Abstract
Introduction
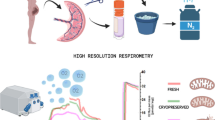
The development of uterine transplantation (UTx) from deceased donors requires knowledge of the tolerance of the uterus to prolonged cold ischemia (CI). This can be evaluated through the use of biological parameters to assess degradation of the organ between its procurement and transplantation. The objective of this study was to analyze changes in the metabolic composition of the storage solution in cases of prolonged CI in uteri from ewes.
Methods
Eighteen uterine auto-transplantations were performed in ewes. CI time was 1 h (T1) or 24 h (T24). Samples of Celsior® were taken when the explanted uterus was flushed (T0) and at the end of CI. A dual approach to metabolic analyses was followed: targeted biochemical analyses targeting several predefined metabolites and non-targeted metabolomics analyses based on nuclear magnetic resonance (NMR).
Results
Metabolic analyses were performed on 16 explanted uteri. Metabolomic profiles differed significantly between T1 and T24 (p = 0.003). Hypoxia-associated degradation of the organ was demonstrated by the significantly higher lactate levels at T24 than at T1 (p < 0.05), accompanied by cell lysis, and significantly higher levels of creatine kinase activity in T24 than in T1 uteri (p < 0.05). Oxidative stress increased over time, with a significantly higher oxidized glutathione/glutathione ratio for T24 than for T1 uteri (p < 0.05).
Conclusion
The metabolic results indicate a significant degradation of the uterus during 24 h of CI. Metabolic analysis of the storage solution could be used as a non-invasive tool for evaluating uterine degradation during CI before transplantation.





Similar content being viewed by others

References
Flyckt R, Kotlyar A, Arian S, Eghtesad B, Falcone T, Tzakis A. Deceased donor uterine transplantation. Fertil Steril. 2017;107:e13.
Kisu I, Kato Y, Obara H, Matsubara K, Matoba Y, Banno K, et al. Emerging problems in uterus transplantation. BJOG Int J Obstet Gynaecol. 2018;125:1352–6.
Ejzenberg D, Andraus W, Baratelli Carelli Mendes LR, Ducatti L, Song A, Tanigawa R, et al. Livebirth after uterus transplantation from a deceased donor in a recipient with uterine infertility. Lancet Lond Engl. 2019;392:2697–704.
Kisu I, Mihara M, Banno K, Umene K, Araki J, Hara H, et al. Risks for donors in uterus transplantation. Reprod Sci Thousand Oaks Calif. 2013;20:1406–15.
Lavoué V, Vigneau C, Duros S, Boudjema K, Levêque J, Piver P, et al. Which donor for uterus transplants: brain-dead donor or living donor? A systematic review. Transplantation. 2017;101:267–73.
Brännström M. Uterus transplantation and beyond. J Mater Sci Mater Med. 2017;28:70.
Bon D, Chatauret N, Giraud S, Thuillier R, Favreau F, Hauet T. New strategies to optimize kidney recovery and preservation in transplantation. Nat Rev Nephrol. 2012;8:339–47.
Favreau F, Giraud S, Bon D, Chatauret N, Thuillier R, Hauet T. Ischemia reperfusion control: the key of kidney graft outcomeMed Sci MS. 2013;29:183–8.
Fiehn O, Kopka J, Dörmann P, Altmann T, Trethewey RN, Willmitzer L. Metabolite profiling for plant functional genomics. Nat Biotechnol. 2000;18:1157–61.
Bonneau E, Tétreault N, Robitaille R, Boucher A, De Guire V. Metabolomics: perspectives on potential biomarkers in organ transplantation and immunosuppressant toxicity. Clin Biochem. 2016;49:377–84.
Barin-Le Guellec C, Largeau B, Bon D, Marquet P, Hauet T. Ischemia/reperfusion-associated tubular cells injury in renal transplantation: Can metabolomics inform about mechanisms and help identify new therapeutic targets? Pharmacol Res. 2018;129:34–43.
