Abstract
Purpose
Gene delivery from biomaterials has become an important tool in tissue engineering. The purpose of this study was to generate a gene vector-doted fibrin glue as a versatile injectable implant to be used in gene therapy supported tissue regeneration.
Methods
Copolymer-protected polyethylenimine(PEI)-DNA vectors (COPROGs), naked DNA and PEI-DNA were formulated with the fibrinogen component of the fibrin glue TISSUCOL® and lyophilized. Clotting parameters upon rehydration and thrombin addition were measured, vector release from fibrin clots was determined. Structural characterizations were carried out by electron microscopy. Reporter and growth factor gene delivery to primary keratinocytes and chondrocytes in vitro was examined. Finally,chondrocyte colonized clots were tested for their potency in cartilage regeneration in a osteochondral defect model.
Results
The optimized glue is based on the fibrinogen component of TISSUCOL®, a fibrin glue widely used in the clinics, co-lyophilized with copolymer-protected polyethylenimine(PEI)- DNA vectors (COPROGs). This material, when rehydrated, forms vector-containing clots in situ upon thrombin addition and is suitable to mediate growth factor gene delivery to primary keratinocytes and primary chondrocytes admixed before clotting. Unprotected PEI-DNA in the same setup was comparatively unsuitable for clot formation while naked DNA was ineffective in transfection. Naked DNA was released rapidly from fibrin clots (>70% within the first seven days) in contrast to COPROGs which remained tightly immobilized over extended periods of time (0.29% release per day). Electron microscopy of chondrocytecolonized COPROG-clots revealed avid endocytotic vector uptake. In situ BMP-2 gene transfection and subsequent expression in chondrocytes grown in COPROG clots resulted in the upregulation of alkaline phosphatase expression and increased extracellular matrix formation in vitro. COPROG-fibrinogen preparations with admixed autologous chondrocytes when clotted in situ in osteochondral defects in the patellar grooves of rabbit femura gave rise to luciferase reporter gene expression detectable for two weeks (n=3 animals per group). However, no significant improvement in cartilage formation in osteochondral defects filled with autologous chondrocytes in BMP-2-COPROG clots was achieved in comparison to controls (n=8 animals per group).
Conclusions
COPROGs co-lyophilized with fibrinogen are a simple basis for an injectable fibrin gluebased gene-activated matrix. The preparation can be used is complete analogy to fibrin glue preparations that are used in the clinics. However, further improvements in transgene expression levels and persistence are required to yield cartilage regeneration in the osteochondral defect model chosen in this study.










Similar content being viewed by others
References
G. E. Friedlaender. Osteogenic protein-1 in treatment of tibial nonunions: current status. Surg Technol Int. 13:249–252 (2004).
A. Valentin-Opran, J. Wozney, C. Csimma, L. Lilly, and G. E. Riedel. Clinical evaluation of recombinant human bone morphogenetic protein-2. Clin. Orthop. Relat. Res. 395:110–120 (2002). doi:10.1097/00003086-200202000-00011.
J. Bonadio, E. Smiley, P. Patil, and S. Goldstein. Localized, direct plasmid gene delivery in vivo: prolonged therapy results in reproducible tissue regeneration. Nat. Med. 5:753–759 (1999). doi:10.1038/10473.
K. Y. Lee, M. C. Peters, K. W. Anderson, and D. J. Mooney. Controlled growth factor release from synthetic extracellular matrices. Nature. 408:998–1000 (2000). doi:10.1038/35044106.
R. R. Chen, and D. J. Mooney. Polymeric growth factor delivery strategies for tissue engineering. Pharm. Res. 20:1103–1112 (2003). doi:10.1023/A:1025034925152.
H. Deppe, A. Stemberger, and M. Hillemanns. Effects of osteopromotive and anti-infective membranes on bone regeneration: an experimental study in rat mandibular defects. Int. J. Oral. Maxillofac. Implants. 18:369–376 (2003).
G. Schmidmaier, B. Wildemann, T. Gabelein, J. Heeger, F. Kandziora, N. P. Haas, and M. Raschke. Synergistic effect of IGF-I and TGF-beta1 on fracture healing in rats: single versus combined application of IGF-I and TGF-beta1. Acta Orthop. Scand. 74:604–610 (2003). doi:10.1080/00016470310018036.
