Abstract
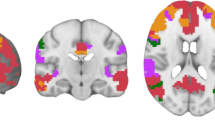
Mild cognitive impairment (MCI) is common in patients with Parkinson’s disease (PD), yet the underlying neural mechanisms of this disease state remain unclear. We investigated alterations in the spontaneous brain activity of PD patients with MCI (PD-MCI) relative to cognitively normal PD patients (PD-CN) and healthy control (HC) subjects. In this work, 13 PD-MCI patients, 16 PD-CN patients, and 16 HC subjects completed resting state functional MRI. Spontaneous brain activity was measured by calculating amplitude of low frequency fluctuation (ALFF) values across the whole brain. Between-group differences and correlations between ALFF values and cognitive test scores were analyzed. ALFF values decreased in the right superior temporal gyrus and increased in the left middle temporal gyrus and left superior frontal gyrus of PD-MCI patients compared with PD-CN patients. In the PD-MCI group, ALFF values in the left middle temporal gyrus were negatively correlated with Montreal Cognitive Assessment and vocabulary test scores, and the ALFF values in the left superior frontal gyrus were negatively correlated with vocabulary test scores. Our study demonstrates that PD-MCI is associated with abnormal spontaneous brain activity in the temporal and frontal lobes. These findings inform the underlying neural mechanism of cognitive impairment in PD.



Similar content being viewed by others
References
Svenningsson P, Westman E, Ballard C et al (2012) Cognitive impairment in patients with Parkinson’s disease: diagnosis, biomarkers, and treatment. Lancet Neurol 11:697–707
Yarnall AJ, Breen DP, Duncan GW et al (2014) Characterizing mild cognitive impairment in incident Parkinson disease: the ICICLE-PD study. Neurology 82:308–316
Aarsland D, Bronnick K, Williams-Gray C et al (2010) Mild cognitive impairment in Parkinson disease: a multicenter pooled analysis. Neurology 75:1062–1069
Pedersen KF, Larsen JP, Tysnes OB et al (2013) Prognosis of mild cognitive impairment in early Parkinson disease: the Norwegian ParkWest study. JAMA Neurol 70:580–586
Melzer TR, Watts R, MacAskill MR et al (2014) Grey matter atrophy in cognitively impaired Parkinson’s disease. J Neurol Neurosurg Psychiatry 83:188–194
Song SK, Lee JE, Park HJ et al (2011) The pattern of cortical atrophy in patients with Parkinson’s disease according to cognitive status. Mov Disord 26:289–296
Mak E, Bergsland N, Dwyer MG et al (2014) Subcortical atrophy is associated with cognitive impairment in mild Parkinson disease: a combined investigation of volumetric changes, cortical thickness, and vertex-based shape analysis. AJNR Am J Neuroradiol 35:2257–2264
Weintraub D, Doshi J, Koka D et al (2011) Neurodegeneration across stages of cognitive decline in Parkinson disease. Arch Neurol 68:1562–1568
Hattori T, Orimo S, Aoki S et al (2012) Cognitive status correlates with white matter alteration in Parkinson’s disease. Hum Brain Mapp 33:727–739
Mak E, Dwyer MG, Ramasamy DP et al (2015) White matter hyperintensities and mild cognitive impairment in Parkinson’s disease. J Neuroimaging 25:754–760
Compta Y, Pereira JB, Rios J et al (2013) Combined dementia-risk biomarkers in Parkinson’s disease: a prospective longitudinal study. Parkinsonism Relat Disord 19:717–724
Ekman U, Eriksson J, Forsgren L et al (2014) Longitudinal changes in task-evoked brain responses in Parkinson’s disease patients with and without mild cognitive impairment. Front Neurosci 8:207
Fox MD, Raichle ME (2007) Spontaneous fluctuations in brain activity observed with functional magnetic resonance imaging. Nat Rev Neurosci 8:700–711
Zang YF, He Y, Zhu CZ et al (2007) Altered baseline brain activity in children with ADHD revealed by resting-state functional MRI. Brain Dev 29:83–91
