Abstract
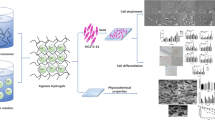
Highly soluble amorphous calcium phosphate powder (ACP) was added to the alginate gel as a buffering agent, in an attempt to enable widely controlled release while avoiding an acidification of the gel-environment. Therapeutic effects of the ACP-containing alginate gel which slowly releases a drug, simvastatin, on osteoporosis model rats were examined. A model drug, simvastatin, incorporated in the alginate gel with ACP up to 0.5%, was continuously released for a long time under the acidic condition. The release rate was controlled by the amount of ACP, serving as a buffer to suppress acidity. When the alginate solution intramuscularly injected in the rat, a soft gel was formed in the injected site. Simvastatin released from the gel containing 0.5% of ACP showed high therapeutic effect on osteoporosis rat. Thus, the present injectable long-sustained release system is expected to be a novel drug delivery controlling device.









Similar content being viewed by others
References
Mundy G, Garrett R, Harris S, Chan J, Chen D, Rossini G, et al. Stimulation of bone formation in vitro and in rodents by statins. Science. 1999;286:1946–9.
Du Z, Chen J, Yan F, Xiao Y. Effects of simvastatin on bone healing around titanium implants in osteoporotic rats. Clin Oral Implants Res. 2009;20:145–50.
Du Z, Chen J, Yan F, Doan N, Ivanovski S, Xiao Y. Serum bone formation marker correlation with improved osseointegration in osteoporotic rats treated with simvastatin. Clin Oral Implants Res. 2011 (in press). doi:10.1111/j.1600-0501.2011.02341.x.
Drachman DE, Edelman ER, Seifert P, Groothuis AR, Bornstein DA, Kamath KR, et al. Neointimal thickening after stent delivery of paclitaxel: change in composition and arrest of growth over six months. J Am Coll Cardiol. 2000;36:2325–32.
Uchida A, Shinto Y, Araki N, Ono K. Slow release of anticancer drugs from porous calcium hydroxyapatite ceramic. J Orthop Res. 1992;10:440–5.
Langer R. Invited review polymeric delivery systems for controlled drug release. Chem Eng Commun. 1980;6:1–48.
Habraken WJ, Wolke JG, Jansen JA. Ceramic composites as matrices and scaffolds for drug delivery in tissue engineering. Adv Drug Deliv Rev. 2007;59:234–48.
Middleton JC, Tipton AJ. Synthetic biodegradable polymers as orthopedic devices. Biomaterials. 2000;21:2335–46.
Jeong B, Bae YH, Lee DS, Kim SW. Biodegradable block copolymers as injectable drug-delivery system. Nature. 1997;388:860–2.
Lin CC, Metters AT. Hydrogels in controlled release formulations: network design and mathematical modeling. Adv Drug Deliv Rev. 2006;58:1379–408.
Wee S, Gombotz WR. Protein release from alginate matrices. Adv Drug Deliv Rev. 1998;31:267–285.
Augst AD, Kong HJ, Mooney DJ. Alginate hydrogels as biomaterials. Macromol Biosci. 2006;6:623–33.
Elnashar MM, Yassin MA, Moneim AEFA, Bary EMA. Surprising performance of alginate beads for the release of low-molecular-weight drugs. J Appl Polym Sci. 2010;116:3021–6.
Donati I, Paoletti S. Material Properties of Alginates. In: Steinbüchel A, series editor, Rehm BHA, editor. Microbiology monographs 13; alginates: biology and applications. Berlin: Springer; 2009. pp. 1–53.
Baron R. Molecular mechanisms of bone resorption by the osteoclast. Anat Rec. 1989;224:317–24.
Eanes ED, Gillessen IH, Postner AS. Intermediate states in the precipitation of hydroxyapatite. Nature. 1965;208:365–7.
Eanes ED, Postner AS. Kinetics and mechanism of conversion of noncrystalline calcium phosphate to crystalline hydroxyapatite. Trans NY Acad Sci II. 1965;28:233–41.
Zahid A. Calcium phosphates in biological and industrial systems. Boston: Kluwer academic publishers; 1998. p. 21–39.
Kokubo T, Kushitani H, Sakka S, Kitsugi T, Yamamuro T. Solutions able to reproduce in vivo surface-structure changes in bioactive glass-ceramic A-W. J Biomed Mater Res. 1990;24:721–34.
Kokubo T, Takadama H. How useful is SBF in predicting in vivo bone bioactivity? Biomaterials. 2006;27:2907–15.
Bitter T, Muir HM. A modified uronic acid carbazole reaction. Anal Biochem. 1962;4:330–4.
Mill PJ. The nature of the interactions between flocculent cells in the flocculation of Saccharomyces cerevisiae. J Gen Microbiol. 1964;35:61–8.
Kim SJ, Lee CK, Lee YM, In Young Kim, Sun I. Kim. Electrical/pH-sensitive swelling behavior of polyelectrolyte hydrogels prepared with hyaluronic acid–poly(vinyl alcohol) interpenetrating polymer networks. React Funct Polym. 2003;55:291–8.
Acknowledgments
This work was partly supported by the Japan Society for the Promotion of Science (nos. 21700494).
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
About this article
Cite this article
Ito, T., Saito, M., Uchino, T. et al. Preparation of injectable auto-forming alginate gel containing simvastatin with amorphous calcium phosphate as a controlled release medium and their therapeutic effect in osteoporosis model rat. J Mater Sci: Mater Med 23, 1291–1297 (2012). https://doi.org/10.1007/s10856-012-4597-3
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s10856-012-4597-3