Abstract
Purpose
To assess the predictive value of procalcitonin (PCT) in the risk of sepsis in patients with stage 5 chronic kidney disease (CKD).
Methods
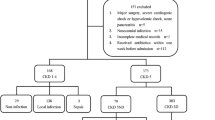
A total of 373 inpatients with stage 5 CKD were retrospectively analyzed. The patients were divided into non-infection group, local infection group, and sepsis group. The clinical characteristics and inflammatory parameters including PCT, C-reactive protein (CRP), white blood cell count (WBC), and neutrophil percentage (NEU%) were compared and the receiver operating characteristic (ROC) curves to predict sepsis were plotted. Related risk factors of sepsis were analyzed by logistic regression analysis.
Results
(1) The hemodialysis ratio of sepsis group was the highest at 92.3%. PCT, CRP, and NEU% were significantly different among the three subgroups (P < 0.05 for all). Total cholesterol and low density lipoprotein (LDL) levels in sepsis group were significantly lower than that in local infection group (P < 0.05 for both). (2) CRP and WBC were unable to predict sepsis (P > 0.05 for all), while PCT and NEU% could predict sepsis with areas under the curve (AUC) of 0.838 and 0.691, respectively (P < 0.05 for all). (3) Multivariate logistic regression analysis showed that PCT > 1.650 ng/mL was a risk factor (OR = 6.926, P = 0.002) while LDL was probably a protective factor (OR = 0.336, P = 0.040) of sepsis in patients with stage 5 CKD.
Conclusions
At stage 5 CKD, the predictive value of PCT for sepsis is best among inflammatory markers, and PCT and LDL levels are independent factors of sepsis.

Similar content being viewed by others
Data availability
All data generated or analyzed during this study are included in this published article.
Abbreviations
- CKD:
-
Chronic kidney disease
- PCT:
-
Procalcitonin
- CRP:
-
C-reactive protein
- WBC:
-
White blood cell count
- NEU%:
-
Neutrophil percentage
- ALAT:
-
Alanine aminotransferase
- ASAT:
-
Aspartate aminotransferase
- ROC:
-
Receiver operating characteristic
- AUC:
-
Areas under the curve
- ESRD:
-
End-stage renal diseases
- RRT:
-
Renal replacement therapy
- SIRS:
-
Systemic inflammatory response syndrome
- GFR:
-
Glomerular filtration rate
- eGFR:
-
Estimated glomerular filtration rate
- SCr:
-
Serum creatinine
- BUN:
-
Blood urea nitrogen
- TCHO:
-
Total cholesterol
- TG:
-
Triglyceride
- LDL:
-
High density lipoprotein
- HDL:
-
Low density lipoprotein
- PD:
-
Peritoneal dialysis
- HD:
-
Hemodialysis
- CAD:
-
Coronary atherosclerotic disease
References
Mills KT, Xu Y, Zhang W, Bundy JD, Chen CS, Kelly TN, Chen J, He J (2015) A systematic analysis of worldwide population-based data on the global burden of chronic kidney disease in 2010. Kidney Int 88(5):950–957. https://doi.org/10.1038/ki.2015.230
Coresh J, Selvin E, Stevens LA, Manzi J, Kusek JW, Eggers P, Van Lente F, Levey AS (2007) Prevalence of chronic kidney disease in the United States. JAMA 298(17):2038–2047. https://doi.org/10.1001/jama.298.17.2038
Perner A, Rhodes A, Venkatesh B, Angus DC, Martin-Loeches I, Preiser JC, Vincent JL, Marshall J, Reinhart K, Joannidis M, Opal SM (2017) Sepsis: frontiers in supportive care, organisation and research. Intensive Care Med 43(4):496–508. https://doi.org/10.1007/s00134-017-4677-4
Girndt M, Sester M, Sester U, Kaul H, Kohler H (2001) Molecular aspects of T- and B-cell function in uremia. Kidney Int Suppl 78:S206–S211. https://doi.org/10.1046/j.1523-1755.2001.59780206.x
