Abstract
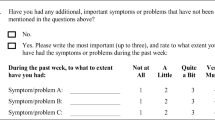
Patients with lung cancer experience considerable distress. Therefore, accurate methods for assessing distress and quality of life over time may play a key role for managing and evaluating palliative care. Alternatives to commonly used standardized questionnaires are individual measures. This study prospectively and retrospectively explored the concerns that 46 patients with inoperable lung cancer spontaneously reported as causing most distress close to diagnosis and 6 months later. Changes in content individually generated through a structured inductive freelisting were compared with EORTC-QLQ-C30+LC13 ratings. The results showed that patients perceived a wide variety of concerns as most distressing and that their concerns changed over time. Between 56 and 62% of these concerns were assessed by items included in the EORTC-QLQ-C30+LC13 questionnaires. Furthermore, patients’ reports of most distress from fatigue, pain and dyspnea were not always reflected in intensity ratings of comparable EORTC-QLQ-C30+LC13 items. These results indicate that items included in standardized measures are not always adequate to assess patients’ concerns, priorities and changes over time. In addition to standardized questionnaires, individualized measures may be useful in the clinical palliative setting for providing detailed information about the individual’s problems and prioritizations.
Similar content being viewed by others
Abbreviations
- HCS:
-
Health Care System
- LC:
-
Lung cancer
- QL:
-
Quality of life
References
Beckles, M. A., Spiro, S. G., Colice, G. L., & Rudd, R. M. (2003). Initial evaluation of the patient with lung cancer: symptoms, signs, laboratory tests, and paraneoplastic syndromes. Chest, 123(1 Suppl), 97S–104S.
Corner, J., Hopkinson, J., Fitzsimmons, D., Barclay, S., & Muers, M. (2005). Is late diagnosis of lung cancer inevitable? Interview study of patients’ recollections of symptoms before diagnosis. Thorax, 60(4), 314–319.
Koyi, H., Hillerdal, G., & Branden, E. (2002). Patient’s and doctors’ delays in the diagnosis of chest tumors. Lung Cancer, 35(1), 53–57.
Tishelman, C., Degner, L. F., Rudman, A., Bertilsson, K., Bond, R., Broberger, E., Doukkali, E., & Levealahti, H. (2005). Symptoms in patients with lung carcinoma: Distinguishing distress from intensity. Cancer, 104(9), 2013–2021.
Tishelman, C., Petersson, L.-M., Degner, L., & Sprangers, M. (in press). Symptom prevalence, intensity and association with distress in patients with inoperable lung cancer in relation to time of death. Journal of Clinical Oncology.
Distress Management [www.nccn.org].
Broberger, E., Tishelman, C., & von Essen, L. (2005). Discrepancies and similarities in how patients with lung cancer and their professional and family caregivers assess symptom occurrence and symptom distress. Journal of Pain and Symptom Management, 29(6), 572–583.
Tishelman, C., Degner, L. F., & Mueller, B. (2000). Measuring symptom distress in patients with lung cancer. A pilot study of experienced intensity and importance of symptoms. Cancer Nursing, 23(2), 82–90.
McCorkle, R., & Young, K. (1978). Development of a symptom distress scale. Cancer Nursing, 1(5), 373–378.
Aaronson, N. K., Ahmedzai, S., Bergman, B., Bullinger, M., Cull, A., Duez, N. J., Filiberti, A., Flechtner, H., Fleishman, S. B., de Haes, J. C. et al. (1993). The European Organization for Research and Treatment of Cancer QLQ-C30: a quality-of-life instrument for use in international clinical trials in oncology. Journal of National Cancer Institute, 85(5), 365–376.
Bergner, M., Bobbitt, R. A., Carter, W. B., & Gilson, B. S. (1981). The sickness impact profile: Development and final revision of a health status measure. Medical Care, 19(8), 787–805.
Sprangers, M. A., & Schwartz, C. E. (1999). Integrating response shift into health-related quality of life research: a theoretical model. Social Science & Medicine, 48(11), 1507–1515.
Ahmed, S., Mayo, N. E., Wood-Dauphinee, S., Hanley, J. A., & Cohen, S. R. (2005). Using the Patient Generated Index to evaluate response shift post-stroke. Qual Life Research, 14(10), 2247–2257.
O’Boyle, C., McGee, H., & Browne, J. (2000). Measuring response shift using the schedule for evaluation of individual quality of life. In Schwartz, C. E., &Sprangers, M. A. (Eds.), Adaptation to changing health: Response shift in quality of life research (pp. 123–136). Washington: American Psychological Association.
