Abstract
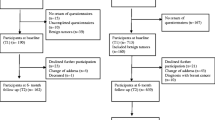
Consecutive patients (n = 221) presenting for initial consultation at a palliative care outpatient clinic were prospectively interviewed and then followed until death. Individual prayer activity (IPA) and global religion scores were associated with quality of life, symptoms, inflammatory markers, and survival. Analyses were adjusted for whether patients were still receiving anti-neoplastic therapies (ANTs) or not. Higher religion scores were associated with lower levels of inflammation in advanced cancer patients still undergoing ANTs. Additionally, higher IPA was an independent good prognostic factor in patients on active ANTs. Further studies are necessary to confirm these findings and to investigate possible biological mechanisms involved.

Similar content being viewed by others
References
Aaronson, N. K., Ahmedzai, S., Bergman, B., Bullinger, M., Cull, A., Duez, N. J., et al. (1993). The European Organization for Research and Treatment of Cancer QLQ-C30: A quality-of-life instrument for use in international clinical trials in oncology. Journal of the National Cancer Institute, 85(5), 365–376.
Alcorn, S. R., Balboni, M. J., Prigerson, H. G., Reynolds, A., Phelps, A. C., Wright, A. A., et al. (2010). “If God wanted me yesterday, I wouldn’t be here today”: Religious and spiritual themes in patients’ experiences of advanced cancer. Journal of Palliative Medicine, 13(5), 581–588.
Aquino, T. A. A., Correia, A. P. M., Marques, A. L. C., Souza, C. G., Fritas, H. C. A., Araújo, I. F., et al. (2009). Atitude religiosa e sentido da vida: Um estudo correlacional. Psicologia: ciência e profissão., 29, 15.
Balboni, T. A., Vanderwerker, L. C., Block, S. D., Paulk, M. E., Lathan, C. S., Peteet, J. R., et al. (2007). Religiousness and spiritual support among advanced cancer patients and associations with end-of-life treatment preferences and quality of life. Journal of Clinical Oncology, 25(5), 555–560.
Beasley, J. M., Newcomb, P. A., Trentham-Dietz, A., Hampton, J. M., Ceballos, R. M., Titus-Ernstoff, L., et al. (2010). Social networks and survival after breast cancer diagnosis. Journal of Cancer Survivorship, 4(4), 372–380.
Bruera, E., Kuehn, N., Miller, M. J., Selmser, P., & Macmillan, K. (1991). The Edmonton Symptom Assessment System (ESAS): A simple method for the assessment of palliative care patients. Journal of Palliative Care, 7(2), 6–9.
Campbell, J. D., Yoon, D. P., & Johnstone, B. (2010). Determining relationships between physical health and spiritual experience, religious practices, and congregational support in a heterogeneous medical sample. Journal of Religion and Health, 49(1), 3–17.
Chen, H., Cheal, K., McDonel Herr, E. C., Zubritsky, C., & Levkoff, S. E. (2007). Religious participation as a predictor of mental health status and treatment outcomes in older persons. International Journal of Geriatric Psychiatry, 22(2), 144–153.
Clinical practice guidelines for quality palliative care, second edition. (2009). Retrieved October 30, 2012, from http://www.nationalconsensusproject.org/guideline.pdf.
Dezutter, J., Wachholtz, A., & Corveleyn, J. (2011). Prayer and pain: The mediating role of positive re-appraisal. Journal of Behavioral Medicine, 34(6), 542–549.
Gillum, R. F., King, D. E., Obisesan, T. O., & Koenig, H. G. (2008). Frequency of attendance at religious services and mortality in a U.S. national cohort. Annals of Epidemiology, 18(2), 124–129.
Holt-Lunstad, J., Steffen, P. R., Sandberg, J., & Jensen, B. (2011). Understanding the connection between spiritual well-being and physical health: An examination of ambulatory blood pressure, inflammation, blood lipids and fasting glucose. Journal of Behavioral Medicine, 34(6), 477–488.
Hui, D., de la Cruz, M., Thorney, S., Parsons, H. A., Delgado-Guay, M., & Bruera, E. (2011). The frequency and correlates of spiritual distress among patients with advanced cancer admitted to an acute palliative care unit. The American Journal of Hospice and Palliative Care, 28(4), 264–270.
Johnson, K. S., Tulsky, J. A., Hays, J. C., Arnold, R. M., Olsen, M. K., Lindquist, J. H., et al. (2011). Which domains of spirituality are associated with anxiety and depression in patients with advanced illness? Journal of General Internal Medicine, 26(7), 751–758.
Koenig, H. G., George, L. K., & Peterson, B. L. (1998). Religiosity and remission of depression in medically ill older patients. American Journal of Psychiatry, 155(4), 536–542.
Lagman, R., & Walsh, D. (2005). Integration of palliative medicine into comprehensive cancer care. Seminars in Oncology, 32(2), 134–138.
Lissoni, P., Messina, G., Parolini, D., Balestra, A., Brivio, F., et al. (2008). A spiritual approach in the treatment of cancer: Relation between faith score and response to chemotherapy in advanced non-small cell lung cancer patients. In Vivo, 22(5), 577–581.