McDonald HI, Thomas SL, Nitsch D (2014) Chronic kidney disease as a risk factor for acute community-acquired infections in high-income countries: a systematic review. BMJ Open 4(4):e004100. https://doi.org/10.1136/bmjopen-2013-004100
Collins AJ, Foley R, Herzog C, Chavers B, Gilbertson D, Ishani A, Kasiske B, Liu J, Mau LW, McBean M, Murray A, St Peter W, Xue J, Fan Q, Guo H, Li Q, Li S, Li S, Peng Y, Qiu Y, Roberts T, Skeans M, Snyder J, Solid C, Wang C, Weinhandl E, Zaun D, Zhang R, Arko C, Chen SC, Dalleska F, Daniels F, Dunning S, Ebben J, Frazier E, Hanzlik C, Johnson R, Sheets D, Wang X, Forrest B, Constantini E, Everson S, Eggers P, Agodoa L (2008) Excerpts from the United States Renal Data System 2007 annual data report. Am J Kidney Dis 51(1 Suppl 1):S1–S320. https://doi.org/10.1053/j.ajkd.2007.11.001
Sarnak MJ, Jaber BL (2000) Mortality caused by sepsis in patients with end-stage renal disease compared with the general population. Kidney Int 58(4):1758–1764. https://doi.org/10.1111/j.1523-1755.2000.00337.x
Wang HE, Shapiro NI, Griffin R, Safford MM, Judd S, Howard G (2012) Chronic medical conditions and risk of sepsis. PLoS ONE 7(10):e48307. https://doi.org/10.1371/journal.pone.0048307
Pepys MB, Hirschfield GM (2003) C-reactive protein: a critical update. J Clin Invest 111(12):1805–1812. https://doi.org/10.1172/jci18921
Sager R, Kutz A, Mueller B, Schuetz P (2017) Procalcitonin-guided diagnosis and antibiotic stewardship revisited. BMC Med 15(1):15. https://doi.org/10.1186/s12916-017-0795-7
Herget-Rosenthal S, Marggraf G, Pietruck F, Husing J, Strupat M, Philipp T, Kribben A (2001) Procalcitonin for accurate detection of infection in haemodialysis. Nephrol Dial Transplant 16(5):975–979
Sitter T, Schmidt M, Schneider S, Schiffl H (2002) Differential diagnosis of bacterial infection and inflammatory response in kidney diseases using procalcitonin. J Nephrol 15(3):297–301
Dahaba AA, Rehak PH, List WF (2003) Procalcitonin and C-reactive protein plasma concentrations in nonseptic uremic patients undergoing hemodialysis. Intensive Care Med 29(4):579–583. https://doi.org/10.1007/s00134-003-1664-8
Dumea R, Siriopol D, Hogas S, Mititiuc I, Covic A (2014) Procalcitonin: diagnostic value in systemic infections in chronic kidney disease or renal transplant patients. Int Urol Nephrol 46(2):461–468. https://doi.org/10.1007/s11255-013-0542-8
Grace E, Turner RM (2014) Use of procalcitonin in patients with various degrees of chronic kidney disease including renal replacement therapy. Clin Infect Dis 59(12):1761–1767. https://doi.org/10.1093/cid/ciu732
Schmidt M, Burchardi C, Sitter T, Held E, Schiffl H (2000) Procalcitonin in patients undergoing chronic hemodialysis. Nephron 84(2):187–188
Meisner M, Schmidt J, Huttner H, Tschaikowsky K (2000) The natural elimination rate of procalcitonin in patients with normal and impaired renal function. Intensive Care Med 26(Suppl 2):S212–S216. https://doi.org/10.1007/bf02900740
Opatrna S, Klaboch J, Opatrny K Jr, Holubec L, Tomsu M, Sefrna F, Topolcan O (2005) Procalcitonin levels in peritoneal dialysis patients. Perit Dial Int 25(5):470–472
Herget-Rosenthal S, Klein T, Marggraf G, Hirsch T, Jakob HG, Philipp T, Kribben A (2005) Modulation and source of procalcitonin in reduced renal function and renal replacement therapy. Scand J Immunol 61(2):180–186. https://doi.org/10.1111/j.0300-9475.2005.01545.x
Steinbach G, Bolke E, Grunert A, Storck M, Orth K (2004) Procalcitonin in patients with acute and chronic renal insufficiency. Wien Klin Wochenschr 116(24):849–853
Yilmaz FM, Yilmaz G, Akay H, Duranay M, Yucel D (2007) Evaluation of a card test for procalcitonin in continuous ambulatory peritoneal dialysis peritonitis. Ann Clin Biochem 44(Pt 5):482–484. https://doi.org/10.1258/000456307781646094
