Abstract
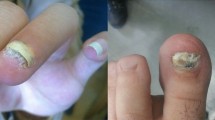
Neoscytalidium dimidiatum is an opportunistic fungus causing cutaneous infections mostly, which are difficult to treat due to antifungal resistance. In Malaysia, N. dimidiatum is associated with skin and nail infections, especially in the elderly. These infections may be mistaken for dermatophyte infections due to similar clinical appearance. In this study, Neoscytalidium isolates from cutaneous specimens, identified using morphological and molecular methods (28 Neoscytalidium dimidiatum and 1 Neoscytalidium sp.), were evaluated for susceptibility towards antifungal agents using the CLSI broth microdilution (M38-A2) and Etest methods. Amphotericin B, voriconazole, miconazole and clotrimazole showed high in vitro activity against all isolates with MIC ranging from 0.0313 to 1 µg/mL. Susceptibility towards fluconazole and itraconazole was noted in up to 10% of isolates, while ketoconazole was inactive against all isolates. Clinical breakpoints for antifungal drugs are not yet available for most filamentous fungi, including Neoscytalidium species. However, the results indicate that clinical isolates of N. dimidiatum in Malaysia were sensitive towards miconazole, clotrimazole, voriconazole and amphotericin B, in vitro.



Similar content being viewed by others
References
Havlickova B, Czaika VA, Friedrich M. Epidemiological trends in skin mycoses worldwide. Mycoses. 2008;51(Suppl 4):2–15. doi:10.1111/j.1439-0507.2008.01606.x.
Crous PW, Slippers B, Wingfield MJ, Rheeder J, Marasas WF, Philips AJ, et al. Phylogenetic lineages in the Botryosphaeriaceae. Stud Mycol. 2006;55:235–53.
Gentles JC, Evans EG. Infection of the feet and nails with Hendersonula toruloidea. Sabouraudia. 1970;8(1):72–5.
Bunyaratavej S, Prasertworonun N, Leeyaphan C, Chaiwanon O, Muanprasat C, Matthapan L. Distinct characteristics of Scytalidium dimidiatum and non-dermatophyte onychomycosis as compared with dermatophyte onychomycosis. J Dermatol. 2015;. doi:10.1111/1346-8138.12768.
Arrese JE, Pierard-Franchimont C, Pierard GE. Scytalidium dimidiatum melanonychia and scaly plantar skin in four patients from the Maghreb: imported disease or outbreak in a Belgian mosque? Dermatology. 2001;202(2):183–5.
Moore MK. Skin and nail infections by non-dermatophytic filamentous fungi. Mykosen Suppl. 1978;1:128–32.
Oyeka CA, Okoli I. Isolation of dermatophytes and non-dermatophytic fungi from soil in Nigeria. Mycoses. 2003;46(8):336–8.
Menotti J, Machouart M, Benderdouche M, Cetre-Sossah C, Morel P, Dubertret L, et al. Polymerase chain reaction for diagnosis of dermatophyte and Scytalidium spp. onychomycosis. Br J Dermatol. 2004;151(2):518–9. doi:10.1111/j.1365-2133.2004.06089.x.
Elinav H, Izhar U, Benenson S, Admon D, Hidalgo-Grass C, Polacheck I, et al. Invasive Scytalidium dimidiatum infection in an immunocompetent adult. J Clin Microbiol. 2009;47(4):1259–63. doi:10.1128/JCM.01874-08.
Hariri A, Choudhury N, Saleh HA. Scytalidium dimidiatum associated invasive fungal sinusitis in an immunocompetent patient. J Laryngol Otol. 2014;128(11):1018–21. doi:10.1017/S002221511400214X.
Ng KP, Saw TL, Madasamy M, Soo Hoo T. Onychomycosis in Malaysia. Mycopathologia. 1999;147(1):29–32.
Ungpakorn R. Mycoses in Thailand: current concerns. Jpn J Med Mycol. 2005;46(2):81–6.
Lacroix C, de Chauvin MF. In vitro activity of amphotericin B, itraconazole, voriconazole, posaconazole, caspofungin and terbinafine against Scytalidium dimidiatum and Scytalidium hyalinum clinical isolates. J Antimicrob Chemother. 2008;61(4):835–7. doi:10.1093/jac/dkn011.
Madrid H, Ruiz-Cendoya M, Cano J, Stchigel A, Orofino R, Guarro J. Genotyping and in vitro antifungal susceptibility of Neoscytalidium dimidiatum isolates from different origins. Int J Antimicrob Agents. 2009;34(4):351–4. doi:10.1016/j.ijantimicag.2009.05.006.