H. Gollwitzer, P. Thomas, P. Diehl, E. Steinhauser, B. Summer, S. Barnstorf, L. Gerdesmeyer, W. Mittelmeier, and A. Stemberger. Biomechanical and allergological characteristics of a biodegradable poly(D,L-lactic acid) coating for orthopaedic implants. J. Orthop. Res. 23:802–809 (2005). doi:10.1016/j.orthres.2005.02.003.
D. J. Mooney, T. Boontheekul, R. Chen, and K. Leach. Actively regulating bioengineered tissue and organ formation. Orthod. Craniofac. Res. 8:141–144 (2005). doi:10.1111/j.1601-6343.2005.00327.x.
L. Cao, and D. J. Mooney. Spatiotemporal control over growth factor signaling for therapeutic neovascularization. Adv. Drug Del. Rev. 59:1340–1350 (2007). doi:10.1016/j.addr.2007.08.012.
L. D. Shea, E. Smiley, J. Bonadio, and D. J. Mooney. DNA delivery from polymer matrices for tissue engineering. Nat. Biotechnol. 17:551–554 (1999). doi:10.1038/9853.
J. Bonadio. Tissue engineering via local gene delivery: update and future prospects for enhancing the technology. Adv. Drug Del. Rev. 44:185–194 (2000). doi:10.1016/S0169-409X(00)00094-6.
L. De Laporte, and L. D. Shea. Matrices and scaffolds for DNA delivery in tissue engineering. Adv. Drug Del. Rev. 59:292–307 (2007). doi:10.1016/j.addr.2007.03.017.
F. Scherer, U. Schillinger, U. Putz, A. Stemberger, and C. Plank. Nonviral vector loaded collagen sponges for sustained gene delivery in vitro and in vivo. J. Gene Med. 4:634–643 (2002). doi:10.1002/jgm.298.
D. Finsinger, J. S. Remy, P. Erbacher, C. Koch, and C. Plank. Protective copolymers for nonviral gene vectors: synthesis, vector characterization and application in gene delivery. Gene Ther. 7:1183–1192 (2000). doi:10.1038/sj.gt.3301227.
C. Rudolph, U. Schillinger, C. Plank, A. Gessner, P. Nicklaus, R. Muller, and J. Rosenecker. Nonviral gene delivery to the lung with copolymer-protected and transferrin-modified polyethylenimine. Biochim. Biophys. Acta. 1573:75–83 (2002).
C. Andree, M. Voigt, A. Wenger, T. Erichsen, K. Bittner, D. Schaefer, K. J. Walgenbach, J. Borges, R. E. Horch, E. Eriksson, and G. B. Stark. Plasmid gene delivery to human keratinocytes through a fibrin-mediated transfection system. Tissue Eng. 7:757–766 (2001). doi:10.1089/107632701753337708.
A. Jozkowicz, A. Fugl, J. Nanobashvili, C. Neumayer, J. Dulak, D. Valentini, P. Funovics, P. Polterauer, H. Redl, and I. Huk. Delivery of high dose VEGF plasmid using fibrin carrier does not influence its angiogenic potency. Int. J. Artif. Organs. 26:161–169 (2003).
K. L. Christman, Q. Fang, M. S. Yee, K. R. Johnson, R. E. Sievers, and R. J. Lee. Enhanced neovasculature formation in ischemic myocardium following delivery of pleiotrophin plasmid in a biopolymer. Biomaterials. 26:1139–1144 (2005). doi:10.1016/j.biomaterials.2004.04.025.
D. Trentin, H. Hall, S. Wechsler, and J. A. Hubbell. Peptide-matrix-mediated gene transfer of an oxygen-insensitive hypoxia-inducible factor-1alpha variant for local induction of angiogenesis. Proc. Natl. Acad. Sci. USA. 103:2506–2511 (2006). doi:10.1073/pnas.0505964102.
J. M. Saul, M. P. Linnes, B. D. Ratner, C. M. Giachelli, and S. H. Pun. Delivery of non-viral gene carriers from sphere-templated fibrin scaffolds for sustained transgene expression. Biomaterials. 28:4705–4716 (2007). doi:10.1016/j.biomaterials.2007.07.026.
A. Breen, P. Dockery, T. O’Brien, and A. Pandit. Fibrin scaffold promotes adenoviral gene transfer and controlled vector delivery. J Biomed Mater Res A. In press (2008).
A. Breen, P. Strappe, A. Kumar, T. O’Brien, and A. Pandit. Optimization of a fibrin scaffold for sustained release of an adenoviral gene vector. J. Biomed. Mater. Res. A. 78:702–708 (2006). doi:10.1002/jbm.a.30735.
