Abstract
Purpose
The aim of this prospective, observational study was to investigate the relationship between premature ejaculation (PE) and female sexual response cycle, using the female sexual function index (FSFI). The FSFI evaluates female sexual function in six domains: desire, arousal, lubrication, orgasm, satisfaction, and pain.
Methods
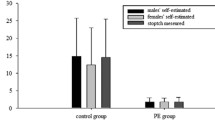
All men were considered to have PE if they fulfilled the criteria of the second Ad Hoc International Society for Sexual Medicine (ISSM) Committee. All men were also assessed by the Premature Ejaculation Diagnostic Tool (PEDT) and intravaginal ejaculatory latency time (IELT) using stopwatch which was held by the partner. All women completed the FSFI.
Results
A total of 181 couples who had regular sexual intercourse with one partner for the past 6 months were enrolled the study. By the definition of ISSM Committee, there were 117 men with PE and 64 men without PE. Partners of men with PE had significantly lower total FSFI scores than did partners of men without PE (21.8 ± 3.5 for PE and 26.4 ± 3.1 for non-PE, p < 0.001). Moreover, all the domains of the FSFI scoring system were separately associated with PE. According to the mean FSFI scores, the 48.43% of women had sexual dysfunction in the non-PE group, and all women had sexual dysfunction in PE group.
Conclusion
PE is associated with female sexual dysfunction and all of the female sexual dysfunction domains, as determined by FSFI scores.

Similar content being viewed by others
References
Laumann EO, Paik A, Rosen RC (1999) Sexual dysfunction in the United States: prevalence and predictors. JAMA 281(6):537–544
Porst H, Montorsi F, Rosen RC, Gaynor L, Grupe S, Alexander J (2007) The premature ejaculation prevalence and attitudes (PEPA) survey: prevalence, comorbidities, and professional help-seeking. Eur Urol 51(3):816–823
Rowland DL, Patrick DL, Rothman M, Gagnon DD (2007) The psychological burden of premature ejaculation. J Urol 177(3):1065–1070
Symonds T, Roblin D, Hart K, Althof S (2003) How does premature ejaculation impact a man s life? J Sex Marital Ther 29(5):361–370
Limoncin E, Tomassetti M, Gravina GL, Ciocca G, Carosa E, Di Sante S, Gentile V, Mirone V, Montorsi F, Lenzi A, Jannini EA (2013) Premature ejaculation results in female sexual distress: standardization and validation of a new diagnostic tool for sexual distress. J Urol 189(5):1830–1835
Hisasue S, Kumamoto Y, Sato Y, Masumori N, Horita H, Kato R, Kobayashi K, Hashimoto K, Yamashita N, Itoh N (2005) Prevalence of female sexual dysfunction symptoms and its relationship to quality of life: a Japanese female cohort study. Urology 65(1):143–148
Nicolosi A, Glasser DB, Kim SC, Marumo K, Laumann EO (2005) Sexual behaviour and dysfunction and help-seeking patterns in adults aged 40–80 years in the urban population of Asian countries. BJU Int 95(4):609–614
McCabe MP, Sharlip ID, Lewis R, Atalla E, Balon R, Fisher AD, Laumann E, Lee SW, Segraves RT (2016) Incidence and prevalence of sexual dysfunction in women and men: a consensus statement from the fourth international consultation on sexual medicine 2015. J Sex Med 13(2):144–152
McCabe MP, Sharlip ID, Atalla E, Balon R, Fisher AD, Laumann E, Lee SW, Lewis R, Segraves RT (2016) Definitions of sexual dysfunctions in women and men: a consensus statement from the fourth international consultation on sexual medicine 2015. J Sex Med 13(2):135–143
Fisher WA, Eardley I, McCabe M, Sand M (2009) Erectile dysfunction (ED) is a shared sexual concern of couples I: couple conceptions of ED. J Sex Med 6(10):2746–2760
Hobbs K, Symonds T, Abraham L, May K, Morris MF (2008) Sexual dysfunction in partners of men with premature ejaculation. Int J Impot Res 20(5):512–517
Hayes RD, Bennett CM, Fairley CK, Dennerstein L (2006) What can prevalence studies tell us about female sexual difficulty and dysfunction? J Sex Med 3(4):589–595
Riley A, Riley E (2005) Premature ejaculation: presentation and associations. An audit of patients attending a sexual problems clinic. Int J Clin Pract 59(12):1482–1487
Jiann BP, Su CC, Yu CC, Wu TT, Huang JK (2009) Risk factors for individual domains of female sexual function. J Sex Med 6(12):3364–3375
