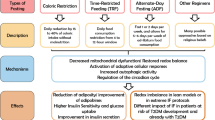
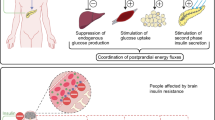
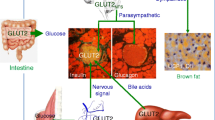
We studied insulin-induced intensification of glucose absorption and glycogen formation in the neocortex of young and old rats. In young animals, the corresponding shifts were clearly expressed; in old rats, insulin exerted nearly no stimulatory action on the processes of glucose metabolism in neocortical tissues. It was hypothesized that this is due to the age-related enhancement of the level of ceramides resulting in changes of the lipid spectrum of the cell membranes and also due to suppression of key components of signal pathways of insulin in the brain (such as Akt/protein kinase В, ARF, protein kinase С, and phospholipase D). These events disturb the signal cascade of the hormone and process of formation of the physiological response. An increase in the amount of ceramides in neocortical tissues of young animals after the action of exogenous С2 ceramide or palmitic acid (precursor of sphingolipids) was accompanied by suppression of the intensification of glucose absorption and insulin-stimulated formation of glycogen. Taking into account a significant increase in the amount of ceramides in the neocortex of old animals (this was shown in our earlier study), we believe that age-related accumulation of ceramide is an important reason for the development of insulin resistance of glucose metabolism in the CNS of old organisms.
Similar content being viewed by others
References
L. Pellerin and P. J. Magistretti, “Glutamate uptake into astrocytes stimulates aerobic glycolysis: a mechanism coupling neuronal activity to glucose utilization,” Proc. Natl. Acad. Sci. USA, 91, No. 22, 10625-10629 (1994).
C. Choeiri, W. Staines, and C. Messier, “Immunohistochemical localization and quantification of glucose transporters in the mouse brain,” Neuroscience, 111, No. 1, 19-34 (2002).
A. M. Brant, T. J. Jess, G. Milligan, et al., “Immunological analysis of glucose transporters expressed in different regions of the rat brain and central nervous system,” Biochem. Biophys. Res. Commun., 192, No. 3, 1297-1302 (1993).
T. Kayano, H. Fukumoto, R. L. Eddy, et al., “Evidence for a family of human glucose transporter-like proteins. Sequence and gene localization of a protein expressed in fetal skeletal muscle and other tissues,” J. Biol. Chem., 263, No. 30, 15245-15248 (1988).
G. W. Gould, A. M. Brant, B. B. Kahn, et al., “Expression of the brain-type glucose transporter is restricted to brain and neuronal cells in mice,” Diabetologia, 35, No. 4, 304-309 (1992).
G. A. Dienel, “Fueling and imaging brain activation,” Am. Soc. Neurochem. Neuro., 4(5), e00093 (2012); doi: 10.1042/AN20120021.
L. K. Bak, A. Schousboe, U. Sonnewald, and H. S. Waagepetersen, “Glucose is necessary to maintain neurotransmitter homeostasis during synaptic activity in cultured glutamatergic neurons,” J. Cerebr. Blood Flow Metab., 26, No. 10, 1285-1297 (2006).
C. Howarth, P. Gleeson, and D. Attwell, “Updated energy budgets for neural computation in the neocortex and cerebellum,” J. Cerebr. Blood Flow Metab., 32, 1222-1232 (2012).
M. V. Ivannikov, M. Sugimori, and R. R. Llinás, “Calcium clearance and its energy requirements in cerebellar neurons,” Cell Calcium, 47, 507-513 (2010).
M. Dinuzzo, S. Mangia, B. Maraviglia, and F. Giove, “The role of astrocytic glycogen in supporting the energetics of neuronal activity,” Neurochem. Res., 37, 2432-2438 (2012).
A. Suzuki, S. A. Stern, O. Bozdagi, et al., “Astrocyteneuron lactate transport is required for long-term memory formation,” Cell, 144, 810-823 (2011).
G. S. Watson and S. Craft, “Modulation of memory by insulin and glucose: neuropsychological observations in Alzheimer’s disease,” Eur. J. Pharmacol., 490, Nos. 1/3, 97-113 (2004).
Z. Laron, “Insulin and the brain,” Arch. Physiol. Biochem., 115, No. 2, 112-116 (2009).
W. Zhao, H. Chen, H. Xu, et al., “Brain insulin receptors and spatial memory. Correlated changes in gene expression, tyrosine phosphorylation, and signaling molecules in the hippocampus of water maze trained rats,” J. Biol. Chem., 274, No. 49, 34893-34902 (1999).
R. Schechter, T. Yanovitch, M. Abboud, et al., “Effects of brain endogenous insulin on neurofilament and MAPK in fetal rat neuron cell cultures,” Brain Res., 808, No. 2, 270-278 (1998).
J. Havrankova, J. Roth, and M. Brownstein, “Insulin receptors are widely distributed in the central nervous system of the rat,” Nature, 272, No. 56, 827-829 (1978).
E. Araki, M. A. Lipes, M. E. Patti, et al., “Alternative pathway of insulin signalling in mice with targeted disruption of the IRS-1 gene,” Nature, 372, No. 6502, 186-190 (1994).
