Abstract
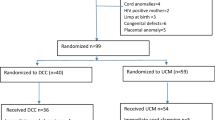
Objectives To describe the demographics, clinical characteristics and referral patterns of premature infants to a regional level IV neonatal intensive care unit (NICU); to determine the prevalence and predictors of back-transport of infants ≤ 32 weeks gestational age in a level IV NICU; for infants not back-transported closer to maternal residence, determine the length of stay beyond attainment of clinical stability. Methods Data (2010–2014) from the Children’s Hospital Neonatal Database and individual chart review for infants ≤ 32 weeks admitted to a level IV NICU whose maternal residence was outside the metro area were included. Bivariate associations of maternal and infant characteristics with back-transport were estimated using two-sample t tests and Fisher’s exact test. Multivariable logistic regression was used to measure independent predictors of back-transport. Clinical stability was defined as the attainment of full volume enteral feedings and low flow nasal cannula. Results A total of 223 infants were eligible for analysis; of whom 26% were back-transported after acute care. In the adjusted analysis, insurance status, distance from maternal residence and gestational age were significantly associated with back-transport. For infants not back-transported closer to maternal residence, median length of stay in the level IV NICU beyond attainment of clinical stability was 28.5 days. Conclusion for Practice Predictors of back-transport include private insurance, greater distance of maternal residence from NICU and younger gestational age. Many preterm infants admitted to a regional NICU for acute care remained hospitalized in a level IV NICU after achieving clinical stability, for which care in a NICU closer to maternal residence may be appropriate.


Similar content being viewed by others
References
American Academy of Pediatrics Committee on Fetus and Newborn. (2012). Levels of neonatal care. Pediatrics, 130(3), 587–597. https://doi.org/10.1542/peds.2012-1999.
Attar, M. A., Lang, S. W., Gates, M. R., Iatrow, A. M., & Bratton, S. L. (2005). Back transport of neonates: Effect on hospital length of stay. Journal of Perinatology, 25(11), 731–736. https://doi.org/10.1038/sj.jp.7211391.
Bastani, F., Abadi, T. A., & Haghani, H. (2015). Effect of family-centered care on improving parental satisfaction and reducing readmission among premature infants: A randomized controlled trial. Journal of Clinical and Diagnostic Research, 9(1), SC04–SC08. https://doi.org/10.7860/JCDR/2015/10356.5444.
Brantley, M. D., Davis, N. L., Goodman, D. A., Callaghan, W. M., & Barfield, W. D. (2017). Perinatal regionalization: A geospatial view of perinatal critical care, United States, 2010–2013. American Journal of Obstetrics and Gynecology, 216(2), 185.e1–185.e10. https://doi.org/10.1016/j.ajog.2016.10.011.
Durbin, D. R., Giardino, A. P., Shaw, K. N., Harris, M. C., & Silber, J. H. (1997). The effect of insurance status on likelihood of neonatal interhospital transfer. Pediatrics, 100(3), E8.
Goldsmit, G., Rabasa, C., Rodriguez, S., Aguirre, Y., Valdes, M., Pretz, D., et al. (2012). Risk factors associated to clinical deterioration during the transport of sick newborn infants. Argentine Archives of Pediatrics, 110(4), 304–309. https://doi.org/10.1590/S0325-00752012000400006.
Gould, J. B., Sarnoff, R., Liu, H., Bell, D. R., & Chavez, G. (1999). Very low birth weight births at non-NICU hospitals: The role of sociodemographic, perinatal, and geographic factors. Journal of Perinatology, 19(3), 197–205.
Holmstrom, S. T., & Phibbs, C. S. (2009). Regionalization and mortality in neonatal intensive care. Pediatric Clinics of North America, 56(3), 617–630. https://doi.org/10.1016/j.pcl.2009.04.006.
Jung, A. L., & Bose, C. L. (1983). Back transport of neonates: Improved efficiency of tertiary nursery bed utilization. Pediatrics, 71(6), 918–922.
