Abstract
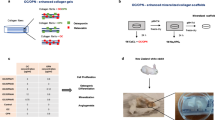
Proper bony tissue regeneration requires mechanical stabilization, an osteogenic biological activity and appropriate scaffolds. The latter two elements can be combined in a hydrogel format for effective delivery, so it can readily adapt to the architecture of the defect. We evaluated a Good Manufacturing Practice-compliant formulation composed of bone marrow-derived mesenchymal stromal cells in combination with bone particles (Ø = 0.25 to 1 µm) and fibrin, which can be readily translated into the clinical setting for the treatment of bone defects, as an alternative to bone tissue autografts. Remarkably, cells survived with unaltered phenotype (CD73+, CD90+, CD105+, CD31−, CD45−) and retained their osteogenic capacity up to 48 h after being combined with hydrogel and bone particles, thus demonstrating the stability of their identity and potency. Moreover, in a subchronic toxicity in vivo study, no toxicity was observed upon subcutaneous administration in athymic mice and signs of osteogenesis and vascularization were detected 2 months after administration. The preclinical data gathered in the present work, in compliance with current quality and regulatory requirements, demonstrated the feasibility of formulating an osteogenic cell-based tissue engineering product with a defined profile including identity, purity and potency (in vitro and in vivo), and the stability of these attributes, which complements the preclinical package required prior to move towards its use of prior to its clinical use.



Similar content being viewed by others
Data availability
All datasets generated for this study are included in the manuscript and the supplementary files.
Abbreviations
- ALP:
-
Alkaline phosphatase
- BM:
-
Bone Marrow
- DMEM:
-
Dulbecco’s Modified Eagle’s Medium
- EPC:
-
Endothelial progenitor cells
- GMP:
-
Good Manufacturing Practice
- HLA:
-
Human Leukocyte Antigen
- HPC:
-
Hematopoietic stem progenitor cells
- HSA:
-
Human serum albumin
- MNC:
-
Mononuclear cell
- MSC:
-
Multipotent Mesenchymal Stromal Cells
- P:
-
Passage number
- PBMC:
-
Peripheral Blood Mononuclear Cells
- TEP:
-
Tissue Engineering Product
References
Giannoudis PV, Einhorn TA, Marsh D (2007) Fracture healing: the diamond concept. Injury 38(Suppl 4):S3–S6
Dias MI, Lourenco P, Rodrigues A, Azevedo J, Viegas C, Ferreira A et al (2007) The effect of the quantitative variation of autologous spongy bone graft applied for bone regeneration in an experimental model of tibia osteotomy. Acta Med Port 20(1):37–46
Wheeler DL, Enneking WF (2005) Allograft bone decreases in strength in vivo over time. Clin Orthop Relat Res 435:36–42
Chou LB, Mann RA, Coughlin MJ, McPeake WT 3rd, Mizel MS (2007) Stress fracture as a complication of autogenous bone graft harvest from the distal tibia. Foot Ankle Int 28(2):199–201
Prat S, Gallardo-Villares S, Vives M, Carreño A, Caminal M, Oliver-Vila I et al (2018) Clinical translation of a mesenchymal stromal cell-based therapy developed in a large animal model and two case studies of the treatment of atrophic pseudoarthrosis. J Tissue Eng Regen Med 12(1):e532–e540
Caminal M, Velez R, Rabanal RM, Vivas D, Batlle-Morera L, Aguirre M et al (2017) A reproducible method for the isolation and expansion of ovine mesenchymal stromal cells from bone marrow for use in regenerative medicine preclinical studies. J Tissue Eng Regen Med 11(12):3408–3416
Hernigou P, Poignard A, Beaujean F, Rouard H (2005) Percutaneous autologous bone-marrow grafting for nonunions. Influence of the number and concentration of progenitor cells. J Bone Joint Surg Am 87(7):1430–1437