A. M. Breen, P. Dockery, T. O’Brien, and A. S. Pandit. The use of therapeutic gene eNOS delivered via a fibrin scaffold enhances wound healing in a compromised wound model. Biomaterials. 29:3143–3151 (2008). doi:10.1016/j.biomaterials.2008.04.020.
C. A. Dunn, Q. Jin, M. Taba Jr., R. T. Franceschi, R. Bruce Rutherford, and W. V. Giannobile. BMP gene delivery for alveolar bone engineering at dental implant defects. Mol. Ther. 11:294–299 (2005). doi:10.1016/j.ymthe.2004.10.005.
M. J. Escamez, M. Carretero, M. Garcia, L. Martinez-Santamaria, I. Mirones, B. Duarte, A. Holguin, E. Garcia, V. Garcia, A. Meana, J. L. Jorcano, F. Larcher, and M. Del Rio. Assessment of optimal virus-mediated growth factor gene delivery for human cutaneous wound healing enhancement. J. Invest. Dermatol. 128:1565–1575 (2008). doi:10.1038/sj.jid.5701217.
R. M. Schek, E. N. Wilke, S. J. Hollister, and P. H. Krebsbach. Combined use of designed scaffolds and adenoviral gene therapy for skeletal tissue engineering. Biomaterials. 27:1160–1166 (2006). doi:10.1016/j.biomaterials.2005.07.029.
F. Teraishi, T. Umeoka, T. Saito, T. Tsukagoshi, N. Tanaka, and T. Fujiwara. A novel method for gene delivery and expression in esophageal epithelium with fibrin glues containing replication-deficient adenovirus vector. Surg. Endosc. 17:1845–1848 (2003). doi:10.1007/s00464-003-8146-5.
L. Wan, D. Li, and Q. Wu. Perivenous application of fibrin glue as external support enhanced adventitial adenovirus transfection in rabbit model. J. Surg. Res. 135:312–316 (2006). doi:10.1016/j.jss.2006.02.056.
C. Andree, W. F. Swain, C. P. Page, M. D. Macklin, J. Slama, D. Hatzis, and E. Eriksson. In vivo transfer and expression of a human epidermal growth factor gene accelerates wound repair. Proc. Natl. Acad. Sci. U.S.A. 91:12188–12192 (1994). doi:10.1073/pnas.91.25.12188.
J. Terebesi, K. Y. Kwok, and K. G. Rice. Iodinated plasmid DNA as a tool for studying gene delivery. Anal. Biochem. 263:120–123 (1998). doi:10.1006/abio.1998.2834.
O. Mykhaylyk, Y. S. Antequera, D. Vlaskou, and C. Plank. Generation of magnetic nonviral gene transfer agents and magnetofection in vitro. Nat. Protoc. 2:2391–2411 (2007). doi:10.1038/nprot.2007.352.
M. Arlt, C. Kopitz, C. Pennington, K. L. Watson, H. W. Krell, W. Bode, B. Gansbacher, R. Khokha, D. R. Edwards, and A. Kruger. Increase in gelatinase-specificity of matrix metalloproteinase inhibitors correlates with antimetastatic efficacy in a T-cell lymphoma model. Cancer Res. 62:5543–5550 (2002).
P. Mainil-Varlet, T. Aigner, M. Brittberg, P. Bullough, A. Hollander, E. Hunziker, R. Kandel, S. Nehrer, K. Pritzker, S. Roberts, and E. Stauffer. Histological assessment of cartilage repair: a report by the Histology Endpoint Committee of the International Cartilage Repair Society (ICRS). J. Bone Joint Surg. Am. 85-A(Suppl 2):45–57 (2003).
T. Tischer, S. Milz, M. Maier, M. Schieker, and M. Benjamin. An immunohistochemical study of the rabbit suprapatella, a sesamoid fibrocartilage in the quadriceps tendon containing aggrecan. J. Histochem. Cytochem. 50:955–960 (2002).
S. Milz, M. Benjamin, and R. Putz. Molecular parameters indicating adaptation to mechanical stress in fibrous connective tissue. Adv. Anat. Embryol. Cell Biol. 178:1–71 (2005). doi:10.1007/3-540-27832-X_1.
J. P. Luzio, P. R. Pryor, and N. A. Bright. Lysosomes: fusion and function. Nat. Rev. Mol. Cell Biol. 8:622–632 (2007). doi:10.1038/nrm2217.
S. Mayor, and R. E. Pagano. Pathways of clathrin-independent endocytosis. Nat. Rev. Mol. Cell Biol. 8:603–612 (2007). doi:10.1038/nrm2216.
