Abstract
Introduction
5-aminolevulinic acid (5-ALA) was approved by the FDA in June 2017 as an intra-operative optical imaging agent for patients with gliomas (suspected World Health Organization Grades III or IV on preoperative imaging) as an adjunct for the visualization of malignant tissue during surgery. 5-ALA fluorescence-guided surgery (FGS) has been in widespread use in Europe and other continents since 2007.
Methods
We reviewed the data available and summarize the most important known uses of 5-ALA FGS and its potential future applications.
Results/conclusions
The technique has been extensively studied, and more than 300 papers have been published on this topic. Visualization of high-grade glioma tissue is robust and reproducible, and can impact the extent of tumor resection and patient outcomes. 5-ALA FGS for other kind of tumors needs further development.
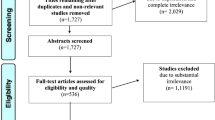
Graphical abstract

Similar content being viewed by others
References
Stummer W, Stepp H, Moller G et al (1998) Technical principles for protoporphyrin-IX-fluorescence guided microsurgical resection of malignant glioma tissue. Acta Neurochir (Wien) 140:995–1000
Albert FKMD, Forsting MMD, Sartor KMD et al (1994) Early postoperative magnetic resonance imaging after resection of malignant glioma: objective evaluation of residual tumor and its influence on regrowth and prognosis. Neurosurgery 34:45–61
Stummer W, Novotny A, Stepp H et al (2000) Fluorescence-guided resection of glioblastoma multiforme by using 5-aminolevulinic acid-induced porphyrins: a prospective study in 52 consecutive patients. J Neurosurg 93:1003–1013
Stummer W, Pichlmeier U, Meinel T et al (2006) Fluorescence-guided surgery with 5-aminolevulinic acid for resection of malignant glioma: a randomised controlled multicentre phase III trial. Lancet Oncol 7:392–401. https://doi.org/10.1016/S1470-2045(06)70665-9
Zhao S, Wu J, Wang C et al (2013) Intraoperative fluorescence-guided resection of high-grade malignant gliomas using 5-aminolevulinic acid-induced porphyrins: a systematic review and meta-analysis of prospective studies. PLoS ONE 8:e63682. https://doi.org/10.1371/journal.pone.0063682
Eljamel S (2015) 5-ALA fluorescence image guided resection of glioblastoma multiforme: a meta-analysis of the literature. Int J Mol Sci 16:10443–10456. https://doi.org/10.3390/ijms160510443
Marko NF, Weil RJ, Schroeder JL et al (2014) Extent of resection of glioblastoma revisited: personalized survival modeling facilitates more accurate survival prediction and supports a maximum-safe-resection approach to surgery. J Clin Oncol 32:774–782. https://doi.org/10.1200/JCO.2013.51.8886
Sanai N, Polley MY, McDermott MW et al (2011) An extent of resection threshold for newly diagnosed glioblastomas. J Neurosurg 115:3–8. https://doi.org/10.3171/2011.2.JNS10998
McGirt MJ, Chaichana KL, Gathinji M et al (2009) Independent association of extent of resection with survival in patients with malignant brain astrocytoma. J Neurosurg 110:156–162. https://doi.org/10.3171/2008.4.17536
Stupp R, Mason WP, van den Bent MJ et al (2005) Radiotherapy plus concomitant and adjuvant temozolomide for glioblastoma. N Engl J Med 352:987–996. https://doi.org/10.1056/NEJMoa043330
Stummer W, Reulen HJ, Meinel T et al (2008) Extent of resection and survival in glioblastoma multiforme: identification of and adjustment for bias. Neurosurgery 62:564–576. https://doi.org/10.1227/01.neu.0000317304.31579.17
