Abstract
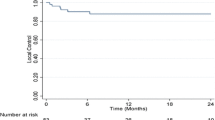
The purpose of this study is to investigate the possible role of stereotactic radiosurgery (SRS) in the management of patients with brain metastases from hepatocellular carcinoma (HCC). Thirty-two consecutive patients with 80 brain metastases from HCC were treated with SRS. Twenty-eight (87.5 %) patients were male, and the mean age of the patients was 54 ± 12 years (range 22–73). Twenty-seven (84.4 %) patients were classified as RTOG RPA Class 2. The mean tumor volume was 6.14 ± 11.3 cm3 (range 0.01–67.3). The mean marginal dose prescribed was 20.1 ± 3.6 Gy (range 10.0–25.0). The median overall survival time after SRS was 11.3 ± 5.8 weeks (95 % CI 0–22.7). A greater total volume of brain metastases (>14 cm3) was the only independent prognostic factor (HR = 2.419; 95 % CI 1.040–5.624; p = 0.040). The actuarial control rate of brain metastases was 51.3 % at 4 months after SRS. The prescribed marginal dose (>18 Gy) was significantly related with the actuarial tumor control (HR = 0.254; 95 % CI 0.089–0.725; p = 0.010). The prognosis of patients with brain metastases from HCC is dismal even with the modern technology of radiosurgery. The marginal dose prescribed should be reevaluated to improve upon the current poor local control rates.



Similar content being viewed by others
References
Han JH, Kim DG, Park JC, Chung HT, Paek SH, Chung YS (2010) Little response of cerebral metastasis from hepatocellular carcinoma to any treatments. J Korean Neurosurg Soc 47:325–331. doi:10.3340/jkns.2010.47.5.325
Seinfeld J, Wagner AS, Kleinschmidt-DeMasters BK (2006) Brain metastases from hepatocellular carcinoma in US patients. J Neurooncol 76:93–98. doi:10.1007/s11060-005-4175-3
Feng M, Ben-Josef E (2011) Radiation therapy for hepatocellular carcinoma. Semin Radiat Oncol 21:271–277. doi:10.1016/j.semradonc.2011.05.002
Bujold A, Dawson LA (2011) Stereotactic radiation therapy and selective internal radiation therapy for hepatocellular carcinoma. Cancer Radiother 15:54–63. doi:10.1016/j.canrad.2010.11.003
Andolino DL, Johnson CS, Maluccio M, Kwo P, Tector AJ, Zook J, Johnstone PA, Cardenes HR (2011) Stereotactic body radiotherapy for primary hepatocellular carcinoma. Int J Radiat Oncol Biol Phys 81:e447–e453. doi:10.1016/j.ijrobp.2011.04.011
Stintzing S, Hoffmann RT, Heinemann V, Kufeld M, Rentsch M, Muacevic A (2010) Radiosurgery of liver tumors: value of robotic radiosurgical device to treat liver tumors. Ann Surg Oncol 17:2877–2883. doi:10.1245/s10434-010-1187-9
Son SH, Choi BO, Ryu MR, Kang YN, Jang JS, Bae SH, Yoon SK, Choi IB, Kang KM, Jang HS (2010) Stereotactic body radiotherapy for patients with unresectable primary hepatocellular carcinoma: dose-volumetric parameters predicting the hepatic complication. Int J Radiat Oncol Biol Phys 78:1073–1080. doi:10.1016/j.ijrobp.2009.09.009
Han JH, Kim DG, Oh CW, Kim CY, Kim YH, Park JH, Kim EK, Jung HW (2012) Progression of the lung cancer primary correlates with the identification of new brain metastases after initial radiosurgery. J Neurooncol 106:161–167. doi:10.1007/s11060-011-0653-y
Kim WH, Kim DG, Han JH, Paek SH, Chung HT, Park CK, Kim CY, Kim YH, Kim JW, Jung HW (2011) Early significant tumor volume reduction after radiosurgery in brain metastases from renal cell carcinoma results in long-term survival. Int J Radiat Oncol Biol Phys. doi:10.1016/j.ijrobp.2011.03.044
Han JH, Kim DG, Chung HT, Paek SH, Park CK, Jung HW (2011) Radiosurgery for large brain metastases. Int J Radiat Oncol Biol Phys. doi:10.1016/j.ijrobp.2011.06.1965
Han JH, Kim DG, Chung HT, Kim CY, Park CK, Chung YS, Paek SH, Yoo MW, Kim BH, Jung HW (2010) Radiosurgery for brain metastasis from advanced gastric cancer. Acta Neurochir (Wien) 152:605–610. doi:10.1007/s00701-009-0554-4
Han JH, Kim DG, Chung HT, Park CK, Paek SH, Kim CY, Jung HW (2008) Gamma knife radiosurgery for skull base meningiomas: long-term radiologic and clinical outcome. Int J Radiat Oncol Biol Phys 72:1324–1332. doi:10.1016/j.ijrobp.2008.03.028
Kano H, Kondziolka D, Lobato-Polo J, Zorro O, Flickinger JC, Lunsford LD (2010) T1/T2 matching to differentiate tumor growth from radiation effects after stereotactic radiosurgery. Neurosurgery 66:486–491. doi:10.1227/01.NEU.0000360391.35749.A5 discussion 491–482