J. Fang, Y. Y. Zhu, E. Smiley, J. Bonadio, J. P. Rouleau, S. A. Goldstein, L. K. McCauley, B. L. Davidson, and B. J. Roessler. Stimulation of new bone formation by direct transfer of osteogenic plasmid genes. Proc. Natl. Acad. Sci. U.S.A. 93:5753–5758 (1996). doi:10.1073/pnas.93.12.5753.
C. Perka, R. S. Spitzer, K. Lindenhayn, M. Sittinger, and O. Schultz. Matrix-mixed culture: new methodology for chondrocyte culture and preparation of cartilage transplants. J. Biomed. Mater. Res. 49:305–311 (2000)doi:10.1002/(SICI)1097-4636(20000305)49:3<305::AID-JBM2>3.0.CO;2-9.
K. Isoda, and S. Saito. In vitro and in vivo fibrochondrocyte growth behavior in fibrin gel: an immunohistochemical study in the rabbit. Am. J. Knee Surg. 11:209–216 (1998).
K. Gelse, and H. Schneider. Ex vivo gene therapy approaches to cartilage repair. Adv. Drug Del. Rev. 58:259–284 (2006). doi:10.1016/j.addr.2006.01.019.
K. Gelse, K. von der Mark, T. Aigner, J. Park, and H. Schneider. Articular cartilage repair by gene therapy using growth factor-producing mesenchymal cells. Arthritis Rheum. 48:430–441 (2003). doi:10.1002/art.10759.
A. J. Chu, S. Beydoun, S. T. Mathews, and J. Hoang. Novel anticoagulant polyethylenimine: inhibition of thrombin-catalyzed fibrin formation. Arch. Biochem. Biophys. 415:101–108 (2003)doi:10.1016/S0003-9861(03)00216-9.
D. Trentin, J. Hubbell, and H. Hall. Non-viral gene delivery for local and controlled DNA release. J. Control Release. 102:263–275 (2005). doi:10.1016/j.jconrel.2004.09.029.
P. Erbacher, T. Bettinger, P. Belguise-Valladier, S. Zou, J. L. Coll, J. P. Behr, and J. S. Remy. Transfection and physical properties of various saccharide, poly(ethylene glycol), and antibody-derivatized polyethylenimines (PEI). J. Gene Med. 1:210–222 (1999). doi:10.1002/(SICI)1521-2254(199905/06)1:3<210::AID-JGM30>3.0.CO;2-U.
P. Erbacher, T. Bettinger, E. Brion, J. L. Coll, C. Plank, J. P. Behr, and J. S. Remy. Genuine DNA/polyethylenimine (PEI) complexes improve transfection properties and cell survival. J. Drug Targ. 12:223–236 (2004). doi:10.1080/10611860410001723487.
A. Kichler, C. Leborgne, and O. Danos. Dilution of reporter gene with stuffer DNA does not alter the transfection efficiency of polyethylenimines. J. Gene Med. 7:1459–1467 (2005). doi:10.1002/jgm.805.
S. Vogt, P. Ueblacker, C. Geis, B. Wagner, G. Wexel, T. Tischer, A. Kruger, C. Plank, M. Anton, V. Martinek, A. B. Imhoff, and B. Gansbacher. Efficient and stable gene transfer of growth factors into chondrogenic cells and primary articular chondrocytes using a VSV.G pseudotyped retroviral vector. Biomaterials. 29:1242–1249 (2008). doi:10.1016/j.biomaterials.2007.11.013.
K. Gelse, Q. J. Jiang, T. Aigner, T. Ritter, K. Wagner, E. Poschl, K. von der Mark, and H. Schneider. Fibroblast-mediated delivery of growth factor complementary DNA into mouse joints induces chondrogenesis but avoids the disadvantages of direct viral gene transfer. Arthritis Rheum. 44:1943–1953 (2001)doi:10.1002/1529-0131(200108)44:8<1943::AID-ART332>3.0.CO;2-Z.
P. Ueblacker, B. Wagner, S. Vogt, G. Salzmann, G. Wexel, A. Kruger, C. Plank, T. Brill, K. Specht, T. Hennig, U. Schillinger, A. B. Imhoff, V. Martinek, and B. Gansbacher. In vivo analysis of retroviral gene transfer to chondrocytes within collagen scaffolds for the treatment of osteochondral defects. Biomaterials. 28:4480–4487 (2007). doi:10.1016/j.biomaterials.2007.06.027.
