Abstract
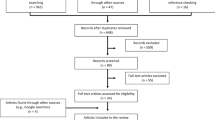
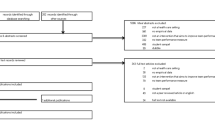
We systematically reviewed the literature to describe how community health workers (CHWs) are involved in occupational health and safety research and to identify areas for future research and research practice strategies. We searched five electronic databases from July 2015 through July 2016. Inclusion criteria were as follows: (1) study took place in the United States, (2) published as a full peer-review manuscript in English, (3) conducted occupational health and safety research, and (4) CHWs were involved in the research. The majority of 17 included studies took place in the agriculture industry (76%). CHWs were often involved in study implementation/design and research participant contact. Rationale for CHW involvement in research was due to local connections/acceptance, existing knowledge/skills, communication ability, and access to participants. Barriers to CHW involvement in research included competing demands on CHWs, recruitment and training difficulties, problems about research rigor and issues with proper data collection. Involving CHWs in occupational health and safety research has potential for improving inclusion of diverse, vulnerable and geographically isolated populations. Further research is needed to assess the challenges and opportunities of involving CHWs in this research and to develop evidence-based training strategies to teach CHWs to be lay-health researchers.

Similar content being viewed by others
Change history
03 April 2018
The original version of this article unfortunately contained a mistake in the affiliation of co-author Ashley M. Bush.
Notes
One study (S07) originated in the Midwestern region but later expanded to the Southwestern U.S.
References
Souza K, Steege AL, Baron SL. Surveillance of occupational health disparities: challenges and opportunities. Am J Ind Med. 2010;53(2):84–94.
Steege AL, Baron SL, Marsh SM, Menéndez CC, Myers JR. Examining occupational health and safety disparities using national data: a cause for continuing concern. Am J Ind Med. 2014;57(5):527–38.
Centers for Disease Control and Prevention. National Occupational Research Agenda (NORA): National Agriculture, Forestry, and Fishing Agenda. Washington, D.C.: NIOSH; 2008. http://www.cdc.gov/niosh/nora/comment/agendas/AgForFish/pdfs/ AgForFishDec2008.pdf. Accessed 4 April 2017.
Murray LR. Sick and tired of being sick and tired: scientific evidence, methods, and research implications for racial and ethnic disparities in occupational health. Am J Public Health. 2003;93(2):221–6.
Okechukwu CA, Souza K, Davis KD, de Castro AB. Discrimination, harassment, abuse, and bullying in the workplace: contribution of workplace injustice to occupational health disparities. Am J Ind Med. 2014;57(5):573–86.
Krieger N. Workers are people too: societal aspects of occupational health disparities - An ecosocial perspective. Am J Ind Med. 2010;53(2):104–15.
Centers for Disease Control and Prevention. National Institute for Occupational Safety and Health. Occupational Health Disparities. https://www.cdc.gov/niosh/ programs/ohd/default.html. Accessed 2 October 2017.
Quesada J, Hart LK, Bourgois P. Structural vulnerability and health: Latino migrant laborers in the United States. Med Anthropology. 2011;30(4):339–62.
Clougherty JE, Souza K, Cullen MR. Work and its role in shaping the social gradient in health. Ann N Y Acad Sci. 2010;1186:102–24.
Rodriguez G, Trejo G, Schiemann E, Quandt SA, Daniel SS, Sandberg JC, et al. Latina workers in North Carolina: work organization, domestic responsibilities, health, and family life. J Immigr Minor Health. 2016;18(3):687–96.
Bureau of Labor Statistics. Foreign-born workers: Labor Force Characteristics—2015. Washington, D.C.: U. S. Department of Labor; 2016. http://www.bls.gov/news.release/pdf/forbrn.pdf. Accessed 4 April 2017.
Bureau of Labor Statistics. Labor Force Characteristics by Race and Ethnicity, 2014. Washington, D.C.: U. S. Department of Labor; 2015. https://www.bls.gov/opub/reports/race-and-ethnicity/2015/home.htm. Accessed 4 April 2017.
Zhang X, Yu S, Wheeler K, Kelleher K, Stallones L, Xiang H. Work-related non-fatal injuries among foreign-born and US-born workers: findings from the U.S. National Health Interview Survey, 1997–2005. Am J Ind Med. 2009;52(1):25–36.
Cummings KJ, Kreiss K. Contingent workers and contingent health: risks of a modern economy. JAMA. 2008;299:448–50.
