Abstract
Purpose
Despite the increasing use of GnRHa to trigger final oocyte maturation in segmented IVF cycles, the effects of trigger modality on chromosomal competence and embryo quality remain controversial. Hence, the purpose of this study was to compare euploidy rates and pregnancy outcomes among hyper-responding women using hCG versus GnRHa trigger.
Methods
This retrospective study included 333 hyper-responders, defined as >15 oocytes retrieved, who underwent preimplantation genetic testing (PGT-A) in segmented IVF cycles using either GnRHa or urinary hCG trigger. Live birth rate (LBR) was the primary outcome of interest. Implantation rate (IR), clinical pregnancy rate (CPR), and euploidy rate were secondary outcomes.
Results
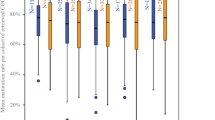
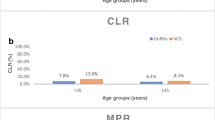
GnRH triggering was associated with improved IR (70.5 vs. 53.2%, p = 0.0475), LBR (51.3 vs. 33.8%, p = 0.0170) compared to hCG. A greater number of oocytes were retrieved (21.9 vs 18.4%, p < 0.001) and euploid embryos produced (2.8 vs. 2.1, p = 0.0109) after GnRHa triggering, while higher euploidy rates were only observed among women <35-years-old (62.0 vs. 51.7%, p = 0.0307) using GnRHa trigger. Higher OHSS rates were observed after hCG triggering (10.6 vs. 2.1%, p = 0.0009).
Conclusion
Hyper-responders who received GnRHa trigger experienced improved pregnancy outcomes and lower rates of OHSS compared to hCG triggering. The higher number of oocytes retrieved and euploid embryos produced may reflect an improved developmental competence using GnRHa triggering due to physiologic induction of both LH and FSH surge or other undefined mechanisms that improve embryo development. However, higher overall euploid rates were only observed among women <35-years-old using the GnRHa trigger. Further prospective studies are required to validate this observation and evaluate the specific influence of different ovulation triggers on gamete developmental competence among hyper-responder women.


Similar content being viewed by others
References
Youssef MA, Van der Veen F, Al-Inany HG, Mochtar MH, Griesinger G, Nagi Mohesen M et al. Gonadotropin-releasing hormone agonist versus HCG for oocyte triggering in antagonist-assisted reproductive technology. The Cochrane database of systematic reviews. 2014(10):Cd008046. doi:https://doi.org/10.1002/14651858.CD008046.pub4.
Kol S, Humaidan P. LH (as HCG) and FSH surges for final oocyte maturation: sometimes it takes two to tango? Reprod BioMed Online. 2010;21(5):590–2. https://doi.org/10.1016/j.rbmo.2010.06.031.
Corbett S, Shmorgun D, Claman P, COMMITTEE REI, CONTRIBUTOR S. The prevention of ovarian hyperstimulation syndrome. Journal of obstetrics and gynaecology Canada : JOGC =. Journal d'obstetrique et gynecologie du Canada : JOGC. 2014;36(11):1024–33. https://doi.org/10.1016/S1701-2163(15)30417-5.
Casper RF. Introduction: gonadotropin-releasing hormone agonist triggering of final follicular maturation for in vitro fertilization. Fertil Steril. 2015;103(4):865–6. https://doi.org/10.1016/j.fertnstert.2015.01.012.
Fatemi HM, Garcia-Velasco J. Avoiding ovarian hyperstimulation syndrome with the use of gonadotropin-releasing hormone agonist trigger. Fertil Steril. 2015;103(4):870–3. https://doi.org/10.1016/j.fertnstert.2015.02.004.
Erb TM, Vitek W, Wakim AN. Gonadotropin-releasing hormone agonist or human chorionic gonadotropin for final oocyte maturation in an oocyte donor program. Fertil Steril. 2010;93(2):374–8. https://doi.org/10.1016/j.fertnstert.2008.12.015.
Humaidan P, Bredkjaer HE, Bungum L, Bungum M, Grøndahl ML, Westergaard L et al. GnRH agonist (buserelin) or hCG for ovulation induction in GnRH antagonist IVF/ICSI cycles: a prospective randomized study. Human reproduction (Oxford, England). 2005;20(5):1213–20. doi:https://doi.org/10.1093/humrep/deh765.