Shaw E, Scott C, Souhami L, Dinapoli R, Kline R, Loeffler J, Farnan N (2000) Single dose radiosurgical treatment of recurrent previously irradiated primary brain tumors and brain metastases: final report of RTOG protocol 90–05. Int J Radiat Oncol Biol Phys 47:291–298
Patchell RA, Tibbs PA, Walsh JW, Dempsey RJ, Maruyama Y, Kryscio RJ, Markesbery WR, Macdonald JS, Young B (1990) A randomized trial of surgery in the treatment of single metastases to the brain. N Engl J Med 322:494–500. doi:10.1056/NEJM199002223220802
Llovet JM, Bruix J (2003) Systematic review of randomized trials for unresectable hepatocellular carcinoma: chemoembolization improves survival. Hepatology 37:429–442. doi:10.1053/jhep.2003.50047
McIntire KR, Vogel CL, Primack A, Waldmann TA, Kyalwazi SK (1976) Effect of surgical and chemotherapeutic treatment on alpha-fetoprotein levels in patients with hepatocellular carcinoma. Cancer 37:677–683
Wulf J, Guckenberger M, Haedinger U, Oppitz U, Mueller G, Baier K, Flentje M (2006) Stereotactic radiotherapy of primary liver cancer and hepatic metastases. Acta Oncol 45:838–847. doi:10.1080/02841860600904821
Tse RV, Hawkins M, Lockwood G, Kim JJ, Cummings B, Knox J, Sherman M, Dawson LA (2008) Phase I study of individualized stereotactic body radiotherapy for hepatocellular carcinoma and intrahepatic cholangiocarcinoma. J Clin Oncol 26:657–664. doi:10.1200/jco.2007.14.3529
Kress MA, Oermann E, Ewend MG, Hoffman RB, Chaudhry H, Collins B (2013) Stereotactic radiosurgery for single brain metastases from non-small cell lung cancer: progression of extracranial disease correlates with distant intracranial failure. Radiat oncol 8:64. doi:10.1186/1748-717X-8-64
Neal MT, Chan MD, Lucas JT Jr, Loganathan A, Dillingham C, Pan E, Stewart JHt, Bourland JD, Shaw EG, Tatter SB, Ellis TL (2013) Predictors of survival, neurologic death, local failure, and distant failure after gamma knife radiosurgery for melanoma brain metastases. World neurosurg. doi:10.1016/j.wneu.2013.02.025
Simonova G, Novotny J, Novotny J Jr, Vladyka V, Liscak R (1995) Fractionated stereotactic radiotherapy with the Leksell gamma knife: feasibility study. Radiother Oncol 37:108–116. doi:016781409501632Q
Hiraoka A, Horiike N, Koizumi Y, Tazuya N, Ichiryu M, Nakahara H, Ochi H, Tanabe A, Doi H, Kodama A, Hasebe A, Ichikawa S, Miyamoto Y, Ninomiya T, Asagi A, Matsubara H, Nadano S, Nishizaki O, Umeda M (2008) Brain metastasis from hepatocellular carcinoma treated with a cyber-knife. Intern Med 47:1993–1996
Wegner RE, Leeman JE, Kabolizadeh P, Rwigema JC, Mintz AH, Burton SA, Heron DE (2013) Fractionated stereotactic radiosurgery for large brain metastases. Am J Clin Oncol. doi:10.1097/COC.0b013e31828aadac
Ogura K, Mizowaki T, Ogura M, Sakanaka K, Arakawa Y, Miyamoto S, Hiraoka M (2012) Outcomes of hypofractionated stereotactic radiotherapy for metastatic brain tumors with high risk factors. J Neurooncol 109:425–432. doi:10.1007/s11060-012-0912-6
Lee DS, Kim YS, Lee CG, Lim JH, Suh CO, Kim HJ, Cho J (2013) Early volumetric change and treatment outcome of metastatic brain tumors after external beam radiotherapy: differential radiotherapy for brain metastasis. Clinical & translational oncology: official publication of the Federation of Spanish Oncology Societies and of the National Cancer Institute of Mexico. doi:10.1007/s12094-013-1016-2
Mathieu D, Kondziolka D, Cooper PB, Flickinger JC, Niranjan A, Agarwala S, Kirkwood J, Lunsford LD (2007) Gamma knife radiosurgery in the management of malignant melanoma brain metastases. Neurosurgery 60:471–481. doi:10.1227/01.NEU.0000255342.10780.52 discussion 481–472
Acknowledgments
This study was supported by grant no. 02-2011-006 from the SNUBH Research Fund.
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
About this article
Cite this article
Han, J.H., Kim, D.G., Chung, HT. et al. Stereotactic radiosurgery for brain metastases from hepatocellular carcinoma. J Neurooncol 115, 45–51 (2013). https://doi.org/10.1007/s11060-013-1192-5
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s11060-013-1192-5