Díez Valle R, Slof J, Galván J et al (2014) Observational, retrospective study of the effectiveness of 5-aminolevulinic acid in malignant glioma surgery in Spain (The VISIONA study). Neurologia. https://doi.org/10.1016/j.nrl.2013.05.004
Jaber M, Wolfer J, Ewelt C et al (2016) The value of 5-aminolevulinic acid in low-grade gliomas and high-grade gliomas lacking glioblastoma imaging features: an analysis based on fluorescence, magnetic resonance imaging, 18F-fluoroethyl tyrosine positron emission tomography, and tumor molecular. Neurosurgery 78:401–411. https://doi.org/10.1227/NEU.0000000000001020 discussion 411
Díez Valle R, Tejada Solis S, Idoate Gastearena MA et al (2011) Surgery guided by 5-aminolevulinic fluorescence in glioblastoma: volumetric analysis of extent of resection in single-center experience. J Neurooncol. https://doi.org/10.1007/s11060-010-0296-4
Stummer W, Tonn JC, Goetz C et al (2014) 5-Aminolevulinic acid-derived tumor fluorescence: the diagnostic accuracy of visible fluorescence qualities as corroborated by spectrometry and histology and postoperative imaging. Neurosurgery 74:310–320. https://doi.org/10.1227/NEU.0000000000000267
Coburger J, Engelke J, Scheuerle A et al (2014) Tumor detection with 5-aminolevulinic acid fluorescence and Gd-DTPA-enhanced intraoperative MRI at the border of contrast-enhancing lesions: a prospective study based on histopathological assessment. Neurosurg Focus 36:E3. https://doi.org/10.3171/2013.11.FOCUS13463
Kiesel B, Mischkulnig M, Woehrer A et al (2018) Systematic histopathological analysis of different 5-aminolevulinic acid-induced fluorescence levels in newly diagnosed glioblastomas. J Neurosurg 129:341–353. https://doi.org/10.3171/2017.4.JNS162991
Roberts DW, Valdes PA, Harris BT et al (2011) Coregistered fluorescence-enhanced tumor resection of malignant glioma: relationships between delta-aminolevulinic acid-induced protoporphyrin IX fluorescence, magnetic resonance imaging enhancement, and neuropathological parameters. Clinical article. J Neurosurg 114:595–603. https://doi.org/10.3171/2010.2.JNS091322
Lau D, Hervey-Jumper SL, Chang S et al (2015) A prospective Phase II clinical trial of 5-aminolevulinic acid to assess the correlation of intraoperative fluorescence intensity and degree of histologic cellularity during resection of high-grade gliomas. J Neurosurg. https://doi.org/10.3171/2015.5.JNS1577
Yamada S, Muragaki Y, Maruyama T et al (2015) Role of neurochemical navigation with 5-aminolevulinic acid during intraoperative MRI-guided resection of intracranial malignant gliomas. Clin Neurol Neurosurg 130:134–139. https://doi.org/10.1016/j.clineuro.2015.01.005
Aldave G, Gonzalez-Huarriz M, Rubio A et al (2018) The aberrant splicing of BAF45d links splicing regulation and transcription in glioblastoma. Neuro Oncology 20:930–941. https://doi.org/10.1093/neuonc/noy007
Idoate MA, Díez Valle R, Echeveste J, Tejada S (2011) Pathological characterization of the glioblastoma border as shown during surgery using 5-aminolevulinic acid-induced fluorescence. Neuropathology. https://doi.org/10.1111/j.1440-1789.2011.01202.x
Piccirillo SG, Dietz S, Madhu B et al (2012) Fluorescence-guided surgical sampling of glioblastoma identifies phenotypically distinct tumour-initiating cell populations in the tumour mass and margin. Br J Cancer 107:462–468. https://doi.org/10.1038/bjc.2012.271
