Abstract
Purpose
To study the role of individual semen parameters on the offspring birth weight and body mass index (BMI) from a population of men evaluated in an assisted reproduction technology (ART) clinic compared to fertile controls.
Methods
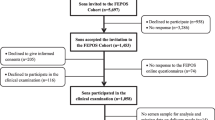
We performed a retrospective study using a cohort with fertile, age-matched controls of men evaluated with semen analysis at the University of Utah Andrology Clinic from 1996 to 2011 and Intermountain Healthcare from 2002 to 2011. We use the offspring from both our sub-fertile cohort and controls using the Utah Population Database. The two main outcomes of interest were offspring birth weight and adolescent BMI.
Results
The offspring of men with impaired sperm parameters had significantly lower birth weight compared to fertile control offspring. Low-concentration offspring weighed 158 g less (95% CI − 278~− 38; p = 0.01), low total count weighed 172 g less (95% CI − 294~− 51; p = 0.005), and low total motility weighed 155 g less (95% CI − 241~− 69; p < 0.001) compared to those of the controls. When we controlled for the use of ART within the sub-fertile group, we found that there was a significant trend of increasing birth weight across levels of total motile count and total sperm count compared to the azoospermic group. We did not find any consistent significant differences between the subject and control adolescence BMI based on semen parameters.
Conclusions
Despite limitations within our population-based dataset, we found that poor quality semen analysis parameters pointed towards an association with low birth weight in the offspring of sub-fertile men compared to the offspring of normal fertile controls. However, in contrast to studies of ART effects on offspring, we did not find evidence of long-term associations between semen quality and offspring BMI.


Similar content being viewed by others
References
Organization WH. Global status report on noncommunicable diseases 2014. 2014.
Temporal and geospatial trends in male factor infertility with assisted reproductive technology in the United States from 1999–2010., (2014).
Assisted reproductive technology surveillance—United States, 2011., (2014).
Carlsen E, Giwercman A, Keiding N, Skakkebaek NE. Evidence for decreasing quality of semen during past 50 years. BMJ. 1992;305(6854):609–13.
Jørgensen N, Joensen UN, Jensen TK, Jensen MB, Almstrup K, Olesen IA, et al. Human semen quality in the new millennium: a prospective cross-sectional population-based study of 4867 men. BMJ Open. 2012;2(4):e000990. https://doi.org/10.1136/bmjopen-2012-000990.
Swan SH, Elkin EP, Fenster L. The question of declining sperm density revisited: an analysis of 101 studies published 1934–1996. Environ Health Perspect. 2000;108(10):961–6.
ESHRE. ESHRE ART fact sheet. 2016. https://www.eshre.eu/Home/ESHRE-Annual-Report-2016.aspx. Accessed 10/31 2016.
Bonduelle M, Wennerholm UB, Loft A, Tarlatzis BC, Peters C, Henriet S, et al. A multi-centre cohort study of the physical health of 5-year-old children conceived after intracytoplasmic sperm injection, in vitro fertilization and natural conception. Hum Reprod. 2005;20(2):413–9.
Ceelen M, van Weissenbruch MM, Vermeiden JPW, van Leeuwen FE, Delemarre-van de Waal HA. Growth and development of children born after in vitro fertilization. Fertil Steril 2008;90(5):1662–1673.
Gibson SB, Figueroa KP, Bromberg MB, Pulst S-M, Cannon-Albright L. Familial clustering of ALS in a population-based resource. Neurology. 2014;82(1):17–22. https://doi.org/10.1212/01.wnl.0000438219.39061.da.
Tuohy TMF, Rowe KG, Mineau GP, Pimentel R, Burt RW, Samadder NJ. Risk of colorectal cancer and adenomas in the families of patients with adenomas: a population-based study in Utah. Cancer. 2014;120(1):35–42. https://doi.org/10.1002/cncr.28227.
