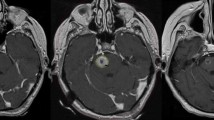
Abstract
Stereotactic Radiotherapy (SRT) is more commonly used for skull base tumors in conjunction with the technical development of radiation intensity modulation. Purpose of this study is to correlate clinical and radiographic characteristics of delayed radiation injury (RI) occurring around central skull base following SRT with SRT dosimetric data. Total of six patients were identified to have developed RI in the vicinity of SRT target volume out of 141 patients who received SRT in he center or near-center of the skull base. The images and medical records were retrospectively reviewed. The analysis was performed for RI location, time of development, imaging and clinical characteristics and evolution of RI and correlated with SRT dosimetric analysis using image fusion with follow-up MRI scans. Mean follow-up time was 24 ± 9 months. During the follow-up period, twelve sites of RI were found in 6 patients. They were clinically symptomatic in 4/6 patients (66.6%) at median 12.5 months after SRT. Mean time interval between SRT and detection of RI was 9 ± 3, 18.5 ± 5, and 13.5 months for brainstem, temporal lobe, and cerebellum/labyrinth lesions, respectively. All RI lesions were included in the region of high SRT doses. After steroid and symptomatic treatment, 50% of RI lesions showed complete response, and 40% showed partial response. RI can occur around the skull base because of irregular shape of target tumor, its close proximity to normal brain parenchyma, and inhomogeneity of dose distribution. Brainstem lesions occurred earlier than temporal lobe RI. The majority of the RI lesions, not mixed with the tumor in this study, showed radiographic and clinical improvement with steroid and symptomatic treatments.



Similar content being viewed by others
References
Ryu S, Khan M, Yin FF et al (2004) Image guided radiosurgery of head and neck cancers. Otolaryngol Head Neck Surg 30(6):690–697
Ryu S, Fang YF, Rock J et al (2003) Image-guided and intensity-modulated radiosurgery for patients with spinal metastasis. Cancer 97(8):2013–2018
Macdonald DR, Cascino TL, Schold SC et al (1990) Response criteria for phase II studies of malignant glioma. J Clin Oncol 8:1277–1280
Djalilian HR, Benson AG, Ziai K et al (2007) Radiation necrosis of the brain after radiosurgery for vestibular schwannoma. Am J Otolaryng 28:338–341
Monheit BE, Fiveash JB, Girkin CA et al (2004) Radionecrosis of the inferior occipital lobes with altitudinal visual field loss after gamma knife radiosurgery. J Neuroophthalmol 24(3):195–199
Takenaka N, Imanishi T, Sasaki H et al (2003) Delayed radiation necrosis with extensive brain edema after gamma knife radiosurgery for multiple cerebral cavernous malformations: case report. Neurol Med Chir (Tokyo) 43(8):391–395
Lorenzo ND, Nolletti A, Palma L et al (1978) Late cerebral radionecrosis. Surg Neurol 10(5):281–290
Al-Mefty O, Kersh JE, Routh A et al (1990) The long-term side effects of radiation therapy for benign brain tumors in adults. J Neurosurg 73(4):502–512
Kumar AJ, Leeds NE, Fuller GN et al (2000) Malignant gliomas: MR imaging spectrum of radiation therapy and chemotherapy-induced necrosis of the brain after treatment. Radiology 217:377–384
Mullins ME, Barest GD, Schaefer PW et al (2005) Radiation necrosis versus glioma recurrence: conventional MR imaging clues to diagnosis. Am J Neuroradiol 26(8):1967–1972
Rogers LR, Scarpace L, Gutierrez J et al (2006) Magnetic resonance imaging characteristics and histological correlates of cerebral radiation necrosis. Neurology 66(S2):335
Chong VF, Rumpel H, Aw YS et al (1999) Temporal lobe necrosis following radiation therapy for nasopharyngeal carcinoma: 1H MR spectroscopic findings. Int J Radiat Oncol Biol Phys 45:699–705
Graves EE, Nelson SJ, Vigneron DB et al (2001) Serial proton MR spectroscopic imaging of recurrent malignant gliomas after gamma knife radiosurgery. Am J Neuroradiol 22:613–624
Cha S (2003) Perfusion MR imaging: basic principles and clinical applications. Magn Reson Imaging Clin N Am 11(3):403–413
Jain R, Scarpace L, Ellika S et al (2007) First-pass perfusion computed tomography: initial experience in differentiating recurrent brain tumors from radiation effects and radiation necrosis. Neurosurgery 61:778–787
Langleben DD, Segall GM (2000) PET in differentiation of recurrent brain tumor from radiation injury. J Nucl Med 41:1861–1867
Chao ST, Suh JH, Raja S et al (2001) The sensitivity and specificity of FDG PET in distinguishing recurrent brain tumor from radionecrosis in patients treated with stereotactic radiosurgery. Int J Cancer 96(3):191–197