Guz G, Colak B, Hizel K, Reis KA, Erten Y, Bali M, Sindel S (2006) Procalcitonin and conventional markers of inflammation in peritoneal dialysis patients and peritonitis. Perit Dial Int 26(2):240–248
Lam MF, Leung JC, Lam CW, Tse KC, Lo WK, Lui SL, Chan TM, Tam S, Lai KN (2008) Procalcitonin fails to differentiate inflammatory status or predict long-term outcomes in peritoneal dialysis-associated peritonitis. Perit Dial Int 28(4):377–384
Amour J, Birenbaum A, Langeron O, Le Manach Y, Bertrand M, Coriat P, Riou B, Bernard M, Hausfater P (2008) Influence of renal dysfunction on the accuracy of procalcitonin for the diagnosis of postoperative infection after vascular surgery. Crit Care Med 36(4):1147–1154. https://doi.org/10.1097/CCM.0b013e3181692966
Levey AS, Coresh J, Bolton K, Culleton B, Harvey KS, Ikizler TA, Johnson CA, Kausz A, Kimmel PL, Kusek J, Levin A (2002) K/DOQI clinical practice guidelines for chronic kidney disease: evaluation, classification, and stratification. Am J Kidney Dis 39(2 Suppl 1):S1–S266
Levey AS, Stevens LA, Schmid CH, Zhang YL, Castro AF III, Feldman HI, Kusek JW, Eggers P, Van Lente F, Greene T, Coresh J (2009) A new equation to estimate glomerular filtration rate. Ann Intern Med 150(9):604–612
Dellinger RP, Levy MM, Rhodes A, Annane D, Gerlach H, Opal SM, Sevransky JE, Sprung CL, Douglas IS, Jaeschke R, Osborn TM, Nunnally ME, Townsend SR, Reinhart K, Kleinpell RM, Angus DC, Deutschman CS, Machado FR, Rubenfeld GD, Webb SA, Beale RJ, Vincent JL, Moreno R (2013) Surviving sepsis campaign: international guidelines for management of severe sepsis and septic shock: 2012. Crit Care Med 41(2):580–637. https://doi.org/10.1097/CCM.0b013e31827e83af
James MT, Quan H, Tonelli M, Manns BJ, Faris P, Laupland KB, Hemmelgarn BR (2009) CKD and risk of hospitalization and death with pneumonia. Am J Kidney Dis 54(1):24–32. https://doi.org/10.1053/j.ajkd.2009.04.005
Davenport A (2009) Peritonitis remains the major clinical complication of peritoneal dialysis: the London, UK, peritonitis audit 2002–2003. Perit Dial Int 29(3):297–302
Mactier R (2009) Peritonitis is still the achilles’ heel of peritoneal dialysis. Perit Dial Int 29(3):262–266
Hildebrand A, Komenda P, Miller L, Rigatto C, Verrelli M, Sood AR, Sathianathan C, Reslerova M, Eng L, Eng A, Sood MM (2010) Peritonitis and exit site infections in First Nations patients on peritoneal dialysis. Clin J Am Soc Nephrol 5(11):1988–1995. https://doi.org/10.2215/cjn.04170510
James MT, Laupland KB, Tonelli M, Manns BJ, Culleton BF, Hemmelgarn BR (2008) Risk of bloodstream infection in patients with chronic kidney disease not treated with dialysis. Arch Intern Med 168(21):2333–2339. https://doi.org/10.1001/archinte.168.21.2333
Orasan OH, Sava M, Iancu M, Cozma A, Saplontai-Pop A, Sarlea Tarmure S, Lungoci C, Orasan RA, Patiu IM, Dumitrascu DL (2015) Serum hyaluronic acid in chronic viral hepatitis B and C: a biomarker for assessing liver fibrosis in chronic hemodialysis patients. Int Urol Nephrol 47(7):1209–1217. https://doi.org/10.1007/s11255-015-1017-x
Orasan OH, Iancu M, Sava M, Saplontai-Pop A, Cozma A, Sarlea ST, Lungoci C, Ungureanu MI, Negrean V, Sampelean D, Dumitrascu DL (2015) Non-invasive assessment of liver fibrosis in chronic viral hepatitis. Eur J Clin Invest 45(12):1243–1251. https://doi.org/10.1111/eci.12543
Trimarchi H, Dicugno M, Muryan A, Lombi F, Iturbe L, Rana MS, Young P, Nau K, Iriarte R, Pomeranz V, Forrester M, Karl A, Alonso M (2013) Pro-calcitonin and inflammation in chronic hemodialysis. Medicina 73(5):411–416