Howard J. Nonstandard work arrangements and worker health and safety. Am J Ind Med. 2017;60(1):1–10.
Kalleberg AL. Good jobs, bad jobs: the rise of polarized and precarious employment systems in the United States, 1970s to 2000s. New York: Russell Sage Foundation; 2011.
Gong F, Baron S, Stock L, Ayala L. Formative research in occupational health and safety intervention for diverse, underserved worker populations: a homecare worker intervention project. Suppl Public Health Rep. 2009;124(Suppl 1):84–9.
Moir S. Ideological influences on participatory research in occupational health and safety: a review of the literature. New Solut. 2005;15(1):15–28.
Baron SL, Beard S, Davis LK, et al. Promoting integrated approaches to reducing health inequities among low-income workers: applying a social ecological framework. Am J Ind Med. 2014;57(5):539–56.
Gong F, Baron S, Ayala L, Stock L, McDevitt S, Heaney C. The role for community-based participatory research in formulating policy initiatives: promoting safety and health for in-home care workers and their consumers. Am J Public Health. 2009;99(Suppl 3):S531–8.
Minkler M, Lee PT, Tom A, et al. Using community-based participatory research to design and initiate a study on immigrant worker health and safety in San Francisco’s Chinatown restaurants. Am J Ind Med. 2010;53:361–71. https://doi.org/10.1002/ajim.20791.
Chang C, Salvatore AL, Lee PT, et al. Adapting to context in Community-Based Participatory Research: “Participatory Starting Points” in a Chinese immigrant worker community. Am J Community Psychol. 2013;51:480–91. https://doi.org/10.1007/s10464-012-9565-z.
Rhodes SD, Foley KL, Zometa CS, Bloom FR. Lay health advisor interventions among Hispanics/Latinos: a qualitative systematic review. Am J Prev Med. 2007;33:418–27.
American Public Health Association. Community health workers. https://www.apha.org/apha-communities/member-sections/community-health-workers. Accessed 4 April 2017.
Ingram M, Sabo S, Rother J, Wennerstrom A, De Zapien JG. Community health workers and community advocacy: addressing health disparities. J Community Health. 2008;33:417–24.
U. S. Department of Health and Human Services. Community Health Worker National Workforce Study. Health Resources Services Administration, Bureau of Health Professions. 2007. http://bhpr.hrsa.gov/healthworkforce/reports/chwstudy2007.pdf. Accessed 4 April 2017.
Bureau of Labor Statistics. Union Members Summary. Washington, D.C.: U. S. Department of Labor; 2017. https://www.bls.gov/news.release/union2.nr0.htm. Accessed 4 April 2017.
U. S. Government Accountability Office. Contingent Workforce. Washington. D.C.: US. Government Accountability Office; 2015. GAO-15-168R http://www.gao.gov/assets/ 670/669766.pdf.
Israel BA, Schurman SJ, House JS. Action research on occupational stress: involving workers as researchers. Int J Health Serv. 1989;19(1):135–55.
Moher D, Liberati A, Tetzlaff J, Altman DG. Preferred reporting items for systematic reviews and meta-analyses: the PRISMA statement. BMJ. 2009;339:b2535.
Liberati A, Altman DG, Tetzlaff J, et al. PRISMA statement for reporting systematic reviews and meta-analyses of studies that evaluate healthcare interventions: explanation and elaboration. BMJ. 2009;339:b2700.
Littell JH, Corcoran J, Pillai V. Systematic reviews and meta-analysis. New York: Oxford University Press; 2008.
Law M, Stewart D, Pollock N, Letts L, Bosch J, Westmorland M. (1998). Guidelines for critical review form—quantitative studies. 1998. http://srs-mcmaster.ca/wp-content/uploads/2015/04/Guidelines-for-Critical-Review-Form-Quantiative-Studies-English.pdf. Accessed 4 April 2017.
National Institutes of Health. Quality Assessment Tool for Observational Cohort and Cross-Sectional Studies. http://www.nhlbi.nih.gov/health-pro/guidelines/in-develop/cardiovascular-risk-reduction/tools/cohort. Accessed 4 April 2017.
Arcury TA, Vallejos QM, Feldman SR, Quandt SA. Treating skin disease: self-management behaviors of Latino farmworkers. J Agromedicine. 2006;11(2):27–35.
Arcury TA, Marin A, Snively BM, et al. Reducing farmworker residential pesticide exposure: evaluation of a lay health advisor intervention. Health Promot Pract. 2009;10(3):447–55.