Hanson HA, Anderson RE, Aston KI, Carrell DT, Smith KR, Hotaling JM. Subfertility increases risk of testicular cancer: evidence from population-based semen samples. Fertil Steril. 2016;105(2):322–8.e1. https://doi.org/10.1016/j.fertnstert.2015.10.027.
World Health Organization. WHO laboratory manual for the examination and processing of human semen. 2010. http://whqlibdoc.who.int/publications/2010/9789241547789_eng.pdf.
World Health Organization. WHO laboratory manual for the examination and processing of human semen. 5th ed. Geneva: World Health Organization; 2010.
Hansen M, Colvin L, Petterson B, Kurinczuk JJ, de Klerk N, Bower C. Twins born following assisted reproductive technology: perinatal outcome and admission to hospital. Hum Reprod. 2009;24(9):2321–31.
Ceelen M, van Weissenbruch MM, Roos JC, Vermeiden JPW, van Leeuwen FE, Delemarre-van de Waal HA. Body composition in children and adolescents born after in vitro fertilization or spontaneous conception. J Clin Endocrinol Metab 2007;92(9):3417–3423.
Halliday J, Wilson C, Hammarberg K, Doyle LW, Bruinsma F, McLachlan R, et al. Comparing indicators of health and development of singleton young adults conceived with and without assisted reproductive technology. Fertil Steril. 2014;101(4):1055–63. https://doi.org/10.1016/j.fertnstert.2014.01.006.
Ludwig AK, Sutcliffe AG, Diedrich K, Ludwig M. Post-neonatal health and development of children born after assisted reproduction: a systematic review of controlled studies. Eur J Obstet Gynecol Reprod Biol. 2006;127(1):3–25.
Jenkins TG, Aston KI, Hotaling JM, Shamsi MB, Simon L, Carrell DT. Teratozoospermia and asthenozoospermia are associated with specific epigenetic signatures. Andrology. 2016;4(5):843–9. https://doi.org/10.1111/andr.12231.
Jenkins TG, Aston KI, Meyer TD, Hotaling JM, Shamsi MB, Johnstone EB, et al. Decreased fecundity and sperm DNA methylation patterns. Fertil Steril. 2016;105(1):51–7.e3. https://doi.org/10.1016/j.fertnstert.2015.09.013.
Jenkins TG, Aston KI, Trost C, Farley J, Hotaling JM, Carrell DT. Intra-sample heterogeneity of sperm DNA methylation. Mol Hum Reprod. 2015;21(4):313–9.
Klaver R, Gromoll J. Bringing epigenetics into the diagnostics of the andrology laboratory: challenges and perspectives. Asian Journal of Andrology. 2014;16(5):669–74. https://doi.org/10.4103/1008-682x.125412.
Krausz C, Sandoval J, Sayols S, Chianese C, Giachini C, Heyn H, et al. Novel insights into DNA methylation features in spermatozoa: stability and peculiarities. PLoS One. 2012;7(10):e44479. https://doi.org/10.1371/journal.pone.0044479.
Bromfield JJ, Schjenken JE, Chin PY, Care AS, Jasper MJ, Robertson SA. Maternal tract factors contribute to paternal seminal fluid impact on metabolic phenotype in offspring. Proc Natl Acad Sci U S A. 2014;111(6):2200–5. https://doi.org/10.1073/pnas.1305609111.
Ceelen M, van Weissenbruch MM, Vermeiden JP, van Leeuwen FE, Delemarre-van de Waal HA. Cardiometabolic differences in children born after in vitro fertilization: follow-up study. J Clin Endocrinol Metab 2008;93(5):1682–1688. doi:https://doi.org/10.1210/jc.2007-2432.
Belva F, Painter R, Bonduelle M, Roelants M, Devroey P, De Schepper J. Are ICSI adolescents at risk for increased adiposity? 2011;27(1):257–64. doi: https://doi.org/10.1093/humrep/der375.
