Purpose
To investigate plasma pharmacokinetics and biodistribution of biodegradable polydisulfide Gd(III) complexes, Gd-DTPA cystine copolymers (GDCP) and Gd-DTPA cystine diethyl ester copolymers (GDCEP) and their efficacy as blood pool MRI contrast agents in comparison with a nondegradable macromolecular agent, Gd-DTPA 1,6-hexanediamine copolymers (GDHC).
Methods
The pharmacokinetics and biodistribution of GDCP and GDCEP with molecular weight of 35 KDa were investigated in Sprague‐Dawley rats after intravenous administration at a dose of 0.1 mmol Gd/kg. GDHC with the same molecular weight was used as a control. The Gd content in the plasma and various tissues and organs were determined by the ICP-OES. Plasma pharmacokinetic parameters were calculated by using a two-compartment model. The contrast enhanced blood pool MR imaging of the agents was evaluated in Sprague‐Dawley rats on a Siemens Trio 3T MR scanner.
Results
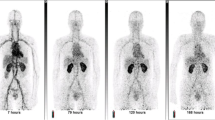
The biodegradable macromolecular agents, GDCP and GDCEP, had faster blood pool clearance than the nondegradable GDHC. The long-term Gd(III) tissue retention of the biodegradable polydisulfide agents was substantially lower than the nondegradable macromolecular agent. Both GDCP and GDCEP resulted in significant blood pool enhancement for the first 2 min post-injection and more rapid disappearance of the enhancement over time than GDHC. The negatively charged GDCP had prolonged enhancement duration as compared to GDCEP. The structure and biodegradability of the macromolecular contrast agents significantly affected their pharmacokinetics and blood pool contrast enhancement.
Conclusion
Both GDCP and GDCEP provided effective contrast enhancement for MR imaging of the blood pool. The accumulation of toxic Gd(III) ions in the body was greatly reduced with GDCP and GDCEP as compared to the nondegradable control.





Similar content being viewed by others
References
P. Caravan, J. J. Ellison, T. J. McMurry, and R. B. Lauffer. Gadolinium(III) chelates as MRI contrast agents: structure, dynamics, and applications. Chem. Rev. 99:2293–2352 (1999).
X. Wang, Y. Feng, T. Ke, M. Schabel, and Z.-R. Lu. Pharmacokinetics and tissue retention of (Gd-DTPA)-cystamine copolymers, a biodegradable macromolecular magnetic resonance imaging contrast agent. Pharm. Res. 22:596–602 (2005).
Y. Zong, X. Wang, K. C. Goodrich, A. M. Mohs, D. L. Parker, and Z.-R. Lu. Contrast-enhanced MRI with new biodegradable macromolecular Gd(III) complexes in tumor-bearing mice. Magn. Reson. Med. 53:835–842 (2005).
R. Laufferand, and T. J. Brady. Preparation and water relaxation properties of proteins labeled with paramagnetic metal chelates. Magn. Reson. Imaging 3:11–16 (1985).
A. A. J. Bogdanov, R. Weissleder, H. W. Frank, A. V. Bogdanova, N. Nossif, B. K. Schaffer, E. Tsai, M. I. Papisov, and T. J. Brady. A new macromolecule as a contrast agent for MR angiography: preparation, properties, and animal studies. Radiology 187:701–706 (1993).
V. P. Torchilin. Polymeric contrast agents for medical imaging. Curr. Pharm. Biotechnol. 1:183–215 (2000).
H. Kobayashiand, and M. W. Brechbiel. Dendrimer-based macromolecular MRI contrast agents: characteristics and application. Mol. Imaging 2:1–10 (2003).
C. Fink, S. Ley, M. Puderbach, C. Plathow, M. Bock, and H. U. Kauczor. 3D pulmonary perfusion MRI and MR angiography of pulmonary embolism in pigs after a single injection of a blood pool MR contrast agent. Eur. Radiol. 14:1291–1296 (2004).
L. E. Gerlowskiand, and R. K. Jain. Microvascular permeability of normal and neoplastic tissues. Microvasc. Res. 31:288–305 (1986).
A. Gossmann, Y. Okuhata, D. M. Shames, T. H. Helbich, T. P. Roberts, M. F. Wendland, S. Huber, and R. C. Brasch. Prostate cancer tumor grade differentiation with dynamic contrast-enhanced MR imaging in the rat: comparison of macromolecular and small-molecular contrast media-preliminary experience. Radiology 213:265–272 (1999).