Humaidan P, Ejdrup Bredkjaer H, Westergaard LG, Yding AC. 1,500 IU human chorionic gonadotropin administered at oocyte retrieval rescues the luteal phase when gonadotropin-releasing hormone agonist is used for ovulation induction: a prospective, randomized, controlled study. Fertil Steril. 2010;93(3):847–54. https://doi.org/10.1016/j.fertnstert.2008.12.042.
Haas J, Ophir L, Barzilay E, Yerushalmi GM, Yung Y, Kedem A et al. GnRH agonist vs. hCG for triggering of ovulation--differential effects on gene expression in human granulosa cells. PLoS One. 2014;9(3):e90359. doi:https://doi.org/10.1371/journal.pone.0090359.
Casarini L, Lispi M, Longobardi S, Milosa F, La Marca A, Tagliasacchi D, et al. LH and hCG action on the same receptor results in quantitatively and qualitatively different intracellular signalling. PLoS One. 2012;7(10):e46682. https://doi.org/10.1371/journal.pone.0046682.
Munoz M, Cruz M, Humaidan P, Garrido N, Perez-Cano I, Meseguer M. The type of GnRH analogue used during controlled ovarian stimulation influences early embryo developmental kinetics: a time-lapse study. Eur J Obstet Gynecol Reprod Biol. 2013;168(2):167–72. https://doi.org/10.1016/j.ejogrb.2012.12.038.
Ghobara T, Gelbaya TA, Ayeleke RO. Cycle regimens for frozen-thawed embryo transfer. The Cochrane database of systematic reviews. 2017;7:Cd003414. doi:https://doi.org/10.1002/14651858.CD003414.pub3.
Thorne J, Loza A, Kaye L, Nulsen J, Benadiva C, Grow D, et al. Euploidy rates between cycles triggered with gonadotropin-releasing hormone agonist and human chorionic gonadotropin. Fertil Steril. 2019;112(2):258–65. https://doi.org/10.1016/j.fertnstert.2019.03.040.
Kaye L, Marsidi A, Rai P, Thorne J, Nulsen J, Engmann L, et al. Frozen blastocyst transfer outcomes in immediate versus delayed subsequent cycles following GnRH agonist or hCG triggers. J Assist Reprod Genet. 2018;35(4):669–75. https://doi.org/10.1007/s10815-017-1111-3.
Tannus S, Turki R, Cohen Y, Son WY, Shavit T, Dahan MH. Reproductive outcomes after a single dose of gonadotropin-releasing hormone agonist compared with human chorionic gonadotropin for the induction of final oocyte maturation in hyper-responder women aged 35–40 years. Fertility and sterility. 2017;107(6):1323–8.e2. doi:https://doi.org/10.1016/j.fertnstert.2017.04.014.
Oudshoorn SC, van Tilborg TC, Eijkemans MJC, Oosterhuis GJE, Friederich J, van Hooff MHA et al. Individualized versus standard FSH dosing in women starting IVF/ICSI: an RCT. Part 2: The predicted hyper responder. Human reproduction (Oxford, England). 2017;32(12):2506–14. doi:https://doi.org/10.1093/humrep/dex319.
Arce JC, Klein BM, La Marca A. The rate of high ovarian response in women identified at risk by a high serum AMH level is influenced by the type of gonadotropin. Gynecological endocrinology : the official journal of the International Society of Gynecological Endocrinology. 2014;30(6):444–50. https://doi.org/10.3109/09513590.2014.892066.
Racowsky C, Vernon M, Mayer J, Ball GD, Behr B, Pomeroy KO, et al. Standardization of grading embryo morphology. J Assist Reprod Genet. 2010;27(8):437–9. https://doi.org/10.1007/s10815-010-9443-2.
Humaidan P, Papanikolaou EG, Tarlatzis BC. GnRHa to trigger final oocyte maturation: a time to reconsider. Human reproduction (Oxford, England). 2009;24(10):2389–94. doi:https://doi.org/10.1093/humrep/dep246.
Engmann L, Siano L, Schmidt D, Nulsen J, Maier D, Benadiva C. GnRH agonist to induce oocyte maturation during IVF in patients at high risk of OHSS. Reprod BioMed Online. 2006;13(5):639–44.
Humaidan P, Kol S, Papanikolaou EG. GnRH agonist for triggering of final oocyte maturation: time for a change of practice? Hum Reprod Update. 2011;17(4):510–24. https://doi.org/10.1093/humupd/dmr008.