Rampazzo E, Della Puppa A, Frasson C et al (2014) Phenotypic and functional characterization of Glioblastoma cancer stem cells identified trough 5-aminolevulinic acid-assisted surgery. J Neurooncol 116:505–513. https://doi.org/10.1007/s11060-013-1348-3
Ross JL, Cooper LAD, Kong J et al (2017) 5-Aminolevulinic acid guided sampling of glioblastoma microenvironments identifies pro-survival signaling at infiltrative margins. Sci Rep 7:15593. https://doi.org/10.1038/s41598-017-15849-w
Widhalm G, Wolfsberger S, Minchev G et al (2010) 5-Aminolevulinic acid is a promising marker for detection of anaplastic foci in diffusely infiltrating gliomas with nonsignificant contrast enhancement. Cancer 116:1545–1552. https://doi.org/10.1002/cncr.24903
von Campe G, Moschopulos M, Hefti M (2012) 5-Aminolevulinic acid-induced protoporphyrin IX fluorescence as immediate intraoperative indicator to improve the safety of malignant or high-grade brain tumor diagnosis in frameless stereotactic biopsies. Acta Neurochir (Wien) 154:585–588. https://doi.org/10.1007/s00701-012-1290-8 discussion 588
Widhalm G, Minchev G, Woehrer A et al (2012) Strong 5-aminolevulinic acid-induced fluorescence is a novel intraoperative marker for representative tissue samples in stereotactic brain tumor biopsies. Neurosurg Rev 35:381–391. https://doi.org/10.1007/s10143-012-0374-5;10.1007/s10143-012-0374-5 discussion 391
Brown TJ, Brennan MC, Li M et al (2016) Association of the extent of resection with survival in glioblastoma: a systematic review and meta-analysis. JAMA Oncol 2:1460–1469. https://doi.org/10.1001/jamaoncol.2016.1373
Kelly PJ, Daumas-Duport C, Kispert DB et al (1987) Imaging-based stereotaxic serial biopsies in untreated intracranial glial neoplasms. J Neurosurg 66:865–874. https://doi.org/10.3171/jns.1987.66.6.0865
Li YM, Suki D, Hess K, Sawaya R (2016) The influence of maximum safe resection of glioblastoma on survival in 1229 patients: can we do better than gross-total resection? J Neurosurg 124:977–988. https://doi.org/10.3171/2015.5.JNS142087
Suchorska B, Jansen NL, Linn J et al (2015) Biological tumor volume in 18FET-PET before radiochemotherapy correlates with survival in GBM. Neurology 84:710–719. https://doi.org/10.1212/WNL.0000000000001262
De Bonis P, Anile C, Pompucci A et al (2013) The influence of surgery on recurrence pattern of glioblastoma. Clin Neurol Neurosurg 115:37–43. https://doi.org/10.1016/j.clineuro.2012.04.005
Eljamel S, Petersen M, Valentine R et al (2013) Comparison of intraoperative fluorescence and MRI image guided neuronavigation in malignant brain tumours, a prospective controlled study. Photodiagnosis Photodyn Ther 10:356–361. https://doi.org/10.1016/j.pdpdt.2013.03.006
Schucht P, Knittel S, Slotboom J et al (2014) 5-ALA complete resections go beyond MR contrast enhancement: shift corrected volumetric analysis of the extent of resection in surgery for glioblastoma. Acta Neurochir (Wien) 156:305–312. https://doi.org/10.1007/s00701-013-1906-7;discussion 312
Aldave G, Tejada S, Pay E et al (2013) Prognostic value of residual fluorescent tissue in glioblastoma patients after gross total resection in 5-aminolevulinic acid-guided surgery. Neurosurgery. https://doi.org/10.1227/NEU.0b013e31828c3974
Tejada S, Díez-Valle R, Aldave G et al (2014) Factors associated with a higher rate of distant failure after primary treatment for glioblastoma. J Neurooncol. https://doi.org/10.1007/s11060-013-1279-z
