Abstract
Purpose
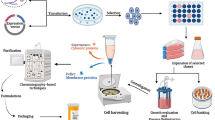
The inhibition of myostatin - a member of the transforming growth factor (TGF–β) family - drives regeneration of functional skeletal muscle tissue. We developed a bioresponsive drug delivery system (DDS) linking release of a myostatin inhibitor (MI) to inflammatory flares of myositis to provide self-regulated MI concentration gradients within tissues of need.
Methods
A protease cleavable linker (PCL) – responding to MMP upregulation – is attached to the MI and site-specifically immobilized on microparticle surfaces.
Results
The PCL disintegrated in a matrix metalloproteinase (MMP) 1, 8, and particularly MMP-9 concentration dependent manner, with MMP-9 being an effective surrogate biomarker correlating with the activity of myositis. The bioactivity of particle-surface bound as well as released MI was confirmed by luciferase suppression in stably transfected HEK293 cells responding to myostatin induced SMAD phosphorylation.
Conclusions
We developed a MMP-responsive DDS for MI delivery responding to inflammatory flare of a diseased muscle matching the kinetics of MMP-9 upregulation, with MMP-9 kinetics matching (patho-) physiological myostatin levels.
ᅟ

Schematic illustration of the matrix metalloproteinase responsive delivery system responding to inflammatory flares of muscle disease. The protease cleavable linker readily disintegrates upon entry into the diseased tissue, therby releasing the mystatin inhibitor.





Similar content being viewed by others
Abbreviations
- ActRIIB:
-
Activin receptor IIB
- au:
-
Arbitrary units
- BCA:
-
Bicinchoninic acid
- BSA:
-
Bovine serum albumin
- CuAAC:
-
Copper(I)-catalyzed azide-alkyne cycloaddition
- DBCO:
-
Dibenzocyclooctyne
- DDS:
-
Drug delivery system
- DM:
-
Differentiation medium
- DMD:
-
Duchenne muscular dystrophy
- ECM:
-
Extracellular matrix
- EDC:
-
1-Ethyl-3-(3dimethylaminopropyl)carbodiimide
- Fmoc:
-
N-α-(9-Fluorenylmethyloxycarbonyl)
- GDF-8:
-
Growth differentiation factor 8
- HPLC:
-
High-performance liquid chromatography
- IGF-I:
-
Insulin-like growth factor I
- IL-1β:
-
Interleukin 1β
- MALDI-MS:
-
Matrix-assisted laser desorption ionization mass spectrometry
- MI:
-
Myostatin inhibitor
- MMP:
-
Matrix metalloproteinase
- MSTN:
-
Myostatin
- MyHC:
-
Myosin heavy chain
- NF-kB:
-
Nuclear factor-kappa B
- NHS:
-
N-hydroxysuccinimide
- PCL:
-
Protease cleavable linker
- PEG:
-
Polyethylene glycol
- PMMA:
-
Poly(methyl methacrylate)
- RLU:
-
Relative light unit
- RT-PCR:
-
Real time polymerase chain reaction
- SBE:
-
SMAD binding element
- SC:
-
Satellite cell
- SPAAC:
-
Strain-promoted azide-alkyne cycloaddition
- SPPS:
-
Solid phase peptide synthesis
- TG:
-
Transglutaminase (human, fXIIIa)
- TGF–β:
-
Transforming growth factor beta
- THPTA:
-
Tris(3-hydroxypropyltriazolylmethyl)amine
- TNF-α:
-
Tumor necrosis factor α
References
Roubenoff R, Hughes VA. Sarcopenia: current concepts. J Gerontol Ser Biol Sci Med Sci. 2000;55(12):M716–24.
Egerman MA, Glass DJ. Signaling pathways controlling skeletal muscle mass. Crit Rev Biochem Mol Biol. 2014;49(1):59–68.