Bueno JG, Martinez C, Zapata B, Sanclemente G, Gallego M, Mesa AC. In vitro activity of fluconazole, itraconazole, voriconazole and terbinafine against fungi causing onychomycosis. Clin Exp Dermatol. 2010;35(6):658–63. doi:10.1111/j.1365-2230.2009.03698.x.
Messer SA, Diekema DJ, Hollis RJ, Boyken LB, Tendolkar S, Kroeger J, et al. Evaluation of disk diffusion and Etest compared to broth microdilution for antifungal susceptibility testing of posaconazole against clinical isolates of filamentous fungi. J Clin Microbiol. 2007;45(4):1322–4. doi:10.1128/JCM.02450-06.
European Committee on Antimicrobial Susceptibility Testing, Breakpoint tables for interpretation of MICs, Version 7.0. www.eucast.org/clinical_breakpoints. 2014. Accessed 24 January 2015.
de Hoog GS, Guarro J, Gené J, Figueras MJ. Atlas of clinical fungi. Utrecht: Centraalbureau voor Schimmelcultures; 2000.
Yazdanparast SA, Barton RC. Arthroconidia production in Trichophyton rubrum and a new ex vivo model of onychomycosis. J Med Microbiol. 2006;55(Pt 11):1577–81. doi:10.1099/jmm.0.46474-0.
Oycka CA, Gugnani HC. Keratin degradation by Scytalidium species and Fusarium solani. Mycoses. 1998;41(1–2):73–6.
Marriott DJ, Wong KH, Aznar E, Harkness JL, Cooper DA, Muir D. Scytalidium dimidiatum and Lecythophora hoffmannii: unusual causes of fungal infections in a patient with AIDS. J Clin Microbiol. 1997;35(11):2949–52.
Sigler L, Summerbell RC, Poole L, Wieden M, Sutton DA, Rinaldi MG, et al. Invasive Nattrassia mangiferae infections: case report, literature review, and therapeutic and taxonomic appraisal. J Clin Microbiol. 1997;35(2):433–40.
Lacaz CS, Pereira AD, Heins-Vaccari EM, Cuce LC, Benatti C, Nunes RS, et al. Onychomycosis caused by Scytalidium dimidiatum. Report of two cases. Review of the taxonomy of the synanamorph and anamorph forms of this coelomycete. Rev Inst Med Trop Sao Paulo. 1999;41(5):319–23.
Roeijmans HJ, De Hoog GS, Tan CS, Figge MJ. Molecular taxonomy and GC/MS of metabolites of Scytalidium hyalinum and Nattrassia mangiferae (Hendersonula toruloidea). J Med Vet Mycol. 1997;35(3):181–8.
Morris-Jones R, Youngchim S, Hextall JM, Gomez BL, Morris-Jones SD, Hay RJ, et al. Scytalidium dimidiatum causing recalcitrant subcutaneous lesions produces melanin. J Clin Microbiol. 2004;42(8):3789–94. doi:10.1128/JCM.42.8.3789-3794.2004.
Hay RJ. Scytalidium infections. Curr Opin Infect Dis. 2002;15(2):99–100.
van Duin D, Casadevall A, Nosanchuk JD. Melanization of Cryptococcus neoformans and Histoplasma capsulatum reduces their susceptibilities to amphotericin B and caspofungin. Antimicrob Agents Chemother. 2002;46(11):3394–400.
Ikeda R, Sugita T, Jacobson ES, Shinoda T. Effects of melanin upon susceptibility of Cryptococcus to antifungals. Microbiol Immunol. 2003;47(4):271–7.
Kondori N, Svensson E, Mattsby-Baltzer I. In vitro susceptibility of filamentous fungi to itraconazole, voriconazole and posaconazole by Clinical and Laboratory Standards Institute reference method and E-test. Mycoses. 2011;54(5):e318–22. doi:10.1111/j.1439-0507.2010.01913.x.
Espinel-Ingroff A, Rezusta A. E-test method for testing susceptibilities of Aspergillus spp. to the new triazoles voriconazole and posaconazole and to established antifungal agents: comparison with NCCLS broth microdilution method. J Clin Microbiol. 2002;40(6):2101–7.
Tortorano AM, Prigitano A, Esposto MC, Arsic Arsenijevic V, Kolarovic J, Ivanovic D, et al. European Confederation of Medical Mycology (ECMM) epidemiological survey on invasive infections due to Fusarium species in Europe. Eur J Clin Microbiol Infect Dis. 2014;. doi:10.1007/s10096-014-2111-1.
Elinav H, Izhar U, Benenson S, Admon D, Hidalgo-Grass C, Polacheck I, et al. Invasive Scytalidium dimidiatum infection in an immunocompetent adult. J Clin Microbiol. 2009;47(4):1259–63. doi:10.1128/JCM.01874-08.