S. C. Hyde, I. A. Pringle, S. Abdullah, A. E. Lawton, L. A. Davies, A. Varathalingam, G. Nunez-Alonso, A. M. Green, R. P. Bazzani, S. G. Sumner-Jones, M. Chan, H. Li, N. S. Yew, S. H. Cheng, A. C. Boyd, J. C. Davies, U. Griesenbach, D. J. Porteous, D. N. Sheppard, F. M. Munkonge, E. W. Alton, and D. R. Gill. CpG-free plasmids confer reduced inflammation and sustained pulmonary gene expression. Nat. Biotechnol. 26:549–551 (2008). doi:10.1038/nbt1399.
Acknowledgements
This work was supported by the Deutsche Forschungsgemeinschaft (Pl 281/1) and Baxter AG, Vienna, Austria, and the German Federal Ministry of Education and Research (grant 0312019A).
Author information
Authors and Affiliations
Corresponding author
Electronic Supplementary Material
Below is the link to the electronic supplementary material.
ESM 1
(DOC 36 KB)
Figure 1
Copolymer-protected gene vectors (COPROGs) are assembled from polycation compacted DNA particles (here: branched PEI-DNA; box in center of figure) and protective copolymers by electrostatic interaction. The synthetic procedure for protective copolymers is shown here schematically and has been described elsewhere (15). Briefly, 3-(2′-pyridyldithio)-propionic acid (1) is reacted with t-butyl-protected glutamic acid under N-(3-dimethylaminopropyl)-N’-ethylcarbodiimide/1-hydroxybenzotriazole activation. The product is deprotected with trifluoroacetic acid to yield compound (2) which is co-polymerized with O,O’-bis(2-aminoethyl)-poly(ethylene glycol) (here: average molecular weight 6,000 Da) under dicyclohexylcarbodiimide activation. After purification by size exclusion chromatography, the reactive copolymer backbone is reacted with the peptide “YE5C” (sequence [Ac-YE5]2K-ahx-C; ahx = 6-aminohexanoic acid). Product (3) thus consists of a PEG backbone (shaded dark gray) and peptide side chains consisting of an anionic moiety (shaded light gray) linked to the backbone via a spacer (shaded intermediate gray). COPROGs are used to prepare vector-loaded fibrinogen components in the next step (Fig. 2) (PPT 175 KB)
Figure 2
Vector-loaded fibrinogen and formation cell-colonized fibrin clots. COPROGs in aqueous solution are mixed with the fibrinogen component of a fibrin glue and lyophilized. Before use, the product is rehydrated and mixed with freshly trypsinized cells of interest. A fibrin clot in which cells become transfected in situ is formed upon thrombin addition. This procedure may be used to fill or seal tissue defects with appropriate cells which upon in situ transfection would start to produce a desired growth factor (PPT 175 KB)
Figure 3
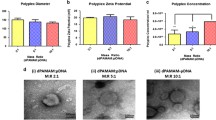
Vector impact on coagulation parameters. Fibrin clot formation was examined by rotation thromboelastography (ROTEG) analysis. Defined amounts of vector formulations were mixed with a fixed amount of fibrinogen solution. Clotting was initiated by thrombin addition. The parameters clotting time (CT; Fig. 3A), maximum clot firmness (MCF; Fig. 3B) and clot formation time (Fig. 3C) were recorded. Shown is the dose-dependent influence of vector formulations on these parameters relative to the values recorded for the control (1 mg/300 µl fibrinogen; clotting initiated by the addition of 0.2 units thrombin in 10 µl). Naked DNA (open squares) has virtually no influence in the examined dose range, unprotected PEI-DNA (open triangles) has little effect on clotting time but a strong impact on MCF and CFT. COPROGs (filled circles) retard clot formation (Fig. 3A) but only have a moderate impact on MCF and CFT up to a ratio of 20 µg DNA per mg fibrinogen. No firm clots are formed at the 30 µg/mg fibrinogen ratio. The data shown are mean values of duplicate measurements. The error bars connect the lower and higher value of the two measurements. The control (0 µg DNA/mg fibrinogen) is the average of 9 measurements, in this case the error bars represent the standard deviation from these 9 measurements (PPT 175 KB)
Rights and permissions
About this article
Cite this article
Schillinger, U., Wexel, G., Hacker, C. et al. A Fibrin Glue Composition as Carrier for Nucleic Acid Vectors. Pharm Res 25, 2946–2962 (2008). https://doi.org/10.1007/s11095-008-9719-8
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s11095-008-9719-8