Trendelenburg AU, Meyer A, Rohner D, Boyle J, Hatakeyama S, Glass DJ. Myostatin reduces Akt/TORC1/p70S6K signaling, inhibiting myoblast differentiation and myotube size. Am J Phys Cell Phys. 2009;296(6):C1258–70.
Cohen S, Nathan JA, Goldberg AL. Muscle wasting in disease: molecular mechanisms and promising therapies. Nat Rev Drug Discov. 2015;14(1):58–74.
Tsuchida K, Nakatani M, Ueztjmi A, Murakami T, Cui XL. Signal transduction pathway through activin receptors as a therapeutic target of musculoskeletal diseases and cancer. Endocr J. 2008;55(1):11–21.
Sriram S, Subramanian S, Juvvuna PK, Ge X, Lokireddy S, McFarlane CD, et al. Myostatin augments muscle-specific ring finger protein-1 expression through an NF-kB independent mechanism in SMAD3 null muscle. Mol Endocrinol. 2014;28(3):317–30.
Yamaki T, Wu C-L, Gustin M, Lim J, Jackman RW, Kandarian SC. Rel A/p65 is required for cytokine-induced myotube atrophy. Am J Phys Cell Phys. 2012;303(2):C135–42.
Reid MB, Li YP. Tumor necrosis factor-alpha and muscle wasting: a cellular perspective. Respir Res. 2001;2(5):269–72.
Lach-Trifilieff E, Minetti GC, Sheppard K, Ibebunjo C, Feige JN, Hartmann S, et al. An antibody blocking activin type II receptors induces strong skeletal muscle hypertrophy and protects from atrophy. Mol Cell Biol. 2014;34(4):606–18.
Gilson H, Schakman O, Kalista S, Lause P, Tsuchida K, Thissen J-P. Follistatin induces muscle hypertrophy through satellite cell proliferation and inhibition of both myostatin and activin. Am J Physiol Endocrinol Metab. 2009;297(1):E157–64.
Latres E, Pangilinan J, Miloscio L, Bauerlein R, Na E, Potocky TB, et al. Myostatin blockade with a fully human monoclonal antibody induces muscle hypertrophy and reverses muscle atrophy in young and aged mice. Skelet Muscle. 2015;5.
Han H, Min H, Boone TC, inventors; Amgen Inc, assignee. Binding agents which inhibit myostatin patent #1581649, Priority claimed as of 20.12.02/USP435923. Apr 19 2011.
Schoser BGH, Blottner D, Stuerenburg HJ. Matrix metalloproteinases in inflammatory myopathies: enhanced immunoreactivity near atrophic myofibers. Acta Neurol Scand. 2002;105(4):309–13.
Fukushima K, Nakamura A, Ueda H, Yuasa K, Yoshida K, Takeda Si, et al. Activation and localization of matrix metalloproteinase-2 and-9 in the skeletal muscle of the muscular dystrophy dog (CXMDJ). Bmc Musculoskeletal Disorders. 2007;8.
Brenner DA, Ohara M, Angel P, Chojkier M, Karin M. Prolonged activation of jun and collagenase genes by tumor-necrosis factor-alpha. Nature. 1989;337(6208):661–3.
Kherif S, Lafuma C, Dehaupas M, Lachkar S, Fournier JG, Verdiere-Sahuque M, et al. Expression of matrix metalloproteinases 2 and 9 in regenerating skeletal muscle: a study in experimentally injured and mdx muscles. Dev Biol. 1999;205(1):158–70.
McCroskery S, Thomas M, Platt L, Hennebry A, Nishimura T, McLeay L, et al. Improved muscle healing through enhanced regeneration and reduced fibrosis in myostatin-null mice. J Cell Sci. 2005;118(15):3531–41.
Nadarajah VD, van Putten M, Chaouch A, Garrood P, Straub V, Lochmueller H, et al. Serum matrix metalloproteinase-9 (MMP-9) as a biomarker for monitoring disease progression in Duchenne muscular dystrophy (DMD). Neuromuscul Disord. 2011;21(8):569–78.