Yew SM, Chan CL, Lee KW, Na SL, Tan R, Hoh CC, et al. A five-year survey of dematiaceous fungi in a tropical hospital reveals potential opportunistic species. PLoS ONE. 2014;9(8):e104352. doi:10.1371/journal.pone.0104352.
Garinet S, Tourret J, Barete S, Arzouk N, Meyer I, Frances C, et al. Invasive cutaneous Neoscytalidium infections in renal transplant recipients: a series of five cases. BMC Infect Dis. 2015;15:535. doi:10.1186/s12879-015-1241-0.
Spriet I, Lambrecht C, Lagrou K, Verhamme B. Successful eradication of Scytalidium dimidiatum-induced ungual and cutaneous infection with voriconazole. Eur J Dermatol. 2012;22(2):197–9. doi:10.1684/ejd.2011.1616.
Benne CA, Neeleman C, Bruin M, de Hoog GS, Fleer A. Disseminating infection with Scytalidium dimidiatum in a granulocytopenic child. Eur J Clin Microbiol Infect Dis. 1993;12(2):118–21.
Guarro J, Pujol I, Aguilar C, Ortoneda M. In vitro antifungal susceptibility of nondermatophytic keratinophilic fungi. Revista Iberoamericana de Micologia. 2000:142–147.
Khan ZU, Ahmad S, Joseph L, Chandy R. Cutaneous phaeohyphomycosis due to Neoscytalidium dimidiatum: first case report from Kuwait. J Mycol Med. 2009;19(2):138–42. doi:10.1016/j.mycmed.2009.02.005.
Oyeka CA, Gugnani HC. Isoconazole nitrate versus clotrimazole in foot and nail infections due to Hendersonula toruloidea, Scytalidium hyalinum and dermatophytes. Mycoses. 1992;35(11–12):357–61.
Moore MK, del Palacio-Hernanz AD, Lopez-Gomez S. Scytalidium hyalinum infection diagnosed in Spain. Sabouraudia. 1984;22(3):243–5.
Santhanam J, Nazmiah N, Aziz MN. Species distribution and antifungal susceptibility patterns of Candida species: is low susceptibility to itraconazole a trend in Malaysia? Med J Malays. 2013;68(4):343–7.
Levi ME, Smith JW. Posttraumatic infection due to Scytalidium dimidiatum. Clin Infect Dis. 1994;18(1):127–8.
Hay RJ. Ketoconazole in the treatment of fungal infection. Clinical and laboratory studies. Am J Med. 1983;74(1B):16–9.
Aamir S, Aman S, Haroon T. Mycetoma caused by Scytalidium dimidiatum. Br J Dermatol. 2003;148(1):174–6.
Gumbo T, Mkanganwi N, Robertson VJ, Masvaire P. Case report. Nattrassia mangiferae endophthalmitis. Mycoses. 2002;45(3–4):118–9.
Grau S, Pozo J, Roma E, Salavert M, Barrueta J, Peral C, et al. Pharmacoeconomic analysis of anidulafungin, micafungin, caspofungin and fluconazole in the treatment of candidemia and/or invasive candidiasis in non-neutropenic adult patients In Spain. Value Health. 2015;18(7):A584–5. doi:10.1016/j.jval.2015.09.1961.
Branco J, Silva AP, Silva RM, Silva-Dias A, Pina-Vaz C, Butler G, et al. Fluconazole and voriconazole resistance in Candida parapsilosis is conferred by gain-of-function mutations in MRR1 transcription factor gene. Antimicrob Agents Chemother. 2015;59(10):6629–33. doi:10.1128/AAC.00842-15.
Farjo QA, Farjo RS, Farjo AA. Scytalidium keratitis: case report in a human eye. Cornea. 2006;25(10):1231–3. doi:10.1097/01.ico.0000230323.28956.b9.
Acknowledgements
We would like to thank Pharmaniaga (Malaysia) for providing antifungal agents for this study. This work was fully funded by a Research University Grant UKM-GUP-2011-118 from Universiti Kebangsaan Malaysia.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
This study is in compliance with institutional ethical requirements of Universiti Kebangsaan Malaysia.
Conflict of interest
The authors declare that they have no conflict of interest.
Rights and permissions
About this article
Cite this article
James, J.E., Santhanam, J., Lee, M.C. et al. In Vitro Antifungal Susceptibility of Neoscytalidium dimidiatum Clinical Isolates from Malaysia. Mycopathologia 182, 305–313 (2017). https://doi.org/10.1007/s11046-016-0085-5
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s11046-016-0085-5