Abstract
Purpose
Several studies investigated the association between the estimated glomerular filtration rate (eGFR) and the concentration of high-density lipoproteins (HDL) in patients without severely damaged kidney function. As results of those studies were inconclusive and contradictory, we wanted to investigate this association in multiple cardiovascular disease (CVD) risk patients without severe kidney disease or renal failure.
Methods
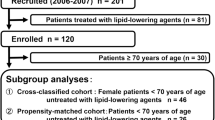
We enrolled a cohort of 187 patients with intermediate and high CVD risk without severe renal disease. We grouped them based on their eGFR into: group 1 (≥ 30 < 60 ml/min/1.73 m2), group 2 (≥ 60 < 90 ml/min/1.73 m2) and group 3 (≥ 90 ml/min/1.73 m2). We analyzed the difference between their HDL levels and assessed the association of HDL and eGFR in three regression models with the following predictors: model 1 (age and gender), model 2 (model 1 plus smoking status, hs-CRP and diabetes mellitus) and model 3 (model 2 plus excessive weight and obesity, hypertension, hypercholesterolemia, hypertriglyceridemia, family history of CVD and medications they used).
Results
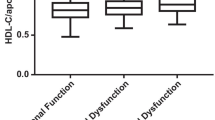
Patients with the lowest eGFR had the lowest HDL values (P = 0.013). In multiple linear regression, HDL was an independent predictor of eGFR (β = 0.189, P = 0.025) which was also shown in multinomial regression for all three models: model 1 [odds ratio (OR) 0.05; 95% confidence interval (CI) 0.007–0.331; P = 0.002], model 2 (OR 0.052; 95% CI 0.006–0.428; P = 0.006) and model 3 (OR 0.2; 95% CI 0.001–0.309; P = 0.005).
Conclusions
Low HDL is an independent predictor of lower eGFR in intermediate and high CVD risk patients without severe kidney disease. In such patients, low HDL could be one of the early indicators of renal failure.
Similar content being viewed by others
References
Ketteler M, Block GA, Evenepoel P et al (2017) Executive summary of the 2017 KDIGO Chronic Kidney Disease—Mineral and Bone Disorder (CKD-MBD) Guideline Update: what’s changed and why it matters. Kidney Int 92:26–36. https://doi.org/10.1016/j.kint.2017.04.006
Hill NR, Fatoba ST, Oke JL et al (2016) Global prevalence of chronic kidney disease—a systematic review and meta-analysis. PLoS One 11:e0158765. https://doi.org/10.1371/journal.pone.0158765
Yee J (2008) Chronic kidney disease—a disease domain complex. Geriatrics 63:30–37
Quinn MP, Cardwell CR, Kee F et al (2011) The finding of reduced estimated glomerular filtration rate is associated with increased mortality in a large UK population. Nephrol Dial Transpl 26:875–880. https://doi.org/10.1093/ndt/gfq505
Odden MC, Tager IB, Gansevoort RT et al (2013) Hypertension and low HDL cholesterol were associated with reduced kidney function across the age spectrum: a collaborative study. Ann Epidemiol 23:106–111. https://doi.org/10.1016/j.annepidem.2012.12.004
Briganti EM, Branley P, Chadban SJ et al (2002) Smoking is associated with renal impairment and proteinuria in the normal population: the AusDiab kidney study. Australian Diabetes, Obesity and Lifestyle Study. Am J Kidney Dis 40:704–712
Ejerblad E, Fored CM, Lindblad P et al (2006) Obesity and risk for chronic renal failure. J Am Soc Nephrol 17:1695–1702. https://doi.org/10.1681/ASN.2005060638
Fox CS, Larson MG, Leip EP et al (2004) Predictors of new-onset kidney disease in a community-based population. JAMA 291:844–850. https://doi.org/10.1001/jama.291.7.844
Hunsicker LG, Adler S, Caggiula A et al (1997) Predictors of the progression of renal disease in the Modification of Diet in Renal Disease Study. Kidney Int 51:1908–1919
Muntner P, Coresh J, Smith JC et al (2000) Plasma lipids and risk of developing renal dysfunction: the atherosclerosis risk in communities study. Kidney Int 58:293–301. https://doi.org/10.1046/j.1523-1755.2000.00165.x
Milman S, Atzmon G, Crandall J, Barzilai N (2014) Phenotypes and genotypes of high density lipoprotein cholesterol in exceptional longevity. Curr Vasc Pharmacol 12:690–697
Barzilai N, Atzmon G, Schechter C et al (2003) Unique lipoprotein phenotype and genotype associated with exceptional longevity. JAMA 290:2030–2040. https://doi.org/10.1001/jama.290.15.2030
Vega GL, Grundy SM (1996) Hypoalphalipoproteinemia (low high density lipoprotein) as a risk factor for coronary heart disease. Curr Opin Lipidol 7:209–216
Kozyraki R, Fyfe J, Kristiansen M et al (1999) The intrinsic factor-vitamin B12 receptor, cubilin, is a high-affinity apolipoprotein A-I receptor facilitating endocytosis of high-density lipoprotein. Nat Med 5:656–661. https://doi.org/10.1038/9504
Hammad SM, Barth JL, Knaak C, Argraves WS (2000) Megalin acts in concert with cubilin to mediate endocytosis of high density lipoproteins. J Biol Chem 275:12003–12008
Moradi H, Vaziri ND, Kashyap ML et al (2013) Role of HDL dysfunction in end-stage renal disease: a double-edged sword. J Ren Nutr 23:203–206. https://doi.org/10.1053/j.jrn.2013.01.022
Roehrs M, Valentini J, Paniz C et al (2011) The relationships between exogenous and endogenous antioxidants with the lipid profile and oxidative damage in hemodialysis patients. BMC Nephrol 12:59. https://doi.org/10.1186/1471-2369-12-59
