Abstract
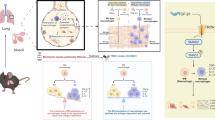
Earlier studies from our laboratory have shown myocardial dysfunction subsequent to chronic O3 exposure in rats may be associated with a decrease in antioxidant reserve and increased activity of inflammatory mediators. The present study tested the hypothesis that O3-induced cardiac dysfunction in healthy adult rats may be due to changes in caveolin-1 and caveolin-3 levels. Sprague–Dawley rats were exposed 8 h/day for 28 and 56 days to filtered air or 0.8 ppm O3. In order to assess the chronic effects to O3, in vivo cardiac function was assessed by measuring LVDP, 24 h after termination of O3 exposure. Compared to rats exposed to filtered air, LVDP values significantly decreased in all O3-exposed animals. This attenuation of cardiac function was associated with increased myocardial TNF-α levels and decreased myocardial activities of superoxidase dismutase. Progressive increases in the expression of myocardial TNF-α in 28 days and 56 days O3-exposed animals were followed by decreases in cardiac caveolin-1 levels. On the other hand, differential changes in the expression of caveolin-3 in hearts from 28 and 56 days O3-exposed animals were independent of intra-cardiac TNF-α levels. These novel findings suggest the interesting possibility that a balance between caveolin-1 and caveolin-3 may be involved in O3-mediated cardiac toxicity.





Similar content being viewed by others
References
Di Filippo C, Marfella R, Capodanno P, Ferraraccio F, Coppola L, Luongo M, Mascolo L, Luongo C, Capuano A, Rossi F, D’Amico M (2008) Acute oxygen-ozone administration to rats protects the heart from ischemia reperfusion infarct. Inflamm Res 57(10):445–449
Merin O, Attias E, Elstein D, Schwalb H, Bitran D, Zimran A, Silberman S (2007) Ozone administration reduces reperfusion injury in an isolated rat heart model. J Card Surg 22(4):339–342
Perepu RSP, Garcia C, Dostal D, Sethi R (2010) Enhanced death signaling in ozone-exposed ischemic-reperfused hearts. Mol Cell Biochem 336(1–2):55–64
Perepu RSP, Dostal DE, Garcia C, Kennedy RH, Sethi R (2012) Cardiac dysfunction subsequent to chronic ozone exposure in rats. Mol Cell Biochem 360(1–2):339–345
Das M, Cui J, Das DK (2007) Generation of survival signal by differential interaction of p38MAPKα and p38MAPKβ with caveolin-1 and caveolin-3 in the adapted heart. J Mol Cell Cardiol 42(1):206–213
Fakhrzadeh L, Laskin JD, Gardner CR, Laskin DL (2004) Superoxide dismutase-overexpressing mice are resistant to ozone-induced tissue injury and increases in nitric oxide and tumor necrosis factor-α. Am J Respir Cell Mol Biol 30(3):280–287
Kaur K, Sharma AK, Dhingra S, Singal PK (2006) Interplay of TNF-α and IL-10 in regulating oxidative stress in isolated adult cardiac myocytes. J Mol Cell Cardiol 41(6):1023–1030
Sethi R, Saini HK, Guo X, Wang X, Elimban V, Dhalla NS (2007) Dependence of changes in β-adrenoceptor signal transduction on type and stage of cardiac hypertrophy. J Appl Physiol 102(3):978–984
Hennekens CH (1998) Increasing burden of cardiovascular disease: current knowledge and future directions for research on risk factors. Circulation 97(11):1095–1102
Ruidavets J-B, Cournot M, Cassadou S, Giroux M, Meybeck M, Ferrieres J (2005) Ozone air pollution is associated with acute myocardial infarction. Circulation 111(5):563–569
Gold DR, Litonjua A, Schwartz J, Lovett E, Larson A, Nearing B, Allen G, Verrier M, Cherry R, Verrier R (2000) Ambient pollution and heart rate variability. Circulation 101(11):1267–1273
Chuang K-J, Chan C-C, Su T-C, Lee C-T, Tang C-S (2007) The effect of urban air pollution on inflammation, oxidative stress, coagulation, and autonomic dysfunction in young adults. Am J Respir Crit Care Med 176(4):370–376
Bocci V (2006) Is it true that ozone is always toxic? The end of a dogma. Toxicol Appl Pharmacol 216(3):493–504
Brook RD (2008) Cardiovascular effects of air pollution. Clin Sci (Lond) 115(6):175–187
Torre-Amione G, Kapadia S, Lee J, Durand JB, Bies RD, Young JB, Mann DL (1996) Tumor necrosis factor-α and tumor necrosis factor receptors in the failing human heart. Circulation 93(4):704–711
Bryant D, Becker L, Richardson J, Shelton J, Franco F, Peshock R, Thompson M, Giroir B (1998) Cardiac failure in transgenic mice with myocardial expression of tumor necrosis factor-α. Circulation 97(14):1375–1381
Von Haehling S, Anker SD (2005) Future prospects of anticytokine therapy in chronic heart failure. Expert Opin Investig Drugs 14(2):163–176
Deswal A, Bozkurt B, Seta Y, Parilti-Eiswirth S, Hayes FA, Blosch C, Mann DL (1999) Safety and efficacy of a soluble P75 tumor necrosis factor receptor (Enbrel, etanercept) in patients with advanced heart failure. Circulation 99(25):3224–3226
Kapadia SR, Oral H, Lee J, Nakano M, Taffet GE, Mann DL (1997) Hemodynamic regulation of tumor necrosis factor-α gene and protein expression in adult feline myocardium. Circ Res 81(2):187–195
Torre-Amione G, Stetson SJ, Youker KA, Durand JB, Radovancevic B, Delgado RM, Frazier OH, Entman ML, Noon GP (1999) Decreased expression of tumor necrosis factor-α in failing human myocardium after mechanical circulatory support: a potential mechanism for cardiac recovery. Circulation 100(11):1189–1193
Kaur K, Dhingra S, Slezak J, Sharma AK, Bajaj A, Singal PK (2009) Biology of TNFα and IL-10, and their imbalance in heart failure. Heart Fail Rev 14(2):113–123
Ballard-Croft C, Locklar AC, Kristo G, Lasley RD (2006) Regional myocardial ischemia-induced activation of MAPKs is associated with subcellular redistribution of caveolin and cholesterol. Am J Physiol Circ Physiol 291(2):H658–H667
Acknowledgments
This work was made possible by the United States Environmental Protection Agency Grant (USEPA Grant # IT-83404401-0), Texas A&M Health Science Research Development Grant (Act # 134403-35402), and funds from TAMHSC Research Startup (Act # 13100-35488). The authors would like to thank Ms. Maggie Ramirez from the TAMUK—Department of Biology and Health Sciences, Dr. Dennis Miller and Mr. Pranjal Manchanda from UT Dallas, and Mr. Vishal Sethi from UT-Pan American for reference checks, literature searches, technical help, software support, and proof reading.
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
About this article
Cite this article
Sethi, R., Manchanda, S., Perepu, R.S.P. et al. Differential expression of caveolin-1 and caveolin-3: potential marker for cardiac toxicity subsequent to chronic ozone inhalation. Mol Cell Biochem 369, 9–15 (2012). https://doi.org/10.1007/s11010-012-1363-2
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s11010-012-1363-2