Abstract
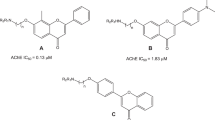
A series of prenylated resveratrol derivatives were designed, semisynthesized and biologically evaluated for inhibition of β-secretase (BACE1) and amyloid-β (Aβ) aggregation as well as free radical scavenging and neuroprotective and neuritogenic activities, as potential novel multifunctional agents against Alzheimer’s disease (AD). The results showed that compound 4b exhibited good anti-Aβ aggregation (IC50 = 4.78 µM) and antioxidant activity (IC50 = 41.22 µM) and moderate anti-BACE1 inhibitory activity (23.70% at 50 µM), and could be a lead compound. Moreover, this compound showed no neurotoxicity along with a greater ability to inhibit oxidative stress on P19-derived neuronal cells (50.59% cell viability at 1 nM). The neuritogenic activity presented more branching numbers (9.33) and longer neurites (109.74 µm) than the control, and was comparable to the quercetin positive control. Taken together, these results suggest compound 4b had the greatest multifunctional activities and might be a very promising lead compound for the further development of drugs for AD.
Graphical Abstract









Similar content being viewed by others
Change history
11 July 2017
An erratum to this article has been published.
References
Alzheimer’s association (2016) Alzheimer’s disease facts and figures. Alzheimers Dement 12:1–80
Okamura H, Ishii S, Ishii T, Eboshida A (2013) Prevalence of dementia in Japan: a systematic review. Dement Geriatr Cogn Disord 36:111–118
Klafki HW, Staufenbiel M, Kornhuber J, Wiltfang J (2006) Therapeutic approaches to Alzheimer’s disease. Brain 129:2840–2855
Terry JRAV, Buccafusco JJ (2003) The cholinergic hypothesis of age and Alzheimer’s disease-related cognitive deficits: recent challenges and their implications for novel drug development. J Pharm Exp Ther 306:821–827
Giacobini E (2004) Cholinesterase inhibitors: new roles and therapeutic alternatives. Pharmocol Res 50:433–440
Selkoe DJ, Hardy J (2016) The amyloid hypothesis of Alzheimer’s disease at 25 years. EMBO Mol Med 8:595–608
Bihel F, Das C, Bowman MJ, Wolfe MS (2004) Discovery of a subnanomolar helical d-tridecapeptide inhibitor of β-secretase. J Med Chem 47:3931–3933
Nishiyama Y, Taguchi H, Hara M, Planque SA, Mitsuda Y, Paul S (2014) Metal-dependent amyloid β-degrading catalytic antibody construct. J Biotechnol 180:17–22
Maccioni RB, Farias G, Morales I, Navarrete L (2010) The revitalized tau hypothesis on Alzheimer’s disease. Arch Med Res 41:226–231
Boutajangout A, Sigurdsson EM, Krishnamurthy PK (2011) Tau as a therapeutic target for Alzheimer’s Disease. Curr Alzheimer Res 8:666–677
Anand P, Singh B (2013) A review on cholinesterase inhibitors for Alzheimer’s disease. Arch Pharm Res 36:375–399
Cavalli A, Bolognesi ML, Minarini A, Rosini M, Tumiatti V, Recanatini M, Melchiorre C (2008) Multi-target-directed ligands to combat Neurodegenerative diseases. J Med Chem 51:347–372
Leon R, Garcia AG, Contelles JM (2013) Recent advances in the multitarget-directed ligands approach for the treatment of Alzheimer’s disease. Med Res Rev 33:139–189
Li RS, Wang XB, Hu XJ, Kong LY (2013) Design, synthesis and evaluation of flavonoid derivatives as potential multifunctional acetylcholinesterase inhibitors against Alzheimer’s disease. Bioorg Med Chem Lett 23:2636–2641
