Abstract
Background
During catheter ablation procedures, non-radiologic navigation systems may reduce fluoroscopic exposure and energy applications, as well as improve procedural success rates.
Objective
To examine the impact of a non-radiologic navigation system on ablation procedures in pediatric patients, the procedural characteristics and success rates prior to and following incorporation of the LocaLisa® (LL) navigation system into a pediatric electrophysiology laboratory were compared.
Methods
Between January 2000 and April 2005, 246 consecutive patients underwent catheter ablation for either Atrioventricular Reentry Tachycardia AVRT (168) or Atrioventricular Nodal Reentry Tachycardia AVNRT (78). Ablation procedures performed prior to LL (108) were compared to ablation procedures performed using LL (113). The first 25 patients using LL were censored to remove the bias of a learning curve.
Results
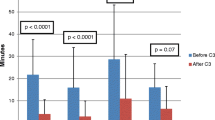
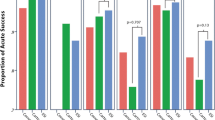
There was no difference in demographic features between the two groups. Statistically significant decreases were found in the diagnostic (11.4 ± 6.1 min v 18.8 ± 9.8 min w/o LL), ablation (5.7 ± 10.3 vs 18.5 ± 20.1 min w/o LL) and total (17.2 ± 12.6 vs 37.3 ± 21.3 min w/o LL) fluoroscopy times for the LL group, as well as in the total number of energy applications (9.0 ± 8.5 vs 12.3 ± 12.2 w/o LL). Success rates were 99.1% w/ LL v 97.2% w/o LL (p = NS). No major complications were observed in either group.
Conclusions
The use of a computer assisted navigation system significantly decreased the diagnostic, ablation, and total fluoroscopy times, as well as the number of energy applications, without affecting procedural success or complication rates. Non-radiologic navigation systems reduce radiation exposure during transcatheter electrophysiologic procedures and thus lower the lifetime radiation cumulative risk, a goal particularly important in children.
Similar content being viewed by others
References
Rosenthal, L. S., Mahesh, M., Beck, T. J., Saul, J. P., Miller, J. M., Kay, N., et al. (1998). Predictors of fluoroscopy time and estimated radiation exposure during radiofrequency catheter ablation procedures. American Journal of Cardiology, 82, 451–458.
Geise, R. A., Peters, N. E., Dunnigan, A. N. N., & Milstein, S. (1996). Radiation doses during pediatric radiofrequency catheter ablation procedures. Pacing and Clinical Electrophysiology, 19, 1605–1611.
Perisinakis, K., Damilakis, J., Theocharopoulos, N., Manios, E., Vardas, P., & Gourtsoyiannis, N. (2001). Accurate assessment of patient effective radiation dose and associated detriment risk from radiofrequency catheter ablation procedures. Circulation, 104, 58–62.
Kovoor, P., Ricciardello, M., Collins, L., Uther, J. B., & Ross, D. L. (1998). Risk to patients from radiation associated with radiofrequency ablation for supraventricular tachycardia. Circulation, 98, 1534–1540.
Kugler, J. D., Danford, D. A., Houston, M. A. K., & Felix, G. (1997). Radiofrequency catheter ablation for paroxysmal supraventricular tachycardia in children and adolescents without structural heart disease. American Journal of Cardiology, 80, 1438–1443.
Kugler, J. D., Danford, D. A., Houston, K. A., & Felix, G. (2002). Pediatric radiofrequency catheter ablation registry success, fluoroscopy time, and complication rate for supraventricular tachycardia: comparison of early and recent eras. Journal of Cardiovascular Electrophysiology, 13, 336–341.
Van Hare, G. F., Javitz, H., Carmelli, D., Saul, J. P., Tanel, R. E., Fischbach, P. S., et al. (2004). Prospective assessment after pediatric cardiac ablation: demographics, medical profiles, and initial outcomes. Journal of Cardiovascular Electrophysiology, 15, 759–770.
Wagner, L. K., Eifel, P. J., & Geise, R. A. (1994). Potential biological effects following high X-ray dose interventional procedures. Journal of Vascular and Interventional Radiology, 5, 71–84.