Yoshida T, Takei T, Shirota S et al (2008) Risk factors for progression in patients with early-stage chronic kidney disease in the Japanese population. Intern Med 47:1859–1864
Ganda A, Magnusson M, Yvan-Charvet L et al (2013) Mild renal dysfunction and metabolites tied to low HDL cholesterol are associated with monocytosis and atherosclerosis. Circulation 127:988–996. https://doi.org/10.1161/CIRCULATIONAHA.112.000682
Krikken JA, Gansevoort RT, Dullaart RPF, PREVEND Study Group (2010) Lower HDL-C and apolipoprotein A-I are related to higher glomerular filtration rate in subjects without kidney disease. J Lipid Res 51:1982–1990. https://doi.org/10.1194/jlr.m005348
Qin X, Wang Y, Li Y et al (2015) Risk factors for renal function decline in adults with normal kidney function: a 7-year cohort study. J Epidemiol Community Health 69:782–788. https://doi.org/10.1136/jech-2014-204962
Wang F, Zheng J, Ye P et al (2013) Association of high-density lipoprotein cholesterol with the estimated glomerular filtration rate in a community-based population. PLoS One 8:e79738. https://doi.org/10.1371/journal.pone.0079738
Grundy SM, Balady GJ, Criqui MH et al (1998) Primary prevention of coronary heart disease: guidance from Framingham: a statement for healthcare professionals from the AHA Task Force on Risk Reduction. American Heart Association. Circulation 97:1876–1887
Shankar A, Leng C, Chia KS et al (2008) Association between body mass index and chronic kidney disease in men and women: population-based study of Malay adults in Singapore. Nephrol Dial Transpl 23:1910–1918. https://doi.org/10.1093/ndt/gfm878
(c2005) Cardiovascular Risk Calculator. http://cvrisk.mvm.ed.ac.uk/calculator/framingham.htm. Accessed 20 April 2016
Levey A, Greene T, Kusek J (2000) A simplified equation to predict glomerular filtration rate from serum creatinine. J Am Soc Nephrol 11:155A
Boerrigter G, Costello-Boerrigter LC, Abraham WT et al (2008) Cardiac resynchronization therapy improves renal function in human heart failure with reduced glomerular filtration rate. J Card Fail 14:539–546. https://doi.org/10.1016/j.cardfail.2008.03.009
Zheng D, Sato S, Arima H et al (2016) Estimated GFR and the effect of intensive blood pressure lowering after acute intracerebral hemorrhage. Am J Kidney Dis 68:94–102. https://doi.org/10.1053/j.ajkd.2016.01.020
Cedeño Mora S, Goicoechea M, Torres E et al (2017) Cardiovascular risk prediction in chronic kidney disease patients. Nefrol Publ Soc Esp Nefrol 37:293–300. https://doi.org/10.1016/j.nefro.2016.10.002
Tomaszewski M, Charchar FJ, Maric C et al (2007) Glomerular hyperfiltration: a new marker of metabolic risk. Kidney Int 71:816–821. https://doi.org/10.1038/sj.ki.5002160
Verhave JC, Hillege HL, Burgerhof JGM et al (2005) The association between atherosclerotic risk factors and renal function in the general population. Kidney Int 67:1967–1973. https://doi.org/10.1111/j.1523-1755.2005.00296.x
Zheng W, Qian G, Hao W et al (2016) Cardiovascular metabolic risk factors and glomerular filtration rate: a rural Chinese population study. Lipids Health Dis 15:180. https://doi.org/10.1186/s12944-016-0346-9
de Boer IH, Astor BC, Kramer H et al (2008) Lipoprotein abnormalities associated with mild impairment of kidney function in the multi-ethnic study of atherosclerosis. Clin J Am Soc Nephrol 3:125–132. https://doi.org/10.2215/CJN.03390807
Bowe B, Xie Y, Xian H et al (2016) Low levels of high-density lipoprotein cholesterol increase the risk of incident kidney disease and its progression. Kidney Int 89:886–896. https://doi.org/10.1016/j.kint.2015.12.034
Textor SC, Misra S, Oderich GS (2013) Percutaneous revascularization for ischemic nephropathy: the past, present, and future. Kidney Int 83:28–40. https://doi.org/10.1038/ki.2012.363
Morton J, Zoungas S, Li Q et al (2012) Low HDL cholesterol and the risk of diabetic nephropathy and retinopathy: results of the ADVANCE study. Diabet Care 35:2201–2206. https://doi.org/10.2337/dc12-0306
Yamamoto S, Yancey PG, Ikizler TA et al (2012) Dysfunctional high-density lipoprotein in patients on chronic hemodialysis. J Am Coll Cardiol 60:2372–2379. https://doi.org/10.1016/j.jacc.2012.09.013
Pedone C, Semeraro R, Chiurco D et al (2013) Reliability of equations to estimate glomerular filtration rate in the very old. Aging Clin Exp Res 20:496–502. https://doi.org/10.1007/BF03324875
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflict of interest
The authors declare that they have no conflict of interest.
Ethical approval
All procedures performed in studies involving human participants were in accordance with the ethical standards of the institutional and/or national research committee and with the 1964 Helsinki Declaration and its later amendments or comparable ethical standards.
Rights and permissions
About this article
Cite this article
Markovic, D., Trgo, G., Prkacin, I. et al. The association between high-density lipoproteins and estimated glomerular filtration rate in patients without severe kidney disease. Int Urol Nephrol 50, 1105–1112 (2018). https://doi.org/10.1007/s11255-018-1851-8
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s11255-018-1851-8