Kunz, S. N., Zupancic, J. A. F., Rigdon, J., Phibbs, C. S., Lee, H. C., Gould, J. B., et al. (2017). Network analysis: A novel method for mapping neonatal acute transport patterns in California. Journal of Perinatology, 37(6), 702–708. https://doi.org/10.1038/jp.2017.20.
Latva, R., Lehtonen, L., Salmelin, R. K., & Tamminen, T. (2007). Visits by the family to the neonatal intensive care unit. Acta Paediatrica, 96(2), 215–220.
Lynch, T. M., Jung, A. L., & Bose, C. L. (1988). Neonatal back transport: Clinical outcomes. Pediatrics, 82(6), 845–851.
March of Dimes. (2016). 2016 Premature Birth Report Card. Retrieved from http://www.marchofdimes.org/materials/premature-birth-report-card-united-states.pdf.
Murthy, K., Dykes, F. D., Padula, M. A., Pallotto, E. K., Reber, K. M., Durand, D. J., et al. (2014). The Children’s Hospitals Neonatal Database: An overview of patient complexity, outcomes and variation in care. Journal of Perinatology, 34(8), 582–586. https://doi.org/10.1038/jp.2014.26.
O’Brien, K., Robson, K., Bracht, M., Cruz, M., Lui, K., Alvaro, R., et al. (2018). Effectiveness of family integrated care in neonatal intensive care units on infant and parent outcomes: A multicentre, multinational, cluster-randomised controlled trial. The Lancet Child & Adolescent Health, 2(4), 245–254. https://doi.org/10.1016/S2352-4642(18)30039-7.
Ortenstrand, A., Westrup, B., Brostrom, E. B., Sarman, I., Akerstrom, S., Brune, T., et al. (2010). The Stockholm Neonatal Family Centered Care Study: Effects on length of stay and infant morbidity. Pediatrics, 125(2), e278–e285. https://doi.org/10.1542/peds.2009-1511.
Phibbs, C. S., & Mortensen, L. (1992). Back transporting infants from neonatal intensive care units to community hospitals for recovery care: Effect on total hospital charges. Pediatrics, 90(1 Pt 1), 22–26.
Profit, J., McCormick, M. C., Escobar, G. J., Richardson, D. K., Zheng, Z., Coleman-Phox, K., et al. (2007). Neonatal intensive care unit census influences discharge of moderately preterm infants. Pediatrics, 119(2), 314–319. https://doi.org/10.1542/peds.2005-2909.
Robles, D., Blumenfeld, Y. J., Lee, H. C., Gould, J. B., Main, E., Profit, J., et al. (2017). Opportunities for maternal transport for delivery of very low birth weight infants. Journal of Perinatology, 37(1), 32–35. https://doi.org/10.1038/jp.2016.174.
Skiold, B., Stewart, M., & Theda, C. (2015). Predictors of unfavorable thermal outcome during newborn emergency retrievals. Air Medical Journal, 34(2), 86–91. https://doi.org/10.1016/j.amj.2014.10.012.
Zarif, M. A., Rest, J., & Vidyasagar, D. (1979). Early retransfer: A method of optimal bed utilization of NICU beds. Critical Care Medicine, 7(8), 327–329.
Acknowledgements
We thank Matthew Nalty with the Eugene S. Farley, Jr. Health Policy Center for his assistance with creation of the referral map.
Funding
This work was supported by the National Institutes of Health (5T32HD007186-37 to Bourque, SL, trainee).
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflict of interest
The authors have no conflicts of interest to disclose.
Rights and permissions
About this article
Cite this article
Bourque, S.L., Levek, C., Melara, D.L. et al. Prevalence and Predictors of Back-Transport Closer to Maternal Residence After Acute Neonatal Care in a Regional NICU. Matern Child Health J 23, 212–219 (2019). https://doi.org/10.1007/s10995-018-2635-6
Published:
Issue Date:
DOI: https://doi.org/10.1007/s10995-018-2635-6