Xu ZC, Wang XB, Yu WY, Xie SS, Li SY, Kong LL (2014) Design, synthesis and biological evaluation of benzylisoquinoline derivatives as multifunctional agents against Alzheimer’s disease. Bioorg Med Chem Lett 24:2368–2373
Lu C, Guo Y, Yan J, Luo Z, Luo HB, Yan M, Huang L, Li X (2013) Design, synthesis, and evaluation of multitarget-directed resveratrol derivatives for the treatment of Alzheimer’s disease. J Med Chem 56:5843–5859
Li SY, Wang XB, Kong LY (2014) Design, synthesis and biological evaluation of imine resveratrol derivatives as multi-targeted agents against Alzheimer’s disease. Eur J Med Chem 71:36–45
Baur JA, Sinclair DA (2006) Therapeutic potential of resveratrol: the in vivo evidence. Nat Rev Drug Discov 5:493–506
Galli RL, Bielinski DF, Szprengiel A, Shukitt-Hale B, Joseph JA (2006) Blueberry supplemented diet reverses age-related decline in hippocampal HSP70 neuroprotection. Neurobiol Aging 27:344–350
Smoliga JM, Baur JA, Hausenblas HA (2011) Resveratrol and health—a comprehensive review of human clinical trials. Mol Nutr Food Res 55:1129–1141
Choi B, Kim S, Jang BG, Kim MJ (2016) Piceatannol, a natural analogue of resveratrol, effectively reduces beta-amyloid levels via activation of alpha-secretase and matrix metalloproteinase-9. J Funct Foods 23:124–134
Yazir Y, Utkan T, Gacar N, Aricioglu F (2015) Resveratrol exerts anti-inflammatory and neuroprotective effects to prevent memory deficits in rats exposed to chronic unpredictable mild stress. Physiol Behav 138:297–304
Turner RS, Thomas RG, Craft S, Van Dyck CH, Mintzer J, Reynolds BA, Aisen PS (2015) A randomized, double-blind, placebo-controlled trial of resveratrol for Alzheimer disease. Neurology 85:1383–1391
Tellone E, Galtieri A, Russo A, Giardina B, Ficarra S (2015) Resveratrol: a focus on several neurodegenerative diseases. Oxid Med Cell Longev doi:10.1155/2015/392169
Ohno M, Sametsky EA, Younkin LH, Oakley H, Younkin SG, Citron M, Disterhoft JF (2004) BACE1 deficiency rescues memory deficits and cholinergic dysfunction in a mouse model of Alzheimer’s disease. Neuron 41:27–33
DaSilva KA, Shaw JE, McLaurin J (2010) Amyloid-β fibrillogenesis: structural insight and therapeutic intervention. Exp Neurol 223:311–321
Nunomura A, Castellani RJ, Zhu X, Moreira PI, Perry G, Smith MA (2006) Involvement of oxidative stress in Alzheimer disease. J Neuropathol Exp Neurol 65:631–641
Mandel S, Youdim MB (2004) Catechin polyphenols: neurodegeneration and neuroprotection in neurodegenerative diseases. Free Radic Biol Med 37:304–317
Singh NA, Mandal AKA, Khan ZA (2016) Potential neuroprotective properties of epigallocatechin-3-gallate (EGCG). Nutr J 15:60
More SV, Koppula S, Kim IS, Kumar H, Kim BW, Choi DK (2012) The role of bioactive compounds on the promotion of neurite outgrowth. Molecules 17:6728–6753
Zhao HF, Li N, Wang Q, Cheng XJ, Li XM, Liu TT (2015) Resveratrol decreases the insoluble Aβ-42 Level in hippocamous and protects the integrity of the blood-brain barrier in AD rats. Neuroscience 310:641–649
Bastianetto S, Zheng WH, Quirion RJ (2000) Neuroprotective abilities of resveratrol and other red wine constituents against nitric oxide-related toxicity in cultured hippocampal neurons. Br J Pharmacol 131:711–720
Vella F, Ferry G, Delagrange P, Boutin JA (2005) NRH:quinone reductase 2: an enzyme of surprises and mysteries. Biochem Pharmacol 71:1–12
Bastianetto S, Menard C, Quirion R (2015) Neuroprotective action of resveratrol. Biochim Biophys Acta 1852:1195–1201