Hernigou P, Beaujean F (2002) Treatment of osteonecrosis with autologous bone marrow grafting. Clin Orthop Relat Res 405:14–23
Vives J, Mirabel C (2019) Multipotent mesenchymal stromal cells from bone marrow for current and potential clinical applications. In: Reis RL (ed) Encyclopedia of tissue engineering and regenerative medicine. Academic Press, Oxford, pp 503–512
Codinach M, Blanco M, Ortega I, Lloret M, Reales L, Coca MI et al (2016) Design and validation of a consistent and reproducible manufacture process for the production of clinical-grade bone marrow-derived multipotent mesenchymal stromal cells. Cytotherapy 18(9):1197–1208
López Fernández A, Barro V, Ortiz-Hernández M, Manzanares-Céspedes MC, Vivas D, Vives J et al (2020) Effect of allogeneic cell-based tissue engineered treatments in a sheep osteonecrosis model. Tissue Eng Part A. https://doi.org/10.1089/ten.TEA.2019.0339
Caminal M, Vélez R, Rabanal RM, Vivas D, Batlle-Morera L, Aguirre M et al (2017) A reproducible method for the isolation and expansion of ovine mesenchymal stromal cells from bone marrow for use in regenerative medicine preclinical studies. J Tissue Eng Regen Med 11(12):3408–3416
Oliver-Vila I, Coca MI, Grau-Vorster M, Pujals-Fonts N, Caminal M, Casamayor-Genesca A et al (2016) Evaluation of a cell-banking strategy for the production of clinical grade mesenchymal stromal cells from Wharton's jelly. Cytotherapy 18(1):25–35
Caminal M, Peris D, Fonseca C, Barrachina J, Codina D, Rabanal RM et al (2016) Cartilage resurfacing potential of PLGA scaffolds loaded with autologous cells from cartilage, fat, and bone marrow in an ovine model of osteochondral focal defect. Cytotechnology 68(4):907–919
Mirabel C, Puente-Massaguer E, Del Mazo-Barbara A, Reyes B, Morton P, Gòdia F et al (2018) Stability enhancement of clinical grade multipotent mesenchymal stromal cell-based products. J Transl Med 16(1):291
Cash JM, Remmers EF, Goldmuntz EA, Crofford LJ, Zha H, Hansen CT et al (1993) Genetic mapping of the athymic nude (RNU) locus in the rat to a region on chromosome 10. Mamm Genome 4(1):37–42
Zachos TA, Bertone AL, Wassenaar PA, Weisbrode SE (2007) Rodent models for the study of articular fracture healing. J Invest Surg 20(2):87–95
Davies G, Grant AG, Duke D, Hermon-Taylor J (1983) Antibody response of nude (RNU/RNU) and hairy (RNU/+) rats to circulating cell surface components from human pancreatic cancer xenografts. Br J Cancer 48(2):239–245
Rolstad B (2001) The athymic nude rat: an animal experimental model to reveal novel aspects of innate immune responses? Immunol Rev 184:136–144
Vishnu Priya M, Sivshanmugam A, Boccaccini AR, Goudouri OM, Sun W, Hwang N et al (2016) Injectable osteogenic and angiogenic nanocomposite hydrogels for irregular bone defects. Biomed Mater 11(3):035017
Panwar A, Tan LP (2016) Current status of bioinks for micro-extrusion-based 3D bioprinting. Molecules 21(6):685
Gopinathan J, Noh I (2018) Recent trends in bioinks for 3D printing. Biomater Res 22:11
Dominici M, Le Blanc K, Mueller I, Slaper-Cortenbach I, Marini F, Krause D et al (2006) Minimal criteria for defining multipotent mesenchymal stromal cells. The International Society for Cellular Therapy position statement. Cytotherapy. 8(4):315–317
Mendicino M, Bailey AM, Wonnacott K, Puri RK, Bauer SR (2014) MSC-based product characterization for clinical trials: an FDA perspective. Cell Stem Cell 14(2):141–145
Dighe PA, Viswanathan P, Mruthunjaya AK, Seetharam RN (2013) Effect of bFGF on HLA-DR expression of human bone marrow-derived mesenchymal stem cells. J Stem Cells 8(1):43–57