Schucht P, Murek M, Jilch A et al (2013) Early re-do surgery for glioblastoma is a feasible and safe strategy to achieve complete resection of enhancing tumor. PLoS ONE 8:e79846. https://doi.org/10.1371/journal.pone.0079846
Coburger J, Scheuerle A, Pala A et al (2017) Histopathological insights on imaging results of intraoperative magnetic resonance imaging, 5-aminolevulinic acid, and intraoperative ultrasound in glioblastoma surgery. Neurosurgery 81:165–174. https://doi.org/10.1093/neuros/nyw143
Suero Molina E, Schipmann S, Stummer W (2017) Maximizing safe resections: the roles of 5-aminolevulinic acid and intraoperative MR imaging in glioma surgery-review of the literature. Neurosurg Rev. https://doi.org/10.1007/s10143-017-0907-z
Cordova JS, Shu H-KG, Liang Z et al (2016) Whole-brain spectroscopic MRI biomarkers identify infiltrating margins in glioblastoma patients. Neuro Oncol 18:1180–1189. https://doi.org/10.1093/neuonc/now036
Bloch O, Han SJ, Cha S et al (2012) Impact of extent of resection for recurrent glioblastoma on overall survival: clinical article. J Neurosurg 117:1032–1038. https://doi.org/10.3171/2012.9.JNS12504
Hickmann A-K, Nadji-Ohl M, Hopf NJ (2015) Feasibility of fluorescence-guided resection of recurrent gliomas using five-aminolevulinic acid: retrospective analysis of surgical and neurological outcome in 58 patients. J Neurooncol 122:151–160. https://doi.org/10.1007/s11060-014-1694-9
Della Puppa A, Ciccarino P, Lombardi G et al (2014) 5-Aminolevulinic acid fluorescence in high grade glioma surgery: surgical outcome, intraoperative findings, and fluorescence patterns. Biomed Res Int 2014:232561. https://doi.org/10.1155/2014/232561
Tykocki T, Michalik R, Bonicki W, Nauman P (2012) Fluorescence-guided resection of primary and recurrent malignant gliomas with 5-aminolevulinic acid. Preliminary results. Neurol Neurochir Pol 46:47–51
Archavlis E, Tselis N, Birn G et al (2014) Salvage therapy for recurrent glioblastoma multiforme: a multimodal approach combining fluorescence-guided resurgery, interstitial irradiation, and chemotherapy. Neurol Res 36:1047–1055. https://doi.org/10.1179/1743132814Y.0000000398
Ringel F, Pape H, Sabel M et al (2016) Clinical benefit from resection of recurrent glioblastomas: results of a multicenter study including 503 patients with recurrent glioblastomas undergoing surgical resection. Neuro Oncol 18:96–104. https://doi.org/10.1093/neuonc/nov145
Nabavi A, Thurm H, Zountsas B et al (2009) Five-aminolevulinic acid for fluorescence-guided resection of recurrent malignant gliomas: a phase ii study. Neurosurgery 65:1070–1077. https://doi.org/10.1227/01.NEU.0000360128.03597.C7
Kamp MA, Felsberg J, Sadat H et al (2015) 5-ALA-induced fluorescence behavior of reactive tissue changes following glioblastoma treatment with radiation and chemotherapy. Acta Neurochir (Wien) 157:204–207. https://doi.org/10.1007/s00701-014-2313-4
Utsuki S, Oka H, Sato S et al (2007) Histological examination of false positive tissue resection using 5-aminolevulinic acid-induced fluorescence guidance. Neurol Med Chir (Tokyo) 47:210–214
Kamp MA, Krause Molle Z, Munoz-Bendix C et al (2018) Various shades of red-a systematic analysis of qualitative estimation of ALA-derived fluorescence in neurosurgery. Neurosurg Rev 41:3–18. https://doi.org/10.1007/s10143-016-0745-4
Coluccia D, Fandino J, Fujioka M et al (2010) Intraoperative 5-aminolevulinic-acid-induced fluorescence in meningiomas. Acta Neurochir (Wien) 152:1711–1719. https://doi.org/10.1007/s00701-010-0708-4