Serefoglu EC, McMahon CG, Waldinger MD, Althof SE, Shindel A, Adaikan G, Becher EF, Dean J, Giuliano F, Hellstrom WJ, Giraldi A, Glina S, Incrocci L, Jannini E, McCabe M, Parish S, Rowland D, Segraves RT, Sharlip I, Torres LO (2014) An evidence-based unified definition of lifelong and acquired premature ejaculation: report of the second international society for sexual medicine ad hoc committee for the definition of premature ejaculation. Sex Med 2:41–59
Serefoglu EC, Cimen HI, Ozdemir AT, Symonds T, Berktas M, Balbay MD (2009) Turkish validation of the premature ejaculation diagnostic tool and its association with intravaginal ejaculatory latency time. Int J Impot Res 21:139–144
Rosen RC, Cappelleri JC, Smith MD, Lipsky J, Peña BM (1999) Development and evaluation of an abridged, 5- item version of the International Index of Erectile Function (IIEF-5) as a diagnostic tool for erectile dysfunction. Int J Impot Res 11:319–326
Beck AT, Ward CH, Mendelson M, Mock J, Erbaugh J (1962) An inventory for measuring depression. Arch Gen Psychiatry 4:561–571
Rosen R, Brown C, Heiman J, Leiblum S, Meston C, Shabsigh R, Ferguson D, D’Agostino R (2000) The female sexual function index (FSFI): a multidimensional self-report instrument for the assessment of female sexual function. J Sex Marital Ther 26:191–208
Cayan F, Dilek S, Akbay E, Cayan S (2008) Sexual function after surgery for stress urinary incontinence: vaginal sling versus Burch colposuspension. Arch Gynecol Obstet 277:31–36
Byers ES, Rehman U (2013) Sexual well-being. In: Tolman D, Diamond L (eds) APA handbook of sexuality and psychology. American Psychological Association, Washington, pp 317–337
Conaglen HM, O’Connor EJ, McCabe MP, Conaglen JV (2010) An investigation of sexual dysfunction in female partners of men with erectile dysfunction: how interviews expand on questionnaire responses. Int J Impot Res 22(6):355–362
Hartmann U, Schedlowski M, Krüger TH (2005) Cognitive and partner-related factors in rapid ejaculation: differences between dysfunctional and functional men. World J Urol 23(2):93–101
Burri A, Giuliano F, McMahon C, Porst H (2014) Female partner’s perception of premature ejaculation and its impact on relationship breakups, relationship quality, and sexual satisfaction. J Sex Med 11(9):2243–2255
McCabe MP, Sharlip ID, Lewis R, Atalla E, Balon R, Fisher AD, Laumann E, Lee SW, Segraves RT (2016) Risk factors for sexual dysfunction among women and men: a consensus statement from the Fourth International Consultation On Sexual Medicine 2015. J Sex Med 13(2):153–167
Burri A, Spector T (2011) Recent and lifelong sexual dysfunction in a female UK population sample: prevalence and risk factors. J Sex Med 8(9):2420–2430
Basson R, Berman J, Burnett A, Derogatis L, Ferguson D, Fourcroy J, Goldstein I, Graziottin A, Heiman J, Laan E, Leiblum S, Padma-Nathan H, Rosen R, Segraves K, Segraves RT, Shabsigh R, Sipski M, Wagner G, Whipple B (2000) Report of the international consensus development conference on female sexual dysfunction: definitions and classifications. J Urol 163(3):888–893
Dogan S, Dogan M (2008) The frequency of sexual dysfunctions in male partners of women with vaginismus in a Turkish sample. Int J Impot Res 20(2):218–221
Bronner G, Kitrey ND, Uziel N, Eli I, Raviv G, Ramon J, Elran E (2015) Correlation between premature ejaculation and female vaginal penetration difficulties. Int J Impot Res 27(4):152–156
Cayan S, Akbay E, Bozlu M, Canpolat B, Acar D, Ulusoy E (2004) The prevalance of female sexual dysfunction and potential risk factors that may impair sexual dysfunction in Turkish woman. Urol Int 72:52–57
Funding
This research received no specific grant from any funding agency in the public, commercial, or not-for-profit sectors.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflict of interest
The authors declare no conflict of interest.
Ethical approval
All procedures performed in studies involving human participants were in accordance with the ethical standards of the institutional and/or national research committee and with the 1964 Declaration of Helsinki and its later amendments or comparable ethical standards. The study was approved by the local committee of ethics.
Informed consent
Informed consent was obtained from all individual participants included in the study.
Rights and permissions
About this article
Cite this article
Canat, L., Değirmentepe, R.B., Atalay, H.A. et al. The relationship between female sexual function index domains and premature ejaculation. Int Urol Nephrol 50, 633–637 (2018). https://doi.org/10.1007/s11255-018-1832-y
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s11255-018-1832-y