Grzywacz JG, Arcury TA, Marin A, et al. Using lay health promoters in occupational health: outcome evaluation in a sample of Latino poultry-processing workers. New Solut. 2009;19(4):449–66.
Luque JS, Monaghan P, Contreras RB, et al. Implementation evaluation of a culturally competent eye injury prevention program for citrus workers in a Florida migrant community. Prog Community Health Partnersh. 2007;1(4):359–69.
Marin A, Carrillo L, Arcury TA, et al. Ethnographic evaluation of a lay health promoter program to reduce occupational injuries among Latino poultry processing workers. Suppl Public Health Rep. 2009;1(124):36–43.
Monaghan P. Lessons learned from a community coalition with diverse stakeholders: the partnership for citrus worker health. Ann Anthropol Pract. 2011;35:27–42.
Monaghan PF, Forst LS, Tovar-Aguilar JA, et al. Preventing eye injuries among citrus harvesters: the community health worker model. Am J Public Health. 2011;101(12):2269–274.
Monaghan PF, Bryant CA, McDermott RJ, et al. Adoption of safety eyewear among citrus harvesters in rural Florida. J Immigr Minor Health. 2012;14:460–66.
Quandt SA, Grzywacz JG, Talton JW, et al. Evaluating the effectiveness of a lay health promoter-led, community-based participatory pesticide safety intervention with farmworker families. Health Promot Pract. 2013;14(3):425–32.
Tovar-Aguilar JA, Monaghan PF, Bryant CA, et al. Improving eye safety in citrus harvest crews through the acceptance of personal protective equipment, community-based participatory research, social marketing, and community health workers. J Agromedicine. 2014;19:107–16.
Forst L, Lacey S, Chen HY, et al. Effectiveness of community health workers for promoting use of safety eyewear by Latino farm workers. Am J Ind Med. 2004;46:607–13.
Forst L, Noth IM, Lacey S, et al. Barriers and benefits of protective eyewear use by Latino farm workers. J Agromedicine. 2006;11(2):11–7.
Forst L, Ahonen E, Zanoni J, et al. More than training: Community-based participatory research to reduce injuries among Hispanic construction workers. Am J Ind Med. 2012;56:827–37.
Liebman AK, Juarez PM, Leyva C, Corona A. A pilot program using promotoras de salud to educate farmworker families about the risks from pesticide exposure. J Agromedicine. 2007;12(2):33–43.
Salvatore AL, Castorina R, Camacho J, et al. Home-based community health worker intervention to reduce pesticide exposures to farmworkers’ children: a randomized-controlled trial. J Expo Sci Environ Epidemiol. 2015;0:1–5.
Bush DE, Wilmsen C, Sasaki T, Barton-Antonio D, Steege AL, Chang C. Evaluation of a pilot promotora program for Latino forest workers in Southern Oregon. Am J Ind Med. 2014;57:788–99.
Farquhar S, Shadbeh N, Samples J, Ventura S, Goff N. Occupational conditions and well-being of indigenous farmworkers. Am J Public Health. 2008;98(11):1956–9.
Rosenthal EL, Wiggins N, Ingram M, Mayfield-Johnson S, De Zapien JG. Community health workers then and now: an overview of national studies aimed at defining the field. J Ambul Care Manag. 2011;34(3):247–59.
Hohl SD, Thompson B, Krok-Schoen JL, Weier RC, Martin M, Bone L, et al. Characterizing community health workers on research teams: results from the Centers for Population Health and Health Disparities. Am J Public Health. 2016;106(4):664–70.
Terpstra J, Coleman KJ, Simon G, Nebeker C. The role of community health workers (CHWs) in health promotion research: ethical challenges and practical solutions. Health Promot Pract. 2011;12(1):86–93.
Bureau of Labor Statistics. Census of Fatal Occupational Injuries Summary, 2015. Washington, D.C.: U. S. Department of Labor; 2016. https://www.bls.gov/ news. release/cfoi.nr0.htm. Accessed 4 April 2017.
Bureau of Labor Statistics. Nonfatal Occupational Injuries and Illnesses Requiring Days Away from Work, 2015. Washington, D.C.: U. S. Department of Labor; 2016. https://www.bls.gov/news.release/pdf/osh2.pdf. Accessed 4 April 2017.
Eggerth DE, Flynn MA. When the third world comes to the first: ethical considerations when working with Hispanic immigrants. Ethics Behav. 2010;20(3–4):229–42.