Luzzani A, Polati E, Dorizzi R, Rungatscher A, Pavan R, Merlini A (2003) Comparison of procalcitonin and C-reactive protein as markers of sepsis. Crit Care Med 31(6):1737–1741. https://doi.org/10.1097/01.ccm.0000063440.19188.ed
Castelli GP, Pognani C, Meisner M, Stuani A, Bellomi D, Sgarbi L (2004) Procalcitonin and C-reactive protein during systemic inflammatory response syndrome, sepsis and organ dysfunction. Crit Care 8(4):R234–R242. https://doi.org/10.1186/cc2877
Schuetz P, Albrich W, Christ-Crain M, Chastre J, Mueller B (2010) Procalcitonin for guidance of antibiotic therapy. Expert Rev Anti-infect Ther 8(5):575–587. https://doi.org/10.1586/eri.10.25
Lee SH, Chan RC, Wu JY, Chen HW, Chang SS, Lee CC (2013) Diagnostic value of procalcitonin for bacterial infection in elderly patients—a systemic review and meta-analysis. Int J Clin Pract 67(12):1350–1357. https://doi.org/10.1111/ijcp.12278
Lu XL, Xiao ZH, Yang MY, Zhu YM (2013) Diagnostic value of serum procalcitonin in patients with chronic renal insufficiency: a systematic review and meta-analysis. Nephrol Dial Transplant 28(1):122–129. https://doi.org/10.1093/ndt/gfs339
Park JH, Kim DH, Jang HR, Kim MJ, Jung SH, Lee JE, Huh W, Kim YG, Kim DJ, Oh HY (2014) Clinical relevance of procalcitonin and C-reactive protein as infection markers in renal impairment: a cross-sectional study. Crit Care 18(6):640. https://doi.org/10.1186/s13054-014-0640-8
Lee SH, Park MS, Park BH, Jung WJ, Lee IS, Kim SY, Kim EY, Jung JY, Kang YA, Kim YS, Kim SK, Chang J, Chung KS (2015) Prognostic implications of serum lipid metabolism over time during sepsis. BioMed Res Int 2015:789298. https://doi.org/10.1155/2015/789298
Guirgis FW, Donnelly JP, Dodani S, Howard G, Safford MM, Levitan EB, Wang HE (2016) Cholesterol levels and long-term rates of community-acquired sepsis. Crit Care 20(1):408. https://doi.org/10.1186/s13054-016-1579-8
Lagrost L, Girard C, Grosjean S, Masson D, Deckert V, Gautier T, Debomy F, Vinault S, Jeannin A, Labbe J, Bonithon-Kopp C (2014) Low preoperative cholesterol level is a risk factor of sepsis and poor clinical outcome in patients undergoing cardiac surgery with cardiopulmonary bypass. Crit Care Med 42(5):1065–1073. https://doi.org/10.1097/ccm.0000000000000165
Feingold KR, Grunfeld C (1997) Lipoproteins: are they important components of host defense? Hepatology 26(6):1685–1686. https://doi.org/10.1002/hep.510260647
Hakeem A, Bhatti S, Chang SM (2014) Screening and risk stratification of coronary artery disease in end-stage renal disease. JACC Cardiovasc Imaging 7(7):715–728. https://doi.org/10.1016/j.jcmg.2013.12.015
Funding
This work was supported by Natural Science Foundation of China (No. 81771798).
Author information
Authors and Affiliations
Contributions
YS and XS conceived of the study, and drafted the manuscript. LJ carried out the Lab testing. XS participated in the design of the study and performed the statistical analysis.
Corresponding author
Ethics declarations
Conflict of interest
The authors declare that they have no competing interests.
Ethical approval
The study has been approved by the Ethics Committee of Soochow University.
Rights and permissions
About this article
Cite this article
Jiang, L., Shao, X., Xing, W. et al. Biomarkers and risk factors for sepsis in stage 5 chronic kidney disease: a retrospective case–control study. Int Urol Nephrol 51, 691–698 (2019). https://doi.org/10.1007/s11255-018-2035-2
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s11255-018-2035-2