Stokkel M, Stevens H, Taphoorn M et al (1999) Differentiation between recurrent brain tumour and post-radiation necrosis: the value of 201Tl SPET versus 18F-FDG PET using a dual-headed coincidence camera–a pilot study. Nucl Med Commun 20(5):411–417
Karlsson B, Lax I, Soderman N et al (1997) Factors influencing the risk for complications following Gamma Knife radiosurgery of cerebral arteriovenous malformations. Radiother Oncol 43(3):275–280
Chin LS, Ma L, Di Biase S et al (2001) Radiation necrosis following gamma knife surgery: a case-controlled comparison of treatment parameters and long-term clinical follow up. J Neurosurg 94(6):899–904
Flickinger JC, Kondziolka D, Pollock BE et al (1997) Complications from arteriovenous malformation radiosurgery: multivariate analysis and risk modeling. Int J Radiat Oncol Biol Phys 8(3):485–490
Flickinger JC, Kondziolka D, Maitz AH et al (1998) Analysis of neurological sequelae from radiosurgery of arteriovenous malformations: how location affects outcome. Int J Radiat Oncol Biol Phys 40(2):273–278
Flickinger JC, Kondziolka D, Lunsford LD et al (2000) Development of a model to predict permanent symptomatic postradiosurgery injury for arteriovenous malformation patients. Arteriovenous Malformation Radiosurgery Study Group. Int J Radiat Oncol Biol Phys 46(5):1143–1148
Voges J, Treuer H, Sturm V et al (1996) Risk analysis of linear accelerator radiosurgery. Int J Radiat Oncol Biol Phys 36(5):1055–1063
Levegrün S, Hof H, Essig M et al (2004) Radiation-induced changes of brain tissue after radiosurgery in patients with arteriovenous malformations: correlation with dose distribution parameters. Int J Radiat Oncol Biol Phys 59(3):796–808
Wanebo JE, Kidd GA, King MC et al (2009) Hyperbaric oxygen therapy for treatment of adverse radiation effects after stereotactic radiosurgery of arteriovenous malformations: case report and review of literature. Surg Neurol 72(2):162–167
Chuba PJ, Aronin P, Bhambhani K et al (1997) Hyperbaric oxygen therapy for radiation-induced brain injury in children. Cancer 80:2005–2012
Ka Leber, Eder HG, Kovac H et al (1998) Treatment of cerebral radionecrosis by hyperbaric oxygen therapy. Stereotact Funct Neurosurg 70(Suppl 1):229–236
Lynn M, Friedman WA (2007) Hyperbaric oxygen in the treatment of a radiosurgical complication: technical case report. Neurosurgery 60(3):E579
Hyperbaric and Undersea Medicine Society Indications for hyperbaric oxygen therapy. http://www.uhms.org. Accessed September 25 2009
Williamson R, Kondziolka D, Kanaan H et al (2008) Adverse radiation effects after radiosurgery may benefit from oral vitamin E and Pentoxifylline therapy: a pilot study. Stereotact Funct Neurosurg 6(6):359–366
Delanian S, Lefaix JL, Maisonobe T et al (2008) Significant clinical improvement in radiation-induced lumbosacral polyradiculopathy by a treatment combining pentoxifylline, tocopherol, and clodronate (Pentoclo). J Neurol Sci 275(1–2):164–166
Kim JH, Brown SL, Kolozsvary A et al (2004) Modification of radiation injury by ramipril, inhibitor of angiotensin-converting enzyme, on optic neuropathy in the rat. Radiat Res 161(2):137–142
Ryu S, Kolozsvary A, Jenrow KA et al (2007) Mitigation of radiation-induced optic neuropathy in rats by ACE inhibitor ramipril: importance of ramipril dose and treatment time. J Neurooncol 82(2):119–124
Diomede L, Albani D, Sottocorno M et al (2001) In vivo anti-inflammatory effect of statins is mediated by nonsterol mevalonate products. Arterioscler Thromb Vasc Biol 21(8):1327–1332
Shishehbor MH, Brennan ML, Aviles RJ et al (2003) Statins promote potent systemic antioxidant effects through specific inflammatory pathways. Circulation 108(4):426–431
Chen J, Zhang ZG, Li Y et al (2003) Statins induce angiogenesis, neurogenesis, and synaptogenesis after stroke. Ann Neurol 53(6):743–751 (Erratum in: Ann Neurol 2005;58(5):818)
Gonzalez J, Kumar AJ, Conrad CA et al (2007) Effect of bevacizumab on radiation necrosis of the brain. Int J Radiat Oncol Biol Phys 67(2):323–326
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
About this article
Cite this article
Schipani, S., Jain, R., Shah, K. et al. Clinical, dosimetric, and radiographic correlation of radiation injury involving the brainstem and the medial temporal lobes following stereotactic radiotherapy for neoplasms of central skull base. J Neurooncol 98, 177–184 (2010). https://doi.org/10.1007/s11060-010-0171-3
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s11060-010-0171-3