Abstract
Purpose
[68Ga]Trishydroxypyridinone (THP)–prostate-specific membrane antigen (PSMA) is a novel tracer that can be labeled in one step by cold reconstitution of a kit with unprocessed generator eluate, targeting PSMA via the lysine-urea-glutamate (KuE) motif. The aim of this study was to evaluate the human imaging characteristics of [68Ga]THP-PSMA.
Procedures
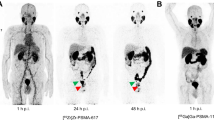
[68Ga]THP-PSMA positron emission tomography (PET)/x-ray computed tomography (CT) was performed in 25 patients with biochemical recurrence after radical prostatectomy for prostate cancer. Urinary and biliary excretion and tumor lesion uptake were quantified using standardized uptake values (SUVs). Imaging characteristics were assessed in terms of non-target organ uptake, background activity, target-to-background ratios (TBRs) of tumor lesions, and frequency of bladder halo artifacts. Findings were compared to a matched cohort of 25 patients undergoing PET/CT with the established agent [68Ga]PSMA I&T.
Results
Physiologic uptake of [68Ga]THP-PSMA was significantly lower in salivary glands (P < 0.0001), liver (P < 0.0001), spleen (P < 0.0001), and kidneys (P < 0.0001) than with [68Ga]PSMA I&T. While biliary tracer excretion of [68Ga]THP-PSMA was negligible, urinary tracer excretion of [68Ga]THP-PSMA was fast, and significantly higher than for [68Ga]PSMA I&T, contributing to a higher frequency of bladder artifacts. Malignant lesion uptake of [68Ga]THP-PSMA assessed as either SUV or TBR was significantly lower than with [68Ga]PSMA I&T.
Conclusion
[68Ga]THP-PSMA yields suitable in vivo uptake characteristics. The simplified synthesis method for [68Ga]THP-PSMA may facilitate wider application and higher patient throughput with PSMA imaging. However, direct intraindividual comparison studies are needed to assess the relative performance of [68Ga]THP-PSMA vs other PSMA ligands in terms of clinical detection rate and image quality.





Similar content being viewed by others
References
Afshar-Oromieh A, Avtzi E, Giesel FL, Holland-Letz T, Linhart HG, Eder M, Eisenhut M, Boxler S, Hadaschik BA, Kratochwil C, Weichert W, Kopka K, Debus J, Haberkorn U (2015) The diagnostic value of PET/CT imaging with the 68Ga-labelled PSMA ligand HBED-CC in the diagnosis of recurrent prostate cancer. Eur J Nucl Med Mol Imaging 42(2):197–209. https://doi.org/10.1007/s00259-014-2949-6
Eiber M, Weirich G, Holzapfel K, Souvatzoglou M, Haller B, Rauscher I, Beer AJ, Wester HJ, Gschwend J, Schwaiger M, Maurer T (2016) Simultaneous 68Ga-PSMA HBED-CC PET/MRI improves the localization of primary prostate cancer. Eur Urol 70(5):829–836. https://doi.org/10.1016/j.eururo.2015.12.053
Schmuck S, Mamach M, Wilke F, von Klot CA, Henkenberens C, Thackeray JT, Sohns JM, Geworski L, Ross TL, Wester HJ, Christiansen H, Bengel FM, Derlin T (2017) Multiple time-point 68Ga-PSMA I&T PET/CT for characterization of primary prostate cancer: value of early dynamic and delayed imaging. Clin Nucl Med 42(6):e286–e293. https://doi.org/10.1097/RLU.0000000000001589
Herrmann K, Bluemel C, Weineisen M, Schottelius M, Wester HJ, Czernin J, Eberlein U, Beykan S, Lapa C, Riedmiller H, Krebs M, Kropf S, Schirbel A, Buck AK, Lassmann M (2015) Biodistribution and radiation dosimetry for a probe targeting prostate-specific membrane antigen for imaging and therapy. J Nucl Med 56(6):855–861. https://doi.org/10.2967/jnumed.115.156133
Eiber M, Maurer T, Souvatzoglou M, Beer AJ, Ruffani A, Haller B, Graner FP, Kubler H, Haberhorn U, Eisenhut M, Wester HJ, Gschwend JE, Schwaiger M (2015) Evaluation of hybrid 68Ga-PSMA ligand PET/CT in 248 patients with biochemical recurrence after radical prostatectomy. J Nucl Med 56(5):668–674. https://doi.org/10.2967/jnumed.115.154153
