Abstract
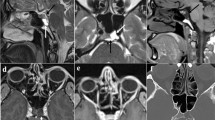
Rathke’s cleft cysts (RCCs), also known as pars intermedia cysts, represent benign lesions formed from remnants of the embryologic Rathke’s pouch. Commonly asymptomatic, they are identified in nearly 1 in 6 healthy volunteers undergoing brain imaging. When symptomatic, they can cause headaches, endocrine dysfunction, and, rarely, visual disturbances. A systematic review of the published English literature was performed focusing on large modern case series of RCCs to describe their natural history, clinicopathologic features, radiographic features, and surgical outcomes, including rates of recurrence. The natural history of asymptomatic RCCs is one of slow growth, suggesting that observation through serial magnetic resonance imaging is appropriate for smaller asymptomatic RCCs. Symptomatic RCCs can be treated by surgical resection with low morbidity, usually through an endonasal transsphenoidal corridor using either a microscope or an endoscope. Surgical treatment frequently provides symptomatic relief of headaches and visual disturbances, and sometimes even improves endocrine dysfunction. Rates of recurrence after surgical treatment range from 16 to 18 % in large series, and higher rates of recurrence are associated with suprasellar location, inflammation and reactive squamous metaplasia in the cyst wall, superinfection of the cyst, and use of a fat graft into the cyst cavity.




Similar content being viewed by others
References
Voelker JL, Campbell RL, Muller J (1991) Clinical, radiographic, and pathological features of symptomatic Rathke’s cleft cysts. J Neurosurg 74:535–544
Fager CA, Carter H (1966) Intrasellar epithelial cysts. J Neurosurg 24:77–81
McGrath P (1971) Cysts of sellar and pharyngeal hypophyses. Pathology 3:123–131
Shanklin WM (1949) On the presence of cysts in the human pituitary. Anat Rec 104:379–407
Teramoto A, Hirakawa K, Sanno N, Osamura Y (1994) Incidental pituitary lesions in 1,000 unselected autopsy specimens. Radiology 193:161–164
Ross DA, Norman D, Wilson CB (1992) Radiologic characteristics and results of surgical management of Rathke’s cysts in 43 patients. Neurosurgery 30:173–178 discussion 178–179
el-Mahdy W, Powell M (1998) Transsphenoidal management of 28 symptomatic Rathke’s cleft cysts, with special reference to visual and hormonal recovery. Neurosurgery 42:7–16 discussion 16–17
Aho CJ, Liu C, Zelman V, Couldwell WT, Weiss MH (2005) Surgical outcomes in 118 patients with Rathke cleft cysts. J Neurosurg 102:189–193
Benveniste RJ, King WA, Walsh J, Lee JS, Naidich TP, Post KD (2004) Surgery for Rathke cleft cysts: technical considerations and outcomes. J Neurosurg 101:577–584
Zada G, Lin N, Ojerholm E, Ramkissoon S (2010) Laws ER: craniopharyngioma and other cystic epithelial lesions of the sellar region: a review of clinical, imaging, and histopathological relationships. Neurosurg Focus 28:E4
Prabhu VC, Brown HG (2005) The pathogenesis of craniopharyngiomas. Childs Nerv Syst 21:622–627
Hsu HY, Piva A, Sadun AA (2004) Devastating complications from alcohol cauterization of recurrent Rathke cleft cyst. Case report. J Neurosurg 100:1087–1090
Harrison MJ, Morgello S, Post KD (1994) Epithelial cystic lesions of the sellar and parasellar region: a continuum of ectodermal derivatives? J Neurosurg 80:1018–1025
Iraci G, Giordano R, Gerosa M, Rigobello L, Di Stefano E (1979) Ocular involvement in recurrent cyst of Rathke’s cleft: case report. Ann Ophthalmol 11:94–98
Matsushima T, Fukui M, Ohta M, Yamakawa Y, Takaki T, Okano H (1980) Ciliated and goblet cells in craniopharyngioma. Light and electron microscopic studies at surgery and autopsy. Acta Neuropathol 50:199–205
Tate MC, Jahangiri A, Blevins L, Kunwar S, Aghi MK (2010) Infected Rathke cleft cysts: distinguishing factors and factors predicting recurrence. Neurosurgery 67:762–769 discussion 769
Isono M, Kamida T, Kobayashi H, Shimomura T, Matsuyama J (2001) Clinical features of symptomatic Rathke’s cleft cyst. Clin Neurol Neurosurg 103:96–100
Jahangiri A, Molinaro AM, Tarapore PE, Blevins L, Jr, Auguste KI, Gupta N, Kunwar S, Aghi MK (2011) Rathke cleft cysts in pediatric patients: presentation, surgical management, and postoperative outcomes. Neurosurg Focus 31:E3