Lutolf MP, Lauer-Fields JL, Schmoekel HG, Metters AT, Weber FE, Fields GB, et al. Synthetic matrix metalloproteinase-sensitive hydrogels for the conduction of tissue regeneration: engineering cell-invasion characteristics. Proc Natl Acad Sci U S A. 2003;100(9):5413–8.
Steinhagen M, Hoffmeister P-G, Nordsieck K, Hoetzel R, Baumann L, Hacker MC, et al. Matrix metalloproteinase 9 (MMP-9) mediated release of MMP-9 resistant stromal cell-derived factor 1 alpha (SDF-1 alpha) from surface modified polymer films. ACS Appl Mater Interfaces. 2014;6(8):5891–9.
van Rijt SH, Boeluekbas DA, Argyo C, Datz S, Lindner M, Eickelberg O, et al. Protease-mediated release of chemotherapeutics from mesoporous silica nanoparticles to ex vivo human and mouse lung tumors. ACS Nano. 2015;9(3):2377–89.
Pompe T, Salchert K, Alberti K, Zandstra P, Werner C. Immobilization of growth factors on solid supports for the modulation of stem cell fate. Nat Protoc. 2010;5(6):1042–50.
Ducry L, Stump B. Antibody-drug conjugates: linking cytotoxic payloads to monoclonal antibodies. Bioconjug Chem. 2010;21(1):5–13.
Zhao H, Heusler E, Jones G, Li L, Werner V, Germershaus O, et al. Decoration of silk fibroin by click chemistry for biomedical application. J Struct Biol. 2014;186(3):420–30.
Luehmann T, Jones G, Gutmann M, Rybak J-C, Nickel J, Rubini M, et al. Bio-orthogonal immobilization of fibroblast growth factor 2 for spatial controlled cell proliferation. ACS Biomater Sci Eng. 2015;1(9):740–6.
Eger S, Scheffner M, Marx A, Rubini M. Synthesis of defined ubiquitin dimers. J Am Chem Soc. 2010;132(46):16337–9.
Gutmann M, Memmel E, Braun AC, Seibel J, Meinel L, Lühmann T. Biocompatible azide–alkyne “click” reactions for surface decoration of glyco-engineered cells. ChemBioChem. 2016;17(9):866–75.
Coin I, Beyermann M, Bienert M. Solid-phase peptide synthesis: from standard procedures to the synthesis of difficult sequences. Nat Protoc. 2007;2(12):3247–56.
Schense JC, Hubbell JA. Cross-linking exogenous bifunctional peptides into fibrin gels with factor XIIIa. Bioconjug Chem. 1999;10(1):75–81.
Nagase H, Fields GB. Human matrix metalloproteinase specificity studies using collagen sequence-based synthetic peptides. Biopolymers. 1996;40(4):399–416.
Alland C, Moreews F, Boens D, Carpentier M, Chiusa S, Lonquety M, et al. RPBS: a web resource for structural bioinformatics. Nucleic Acids Res. 2005;33:W44–9.
Pettersen EF, Goddard TD, Huang CC, Couch GS, Greenblatt DM, Meng EC, et al. UCSF chimera - a visualization system for exploratory research and analysis. J Comput Chem. 2004;25(13):1605–12.
Schagger H. Tricine-SDS-PAGE. Nat Protoc. 2006;1(1):16–22.
Jonk LJC, Itoh S, Heldin CH, ten Dijke P, Kruijer W. Identification and functional characterization of a Smad binding element (SBE) in the JunB promoter that acts as a transforming growth factor-beta, activin, and bone morphogenetic protein-inducible enhancer. J Biol Chem. 1998;273(33):21145–52.
