Abstract
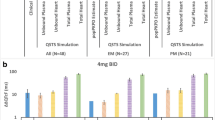
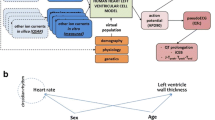
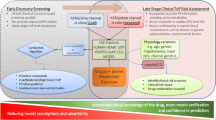
Plasma drug concentration and electrocardiogram (ECG) data from a drug–drug interaction (DDI) study employing the metabolic inhibitor itraconazole have been used as part of a prospectively defined pharmacokinetic/pharmacodynamic modelling strategy to quantify the potential for QT interval prolongation from basmisanil, an investigational compound. ECG data were collected on multiple days during repeat dosing treatment regimens, thereby allowing the capture of QT data across a wide range of drug concentrations in each study participant and encompassing both “therapeutic” and “supra-therapeutic” exposures. The data were used to develop a non-linear mixed effect concentration-QT (C-QT) model that differentiated drug-induced QT prolongation from other factors altering QT interval duration. Food effects were accounted by quantitating their influences on the parameters describing the diurnal variation of QT. The final model demonstrated that itraconazole does not cause QT prolongation, while for basmisanil, the 1-sided upper 95% CI of the QT interval at 240 mg (the highest dose tested in ongoing phase 2 studies) with DDI, was below the 10 ms threshold considered to be of clinical significance by regulatory authorities. The empirical modelling was complemented with a human mechanistic cardiac single cell model that was used to simulate the change in action potential duration as a function of drug concentration. The results of the two approaches were in agreement, suggesting that the effect of basmisanil on QT interval duration can be attributed to the effect on hERG alone. The C-QT model for basmisanil can be used to derive the QT interval corrected changes in heart rate (QTc) and thus inform cardiac safety strategy in later development without the need for a separate, dedicated study.







Similar content being viewed by others
References
Nelson CH, Wang L, Fang L, Weng W, Cheng F, Hepner M, Lin J, Garnett C, Ramanathan SA (2015) Quantitative framework to evaluate proarrhythmic risk in a first-in-human study to support waiver of a thorough QT study. Clin Pharmacol Ther. 98(6):630–638
Darpo B, Benson C, Dota C, Ferber G, Garnett C, Green CL, Jarugula V, Johannesen L, Keirns J, Krudys K, Liu J, Ortemann-Renon C, Riley S, Sarapa N, Smith B, Stoltz RR, Zhou M, Stockbridge N (2015) Results from the IQ-CSRC prospective study support replacement of the thorough QT study by QT assessment in the early clinical phase. Clin Pharmacol Ther 97(4):326–335
Darpo B, Garnett C, Keirns J, Stockbridge N (2015) Implications of the IQ-CSRC prospective study: time to revise ICH E14. Drug Saf 38:773–780
Murphy PJ, Yasuda S, Nakai K, Yoshinaga T, Hall N, Zhou M, Aluri J, Rege B, Moline M, Ferry J, Darpo B (2017) Concentration-response modeling of ECG data from early-phase clinical studies as an alternative clinical and regulatory approach to assessing QT risk: experience from the development program of Lemborexant. J Clin Pharmacol 57(1):96–104
E14 Implementation Working Group. ICH E14 Guideline 2015. The clinical evaluation of QT/QTc interval prolongation and proarrhythmic potential for non-antiarrhythmic drugs questions & answers (R3), 10 December
ICH Harmonised Tripartite Guideline 2005. The clinical evaluation of QT/QTc interval prolongation and proarrhythmic potential for non-antiarrhytmic drugs E14
Stillhart C, Parrott N, Lindenberg M, Chalus P, Bentley D, Szepes A (2017) Characterising drug release from immediate-release formulations of a poorly soluble compound, basmisanil, through absorption modelling and dissolution testing. AAPS J 19(3):827
Ten Tusscher KH, Panfilov AV (2006) Alternans and spiral breakup in a human ventricular tissue model. Am J Physiol Heart Circ Physiol 291(3):H1088–H1100
Piotrovsky V (2005) Pharmacokinetic-pharamcodynamic modeling in the data analysis and interpretation of drug-induced QT/QTc prsolongation. AAPS J 7:E608
