Abstract
Background
The control mechanisms during general anesthesia include circulation parameters and vegetative reactions. A possible way to quantify vegetative reactions is to measure the impedance of the skin. An activation of the eccrine sweat glands via sympathetic sudomotor fibers induces a secretion of sweat, which generates a drop in skin impedance. The aim of the present study was to investigate the influence which different stressors and measurement electrodes have upon skin impedance.
Material and Method
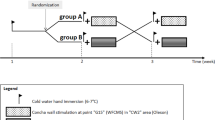
The changes in skin impedance and were measured after application of various stimuli (T1 value at rest, T2 acoustic stimulus, T3 visual stimulus, T4 tactile stimulus, T5 pain stimulus, T6 Valsalva manoeuvre, T7 forced inspiration/expiration). About 62 awake subjects underwent four standardized test sequences, during which several types of electrodes and recording sites (palmarly, plantarly) were explored.
Results
All physiological (T6–T7) and external stimuli (T2–T5) led to significant changes in skin impedance (14.9 ±α8.2 kΩ) and heart rate. These changes happened independently of BMI, gender and measurement electrode types. The time it took to react to the stimuli was significantly shorter for palmar applications than that obtained from plantar sites. The reaction times were as follows: palmarly 1.2 ±α0.5 seconds for solidgel electrodes and 1.15 ±±0.5 seconds for hydrogel electrodes, plantarly 2.3 ±±1.0 seconds for solidgel electrodes and 2.21 ±±1.2 seconds for hydrogel electrodes. The forced inspiration and expiration manoeuvres generated greater variations in skin impedance than did pain stimulus and acoustic stimulus. Measurements that were performed with solidgel electrodes revealed significantly greater average decreases in skin impedance following exposure to a stimulus.
Conclusion(s)
External, but primarily also physiological stressors, generate direct and reproducible variations in skin impedance. Solidgel ECG electrodes should be used for all measurements.
Similar content being viewed by others
References
Selye H. Forty years of stress research: principal remaining problems and misconceptions. Can Med Assoc J 1976;115:53–56
Price E, Korr I. Relationship between Sweat gland activity and electrical resistance of the skin. J Physiol 1957; 10:505–510
Bloch V. New aspects of the psychogalvanic or electrodermographic method as a criterion of emotional tensions. Annee Psychol 1952; 52:329–362
Critchley HD, Elliott R, Mathias CJ, Dolan RJ. Neural activity relating to generation and representation of galvanic skin conductance responses: a functional magnetic resonance imaging study. J Neurosci 2000; 20:3033–3040
Bechara A, Tranel D, Damasio H, Damasio AR. Failure to respond autonomically to anticipated future outcomes following damage to prefrontal cortex. Cereb Cortex 1996; 6:215–225
Buchel C, Morris J, Dolan R, Friston K. Brain systems mediating aversive conditioning: an event-related fMRI study. Neuron 1998; 20:947–957
Mangina CA, Beuzeron-Mangina JH. Direct electrical stimulation of specific human brain structures and bilateral electrodermal activity. Int J Psychophysiol 1996; 22:1–8
Oscar-Berman M, Gade A. Electrodermal measures of arousal in humans with cortical or subcortical brain damage. In: Kimmel H ed. The orientating reflex in humans. Hillsdale, NJ: Erlbaum; 1979, pp. 665–676
Gjerstad AC, Storm H, Hagen R, Huiku M, Qvigstad E, Raeder J. Comparison of skin conductance with entropy during intubation, titanic stimulation and emergence from general anaesthesia. Acta Anaesthesiol Scand 2007; 51:8–15
Gjerstad AC, Storm H, Hagen R, Huiku M, Qvigstad E, Raeder J. Skin conductance or entropy for detection of non-noxious stimulation during different clinical levels of sedation. Acta Anaesthesiol Scand 2007; 51:1–7
Ledowski T, Bromilow J, Paech MJ, Storm H, Hacking R, Schug SA. Skin conductance monitoring compared with Bispectral Index to assess emergence from total i.v. anaesthesia using propofol and remifentanil. Br J Anaesth 2006; 97:817–821
Sato K, Dobson RL. Regional and individual variations in the function of the human eccrine sweat gland. J Invest Dermatol 1970; 54:443–449
Grimmes S. Psychogalvanic reflex and changes in electrical parameters of dry skin. Med Biol Eng Comput 1982;20:734–740
Grimmes S. Impedance measurement of individual skin surface electrodes. Med Biol Eng Comput 1983; 21:750–755
Janitzki A, Föckeler W. A mobile system for signal adaptive data storage-application in physiological measurements. Measurement 1986; 4:82–86