Dietlein F, Kobe C, Neubauer S, Schmidt M, Stockter S, Fischer T, Schomäcker K, Heidenreich A, Zlatopolskiy BD, Neumaier B, Drzezga A, Dietlein M (2017) PSA-stratified performance of 18F- and 68Ga-labeled tracers in PSMA-PET imaging of patients with biochemical recurrence of prostate cancer. J Nucl Med 58(6):947–952. https://doi.org/10.2967/jnumed.116.185538
Schmuck S, Nordlohne S, von Klot CA, Henkenberens C, Sohns JM, Christiansen H, Wester HJ, Ross TL, Bengel FM, Derlin T (2017) Comparison of standard and delayed imaging to improve the detection rate of [68Ga]PSMA I&T PET/CT in patients with biochemical recurrence or prostate-specific antigen persistence after primary therapy for prostate cancer. Eur J Nucl Med Mol Imaging 44(6):960–968. https://doi.org/10.1007/s00259-017-3669-5
Rowe SP, Macura KJ, Mena E, Blackford AL, Nadal R, Antonarakis ES, Eisenberger M, Carducci M, Fan H, Dannals RF, Chen Y, Mease RC, Szabo Z, Pomper MG, Cho SY (2016) PSMA-based [(18)F]DCFPyL PET/CT is superior to conventional imaging for lesion detection in patients with metastatic prostate cancer. Mol Imaging Biol 18(3):411–419. https://doi.org/10.1007/s11307-016-0957-6
Giesel FL, Hadaschik B, Cardinale J, Radtke J, Vinsensia M, Lehnert W, Kesch C, Tolstov Y, Singer S, Grabe N, Duensing S, Schäfer M, Neels OC, Mier W, Haberkorn U, Kopka K, Kratochwil C (2017) F-18 labelled PSMA-1007: biodistribution, radiation dosimetry and histopathological validation of tumor lesions in prostate cancer patients. Eur J Nucl Med Mol Imaging 44(4):678–688. https://doi.org/10.1007/s00259-016-3573-4
Weineisen M, Schottelius M, Simecek J, Baum RP, Yildiz A, Beykan S, Kulkarni HR, Lassmann M, Klette I, Eiber M, Schwaiger M, Wester HJ (2015) 68Ga- and 177Lu-labeled PSMA I&T: optimization of a PSMA-targeted theranostic concept and first proof-of-concept human studies. J Nucl Med 56(8):1169–1176. https://doi.org/10.2967/jnumed.115.158550
Schmuck S, von Klot CA, Henkenberens C, Sohns JM, Christiansen H, Wester HJ, Ross TL, Bengel FM, Derlin T (2017) Initial experience with volumetric 68Ga-PSMA I&T PET/CT for assessment of whole-body tumor burden as a quantitative imaging biomarker in patients with prostate cancer. J Nucl Med 58(12):1962–1968. https://doi.org/10.2967/jnumed.117.193581
Derlin T, Weiberg D, von Klot C, Wester HJ, Henkenberens C, Ross TL, Christiansen H, Merseburger AS, Bengel FM (2016) 68Ga-PSMA I&T PET/CT for assessment of prostate cancer: evaluation of image quality after forced diuresis and delayed imaging. Eur Radiol 26(12):4345–4353. https://doi.org/10.1007/s00330-016-4308-4
Ebenhan T, Vorster M, Marjanovic-Painter B, Wagener J, Suthiram J, Modiselle M, Mokaleng B, Zeevaart J, Sathekge M (2015) Development of a single vial kit solution for radiolabeling of 68Ga-DKFZ-PSMA-11 and its performance in prostate cancer patients. Molecules 20(8):14860–14878. https://doi.org/10.3390/molecules200814860
Berry DJ, Ma Y, Ballinger JR, Tavaré R, Koers A, Sunassee K, Zhou T, Nawaz S, Mullen GED, Hider RC, Blower PJ (2011) Efficient bifunctional gallium-68 chelators for positron emission tomography: tris (hydroxypyridinone) ligands. Chem Commun 47(25):7068–7070. https://doi.org/10.1039/c1cc12123e
Ma MT, Cullinane C, Waldeck K, Roselt P, Hicks RJ, Blower PJ (2015) Rapid kit-based 68Ga-labelling and PET imaging with THP-Tyr(3)-octreotate: a preliminary comparison with DOTA-Tyr(3)-octreotate. EJNMMI Res 5(1):52. https://doi.org/10.1186/s13550-015-0131-1