Tyl B, Kabbaj M, Azzam S et al (2012) Lack of significant effect of bilastine administered at therapeutic and supratherapeutic doses and concomitantly with ketoconazole on ventricular repolarization: results of a thorough QT study (TQTS) with QT-concentration analysis. J Clin Pharmacol 52(6):893–903
Ruiz-Garcia A, Houk BE, Pithavala YK, Toh M, Sarapa N, Tortorici MA (2015) Effect of axitinib on the QT interval in healthy volunteers. Cancer Chemother Pharmacol 75(3):619–628
Ke AB, Zamek-Gliszczynski MJ, Higgins JW et al (2014) Itraconazole and clarithromycin as ketoconazole alternatives for clinical CYP3A inhibition studies. Clin Pharmacol Ther 95(5):473–476
Lehr T, Staab A, Trommeshauser D et al (2010) Semi-mechanistic population pharmacokinetic drug-drug interaction modelling of a long half-life substrate and itraconazole. Clin Pharmacokinet 49(1):53–66
Abuhelwa AY, Foster DJR, Mudge S, Hayes D, Upton RN (2015) Population pharmacokinetic modeling of itraconazole and hydroxyitraconazole for oral SUBA-itraconazole and Sporanox capsule formulations in healthy subjects in fed and fasted states. Antimicrob Agents Chemother 59:5681–5696
Sung DJ, Kim JG, Won KJ et al (2012) Blockade of K+ and Ca2+ channels by azole antifungal agents in neonatal rat ventricular myocytes. Biol Pharm Bull 35(9):1469–1475
Qu Y, Fang M, Gao B, Amouzadeh HR, Li N, Narayanan P, Acton P, Lawrence J, Vargas HM (2013) Itraconazole decreases left ventricular contractility in isolated rabbit heart: mechanism of action. Toxicol Appl Pharmacol 268(2):113–122
Park JY, Shon JH, Kim KA et al (2006) Combined effects of itraconazole and CYP2D6*10 genetic polymorphism on the pharmacokinetics and pharmacodynamics of haloperidol in healthy subjects. J Clin Psychopharmacol 26(2):135–142
Iribarren C, Round AD, Peng JA et al (2013) Validation of a population-based method to assess drug-induced alterations in the QT interval: a self-controlled crossover study. Pharmacoepidemiol Drug Saf 22(11):1222–1232
Taubel J et al (2012) Shortening of the QT interval after food can be used to demonstrate assay sensitivity in thorough QT studies. J Clin Pharmacol. 52:1558
Mohamed MF, Zeng J, Jiang P, Hosmane B, Othman AA (2017) Use of early clinical trial data to support thorough QT study waiver for upadacitinib and utility of food effect to demonstrate ECG assay sensitivity. Clin Pharmacol Ther. https://doi.org/10.1002/cpt.804
Ferber G, Fernandes S, Täubel J (2017) Estimation of the power of the food effect on QTc to show assay sensitivity. J Clin Pharmacol. 58:81–88
Sciot B, Vandenberk B, Huijghebaert S, Goovaerts G, Van Huffel S, Ector J, Willems R (2016) Influence of food intake on the QT and QT/RR relation. J Electrocardiol 49(5):7
Colatsky T et al (2016) The comprehensive in vitro proarrhythmia assay (CiPA) initiative: update on progress. J Pharmacol Toxicol Methods 81:15–20
Mirams G et al (2011) Simulation of multiple ion channel block provides improved early prediction of compounds’ clinical torsadogenic risk. Cardiovasc Res 91(1):53–61
Fermini B, Fossa A (2003) The impact of drug-induced QT interval prolongation on drug discovery and development. Nat Rev Drug Discov 2:439–447
Xue J (2009) Robust QT interval estimation: from algorithm to validation. Ann Noninvasive Electrocardiol 18:S35
Author information
Authors and Affiliations
Corresponding author
Additional information
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Electronic supplementary material
Below is the link to the electronic supplementary material.
Rights and permissions
About this article
Cite this article
Jaminion, F., Bentley, D., Wang, K. et al. PKPD and cardiac single cell modeling of a DDI study with a CYP3A4 substrate and itraconazole to quantify the effects on QT interval duration. J Pharmacokinet Pharmacodyn 47, 447–459 (2020). https://doi.org/10.1007/s10928-020-09696-y
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s10928-020-09696-y