participants or animals performed by any of the authors.
Rights and permissions
About this article
Cite this article
Chen, GL., Shen, DH., Wei, J. et al. Incidental pulmonary embolism in suspected stroke patients undergoing carotid CT angiography. Radiol med 123, 399–405 (2018). https://doi.org/10.1007/s11547-018-0860-0
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s11547-018-0860-0