Humaidan P, Bredkjaer HE, Bungum L, Bungum M, Grondahl ML, Westergaard L et al. GnRH agonist (buserelin) or hCG for ovulation induction in GnRH antagonist IVF/ICSI cycles: a prospective randomized study. Human reproduction (Oxford, England). 2005;20(5):1213–20. doi:https://doi.org/10.1093/humrep/deh765.
Balasch J, Tur R, Creus M, Buxaderas R, Fabregues F, Ballesca JL, et al. Triggering of ovulation by a gonadotropin releasing hormone agonist in gonadotropin-stimulated cycles for prevention of ovarian hyperstimulation syndrome and multiple pregnancy. Gynecological endocrinology : the official journal of the International Society of Gynecological Endocrinology. 1994;8(1):7–12.
Kolibianakis EM, Schultze-Mosgau A, Schroer A, van Steirteghem A, Devroey P, Diedrich K et al. A lower ongoing pregnancy rate can be expected when GnRH agonist is used for triggering final oocyte maturation instead of HCG in patients undergoing IVF with GnRH antagonists. Human reproduction (Oxford, England). 2005;20(10):2887–92. doi:https://doi.org/10.1093/humrep/dei150.
Reddy J, Turan V, Bedoschi G, Moy F, Oktay K. Triggering final oocyte maturation with gonadotropin-releasing hormone agonist (GnRHa) versus human chorionic gonadotropin (hCG) in breast cancer patients undergoing fertility preservation: an extended experience. J Assist Reprod Genet. 2014;31(7):927–32. https://doi.org/10.1007/s10815-014-0248-6.
Acevedo B, Gomez-Palomares JL, Ricciarelli E, Hernandez ER. Triggering ovulation with gonadotropin-releasing hormone agonists does not compromise embryo implantation rates. Fertil Steril. 2006;86(6):1682–7. https://doi.org/10.1016/j.fertnstert.2006.05.049.
Griesinger G, Kolibianakis EM, Papanikolaou EG, Diedrich K, Van Steirteghem A, Devroey P, et al. Triggering of final oocyte maturation with gonadotropin-releasing hormone agonist or human chorionic gonadotropin. Live birth after frozen-thawed embryo replacement cycles. Fertil Steril. 2007;88(3):616–21. https://doi.org/10.1016/j.fertnstert.2006.12.006.
Ata B, Kaplan B, Danzer H, Glassner M, Opsahl M, Tan SL, et al. Array CGH analysis shows that aneuploidy is not related to the number of embryos generated. Reprod BioMed Online. 2012;24(6):614–20. https://doi.org/10.1016/j.rbmo.2012.02.009.
Cedars MI. Fresh versus frozen: initial transfer or cumulative cycle results: how do we interpret results and design studies? Fertil Steril. 2016;106(2):251–6. https://doi.org/10.1016/j.fertnstert.2016.06.001.
Blockeel C, Drakopoulos P, Santos-Ribeiro S, Polyzos NP, Tournaye H. A fresh look at the freeze-all protocol: a SWOT analysis. Human reproduction (Oxford, England). 2016;31(3):491–7. doi:https://doi.org/10.1093/humrep/dev339.
Zhu Q, Chen Q, Wang L, Lu X, Lyu Q, Wang Y, et al. Live birth rates in the first complete IVF cycle among 20 687 women using a freeze-all strategy. Hum Reprod. 2018;33(5):924–9. https://doi.org/10.1093/humrep/dey044.
Wong KM, van Wely M, Mol F, Repping S, Mastenbroek S. Fresh versus frozen embryo transfers in assisted reproduction. The Cochrane database of systematic reviews. 2017;3:Cd011184. doi:https://doi.org/10.1002/14651858.CD011184.pub2.
Acharya KS, Acharya CR, Bishop K, Harris B, Raburn D, Muasher SJ. Freezing of all embryos in in vitro fertilization is beneficial in high responders, but not intermediate and low responders: an analysis of 82,935 cycles from the Society for Assisted Reproductive Technology registry. Fertil Steril. 2018;110:880–7. https://doi.org/10.1016/j.fertnstert.2018.05.024.
Eppig JJ. FSH stimulates hyaluronic acid synthesis by oocyte-cumulus cell complexes from mouse preovulatory follicles. Nature. 1979;281(5731):483–4.
Zelinski-Wooten MB, Hutchison JS, Hess DL, Wolf DP, Stouffer RL. Follicle stimulating hormone alone supports follicle growth and oocyte development in gonadotrophin-releasing hormone antagonist-treated monkeys. Human reproduction (Oxford, England). 1995;10(7):1658–66.