Millesi M, Kiesel B, Mischkulnig M et al (2016) Analysis of the surgical benefits of 5-ALA-induced fluorescence in intracranial meningiomas: experience in 204 meningiomas. J Neurosurg 125:1408–1419. https://doi.org/10.3171/2015.12.JNS151513
Valdes PA, Bekelis K, Harris BT et al (2014) 5-Aminolevulinic acid-induced protoporphyrin IX fluorescence in meningioma: qualitative and quantitative measurements in vivo. Neurosurgery 10(Suppl 1):73–74. https://doi.org/10.1227/NEU.0000000000000117
Kajimoto Y, Kuroiwa T, Miyatake S, et al (2007) Use of 5-aminolevulinic acid in fluorescence-guided resection of meningioma with high risk of recurrence. Case report. J Neurosurg 106:1070–1074. https://doi.org/10.3171/jns.2007.106.6.1070
Cornelius JF, Slotty PJ, Kamp MA et al (2014) Impact of 5-aminolevulinic acid fluorescence-guided surgery on the extent of resection of meningiomas—with special regard to high-grade tumors. Photodiagnosis Photodyn Ther 11:481–490. https://doi.org/10.1016/j.pdpdt.2014.07.008
Morofuji Y, Matsuo T, Hayashi Y et al (2008) Usefulness of intraoperative photodynamic diagnosis using 5-aminolevulinic acid for meningiomas with cranial invasion: technical case report. Neurosurgery 62:102–104. https://doi.org/10.1227/01.neu.0000317378.22820.46
Della Puppa A, Rustemi O, Gioffre G et al (2014) Predictive value of intraoperative 5-aminolevulinic acid-induced fluorescence for detecting bone invasion in meningioma surgery. J Neurosurg 120:840–845. https://doi.org/10.3171/2013.12.JNS131642
Wilbers E, Hargus G, Wolfer J, Stummer W (2014) Usefulness of 5-ALA (Gliolan(R))-derived PPX fluorescence for demonstrating the extent of infiltration in atypical meningiomas. Acta Neurochir (Wien) 156:1853–1854
Scheichel F, Ungersboeck K, Kitzwoegerer M, Marhold F (2017) Fluorescence-guided resection of extracranial soft tissue tumour infiltration in atypical meningioma. Acta Neurochir (Wien) 159:1027–1031. https://doi.org/10.1007/s00701-017-3166-4
Valdes PA, Jacobs V, Harris BT et al (2015) Quantitative fluorescence using 5-aminolevulinic acid-induced protoporphyrin IX biomarker as a surgical adjunct in low-grade glioma surgery. J Neurosurg 123:771–780. https://doi.org/10.3171/2014.12.JNS14391
Wei L, Roberts DW, Sanai N, Liu JTC (2018) Visualization technologies for 5-ALA-based fluorescence-guided surgeries. J Neurooncol. https://doi.org/10.1007/s11060-018-03077-9
Evers G, Kamp M, Warneke N et al (2017) 5-Aminolaevulinic acid-induced fluorescence in primary central nervous system lymphoma. World Neurosurg 98:375–380. https://doi.org/10.1016/j.wneu.2016.11.011
Yamamoto J, Kitagawa T, Akiba D, Nishizawa S (2015) 5-Aminolevulinic acid-induced fluorescence in cerebellar primary central nervous system lymphoma: a case report and literature review. Turk Neurosurg 25:796–800. https://doi.org/10.5137/1019-5149.JTN.10594-14.1
Yamamoto T, Ishikawa E, Miki S et al (2015) Photodynamic diagnosis using 5-aminolevulinic acid in 41 biopsies for primary central nervous system lymphoma. Photochem Photobiol 91:1452–1457. https://doi.org/10.1111/php.12510
Takeda J, Nonaka M, Li Y et al (2017) 5-ALA fluorescence-guided endoscopic surgery for mixed germ cell tumors. J Neurooncol 134:119–124. https://doi.org/10.1007/s11060-017-2494-9