Guy AJ, Nath J, Cobbold M, Ludwig C, Tennant DA, Inston NG, et al. Metabolomic analysis of perfusate during hypothermic machine perfusion of human cadaveric kidneys. Transplantation. 2015;99:754–9.
Bon D, Billault C, Claire B, Thuillier R, Hebrard W, Boildieu N, et al. Analysis of perfusates during hypothermic machine perfusion by NMR spectroscopy: a potential tool for predicting kidney graft outcome. Transplantation. 2014;97:810–6.
Dahm-Kähler P, Wranning C, Lundmark C, Enskog A, Mölne J, Marcickiewicz J, et al. Transplantation of the uterus in sheep: methodology and early reperfusion events. J Obstet Gynaecol Res. 2008;34:784–93.
Tricard J, Ponsonnard S, Tholance Y, Mesturoux L, Lachatre D, Couquet C, et al. Uterus tolerance to extended cold ischemic storage after auto-transplantation in ewes. Eur J Obstet Gynecol Reprod Biol. 2017;214:162–7.
Wranning CA, Marcickiewicz J, Enskog A, Dahm-Kähler P, Hanafy A, Brännström M. Fertility after autologous ovine uterine-tubal-ovarian transplantation by vascular anastomosis to the external iliac vessels. Hum Reprod Oxf Engl. 2010;25:1973–9.
Ziegler F, Le Boucher J, Coudray-Lucas C, Cynober L. Plasma amino-acid determinations by reversed-phase HPLC: improvement of the orthophthalaldehyde method and comparison with ion exchange chromatography. J Autom Chem. 1992;14:145–9.
Wei L, Xue T, Yang H, Zhao G-Y, Zhang G, Lu Z-H, et al. Modified uterine allotransplantation and immunosuppression procedure in the sheep model. PLoS One. 2013;8:e81300.
Wranning CA, Dahm-Kähler P, Mölne J, Nilsson UA, Enskog A, Brännström M. Transplantation of the uterus in the sheep: oxidative stress and reperfusion injury after short-time cold storage. Fertil Steril. 2008;90:817–26.
Karam G. Safety of the use of Celsior in kidney-pancreas transplantation. Progres En Urol J Assoc Francaise Urol Soc Francaise Urol. 2003;13:46–9.
Testa G, Koon EC, Johannesson L, McKenna GJ, Anthony T, Klintmalm GB, et al. Living donor uterus transplantation: a single center’s observations and lessons learned from early setbacks to technical success. Am J Transplant Off J Am Soc Transplant Am Soc Transpl Surg. 2017;17:2901–10.
Brännström M, Johannesson L, Dahm-Kähler P, Enskog A, Mölne J, Kvarnström N, et al. First clinical uterus transplantation trial: a six-month report. Fertil Steril. 2014;101:1228–36.
Favreau F, Petit-Paris I, Hauet T, Dutheil D, Papet Y, Mauco G, et al. Cyclooxygenase 1-dependent production of F2-isoprostane and changes in redox status during warm renal ischemia-reperfusion. Free Radic Biol Med. 2004;36:1034–42.
Wranning CA, Mölne J, El-Akouri RR, Kurlberg G, Brännström M. Short-term ischaemic storage of human uterine myometrium--basic studies towards uterine transplantation. Hum Reprod Oxf Engl. 2005;20:2736–44.
Faure JP, Petit I, Zhang K, Dutheil D, Doucet C, Favreau F, et al. Protective roles of polyethylene glycol and trimetazidine against cold ischemia and reperfusion injuries of pig kidney graft. Am J Transplant Off J Am Soc Transplant Am Soc Transpl Surg. 2004;4:495–504.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
The research protocol was accepted by the regional ethics committee for animal experimentation in the Limousin region (CREEAL) (approval number 06-2014-06). Animal welfare was ensured in accordance with EU Directive 2010-63.
Additional information
Publisher’s note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
About this article
Cite this article
Tardieu, A., Chazelas, P., Faye, PA. et al. Changes in the metabolic composition of storage solution with prolonged cold ischemia of the uterus. J Assist Reprod Genet 36, 1169–1178 (2019). https://doi.org/10.1007/s10815-019-01477-y
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s10815-019-01477-y