Young JD, Abbate V, Imberti C, Meszaros LK, Ma MT, Terry SYA, Hider RC, Mullen GE, Blower PJ (2017) 68Ga-THP-PSMA: a PET imaging agent for prostate cancer offering rapid, room temperature, one-step kit-based radiolabeling. J Nucl Med 58(8):1270–1277. https://doi.org/10.2967/jnumed.117.191882
Martin R, Jüttler S, Müller M, Wester HJ (2014) Cationic eluate pretreatment for automated synthesis of [68Ga]CPCR4.2. Nucl Med Biol 41(1):84–89. https://doi.org/10.1016/j.nucmedbio.2013.09.002
Giesel FL, Fiedler H, Stefanova M, Sterzing F, Rius M, Kopka K, Moltz JH, Afshar-Oromieh A, Choyke PL, Haberkorn U, Kratochwil C (2015) PSMA PET/CT with Glu-urea-Lys-(Ahx)-[68Ga(HBED-CC)] versus 3D CT volumetric lymph node assessment in recurrent prostate cancer. Eur J Nucl Med Mol Imaging 42(12):1794–1800. https://doi.org/10.1007/s00259-015-3106-6
McCarthy M, Langton T, Kumar D, Campbell A (2017) Comparison of PSMA-HBED and PSMA-I&T as diagnostic agents in prostate carcinoma. Eur J Nucl Med Mol Imaging 44:1455–1462. https://doi.org/10.1007/s00259-017-3699-z
Silver DA, Pellicer I, Fair WR, Heston WD, Cordon-Cardo C (1997) Prostate-specific membrane antigen expression in normal and malignant human tissues. Clin Cancer Res 3(1):81–85.
Uprimny C, Kroiss AS, Decristoforo C, Fritz J, Warwitz B, Scarpa L, Roig LG, Kendler D, von Guggenberg E, Bektic J, Horninger W, Virgolini IJ (2017) Early dynamic imaging in 68Ga- PSMA-11 PET/CT allows discrimination of urinary bladder activity and prostate cancer lesions. Eur J Nucl Med Mol Imaging 44(5):765–775. https://doi.org/10.1007/s00259-016-3578-z
Afshar-Oromieh A, Sattler LP, Mier W, Hadaschik BA, Debus J, Holland-Letz T, Kopka K, Haberkorn U (2017) The clinical impact of additional late PET/CT imaging with 68Ga-PSMA-11 (HBED-CC) in the diagnosis of prostate cancer. J Nucl Med 58(5):750–755. https://doi.org/10.2967/jnumed.116.183483
Afshar-Oromieh A, Holland-Letz T, Giesel FL, Kratochwil C, Mier W, Haufe S, Debus N, Eder M, Eisenhut M, Schäfer M, Neels O, Hohenfellner M, Kopka K, Kauczor HU, Debus J, Haberkorn U (2017) Diagnostic performance of 68Ga-PSMA-11 (HBED-CC) PET/CT in patients with recurrent prostate cancer: evaluation in 1007 patients. Eur J Nucl Med Mol Imaging 44(8):1258–1268. https://doi.org/10.1007/s00259-017-3711-7
Hope TA, Truillet C, Ehman EC, Afshar-Oromieh A, Aggarwal R, Ryan CJ, Carroll PR, Small EJ, Evans MJ (2017) 68Ga-PSMA-11 PET imaging of response to androgen receptor inhibition: first human experience. J Nucl Med 58(1):81–84. https://doi.org/10.2967/jnumed.116.181800
Hofman MS, Eu P, Jackson P, Hong E, Binns D, Iravani A, Murphy D, Mitchell C, Siva S, Hicks RJ, Young JD, Blower P, Mullen GE (2017) Cold kit PSMA PET imaging: phase I study of 68Ga-THP-PSMA PET/CT in patients with prostate cancer. J Nucl Med. https://doi.org/10.2967/jnumed.117.199554
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflicts of Interest and Sources of Funding
Dr. Hans-Jürgen Wester is a shareholder of Scintomics. THP-PSMA was provided by ROTOP Pharmaka GmbH under an academic agreement, and Dr. Cathleen Juhl, Steffi Teichert, and Dr. Johanna Zörgiebel are employees of ROTOP Pharmaka GmbH. No other potential conflict of interest relevant to this article was reported.
Rights and permissions
About this article
Cite this article
Derlin, T., Schmuck, S., Juhl, C. et al. Imaging Characteristics and First Experience of [68Ga]THP-PSMA, a Novel Probe for Rapid Kit-Based Ga-68 Labeling and PET Imaging: Comparative Analysis with [68Ga]PSMA I&T. Mol Imaging Biol 20, 650–658 (2018). https://doi.org/10.1007/s11307-018-1160-8
Published:
Issue Date:
DOI: https://doi.org/10.1007/s11307-018-1160-8