Cho JK, Ryu YB, Curtis-Long MJ, Kim JY, Kim D, Lee WS, Park KH (2011) Inhibition and structural reliability of prenylated flavones from the stem bark of Morus lhou on β-secretase (BACE-1). Bioorg Med Chem Lett 21:2945–2948
Marumoto S, Miyazawa M (2012) Structure–activity relationships for naturally occurring coumarins as β-secretase inhibitor. Bioorg Med Chem 20:784–788
Chanmahasathien W, Li Y, Satake M, Oshima Y, Ruangrungsi N, Ohizumi Y (2003) Prenylated xanthones with NGF-potentiating activity from Garcinia xanthochymus. Phytochemistry 64:981–986
Kano Y, Horie N, Doi S, Aramaki F, Maeda H, Hiragami F, Kawamura K, Motoda H, Koike Y, Akiyama J, Eguchi S, Hashimoto K (2008) Artepillin C derived from propolis induces neurite outgrowth in PC12m3 cells via ERK and p38 MAPK pathways. Neurochem Res 33:1795–1803
Chao J, Li H, Cheng KW, Yu MS, Chang RC, Wang M (2010) Protective effects of pinostilbene, a resveratrol methylated derivative, against 6-hydroxydopamine-induced neurotoxicity in SH-SY5Y cells. J Nutr Biochem 21:482–489
Orsini F, Verotta L, Lecchi M, Restano R, Curia G, Redaelli E, Wanke E (2004) Resveratrol derivatives and their role as potassium channels modulators. J Nat Prod 67:421–426
Ruan BF, Huang XF, Ding H, Xu C, Ge HM, Zhu HL, Tan RX (2006) Synthesis and cytotoxic evaluation of a series of resveratrol derivatives. Chem Biodivers 3:975–981
Kumano T, Richard SB, Noel JP, Nishiyama M, Kuzuyama T (2008) Chemoenzymatic syntheses of prenylated aromatic small molecules using Streptomyces prenyltransferases with relaxed substrate specificities. Bioorg Med Chem 16:8117–8126
Park BH, Lee HJ, Lee YR (2011) Total synthesis of chiricanine A, arahypin-1, trans-arachidin-2, trans-arachidin-3, and arahypin-5 from peanut seeds. J Nat Prod 74:644–649
Verotta L, Orsini F, Gerhauser C, Klimo K (2009) Biologically-activity stilbene derivatives and compositions thereof. PCT Int Appl WO 2009012910 A1 (patent number)
Kumano T, Tomita T, Nishiyama M, Kuzuyama T (2010) Functional characterization of the promiscuous prenyltransferase responsible for furaquinocin biosynthesis identification of a physiological polyketide substrate and its prenylated reaction products. J Biol Chem 285:39663–39671
Rodríguez RA, Lahoz IR, Faza ON, Cid MM, Lopez CS (2012) Theoretical and experimental exploration of the photochemistry of resveratrol: beyond the simple double bond isomerization. Org Biomol Chem 10:9175–9182
Mattarei A, Azzolini M, Carraro M, Sassi N, Zoratti M, Paradisi C, Biasutto L (2013) Acetal derivatives as prodrugs of resveratrol. Mol Pharm 10:2781–2792
Hartung AM, Beutler JA, Navarro HA, Wiemer DF, Neighbors JD (2014) Stilbenes as K-selective, non-nitrogenous opioid receptor antagonists. J Nat Prod 77:311–319
Jiaranaikulwanitch J, Boonyarat C, Fokin VV, Vajragupta O (2010) Triazolyl tryptoline derivatives as β-secretase inhibitors. Bioorg Med Chem Lett 20:6572–6576
Jiaranaikulwanitch J, Govitrapong P, Fokin VV, Vajragupta O (2012) From BACE1 inhibitor to multifunctionality of tryptoline and tryptamine triazole derivatives for Alzheimer’s disease. Molecules 17:8312–8333
Brand-Williams W, Cuvelier ME, Berset C (1995) Use of a free radical method to evaluate antioxidant activity. Lebensm Wiss Technol 28:25–30
McBurney MW (1993) P19 embryonal carcinoma cells. Intl J Dev Biol 37:135–140