Lillehei KO, Widdel L, Arias Astete CA, Wierman ME, Kleinschmidt-Demasters BK, Kerr JM (2010) Transsphenoidal resection of 82 Rathke cleft cysts: limited value of alcohol cauterization in reducing recurrence rates. J Neurosurg 27:27
Kim JE, Kim JH, Kim OL, Paek SH, Kim DG, Chi JG, Jung HW (2004) Surgical treatment of symptomatic Rathke cleft cysts: clinical features and results with special attention to recurrence. J Neurosurg 100:33–40
Potts MB, Jahangiri A, Lamborn KR, Blevins LS, Kunwar S, Aghi MK (2011) Suprasellar Rathke cleft cysts: clinical presentation and treatment outcomes. Neurosurgery 69:1058–1068 discussion 1068–1057
Kasperbauer JL, Orvidas LJ, Atkinson JL, Abboud CF (2002) Rathke cleft cyst: diagnostic and therapeutic considerations. Laryngoscope 112:1836–1839
Mukherjee JJ, Islam N, Kaltsas G, Lowe DG, Charlesworth M, Afshar F, Trainer PJ, Monson JP, Besser GM, Grossman AB (1997) Clinical, radiological and pathological features of patients with Rathke’s cleft cysts: tumors that may recur. J Clin Endocrinol Metab 82:2357–2362
Komatsu F, Tsugu H, Komatsu M, Sakamoto S, Oshiro S, Fukushima T, Nabeshima K, Inoue T (2010) Clinicopathological characteristics in patients presenting with acute onset of symptoms caused by Rathke’s cleft cysts. Acta Neurochir (Wien) 152:1673–1678
Nishikawa T, Takahashi JA, Shimatsu A, Hashimoto N (2007) Hypophysitis caused by Rathke’s cleft cyst. Case report. Neurol Med Chir (Tokyo) 47:136–139
Roncaroli F, Bacci A, Frank G, Calbucci F (1998) Granulomatous hypophysitis caused by a ruptured intrasellar Rathke’s cleft cyst: report of a case and review of the literature. Neurosurgery 43:146–149
Schittenhelm J, Beschorner R, Psaras T, Capper D, Nagele T, Meyermann R, Saeger W, Honegger J, Mittelbronn M (2008) Rathke’s cleft cyst rupture as potential initial event of a secondary perifocal lymphocytic hypophysitis: proposal of an unusual pathogenetic event and review of the literature. Neurosurg Rev 31:157–163
Sonnet E, Roudaut N, Meriot P, Besson G, Kerlan V (2006) Hypophysitis associated with a ruptured Rathke’s cleft cyst in a woman, during pregnancy. J Endocrinol Invest 29:353–357
Albini CH, MacGillivray MH, Fisher JE, Voorhess ML, Klein DM (1988) Triad of hypopituitarism, granulomatous hypophysitis, and ruptured Rathke’s cleft cyst. Neurosurgery 22:133–136
Daikokuya H, Inoue Y, Nemoto Y, Tashiro T, Shakudo M, Ohata K (2000) Rathke’s cleft cyst associated with hypophysitis: MRI. Neuroradiology 42:532–534
Hama S, Arita K, Tominaga A, Yoshikawa M, Eguchi K, Sumida M, Inai K, Nishisaka T, Kurisu K (1999) Symptomatic Rathke’s cleft cyst coexisting with central diabetes insipidus and hypophysitis: case report. Endocr J 46:187–192
Oka H, Kawano N, Yagishita S, Kobayashi I, Saegusa H, Fujii K (1997) Ciliated craniopharyngioma indicates histogenetic relationship to Rathke cleft epithelium. Clin Neuropathol 16:103–106
Hama S, Arita K, Nishisaka T, Fukuhara T, Tominaga A, Sugiyama K, Yoshioka H, Eguchi K, Sumida M, Heike Y, Kurisu K (2002) Changes in the epithelium of Rathke cleft cyst associated with inflammation. J Neurosurg 96:209–216
Byun WM, Kim OL, Kim D (2000) MR imaging findings of Rathke’s cleft cysts: significance of intracystic nodules. AJNR Am J Neuroradiol 21:485–488
Sanno N, Oyama K, Tahara S, Teramoto A, Kato Y (2003) A survey of pituitary incidentaloma in Japan. Eur J Endocrinol 149:123–127
Eisenberg HM, Sarwar M, Schochet S Jr (1976) Symptomatic Rathke’s cleft cyst. Case report. J Neurosurg 45:585–588
Frank G, Sciarretta V, Mazzatenta D, Farneti G, Modugno GC, Pasquini E (2005) Transsphenoidal endoscopic approach in the treatment of Rathke’s cleft cyst. Neurosurgery 56:124–128 discussion 129
Laws ER, Kanter AS (2004) Rathke cleft cysts. J Neurosurg 101:571–572 discussion 572
Chuang CC, Chen YL, Jung SM, Pai PC (2010) A giant retroclival Rathke’s cleft cyst. J Clin Neurosci 17:1189–1191
Raper DM, Besser M (2009) Clinical features, management and recurrence of symptomatic Rathke’s cleft cyst. J Clin Neurosci 16:385–389
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
About this article
Cite this article
Han, S.J., Rolston, J.D., Jahangiri, A. et al. Rathke’s cleft cysts: review of natural history and surgical outcomes. J Neurooncol 117, 197–203 (2014). https://doi.org/10.1007/s11060-013-1272-6
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s11060-013-1272-6