Peacock N, Issel LM, Townsell SJ, Chapple-McGruder T, Handler A. An innovative method to involve community health workers as partners in evaluation research. Am J Public Health. 2011;101(12):2275–80.
Minkler M. Community-based research partnerships: challenges and opportunities. J Urban Health. 2005;82(2):ii3–ii12.
Findley SE, Matos S, Hicks AL, Campbell A, Moore A, Diaz D. Building a consensus on community health workers’ scope of practice: lessons from New York. Am J Public Health. 2012;102(10):1981–87.
O’Brien MJ, Squires AP, Bixby RA, Larson SC. Role development of community health workers: an examination of selection and training processes in the intervention literature. Am J Prev Med. 2009;37(6 Suppl 1):S262–9.
Cargo M, Mercer SL. The value and challenges of participatory research: strengthening its CHW Role in Occupational Safety and Health Research practice. Annu Rev Public Health. 2008;29(1):325–50.
Weerts DJ, Sandmann LR. Building a two-way street: challenges and opportunities for community engagement at research universities. Rev High Educ. 2008;32(1):73–106.
Sabo S, Wennerstrom A, Phillips D, et al. Community health worker professional advocacy: voices of action from the 2014 National Community Health Worker Advocacy Survey. J Ambul Care Manag. 2015;38(3):225–35.
National Community Health Worker Advocacy Survey: 2014 Preliminary Data Report for the United States and Territories. Mel & Enid Zuckerman College of Public Health, Arizona Prevention Research Center, University of Arizona, Tucson.
Poole DL. Building community capacity to promote social and public health: challenges for universities. Health Soc Work. 1997;22(3):163–70.
Funding
The work presented in this paper was supported by the CDC/NIOSH Cooperative Agreement 5U54OH007547-16. Its contents are solely the responsibility of the authors and do not necessarily represent the official views of CDC/NIOSH.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflict of interest
Each author of this paper declares that she has no conflict of interest.
Ethical Approval
This article does not contain any studies with human participants performed by any of the authors.
Informed Consent/Human Research Protection
This is a systematic review of published articles. Institutional review board approval was not needed.
Appendix
Appendix
Search strategy example
Database searched | Search terms used |
|---|---|
Web of Science | (“community health worker*” OR “community health outreach worker*” OR “community liaison*” OR “community outreach worker*” OR “community organizer*” OR “community health adviser*” OR “community health representative*” OR “community health advocate*” OR “community health agent*” OR “community health distributor*” OR “community health surveyor*” OR “community health assistant” OR “community health assistants” OR “peer educator*” OR “peer counselor*” OR “peer health educator*” OR “public health aide*” OR “lay health educator*” OR “lay health adviser*” OR “patient navigator*” OR “outreach worker*” OR “volunteer health worker*” OR “health educator*” OR “health ambassador*” OR “health advocate*” OR “health promoter” OR “health promoters” OR “enrollment specialist*” OR “workplace champion” OR champion OR promotora* OR promotores OR “promotoras de salud” OR “worker center” OR “worker leader” OR “worker leaders”) AND (interview* OR “quantitative research” OR “qualitative research” OR “empirical research” OR “mixed methods research” OR “program evaluation” OR evaluation OR assessment OR “focus group*” OR methodology OR “longitudinal stud*” OR “comparative stud*” OR “multicenter stud*” OR “observational stud*” OR “clinical trial*” OR “case stud*” OR “validation stud*” OR “prospective stud*” OR “retrospective stud*” OR intervention OR “community participatory research” OR “ethical research practice*” OR interview* OR “research integrity” OR survey* OR “data collection” OR recruitment OR “study recruitment” OR “research recruitment”) AND (“occupational safety” OR “occupational illness*” OR “occupational disease*” OR “occupational health” OR “occupational health and safety” OR “occupational injur*” OR “occupational hazard” OR “occupational hazards” OR “occupational health service*” OR “work* health” OR “work* safety” OR “work* disease*” OR “industrial health” OR “employ* safety” OR “employ* health” OR “industrial health” OR “industrial hygiene” OR “farm worker*” OR farmworker* OR farmer* OR construction worker* OR home health aide* OR home care aide*) |
Rights and permissions
About this article
Cite this article
Swanberg, J.E., Nichols, H.M., Clouser, J.M. et al. A Systematic Review of Community Health Workers’ Role in Occupational Safety and Health Research. J Immigrant Minority Health 20, 1516–1531 (2018). https://doi.org/10.1007/s10903-018-0711-z
Published:
Issue Date:
DOI: https://doi.org/10.1007/s10903-018-0711-z