Bernard, H. R. (2006). Research methods in anthropology: Qualitative and quantitative approaches (4th ed.). Lanham: AltaMira Press.
Christian, P., Bentley, M. E., Pradhan, R., & West, K. P., Jr. (1998). An ethnographic study of night blindness “ratauni” among women in the Terai of Nepal. Social Science & Medicine, 46(7), 879–889.
Strauss, R. P., Sengupta, S., Kegeles, S., McLellan, E., Metzger, D., Eyre, S., Khanani, F., Emrick, C. B., & MacQueen, K. M. (2001). Willingness to volunteer in future preventive HIV vaccine trials: issues and perspectives from three, U.S. communities. Journal of Acquired Immune Deficiency Syndrome, 26(1), 63–71.
Bergman, B., Aaronson, N. K., Ahmedzai, S., Kaasa, S., & Sullivan, M. (1994). The EORTC QLQ-LC13: a modular supplement to the EORTC Core Quality of Life Questionnaire (QLQ-C30) for use in lung cancer clinical trials. EORTC Study Group on Quality of Life. European Journal of Cancer, 30A(5), 635–642.
Montazeri, A., Gillis, C. R., & McEwen, J. (1998). Quality of life in patients with lung cancer: a review of literature from 1970 to 1995. Chest, 113(2), 467–481.
Michelson, H., Bolund, C., Nilsson, B., & Brandberg, Y. (2000). Health-related quality of life measured by the EORTC QLQ-C30—reference values from a large sample of Swedish population. Acta Oncology, 39(4), 477–484.
McCorkle, R., & Quint-Benoliel, J. (1983). Symptom distress, current concerns and mood disturbance after diagnosis of life-threatening disease. Social Science & Medicine, 17(7), 431–438.
Carver, C. S., & Scheier, M. F. (2000). Scaling back goals and recalibration of the affect system are processes in normal adaptive self-regulation: understanding ‘response shift’ phenomena. Soc Sci Med, 50(12), 1715–1722.
Sharpe, L., & Curran, L. (2006). Understanding the process of adjustment to illness. Soc Sci Med, 62(5), 1153–1166.
Higginson, I., Priest, P., & McCarthy, M. (1994). Are bereaved family members a valid proxy for a patient’s assessment of dying? Soc Sci Med, 38(4), 553–557.
Sharpe, L., Butow, P., Smith, C., McConnell, D., & Clarke, S. (2005). Changes in quality of life in patients with advanced cancer: evidence of response shift and response restriction. Journal of psychosomatic research, 58(6), 497–504.
Stromgren, A. S., Sjogren, P., Goldschmidt, D., Petersen, M. A., Pedersen, L., & Groenvold, M. (2005). Symptom priority and course of symptomatology in specialized palliative care. Journal of pain and symptom management, 31(3), 199–206.
Wagner, J. A. (2005). Response shift and glycemic control in children with diabetes. Health Qual Life Outcomes, 3(1), 38.
Bradburn, N. M., Rips, L. J., & Shevell, S. K. (1987). Answering autobiographical questions: The impact of memory and inference on surveys. Science, 236(4798), 157–161.
Henry, B., Moffitt, T. E., Caspi, A., Langley, J., & Silva, P. A. (1994). On the “Rembrance of Things Past”: A longitudinal evaluation of the retrospective method. Psychological Assessment, 6(2), 92–101.
Herdman, M. (2000). The measurement of health related quality of life. Medicina Clinica (Barc), 114(Suppl 3), 22–25.
Acknowledgements
The authors thank the following sources for financial support: The Swedish Cancer Society, The Swedish Heart-Lung Foundation, The Swedish Foundation for Health Care Sciences and Allergy Research, The Research Board for Health Caring Sciences at Karolinska Institutet, and the Department of Neurobiology, Care Sciences and Society at Karolinska Institutet. We also thank Coop Sweden for their support. We would like to express our sincere thanks to Kristina Bertilsson and the other research team colleagues Helena Leveälahti, Ann Rudman and Joakim Öhlén for helpful input and discussions about categorization.
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
About this article
Cite this article
Broberger, E., Tishelman, C., von Essen, L. et al. Spontaneous reports of most distressing concerns in patients with inoperable lung cancer: at present, in retrospect and in comparison with EORTC-QLQ-C30+LC13. Qual Life Res 16, 1635–1645 (2007). https://doi.org/10.1007/s11136-007-9266-5
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s11136-007-9266-5