Calkins, H., Niklason, L., Sousa, J., el-Atassi, R., Langberg, J., & Morady, F. (1991). Radiation exposure during radiofrequency catheter ablation of accessory atrioventricular connections. Circulation, 84, 2376–2382.
Lindsay, B. D., Eichung, J. O., Ambos, H. D., & Cain, M. E. (1992). Radiation exposure to patients and medical personnel during radiofrequency catheter ablation for supraventricular tachycardia. American Journal of Cardiology, 70, 218–223.
Committee on the Biological Effects of Ionizing Radiations Board on Radiation Effects. Research Commission on Life Sciences. National Research Council. (1990) Health effects of exposure to low levels of ionizing radiation. BEIR V. Washington, DC: National Academy Press.
Rotter, M., Takahashi, Y., Sanders, P., Haissaguerre, M., Jais, P., Hsu, L.-F., et al. (2005). Reduction of fluoroscopy exposure and procedure duration during ablation of atrial fibrillation using a novel anatomical navigation system. European Heart Journal, 26, 1415–1421.
Earley, M. J., Showkathali, R., Alzetani, M., Kistler, P. M., Gupta, D., Abrams, D. J., et al. (2006). Radiofrequency ablation of arrhythmias guided by non-fluoroscopic catheter location: A prospective randomized trial. European Heart Journal, 27, 1223–1229.
Papagiannis, J., Tsoutsinos, A., Kirvassilis, G., Sofianidou, I., Koussi, T., Laskari, C., et al. (2006). Nonfluoroscopic catheter navigation for radiofrequency catheter ablation of supraventricular tachycardia in children. Pacing and Clinical Electrophysiology, 29, 971–978.
Drago, F., Silvetti, M. S., Pino, A., Grutter, G., Bevilacqua, M., & Leibovich, S. (2002). Exclusion of fluoroscopy during ablation treatment of right accessory pathway in children. Journal of Cardiovascular Electrophysiology, 13, 778–782.
Kammeraad, J., ten Cate, F. U., Simmers, T., Emmel, M., Wittkampf, F. H. M., & Sreeram, N. (2004). Radiofrequency catheter ablation of atrioventricular nodal reentrant tachycardia in children aided by the LocaLisa mapping system. Europace, 6, 209–214.
Dick, M. d., O’Connor, B. K., Serwer, G. A., LeRoy, S., & Armstrong, B. (1991). Use of radiofrequency current to ablate accessory connections in children. Circulation, 84, 2318–2324.
Papez, A. L., Al-Ahdab, M., Dick, M. II, & Fischbach, P. S. (2006). Transcatheter cryotherapy for the treatment of supraventricular tachyarrhythmias in children: A single center experience. J Interv Card Electrophysiol, 15, 191–196.
Hirshfeld, J. W., Jr., Balter, S., Brinker, J. A., Kern, M. J., Klein, L. W., Lindsay, B. D., et al. (2004). ACCF/AHA/HRS/SCAI clinical competence statement on physician knowledge to optimize patient safety and image quality in fluoroscopically guided invasive cardiovascular procedures: a report of the American College of Cardiology Foundation/American Heart Association/American College of Physicians Task Force on Clinical Competence and Training. Journal of the American College of Cardiology, 44, 2259–2282.
Schueler, B. A., Julsrud, P. R., Gray, J. E., Stears, J. G., & Wu, K. Y. (1994). Radiation exposure and efficacy of exposure-reduction techniques during cardiac catheterization in children. American Journal of Radiology, 162, 173–177.
McFadden, S. L., Mooney, R. B., & Shepherd, P. H. (2002). X-ray dose and associated risks from radiofrequency catheter ablation procedures. British Journal of Radiology, 75, 253–265.
Wittkampf, F. H. M., Wever, E. F. D., Derksen, R., Ramanna, H., Hauer, R. N. W., & Robles de Medina, E. O. (1999). Accuracy of the localisa system in catheter ablation procedures. Journal of Electrocardiology, 32, 7–12.
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
About this article
Cite this article
Papez, A.L., al-Ahdab, M., Dick, M. et al. Impact of a computer assisted navigation system on radiation exposure during pediatric ablation procedures. J Interv Card Electrophysiol 19, 121–127 (2007). https://doi.org/10.1007/s10840-007-9148-3
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s10840-007-9148-3