MacPherson PA, McBurney MW (1995) P19 embryonal carcinoma cells: a source of cultured neurons amenable to genetic manipulation. Methods 7:238–252
Tadtong S, Athikomkulchai S, Sareedenchai V (2012) Neuritogenic activity of Thai plant extracts. J Health Res 26:293–296
Tangsaengvit N, Kitphati W, Tadtong S, Bunyapraphatsara N, Nukoolkarn V (2013) Neurite outgrowth and neuroprotective effects of quercetin from Caesalpinia mimosoides Lamk. on oultured P19-derived neurons. Evid Based Complement Alternat Med doi:10.1155/2013/838051
Tadtong S, Kanlayavattanakul M, Lourith N (2013) Neuritogenic and neuroprotective activities of fruit residues. Nat Prod Commun 8:1583–1586
Hamada Y, Miyamoto N, Kiso Y (2015) Novel β-amyloid aggregation inhibitors possessing a turn mimic. Bioorg Med Chem Lett 25:1572–1576
Ahmed M, Davis J, Aucoin D, Sato T, Ahuja S, Aimoto S, Elliott JI, Nostrand WV, Smith SO (2010) Structural conversion of neurotoxic amyloid-beta(1–42) oligomers to fibrils. Nat Struct Mol Biol 17:561–567
Shimizu H, Tosaki A, Kaneko K, Hisano T, Sakurai T, Nukina N (2008) Crystal structure of an active form of BACE1, an enzyme responsible for amyloid β protein production. Mol Cell Biol 28:3663–3671
Kim SH, Kumar CN, Kim HJ, Kim DH, Cho J, Jin C, Lee YS (2009) Glucose-containing flavones—their synthesis and antioxidant and neuroprotective activities. Bioorg Med Chem Lett 19:6009–6013
Hossain SU, Bhattacharya S (2007) Synthesis of O-prenylated and O geranylated derivatives of 5-benzylidene2,4-thiazolidinediones and evaluation of their free radical scavenging activity as well as effect on some phase II antioxidant/detoxifying enzymes. Bioorg Med Chem Lett 17:1149–1154
Tadtong S, Meksuriyen D, Tanasupawat S, Isobe M, Suwanborirux K (2007) Geldanamycin derivatives and neuroprotective effect on cultured P19-derived neurons. Bioorg Med Chem Lett 17:2939–2943
More SV, Koppula S, Kim IS, Kumar H, Kim BW, Choi DK (2012) The role of bioactive compounds on the promotion of neurite outgrowth. Molecules 7:6728–6753
Li P, Matsunaga K, Yumakuni T, Ohizumi Y (2002) Picrosides I and II, selective enhancers of the mitogen-activated protein kinase-dependent signaling pathway in the action of neuritogenic substances on PC12D cells. Life Sci 71:1821–1835
Acknowledgements
This project was supported by Mahidol University and the National Research Council of Thailand (NRCT). This work was supported in part by a grant from the Dementia Drug Resource Development Center Project (DRC), the Ministry of Education, Culture, Sports, Science and Technology (MEXT), Japan (S1511016). We also express their gratitude for research funding from the Meiji Pharmaceutical University Asia/Africa Center for Drug Discovery (MPU-AACDD).
Author information
Authors and Affiliations
Corresponding author
Additional information
The original version of this article was revised: The chemical structures of compounds 3a-d, 4a-c, and 5a-c were incorrect and it has been updated in this article.
Electronic supplementary material
Below is the link to the electronic supplementary material.
Rights and permissions
About this article
Cite this article
Puksasook, T., Kimura, S., Tadtong, S. et al. Semisynthesis and biological evaluation of prenylated resveratrol derivatives as multi-targeted agents for Alzheimer’s disease. J Nat Med 71, 665–682 (2017). https://doi.org/10.1007/s11418-017-1097-2
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s11418-017-1097-2