Lucchetti, G., Lucchetti, A. L., & Koenig, H. G. (2011). Impact of spirituality/religiosity on mortality: Comparison with other health interventions. Explore (NY), 7(4), 234–238.
McCullough, M. E., Hoyt, W. T., Larson, D. B., Koenig, H. G., & Thoresen, C. (2000). Religious involvement and mortality: A meta-analytic review. Health Psychology, 19(3), 211–222.
Meraviglia, M. G. (2002). Prayer in people with cancer. Cancer Nursing, 25(4), 326–331.
Messina, G., Lissoni, P., Marchiori, P., Bartolacelli, E., Brivio, F., & Magotti, L. (2010). Enhancement of the efficacy of cancer chemotherapy by the pineal hormone melatonin and its relation with the psychospiritual status of cancer patients. Journal of Research in Medical Science, 15(4), 225–228.
Naing, A., Stephen, S. K., Frenkel, M., Chandhasin, C., Hong, D. S., Lei, X., et al. (2011). Prevalence of complementary medicine use in a phase 1 clinical trials program: The MD Anderson Cancer Center Experience. Cancer, 117(22), 5142–5150.
Nelson, C., Jacobson, C. M., Weinberger, M. I., Bhaskaran, V., Rosenfeld, B., Breitbart, W., et al. (2009). The role of spirituality in the relationship between religiosity and depression in prostate cancer patients. Annals of Behavioral Medicine, 38(2), 105–114.
Nelson, C. J., Rosenfeld, B., Breitbart, W., & Galietta, M. (2002). Spirituality, religion, and depression in the terminally ill. Psychosomatics, 43(3), 213–220.
O’Connor, P. J., Pronk, N. P., Tan, A., & Whitebird, R. R. (2005). Characteristics of adults who use prayer as an alternative therapy. American Journal of Health Promotion, 19(5), 369–375.
Oh, B., Butow, P. N., Mullan, B. A., Clarke, S. J., Beale, P. J., Pavlakis, N., et al. (2012). Effect of medical Qigong on cognitive function, quality of life, and a biomarker of inflammation in cancer patients: A randomized controlled trial. Supportive Care in Cancer, 20(6), 1235–1242.
Purnell, J. Q., Andersen, B. L., & Wilmot, J. P. (2009). Religious practice and spirituality in the psychological adjustment of survivors of breast cancer. Counseling and Values, 53(3), 165.
Schnall, E., Wassertheil-Smoller, S., Swencionis, C., Zemon, V., Tinker, L., O’Sullivan, M. J., et al. (2010). The relationship between religion and cardiovascular outcomes and all-cause mortality in the Women’s Health Initiative Observational Study. Health Psycholgy, 25(2), 249–263.
Seeman, T. E., Dubin, L. F., & Seeman, M. (2003). Religiosity/spirituality and health. A critical review of the evidence for biological pathways. American Psychologist, 58(1), 53–63.
Stefanek, M., McDonald, P. G., & Hess, S. A. (2005). Religion, spirituality and cancer: Current status and methodological challenges. Psychooncology, 14(6), 450–463.
Stewart, D. E., & Yuen, T. (2011). A systematic review of resilience in the physically ill. Psychosomatics, 52(3), 199–209.
Tarakeshwar, N., Vanderwerker, L. C., Paulk, E., Pearce, M. J., Kasl, S. V., & Prigerson, H. G. (2006). Religious coping is associated with the quality of life of patients with advanced cancer. Journal of Palliative Medicine, 9(3), 646–657.
Zhang, B., Nilsson, M. E., & Prigerson, H. G. (2012). Factors important to patients’ quality of life at the end of life. Archives of Internal Medicine, 172(15), 1133–1142.
Acknowledgments
The authors would like to thank the Learning and Research Institute of Barretos Cancer Hospital for revising the English text. We would like to thank the research nurses Camila Crovador and Camila Ito, and also Mr. André Vitor Spindola da Silva, from Researcher Support Center of Barretos Cancer Hospital for their help in data collection. Dr. Carlos Eduardo Paiva obtained his Masther (2006–2008) and PhD (2009–2011) degrees at the Faculty of Medicine of Botucatu (FMB), UNESP, Brazil. At this moment, Dr. Carlos is a post-doctoral fellow at FMB, working with the development of a new brief quality of life instrument directed to low educational patients. He is working at the Department of Medical Oncology and also at the Department of Palliative Care from Barretos Cancer Hospital (BCH, Barretos, SP, Brazil) since 2009. In addition, since 2011, he is one of the Professors from the Post-Graduation Program (MSc/PhD) from BCH. His research projects are focusing on palliative care and quality of life of cancer patients.
Conflit of Interest
The authors declare no conflict of interest.
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
About this article
Cite this article
Paiva, C.E., Paiva, B.S.R., Yennurajalingam, S. et al. The Impact of Religiosity and Individual Prayer Activities on Advanced Cancer Patients’ Health: Is There Any Difference in Function of Whether or Not Receiving Palliative Anti-neoplastic Therapy?. J Relig Health 53, 1717–1727 (2014). https://doi.org/10.1007/s10943-013-9770-6
Published:
Issue Date:
DOI: https://doi.org/10.1007/s10943-013-9770-6