Andersen CY. Effect of FSH and its different isoforms on maturation of oocytes from pre-ovulatory follicles. Reprod BioMed Online. 2002;5(3):232–9. https://doi.org/10.1016/s1472-6483(10)61826-3.
Andersen CY, Ziebe S, Guoliang X, Byskov AG. Requirements for human chorionic gonadotropin and recombinant human luteinizing hormone for follicular development and maturation. J Assist Reprod Genet. 1999;16(8):425–30. https://doi.org/10.1023/a:1020569508927.
Atef A, Francois P, Christian V, Marc-Andre S. The potential role of gap junction communication between cumulus cells and bovine oocytes during in vitro maturation. Mol Reprod Dev. 2005;71(3):358–67. https://doi.org/10.1002/mrd.20281.
Lamb JD, Shen S, McCulloch C, Jalalian L, Cedars MI, Rosen MP. Follicle-stimulating hormone administered at the time of human chorionic gonadotropin trigger improves oocyte developmental competence in in vitro fertilization cycles: a randomized, double-blind, placebo-controlled trial. Fertil Steril. 2011;95(5):1655–60. https://doi.org/10.1016/j.fertnstert.2011.01.019.
Zeleznik AJ, Midgley AR Jr, Reichert LE Jr. Granulosa cell maturation in the rat: increased binding of human chorionic gonadotropin following treatment with follicle-stimulating hormone in vivo. Endocrinology. 1974;95(3):818–25. https://doi.org/10.1210/endo-95-3-818.
Richards JS, Ireland JJ, Rao MC, Bernath GA, Midgley AR Jr, Reichert LE Jr. Ovarian follicular development in the rat: hormone receptor regulation by estradiol, follicle stimulating hormone and luteinizing hormone. Endocrinology. 1976;99(6):1562–70. https://doi.org/10.1210/endo-99-6-1562.
Humaidan P, Westergaard LG, Mikkelsen AL, Fukuda M, Yding AC. Levels of the epidermal growth factor-like peptide amphiregulin in follicular fluid reflect the mode of triggering ovulation: a comparison between gonadotrophin-releasing hormone agonist and urinary human chorionic gonadotrophin. Fertil Steril. 2011;95(6):2034–8. https://doi.org/10.1016/j.fertnstert.2011.02.013.
Ben-Ami I, Komsky A, Bern O, Kasterstein E, Komarovsky D, Ron-El R. In vitro maturation of human germinal vesicle-stage oocytes: role of epidermal growth factor-like growth factors in the culture medium. Human reproduction (Oxford, England). 2011;26(1):76–81. doi:https://doi.org/10.1093/humrep/deq290.
Inoue Y, Miyamoto S, Fukami T, Shirota K, Yotsumoto F, Kawarabayashi T. Amphiregulin is much more abundantly expressed than transforming growth factor-alpha and epidermal growth factor in human follicular fluid obtained from patients undergoing in vitro fertilization-embryo transfer. Fertil Steril. 2009;91(4):1035–41. https://doi.org/10.1016/j.fertnstert.2008.01.014.
Gurbuz AS, Gode F, Uzman MS, Ince B, Kaya M, Ozcimen N, et al. GnRH agonist triggering affects the kinetics of embryo development: a comparative study. Journal of ovarian research. 2016;9:22. https://doi.org/10.1186/s13048-016-0229-8.
Fiedler K, Ezcurra D. Predicting and preventing ovarian hyperstimulation syndrome (OHSS): the need for individualized not standardized treatment. Reproductive biology and endocrinology : RB&E. 2012;10:32. https://doi.org/10.1186/1477-7827-10-32.
Acknowledgements
We would like to thank colleagues at the University of British Columbia and Olive Fertility Centre.
Funding sources
None.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflict of interest
The authors report no conflict of interest.
Additional information
Publisher’s note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Electronic supplementary material
Supplemental Table 1
Characteristics of different doses of hCG trigger. Statistical significance was defined as P ≤ 0.05. (DOCX 15 kb)
Supplemental Table 2
OHSS outcomes of ovarian stimulation cycles. Statistical significance was defined as P ≤ 0.05. (DOCX 15 kb)
Rights and permissions
About this article
Cite this article
Tan, J., Jing, C., Zhang, L. et al. GnRH triggering may improve euploidy and live birth rate in hyper-responders: a retrospective cohort study. J Assist Reprod Genet 37, 1939–1948 (2020). https://doi.org/10.1007/s10815-020-01842-2
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s10815-020-01842-2