Schwilden H, Kochs E, Daunderer M, Jeleazcov Ch, Scheller B, Schneider G, Schuttler J, Schwender D, Stockmanns G, Poppel E. Concurrent recording of AEP, SSEP and EEG parameters during anaesthesia: a factor analysis. Br J Anaesth 2005;95:197–206
Rossini PM, Opsomer RJ, Boccasena P. Sudomotor skin responses following nerve and brain stimulation. Electroencephalogr Clin Neurophysiol 1993; 89:442–446
Gutrecht J. A sympathetic skin response. Clin Neurophysiol 1994;11:519–524
Jörg J, Boucsein W. Die sympathische Hautreaktion (SSR). Klin Neurophysiol 1998; 29:186–197
Dudel J. Informationsvermittlung durch elektrische Erregung. In: Schmidt RF, Thews G, Hrsg. Physiologie des Menschen. Berlin, Heidelberg, New York: Springer-Verlag, 1995; 26: 20–42
Aramaki S, Kira Y, Hirasawa Y. A study of the normal values and habituation phenomenon of sympathetic skin response. Am J Phys Med Rehabil 1997; 76:2–7
Sharma K, Romano J, Ayyar D, Rotta F, Facca A, Sanchez-Ramos J. Sympathetic skin response and heart rate variability in patients with Huntington disease. Arch Neurol 1999; 56 :1248–1252
Rickles WH Jr, Day JL. Electrodermal activity in non-palmar skin sites. Psychophysiology 1968; 4:421–435
Veanbles PH, Sayer E. On the measurement of the level of skin potential. Br J Psychol 1954; 54: 251–260
Venables PH, Christie MJ. Electrodermal activity. In Martin I, Veanables PH (eds.) Techniques in psychophysiology. New York: Wiley, 1980
Fowles DC, Christie MJ, Edelberg R, Grings WW, Lykken DT, Venables PH. Committee report. Publication recommendations for electrodermal measurements. Psychophysiology 1981;18:232–239
Lykken DT, Venables PH. Direct measurement of skin conductance: a proposal for standardization. Psychophysiology 1971; 8:656–672
Eichmeier J. Medizinische Elektronik. Berlin, Heidelberg, New York: Springer Verlag; 1983
Sagberg F. Dependence of EDR recovery times and other electrodermal measures on scale of measurement: a methodological clarification. Psychophysiology 1980; 17:506–509
Boucsein W, Hoffmann G. A direct comparison of the skin conductance and skin resistance methods. Psychophysiology 1979;16:66–70
Boucsein W, Baltissen R, Euler M. Dependence of skin conductance reactions and skin resistance reactions upon previous level. Psychophysiology 1984; 21:212–218
Lidberg L, Wallin G. Sympathetic skin nerve discharges in relation to amplitude of skin response. Psychophysiology 1981;18:268–270
Wallin G, Blumberg H, Hynnin P. Intraneural stimulation as a method to study sympathetic function in the human skin. Neurosci Lett 1983; 36:189–194
Janitzki AS, Vedder N. Mehrkanal-Hautwiderstandsmessungen. Biomed Technik 1987; 32:98–107
Edelberg R. Electrical properties of the skin. In CC Brown (ed). Methods in psychophysiology. Baltimore: Williams & Wilkins; 1967; pp. 1–53
Barry RJ. Comparability of EDA effects obtained with constant-current skin resistance and constant-voltage skin conductance methods. Physiol Psychol 1981; 9:325–328
Fowles DC, Schneider RE. Effects of epidermal hydration on skin conductance responses and levels. Biol Psychol 1974;2:67–77
McAdams ET, Jossinet J, Lackermeier A, Risacher F. Factors affecting electrode-gel-skin interface impedance in electrical impedance tomography. Med Biol Eng Comput 1996; 34:397–408
Fowles DC, Schneider RE. Electrolyte medium effects on measurements of palmar skin potential. Psychophysiology 1978; 15:474–482
Eisdorfer C, Doerr HO, Follette W. Electrodermal reactivity: an analysis by age and sex. J Human Stress 1980; 6:39–42
Krishnamurthy N, Ahamed SM, Vengadesh GS, Balakumar B, Srinivasan V. Influence of respiration on human sympathetic skin response. Indian J Physiol Pharmacol 1996; 40:350–354
Macefield VG, Wallin BG. Respiratory and cardiac modulation of single sympathetic vasoconstrictor and sudomotor neurones to human skin. J Physiol 1999; 516:303–314
Author information
Authors and Affiliations
Corresponding author
Additional information
Winterhalter M, Schiller J, Münte S, Bund M, Hoy L, Weilbach C, Piepenbrock S, Rahe-Meyer N. Prospective investigation into the influence of various stressors on skin impedance.
Rights and permissions
About this article
Cite this article
Winterhalter, M., Schiller, J., Münte, S. et al. Prospective Investigation into the Influence of Various Stressors on Skin Impedance. J Clin Monit Comput 22, 67–74 (2008). https://doi.org/10.1007/s10877-007-9107-7
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s10877-007-9107-7