Hou Y, Wu X, Hallett M et al (2014) Frequency-dependent neural activity in Parkinson’s disease. Hum Brain Mapp 35:5815–5833
Hu X, Song X, Li E et al (2015) Altered resting-state brain activity and connectivity in depressed Parkinson’s disease. PLoS ONE 10:e131133
Kwak Y, Peltier SJ, Bohnen NI et al (2012) L-DOPA changes spontaneous low-frequency BOLD signal oscillations in Parkinson’s disease: a resting state fMRI study. Front Syst Neurosci 6:52
Skidmore FM, Yang M, Baxter L et al (2013) Reliability analysis of the resting state can sensitively and specifically identify the presence of Parkinson disease. Neuroimage 75:249–261
Hughes AJ, Daniel SE, Kilford L et al (1992) Accuracy of clinical diagnosis of idiopathic Parkinson’s disease: a clinico-pathological study of 100 cases. J Neurol Neurosurg Psychiatry 55:181–184
Litvan I, Goldman JG, Troster AI et al (2012) Diagnostic criteria for mild cognitive impairment in Parkinson’s disease: Movement Disorder Society Task Force guidelines. Mov Disord 27:349–356
Song XW, Dong ZY, Long XY et al (2011) REST: a toolkit for resting-state functional magnetic resonance imaging data processing. PLoS ONE 6:e25031
Rektorova I, Biundo R, Marecek R et al (2014) Grey matter changes in cognitively impaired Parkinson’s disease patients. PLoS ONE 9:e85595
Pereira JB, Junque C, Marti MJ et al (2009) Structural brain correlates of verbal fluency in Parkinson’s disease. NeuroReport 20:741–744
Tang Y, Ge J, Liu F et al (2016) Cerebral metabolic differences associated with cognitive impairment in Parkinson’s disease. PLoS ONE 11:e152716
Tard C, Demailly F, Delval A et al (2015) Hypometabolism in posterior and temporal areas of the brain is associated with cognitive decline in Parkinson’s disease. J Parkinsons Dis 5:569–574
Benz N, Hatz F, Bousleiman H et al (2014) Slowing of EEG background activity in Parkinson’s and Alzheimer’s disease with early cognitive dysfunction. Front Aging Neurosci 6:314
Shimamura AP (1995) Memory and the prefrontal cortex. Ann N Y Acad Sci 769:151–159
Xu Y, Wei X, Liu X et al (2015) Low cerebral glucose metabolism: a potential predictor for the severity of vascular parkinsonism and Parkinson’s disease. Aging Dis 6:426–436
He X, Zhang Y, Chen J et al (2017) Changes in theta activities in the left posterior temporal region, left occipital region and right frontal region related to mild cognitive impairment in Parkinson’s disease patients. Int J Neurosci 127:66–72
Zhao Z, Lu J, Jia X et al (2014) Selective changes of resting-state brain oscillations in aMCI: an fMRI study using ALFF. Biomed Res Int 2014:920902
Buckner RL (2004) Memory and executive function in aging and AD: multiple factors that cause decline and reserve factors that compensate. Neuron 44:195–208
Wang L, Zang Y, He Y et al (2006) Changes in hippocampal connectivity in the early stages of Alzheimer’s disease: evidence from resting state fMRI. Neuroimage 31:496–504
Eklund A, Nichols TE, Knutsson H (2016) Cluster failure: why fMRI inferences for spatial extent have inflated false-positive rates. Proc Natl Acad Sci USA 113:7900–7905
Acknowledgements
This work was supported by the National Natural Science Foundation of China (81271429 and 81571228).
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflict of interest
The authors declare that they have no conflict of interest
Additional information
SPECIAL TOPIC: Mapping the Human Brain Function In Vivo
Linlin Gao and Xuemin Wu contributed equally to this work.
Electronic supplementary material
Below is the link to the electronic supplementary material.
About this article
Cite this article
Gao, L., Wu, X., Zhang, J. et al. Brain activity in Parkinson’s disease patients with mild cognitive impairment. Sci. Bull. 61, 1876–1883 (2016). https://doi.org/10.1007/s11434-016-1205-9
Received:
Revised:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s11434-016-1205-9