R. Weissleder, A. J. Bogdanov, C. H. Tung, and H. J. Weinmann. Size optimization of synthetic graft copolymers for in vivo angiogenesis imaging. Bioconjug. Chem. 12:213–219 (2001).
Q. G. de Lussanet, S. Langereis, R. G. Beets-Tan, M. H. van Genderen, A. W. Griffioen, J. M. van Engelshoven, and W. H. Backes. Dynamic contrast-enhanced MR imaging kinetic parameters and molecular weight of dendritic contrast agents in tumor angiogenesis in mice. Radiology 235:65–72 (2005).
B. F. Jordan, M. Runquist, N. Raghunand, R. J. Gillies, W. R. Tate, G. Powis, and A. F. Baker. The thioredoxin-1 inhibitor 1-methylpropyl 2-imidazolyl disulfide (PX-12) decreases vascular permeability in tumor xenografts monitored by dynamic contrast enhanced magnetic resonance imaging. Clin. Cancer Res. 11:529–536 (2005).
P. Marzola, A. Degrassi, L. Calderan, P. Farace, E. Nicolato, C. Crescimanno, M. Sandri, A. Giusti, E. Pesenti, A. Terron, A. Sbarbati, and F. Osculati. Early antiangiogenic activity of SU11248 evaluated in vivo by dynamic contrast-enhanced magnetic resonance imaging in an experimental model of colon carcinoma. Clin. Cancer Res. 11:5827–5832 (2005).
D. Wang, S. C. Miller, M. Sima, D. Parker, H. Buswell, K. C. Goodrich, P. Kopeckova, and J. Kopecek. The arthrotropism of macromolecules in adjuvant-induced arthritis rat model: a preliminary study. Pharm. Res. 21:1741–1749 (2004).
B. Misselwitz, H. Schmitt-Willich, W. Ebert, T. Frenzel, and H. J. Weinmann. Pharmacokinetics of Gadomer-17, a new dendritic magnetic resonance contrast agent. Magma 12:128–134 (2001).
M. S. Dirksen, H. J. Lamb, P. Kunz, P. Robert, C. Corot, and A. de Roos. Improved MR coronary angiography with use of a new rapid clearance blood pool contrast agent in pigs. Radiology 227:802–808 (2003).
H. Kobayashi, and M. W. Brechbiel. Nano-sized MRI contrast agents with dendrimer cores. Adv. Drug Deliv. Rev. 57:2271–2286 (2005).
Z.-R. Lu, A. M. Mohs, Y. Zong, and Y. Feng. Polydisulfide Gd(III) chelates as biodegradable macromolecular magnetic resonance imaging contrast agents. Intl. J. Nanomed. 31–40 (2006).
Z.-R. Lu, D. L. Parker, K. C. Goodrich, X. Wang, J. G. Dalle, and H. R. Buswell. Extracellular biodegradable macromolecular gadolinium(III) complexes for MRI. Magn. Reson. Med. 51:27–34 (2004).
Z.-R. Lu, X. Wang, D. L. Parker, K. C. Goodrich, and H. R. Buswell. Poly(l-glutamic acid) Gd(III)-DOTA conjugate with a degradable spacer for magnetic resonance imaging. Bioconjug. Chem. 14:715–719 (2003).
T. Kaneshiro, T. Ke, E.-K. Jeong, D. L. Parker and Z.-R. Lu. Synthesis and characterization of (Gd-DTPA)-(l-cystine bisalkylamide) copolymers as novel biodegradable macromolecular MRI contrast agents. Pharm. Res. In press: (2006).
Acknowledgments
The research work is supported in part by the NIH grants R33 CA095873 and R01 EB00489. The authors thank Sheryl Dutson and Melody Johnson for technical support and valuable discussion.
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
About this article
Cite this article
Feng, Y., Zong, Y., Ke, T. et al. Pharmacokinetics, Biodistribution and Contrast Enhanced MR Blood Pool Imaging of Gd-DTPA Cystine Copolymers and Gd-DTPA Cystine Diethyl Ester Copolymers in a Rat Model. Pharm Res 23, 1736–1742 (2006). https://doi.org/10.1007/s11095-006-9028-z
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s11095-006-9028-z