Hart R, Norman RJ. The longer-term health outcomes for children born as a result of IVF treatment: part I—general health outcomes. Hum Reprod Update. 2013;19(3):232–43. https://doi.org/10.1093/humupd/dms062.
Sakka SD, Loutradis D, Kanaka-Gantenbein C, Margeli A, Papastamataki M, Papassotiriou I, et al. Absence of insulin resistance and low-grade inflammation despite early metabolic syndrome manifestations in children born after in vitro fertilization. Fertil Steril. 2010;94(5):1693–9.
Ceelen M, van Weissenbruch MM, Prein J, Smit JJ, Vermeiden JPW, Spreeuwenberg M, et al. Growth during infancy and early childhood in relation to blood pressure and body fat measures at age 8-18 years of IVF children and spontaneously conceived controls born to subfertile parents. Hum Reprod. 2009;24(11):2788–95.
Ward WS. Function of sperm chromatin structural elements in fertilization and development. Mol Hum Reprod. 2010;16(1):30–6. https://doi.org/10.1093/molehr/gap080.
Hammoud SS, Nix DA, Zhang H, Purwar J, Carrell DT, Cairns BR. Distinctive chromatin in human sperm packages genes for embryo development. Nature. 2009;460(7254):473–8. https://doi.org/10.1038/nature08162.
Barker DJP. Adult consequences of fetal growth restriction. Clin Obstet Gynecol. 2006;49(2):270–83.
Osmond C, Barker DJ. Fetal, infant, and childhood growth are predictors of coronary heart disease, diabetes, and hypertension in adult men and women. Environ Health Perspect. 2000;108(Suppl 3):545–53.
Eisenberg ML, Kim S, Chen Z, Sundaram R, Schisterman EF, Buck Louis GM. The relationship between male BMI and waist circumference on semen quality: data from the LIFE study. Hum Reprod. 2014;29(2):193–200.
Hammiche F, Laven JS, Twigt JM, Boellaard WP, Steegers EA, Steegers-Theunissen RP. Body mass index and central adiposity are associated with sperm quality in men of subfertile couples. Hum Reprod. 2012;27(8):2365–72. https://doi.org/10.1093/humrep/des177.
Soubry A, Murphy SK, Wang F, Huang Z, Vidal AC, Fuemmeler BF, et al. Newborns of obese parents have altered DNA methylation patterns at imprinted genes. Int J Obes (2005). 2015;39(4):650–7. https://doi.org/10.1038/ijo.2013.193.
Donkin I, Versteyhe S, Ingerslev Lars R, Qian K, Mechta M, Nordkap L, et al. Obesity and bariatric surgery drive epigenetic variation of spermatozoa in humans. Cell Metab. 2016;23(2):369–78. https://doi.org/10.1016/j.cmet.2015.11.004.
Li Z, Wang YA, Ledger W, Edgar DH, Sullivan EA. Clinical outcomes following cryopreservation of blastocysts by vitrification or slow freezing: a population-based cohort study. Hum Reprod. 2014;29(12):2794–801. https://doi.org/10.1093/humrep/deu246.
Funding
This investigation was supported in part by from the National Center for Research Resources and the National Center for Advancing Translational Sciences, National Institutes of Health, through Grant 5UL1TR001067-02.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
This study was approved by the Institutional Review Boards of the University of Utah and Intermountain Health Care by the Utah Resource for Genetic and Epidemiologic Research (www.research.utah.edu/rge/) #IRB_00069711.
Electronic supplementary material
Supplemental Table 1
(DOCX 63.6 kb)
Rights and permissions
About this article
Cite this article
Anderson, R.E., Hanson, H.A., Thai, D. et al. Do paternal semen parameters influence the birth weight or BMI of the offspring? A study from the Utah Population Database. J Assist Reprod Genet 35, 793–799 (2018). https://doi.org/10.1007/s10815-018-1154-0
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s10815-018-1154-0