L. Plum, M. Schubert, and J. C. Brüning, “The role of insulin receptor signaling in the brain,” Trends Endocrinol. Metab., 16, No. 2, 59-65 (2005).
C. A. Grillo, G. G. Piroli, R. M. Hendry, and L. P. Reagan, “Insulin-stimulated translocation of GLUT4 to the plasma membrane in rat hippocampus is PI3-kinase dependent,” Brain Res., 1296, 35-45 (2009).
S. M. de la Monte, “Insulin resistance and Alzheimer’s disease,” BMB Rep., 42, No. 8, 475-481 (2009).
S. M. de la Monte, E. Re, L. Longato, and M. Tong, “Dysfunctional pro-ceramide, ER stress, and insulin/IGF signaling networks with progression of Alzheimer’s disease,” J. Alzheimer’s Dis., 30, Suppl. 2, S217-S229 (2012).
D. Kapogiannis and M. P. Mattson, “Disrupted energy metabolism and neuronal circuit dysfunction in cognitive impairment and Alzheimer’s disease,” Lancet Neurol., 10, 187-198 (2011).
J. A. Chavez, W. L. Holland, J. Bar, et al., “Acid ceramidase overexpression prevents the inhibitory effects of saturated fatty acids on insulin signaling,” J. Biol. Chem., 280, No. 20, 20148-20153 (2005).
M. Heni, A. M. Hennige, A. Peter, et al., “Insulin promotes glycogen storage and cell proliferation in primary human astrocytes,” PLoS ONE, 6, No. 6, e21594 (2011).
O. N. Lowry, N. J. Rosebrough, A. L. Farr, and R. J. Randal, “Protein measurement with the folin phenol reagent,” J. Biol. Chem., 193, 365-375 (1951).
N. A. Babenko and V. S. Kharchenko, “Ceramides inhibit phospholipase D-dependent insulin signaling in liver cells of old rats,” Biochemistry, 77, No. 2, 180-186 (2012).
N. A. Babenko, L. K. Hassouneh, V. S. Kharchenko, and V. V. Garkavenko, “Vitamin E prevents the agedependent and palmitate-induced disturbances of sphingolipid turnover in liver cells,” Age (Dordr.), 34, 905-915 (2012).
N. A. Babenko and V. S. Kharchenko, “Role of ceramides in disruption of insulin signaling in the rat diaphragm under in vivo and in vitro conditions,” Probl. Endokrinol. Patol., No. 1, 37-43 (2009).
N. A. Babenko and V. S. Kharchenko, “Age-related changes in the phospholipase D-dependent signal pathway of insulin in the rat neocortex,” Neurophysiology, 45, No. 2, 120-127 (2013).
N. A. Babenko and Y. A. Semenova, “Effects of long-term fish oil-enriched diet on the sphingolipid metabolism in brain of old rats,” Exp. Gerontol., 45, No. 5, 375-380 (2010).
G. A. Salvador, S. J. Pasquare, M. G. Ilincheta de Boschero, and N. M. Giusto, “Differential modulation of phospholipase D and phosphatidate phosphohydrolase during aging in rat cerebral cortex synaptosomes,” Exp. Gerontol., 37, No. 4, 543-552 (2002).
Y. Xu, B. R. Rubin, C. M. Orme, et al., “Dual-mode of insulin action controls GLUT4 vesicle exocytosis,” J. Cell Biol., 193, No. 4, 643-653 (2011).
I. N. Singh, L. M. Stromberg, S. G. Bourgoin, et al., “Ceramide inhibition of mammalian phospholipase D1 and D2 activities is antagonized by phosphatidylinositol 4,5-bisphosphate,” Biochemistry, 40, 11227-11233 (2001).
A. Abousalham, C. Liossis, L. O’Brien, and D. N. Brindley, “Cell-permeable ceramides prevent the activation of phospholipase D by ADP-ribosylation factor and RhoA,” J. Biol. Chem., 272, 1069-1075 (1997).
A. S. Mebarek, H. Komati, F. Naro, et al., “Inhibition of de novo ceramide synthesis upregulates phospholipase D and enhances myogenic differentiation,” J. Cell. Sci., 120, Part 3, 407-416 (2007).
A. Gidwani, H. A. Brown, D. Holowka, and B. Baird, “Disruption of lipid order by short-chain ceramides correlates with inhibition of phospholipase D and downstream signaling by FcepsilonRI,” J. Cell Sci., 116, 3177-3187 (2003).
S. Patil, D. Balu, J. Melrose, and C. Chan, “Brain regionspecificity of palmitic acid-induced abnormalities associated with Alzheimer’s disease,” BMC Res. Notes, 4, 1-20 (2008).
N. D. Ridgway and D. L. Merriam, “Metabolism of short-chain ceramide and dihydroceramide analogues in Chinese hamster ovary (CHO) cells,” Biochim. Biophys. Acta, 1256, No. 1, 57-70 (1995).
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
About this article
Cite this article
Babenko, N.A., Kharchenko, V.S. Effects of Aging and Experimentally Induced Modifications of Signal Pathways on Insulin-Induced Shifts of Glucose Metabolism in the Rat Neocortex. Neurophysiology 47, 16–22 (2015). https://doi.org/10.1007/s11062-015-9491-4
Received:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s11062-015-9491-4