Grau-Vorster M, Rodríguez L, Torrents-Zapata S, Vivas D, Codinach M, Blanco M et al (2019) Levels of IL-17F and IL-33 correlate with HLA-DR activation in clinical-grade human bone marrow-derived multipotent mesenchymal stromal cell expansion cultures. Cytotherapy 21(1):32–40
Grau-Vorster M, Laitinen A, Nystedt J, Vives J (2019) HLA-DR expression in clinical-grade bone marrow-derived multipotent mesenchymal stromal cells: a two-site study. Stem Cell Res Ther 10(1):164
Matoba S, Tatsumi T, Murohara T, Imaizumi T, Katsuda Y, Ito M et al (2008) Long-term clinical outcome after intramuscular implantation of bone marrow mononuclear cells (therapeutic angiogenesis by cell transplantation [TACT] trial) in patients with chronic limb ischemia. Am Heart J 156(5):1010–1018
Korf-Klingebiel M, Kempf T, Sauer T, Brinkmann E, Fischer P, Meyer GP et al (2008) Bone marrow cells are a rich source of growth factors and cytokines: implications for cell therapy trials after myocardial infarction. Eur Heart J 29(23):2851–2858
Friedenstein AJ, Chailakhyan RK, Gerasimov UV (1987) Bone marrow osteogenic stem cells: in vitro cultivation and transplantation in diffusion chambers. Cell Tissue Kinet 20(3):263–272
Prockop DJ (1997) Marrow stromal cells as stem cells for nonhematopoietic tissues. Science 276(5309):71–74
Pittenger MF, Mackay AM, Beck SC, Jaiswal RK, Douglas R, Mosca JD et al (1999) Multilineage potential of adult human mesenchymal stem cells. Science 284(5411):143–147
Buchta C, Dettke M, Funovics PT, Hocker P, Knobl P, Macher M et al (2004) Fibrin sealant produced by the CryoSeal FS System: product chemistry, material properties and possible preparation in the autologous preoperative setting. Vox Sang 86(4):257–262
Noori A, Ashrafi SJ, Vaez-Ghaemi R, Hatamian-Zaremi A, Webster TJ (2017) A review of fibrin and fibrin composites for bone tissue engineering. Int J Nanomed 12:4937–4961
Mankad PS, Codispoti M (2001) The role of fibrin sealants in hemostasis. Am J Surg 182(2 Suppl):21S–S28
Amrani DL, Diorio JP, Delmotte Y (2001) Wound healing Role of commercial fibrin sealants. Ann N Y Acad Sci 936:566–579
Carless PA, Anthony DM, Henry DA (2002) Systematic review of the use of fibrin sealant to minimize perioperative allogeneic blood transfusion. Br J Surg 89(6):695–703
Currie LJ, Sharpe JR, Martin R (2001) The use of fibrin glue in skin grafts and tissue-engineered skin replacements: a review. Plast Reconstr Surg 108(6):1713–1726
Liu G, Li Y, Sun J, Zhou H, Zhang W, Cui L et al (2010) In vitro and in vivo evaluation of osteogenesis of human umbilical cord blood-derived mesenchymal stem cells on partially demineralized bone matrix. Tissue Eng Part A 16(3):971–982
Cabrera-Pérez R, Monguió-Tortajada M, Gámez-Valero A, Rojas-Márquez R, Borràs FE, Roura S et al (2019) Osteogenic commitment of Wharton's jelly mesenchymal stromal cells: mechanisms and implications for bioprocess development and clinical application. Stem Cell Res Ther 10(1):356
Seebach E, Freischmidt H, Holschbach J, Fellenberg J, Richter W (2014) Mesenchymal stroma cells trigger early attraction of M1 macrophages and endothelial cells into fibrin hydrogels, stimulating long bone healing without long-term engraftment. Acta Biomater 10(11):4730–4741
Yamada Y, Ueda M, Naiki T, Takahashi M, Hata K, Nagasaka T (2004) Autogenous injectable bone for regeneration with mesenchymal stem cells and platelet-rich plasma: tissue-engineered bone regeneration. Tissue Eng 10(5–6):955–964
Yamada Y, Nakamura S, Ito K, Umemura E, Hara K, Nagasaka T et al (2013) Injectable bone tissue engineering using expanded mesenchymal stem cells. Stem Cells 31(3):572–580
