Abstract
Purpose
Arrhythmia recurrence following pulmonary vein isolation (PVI) occurs predominantly due to the reconnection of previously isolated pulmonary veins (PVs). The prognostic implications of detection and treatment of acute PV reconnection are not well understood. We aim to examine the prognostic significance of acute PV reconnection on arrhythmia recurrence at 1 year following PVI.
Methods
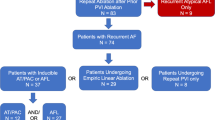
This prospective study included 44 patients (22 men, 60 ± 7 years) who underwent index PVI procedure for treatment of atrial fibrillation (AF). Acute PV reconnection and/or dormant PV conduction were assessed sequentially in response to a 30-min waiting period, intravenous isoproterenol infusion and/or adenosine. All cases of acute PV reconnection and/or dormant conduction were successfully targeted with additional ablation.
Results
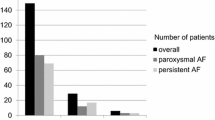
Freedom from AF at 1 year was 75 % (83.3 % in paroxysmal and 65 % in persistent AF, p = ns). Acute PV reconnection and/or dormant conduction were evident in 16 of 44 patients (36.3 %). AF recurrence was documented in eight of 16 patients with, but only in three of 28 patients without acute reconnection (p = 0.009). Three patients underwent a redo procedure, all from the group of patients with acute PV reconnection. In a multivariate model, acute PV reconnection was a strong independent predictor of arrhythmia recurrence (hazards ratio [HR], 6.36; 95 % confidence interval [CI], 1.12–31.6).
Conclusion
Identification of acute PV reconnection, even when successfully targeted, is a strong predictor of arrhythmia recurrence following PVI.




Similar content being viewed by others
Abbreviations
- AAD:
-
Anti-arrhythmic drug
- AF:
-
Atrial fibrillation
- BMI:
-
Body mass index
- LA:
-
Left atrium
- LVEF:
-
Left ventricular ejection fraction
- OSA:
-
Obstructive sleep apnea
- PV:
-
Pulmonary vein
- PVI:
-
Pulmonary vein isolation
References
Kowal, R. C. (2012). PVI's inconvenient truths: lights out for dormant reconnection? Journal of Cardiovascular Electrophysiology, 23(3), 261–263.
Cappato, R., Negroni, S., Pecora, D., Bentivegna, S., Lupo, P. P., Carolei, A., et al. (2003). Prospective assessment of late conduction recurrence across radiofrequency lesions producing electrical disconnection at the pulmonary vein ostium in patients with atrial fibrillation. Circulation, 108(13), 1599–1604.
Gerstenfeld, E. P., Callans, D. J., Dixit, S., Zado, E., & Marchlinski, F. E. (2003). Incidence and location of focal atrial fibrillation triggers in patients undergoing repeat pulmonary vein isolation: implications for ablation strategies. Journal of Cardiovascular Electrophysiology, 14(7), 685–690.
Ouyang, F., Antz, M., Ernst, S., Hachiya, H., Mavrakis, H., Deger, F. T., et al. (2005). Recovered pulmonary vein conduction as a dominant factor for recurrent atrial tachyarrhythmias after complete circular isolation of the pulmonary veins: lessons from double Lasso technique. Circulation, 111(2), 127–135.
Kowalski, M., Grimes, M. M., Perez, F. J., Kenigsberg, D. N., Koneru, J., Kasirajan, V., et al. (2012). Histopathologic characterization of chronic radiofrequency ablation lesions for pulmonary vein isolation. Journal of the American College of Cardiology, 59(10), 930–938.
Arentz, T., Macle, L., Kalusche, D., Hocini, M., Jais, P., Shah, D., et al. (2004). “Dormant” pulmonary vein conduction revealed by adenosine after ostial radiofrequency catheter ablation. Journal of Cardiovascular Electrophysiology, 15(9), 1041–1047.
Tritto, M., De Ponti, R., Salerno-Uriarte, J. A., Spadacini, G., Marazzi, R., Moretti, P., et al. (2004). Adenosine restores atrio-venous conduction after apparently successful ostial isolation of the pulmonary veins. European Heart Journal, 25(23), 2155–2163.
Hachiya, H., Hirao, K., Takahashi, A., Nagata, Y., Suzuki, K., Maeda, S., et al. (2007). Clinical implications of reconnection between the left atrium and isolated pulmonary veins provoked by adenosine triphosphate after extensive encircling pulmonary vein isolation. Journal of Cardiovascular Electrophysiology, 18(4), 392–398.