Ebert R, Jovanovic M, Ulmer M, Schneider D, Meissner-Weigl J, Adamski J, et al. Down-regulation by nuclear factor kappa B of human 25-hydroxyvitamin D-3 1 alpha-hydroxylase promoter. Mol Endocrinol. 2004;18(10):2440–50.
Schmittgen TD, Livak KJ. Analyzing real-time PCR data by the comparative CT method. Nat Protoc. 2008;3(6):1101–8.
O’Connell JP, Willenbrock F, Docherty AJP, Eaton D, Murphy G. Analysis of the role of the COOH-terminal domain in the activation, proteolytic activity, and tissue inhibitor of metalloproteinase interactions of gelatinase B. J Biol Chem. 1994;269(21):14967–73.
Staros JV, Wright RW, Swingle DM. Enhancement by N-hydroxysulfosuccinimide of water-soluble carbodiimide-mediated coupling reactions. Anal Biochem. 1986;156(1):220–2.
Lienemann PS, Karlsson M, Sala A, Wischhusen HM, Weber FE, Zimmermann R, et al. A versatile approach to engineering biomolecule-presenting cellular microenvironments. Adv Healthcare Mater. 2013;2(2):292–6.
Luehmann T, Haenseler P, Grant B, Hall H. The induction of cell alignment by covalently immobilized gradients of the 6th Ig-like domain of cell adhesion molecule L1 in 3D-fibrin matrices. Biomaterials. 2009;30(27):4503–12.
Huisgen R. Kinetics and mechanism of 1,3-dipolar cycloadditions. Angew Chem Int Ed Engl. 1963;2(11):633–45.
Agard NJ, Prescher JA, Bertozzi CR. A strain-promoted 3 + 2 azide-alkyne cycloaddition for covalent modification of blomolecules in living systems. J Am Chem Soc. 2004;126(46):15046–7.
Lutz J-F, Zarafshani Z. Efficient construction of therapeutics, bioconjugates, biomaterials and bioactive surfaces using azide-alkyne “click” chemistry. Adv Drug Deliv Rev. 2008;60(9):958–70.
Debets MF, van Berkel SS, Schoffelen S, Rutjes FPJT, van Hest JCM, van Delft FL. Aza-dibenzocyclooctynes for fast and efficient enzyme PEGylation via copper-free (3 + 2) cycloaddition. Chem Commun. 2010;46(1):97–9.
Chargé SBP, Rudnicki MA. Cellular and molecular regulation of muscle regeneration. Physiol Rev. 2004;84(1):209–38.
Bikle DD, Tahimic C, Chang W, Wang Y, Philippou A, Barton ER. Role of IGF-I signaling in muscle bone interactions. Bone. 2015;80:79–88.
Bursac N, Juhas M, Rando TA. Synergizing engineering and biology to treat and model skeletal muscle injury and disease. In: Yarmush ML, editor. Annual review of biomedical engineering, Vol 17. Annual Review of Biomedical Engineering. 172015. p. 217–42.
ACKNOWLEDGMENTS AND DISCLOSURES
We thank Petra Knaus (Freie Universität Berlin, Germany) for providing us with the pGl3ti-SBE constructs and Melanie Krug for excellent technical assistance. We thank Dr. Joachim Nickel for providing C2C12 myoblast cells. The financial support of the Bavarian research foundation (grant # AZ-1044-12 ‘FORMOsA’) and the Deutsche Forschungsgemeinschaft (DFG; ME 3820/3-1) are gratefully acknowledged. H.G. is full time associate of Gilyos GmbH.
Author information
Authors and Affiliations
Corresponding author
Electronic supplementary material
Below is the link to the electronic supplementary material.
ESM 1
(PDF 779 kb)
Rights and permissions
About this article
Cite this article
Braun, A.C., Gutmann, M., Ebert, R. et al. Matrix Metalloproteinase Responsive Delivery of Myostatin Inhibitors. Pharm Res 34, 58–72 (2017). https://doi.org/10.1007/s11095-016-2038-6
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s11095-016-2038-6