Yamada Y, Nakamura S, Ito K, Kohgo T, Hibi H, Nagasaka T et al (2008) Injectable tissue-engineered bone using autogenous bone marrow-derived stromal cells for maxillary sinus augmentation: clinical application report from a 2-6-year follow-up. Tissue Eng Part A 14(10):1699–1707
Kargozar S, Mozafari M, Hashemian SJ, Brouki Milan P, Hamzehlou S, Soleimani M et al (2018) Osteogenic potential of stem cells-seeded bioactive nanocomposite scaffolds: a comparative study between human mesenchymal stem cells derived from bone, umbilical cord Wharton's jelly, and adipose tissue. J Biomed Mater Res B Appl Biomater 106(1):61–72
Shimizu T, Akahane M, Morita Y, Omokawa S, Nakano K, Kira T et al (2015) The regeneration and augmentation of bone with injectable osteogenic cell sheet in a rat critical fracture healing model. Injury 46(8):1457–1464
Ma D, Zhong C, Yao H, Liu Y, Chen F, Li J et al (2011) Engineering injectable bone using bone marrow stromal cell aggregates. Stem Cells Dev 20(6):989–999
Acknowledgements
The authors would like to acknowledge former members of Xcelia and current members of Servei de Teràpia Cel·lular (Banc de Sang i Teixits, Barcelona) for technical support and advice.
Funding
This work has been developed in the context of ADVANCE(CAT) with the support of ACCIÓ (Catalonia Trade & Investment; Generalitat de Catalunya) and the European Community under the Catalonian ERDF operational program (European Regional Development Fund) 2014-2020, Generalitat de Catalunya (Departament de Salut) PERIS Acció Instrumental de Programes de Recerca Orientats (SLT002/16/00234) and by the Spanish Cell Therapy Network (TerCel, expedient number: RD16/0011/0028). Project PI19/01788 is funded by Instituto de Salud Carlos III and co-funded by European Union (ERDF/ESF)—A way to build Europe. JV’s laboratory is awarded by the Generalitat de Catalunya as Consolidated Research Group (ref. 2017SGR719).
Author information
Authors and Affiliations
Contributions
DV, MGV, IOV and JV performed experiments and analysed data; JGL and JV conceived the study; DV and JV revised data and wrote the manuscript. All authors revised and approved the final version of the manuscript.
Corresponding author
Ethics declarations
Conflict of interest
All authors declares that they have no conflict of interest.
Ethical approval
Cells were sourced from Banc de Sang i Teixits’ Biobank (Barcelona, Spain) and had appropriate donor informed consent for use in research. Authorization issued by Hospital de la Vall d’Hebron’s Ethics Committee (Barcelona, Spain) to JV. All animal care and experimental procedures adhered to the recommendations of local, national, and European laws (Decret 214 de 1997, Real Decreto 53 de 2013, European directive 86/609/CEE of 1986, respectively) and were approved by the Universitat Autònoma de Barcelona’s Ethical Committee on Human and Animal Experimentation (Ref. No. CEAAH 1972), and registered by Generalitat de Catalunya (Reg. No. DMAiH 6967).
Additional information
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Electronic supplementary material
Below is the link to the electronic supplementary material.
Rights and permissions
About this article
Cite this article
Vivas, D., Grau-Vorster, M., Oliver-Vila, I. et al. Evaluation of a cell-based osteogenic formulation compliant with good manufacturing practice for use in tissue engineering. Mol Biol Rep 47, 5145–5154 (2020). https://doi.org/10.1007/s11033-020-05588-z
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s11033-020-05588-z