Matsuo, S., Yamane, T., Date, T., Inada, K., Kanzaki, Y., Tokuda, M., et al. (2007). Reduction of AF recurrence after pulmonary vein isolation by eliminating ATP-induced transient venous re-conduction. Journal of Cardiovascular Electrophysiology, 18(7), 704–708.
Kumagai, K., Naito, S., Nakamura, K., Hayashi, T., Fukazawa, R., Sato, C., et al. (2010). ATP-induced dormant pulmonary veins originating from the carina region after circumferential pulmonary vein isolation of atrial fibrillation. Journal of Cardiovascular Electrophysiology, 21(5), 494–500.
Gula, L. J., Massel, D., Leong-Sit, P., Gray, C., Fox, D. J., Segal, O. R., et al. (2011). Does adenosine response predict clinical recurrence of atrial fibrillation after pulmonary vein isolation? Journal of Cardiovascular Electrophysiology, 22(9), 982–986.
Miyazaki, S., Kuwahara, T., Kobori, A., Takahashi, Y., Takei, A., Sato, A., et al. (2012). Impact of adenosine-provoked acute dormant pulmonary vein conduction on recurrence of atrial fibrillation. Journal of Cardiovascular Electrophysiology, 23(3), 256–260.
Calkins, H., Kuck, K.-H., Cappato, R., Brugada, J., Camm, A. J., Chen, S.-A., et al. (2012). 2012 HRS/EHRA/ECAS Expert Consensus Statement on Catheter and Surgical Ablation of Atrial Fibrillation: recommendations for patient selection, procedural techniques, patient management and follow-up, definitions, endpoints, and research trial design. Europace : European Pacing, Arrhythmias, and Cardiac Electrophysiology, 14(4), 528–606.
Fein, A. S., Shvilkin, A., Shah, D., Haffajee, C. I., Das, S., Kumar, K., et al. (2013). Treatment of obstructive sleep apnea reduces the risk of atrial fibrillation recurrence following catheter ablation. Journal of the American College of Cardiology.
Datino, T., Macle, L., Chartier, D., Comtois, P., Khairy, P., Guerra, P. G., et al. (2011). Differential effectiveness of pharmacological strategies to reveal dormant pulmonary vein conduction: a clinical–experimental correlation. Heart Rhythm : The Official Journal of the Heart Rhythm Society, 8(9), 1426–1433.
Wang, X.-H., Liu, X., Sun, Y.-M., Gu, J.-N., Shi, H.-F., Zhou, L., et al. (2007). Early identification and treatment of PV re-connections: role of observation time and impact on clinical results of atrial fibrillation ablation. Europace: European Pacing, Arrhythmias, and Cardiac Electrophysiology, 9(7), 481–486.
Yamane, T., Matsuo, S., Date, T., Lellouche, N., Hioki, M., Narui, R., et al. (2011). Repeated provocation of time- and ATP-induced early pulmonary vein reconnections after pulmonary vein isolation: eliminating paroxysmal atrial fibrillation in a single procedure. Circulation Arrhythmia and Electrophysiology, 4(5), 601–608.
Hutchinson, M. D., Garcia, F. C., Mandel, J. E., Elkassabany, N., Zado Pa-C, E. S., Riley, M. P., et al. (2012). Efforts to enhance catheter stability improve atrial fibrillation ablation outcome. Heart Rhythm, 10(3), 347–353.
Haldar, S., Jarman, J. W. E., Panikker, S., Jones, D. G., Salukhe, T., Gupta, D., et al. (2012). Contact force sensing technology identifies sites of inadequate contact and reduces acute pulmonary vein reconnection: a prospective case control study. International journal of cardiology.
Reddy, V. Y., Shah, D., Kautzner, J., Schmidt, B., Saoudi, N., Herrera, C., et al. (2012). The relationship between contact force and clinical outcome during radiofrequency catheter ablation of atrial fibrillation in the TOCCATA study. Heart Rhythm, 9(11), 1789–1795.
Conflict of interest
E. Anter received research grants from Biosense Webster and Rhythmia Medical. F.M. Contreras-Valdes, A. Shvilkin and C.M. Tschabrunn have no conflicts of interest. M.E. Josephson received research grants and speaking honoraria from Medtronic.
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
About this article
Cite this article
Anter, E., Contreras-Valdes, F.M., Shvilkin, A. et al. Acute pulmonary vein reconnection is a predictor of atrial fibrillation recurrence following pulmonary vein isolation. J Interv Card Electrophysiol 39, 225–232 (2014). https://doi.org/10.1007/s10840-013-9864-9
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s10840-013-9864-9