Kamp MA, Munoz-Bendix C, Mijderwijk HJ, Turowski B, Dibué-Adjei M, von Saß C, Cornelius JF, Steiger HJ, Rapp M, Sabel M (2018) Is 5-ALA fluorescence of cerebral metastases a prognostic factor for local recurrence and overall survival? J Neuroncol. https://doi.org/10.1007/s11060-018-03066-y
Utsuki S, Oka H, Kijima C et al (2011) Utility of intraoperative fluorescent diagnosis of residual hemangioblastoma using 5-aminolevulinic acid. Neurol India 59:612–615. https://doi.org/10.4103/0028-3886.84349
Utsuki S, Oka H, Sato K et al (2010) Fluorescence diagnosis of tumor cells in hemangioblastoma cysts with 5-aminolevulinic acid. J Neurosurg 112:130–132. https://doi.org/10.3171/2009.5.JNS08442
Bernal Garcia LM, Cabezudo Artero JM, Marcelo Zamorano MB, Gilete Tejero I (2015) Fluorescence-guided resection with 5-aminolevulinic Acid of subependymomas of the fourth ventricle: report of 2 cases: technical case report. Neurosurgery 11(Suppl 2):E364–E371. https://doi.org/10.1227/NEU.0000000000000682 discussion E371
Stummer W, Rodrigues F, Schucht P et al (2014) Predicting the “usefulness” of 5-ALA-derived tumor fluorescence for fluorescence-guided resections in pediatric brain tumors: a European survey. Acta Neurochir (Wien) 156:2315–2324. https://doi.org/10.1007/s00701-014-2234-2
Inoue T, Kanamori M, Sonoda Y et al (2008) Glioblastoma multiforme developing separately from the initial lesion 9 years after successful treatment for gliomatosis cerebri: a case report. Neurol Surg 36:709–715
Beck TJ, Kreth FW, Beyer W et al (2007) Interstitial photodynamic therapy of nonresectable malignant glioma recurrences using 5-aminolevulinic acid induced protoporphyrin IX. Lasers Surg Med 39:386–393. https://doi.org/10.1002/lsm.20507
Stummer W, Beck T, Beyer W et al (2008) Long-sustaining response in a patient with non-resectable, distant recurrence of glioblastoma multiforme treated by interstitial photodynamic therapy using 5-ALA: case report. J Neurooncol 87:103–109. https://doi.org/10.1007/s11060-007-9497-x
Etminan N, Peters C, Ficnar J et al (2011) Modulation of migratory activity and invasiveness of human glioma spheroids following 5-aminolevulinic acid-based photodynamic treatment. Laboratory investigation. J Neurosurg 115:281–288. https://doi.org/10.3171/2011.3.JNS10434
Castano AP, Mroz P, Hamblin MR (2006) Photodynamic therapy and anti-tumour immunity. Nat Rev Cancer 6:535–545. https://doi.org/10.1038/nrc1894
Dupont C, Vermandel M, Leroy H-A et al (2018) Intraoperative photodynamic therapy for glioblastomas: study protocol for a Phase I Clinical Trial. Neurosurgery. https://doi.org/10.1093/neuros/nyy324
Funding
This study did not receive any funding.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflict of interest
Walter Stummer has received speaker and consultant fees by Carl Zeiss, Leica, Medac, NXDC. Constantinos Hadjipanayis is a consultant for NXDC and Synaptive Medical Inc. He will receive potential royalties from NXDC. He has also received speaker fees by Carl Zeiss and Leica. Ricardo Díez Valle has received speaker fees by Medac.
Research involving human participants or animals
This article does not contain any studies with human participants or animals performed by any of the authors.
Rights and permissions
About this article
Cite this article
Díez Valle, R., Hadjipanayis, C.G. & Stummer, W. Established and emerging uses of 5-ALA in the brain: an overview. J Neurooncol 141, 487–494 (2019). https://doi.org/10.1007/s11060-018-03087-7
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s11060-018-03087-7