Abstract
Purpose
Prior studies suggest that pregnancy outcomes after autologous oocyte cryopreservation are similar to fresh in vitro fertilization (IVF) cycles. It is unknown whether there are differences in pregnancy and perinatal outcomes between cryopreserved oocytes and cryopreserved embryos.
Methods
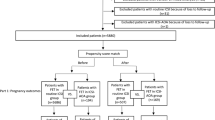
This is a retrospective cohort study comparing pregnancy and perinatal outcomes between oocyte and embryo cryopreservation at a university-based fertility center. We included 42 patients and 68 embryo transfers in patients who underwent embryo transfer after elective oocyte preservation (frozen oocyte-derived embryo transfer (FOET)) from 2005 to 2015. We compared this group to 286 patients and 446 cycles in women undergoing cryopreserved embryo transfer (frozen embryo transfer (FET)) from 2012 to 2015.
Results
Five hundred fourteen transfer cycles were included in our analysis. The mean age was lower in the FOET vs FET group (34.3 vs 36.0 years), but there were no differences in ovarian reserve markers. Thawed oocytes had lower survival than embryos (79.1 vs 90.1%); however, fertilization rates were similar (76.2 vs 72.8%). In the FOET vs FET groups, clinical pregnancies were 26.5 and 30%, and live birth rates were 25 and 25.1%. Miscarriages were higher in the FET group, 8.1 vs 1.5%. There were no differences in perinatal outcomes between the two groups. The mean gestational age at delivery was 39.1 vs 38.6 weeks, mean birth weight 3284.2 vs 3161.1 gms, preterm gestation rate 5.9 vs 13.4%, and multiple gestation rate 5.9 vs 11.6%.
Conclusions
In our study, live birth rates and perinatal outcomes were not significantly different in patients after oocyte and embryo cryopreservation.

Similar content being viewed by others
References
Faddy MJ, Gosden RG, Gougeon A, Richardson SJ, Nelson JF. Accelerated disappearance of ovarian follicles in mid-life: implications for forecasting menopause. Hum Reprod. 1992;7:1342–6.
Cil AP, Turkgeldi L, Seli E. Oocyte cryopreservation as a preventative measure for age-related fertility loss. Semin Reprod Med. 2015 Nov;33(6):429–35.
Mertes H, Pennings G. Social egg freezing: for better, not for worse. Repro Biomed Online. 2011;23:824–9.
Rienzi L, Gracia C, Maggiulli R, LaBarbera AR, Kaser KJ, Ubaldi FM, et al. Oocyte, embryo and blastocyst cryopreservation in ART: systematic review and meta-analysis comparing slow-freezing versus vitrification to produce evidence for the development of global guidance. Hum Reprod Update. 2017;1;23(2):139–55.
Debrock S, Peeraer K, Fernandez Gallardo E, De Neubourg D, Spiessens C, D’Hooghe TM. Vitrification of cleavage stage day 3 embryos results in higher live birth rates than conventional slow freezing: a RCT. Hum Reprod. 2015;30(3):1820–30.
Fasano G, Fontenelle N, Vannin AS, Biramane J, Devreker F, Englert Y, et al. A randomized controlled trial comparing two vitrification methods versus slow-freezing for cryopreservation of human cleavage stage embryos. J Assist Reprod Genet. 2014 Feb;31(2):241–7.
Cobo A, Meseguer M, Remohí J, Pellicer A. Use of cryo-banked oocytes in an ovum donation programme: a prospective, randomized, controlled, clinical trial. Hum Reprod. 2010;25(9):2239–46.
Richter KS, Shipley SK, Vearry I, Tucker MJ, Wildra EA. Cryopreserved embryo transfers suggest that endometrial receptivity may contribute to reduced success rates of later developing embryos. Fertil Steril. 2006;86:862–6.
Roque M, Lattes K, Serra S, Psych IS, Geber S, Carreras R, et al. Fresh embryo transfer versus frozen embryo transfer in in vitro fertilization cycles: a systematic review and meta-analysis. Fertil Steril. 2013;99(1):156–62.
Paulson RJ. Hormonal induction of endometrial receptivity. Fertil Steril. 2011;96:530–5.
Cobo A, Diaz C. Clinical application of oocyte vitrification: a systematic review and meta-analysis of randomized controlled trials. Fertil Steril. 2011 Aug;96(2):277–85.
Loutradi KE, Kolibianakis EM, Venetis CA, Papanikolau EG, Pados G, Bontis I, et al. Cryopreservation of human embryos by vitrification or slow freezing: a systematic review and meta-analysis. Fertil Steril. 2008;90(1):186–93.
Fernández-Shaw S, Cercas R, Braña C, Villas C, Pons I. Ongoing and cumulative pregnancy rate after cleavage-stage versus blastocyst-stage embryo transfer using vitrification for cryopreservation: impact of age on the results. J Assist Reprod Genetic. 2015 Feb;32(2):177–84.
Glujovsky D, Blake D, Farquhar C, Bardach A. Cleavage stage versus blastocyst stage embryo transfer in assisted reproductive technology. Cochrane Database Syst Rev. 2012;11(7):CD002118.
American Society for Reproductive Medicine: Criteria for number of embryos to transfer: a committee opinion. Practice Committee of the American Society for Reproductive Medicine. Practice Committee of Society for assisted reproductive technology. Fertil Steril. 2013 Jan;99(1):44–6.
Grifo JA, Noyes N. Delivery rate using cryopreserved oocytes is comparable to conventional in vitro fertilization using fresh oocytes: potential fertility preservation for female cancer patients. Fertil Steril. 2010;93(2):391–6.
Forman EJ, Li X, Ferry KM, Scott K, Treff NR, Scott RT. Oocyte vitrification does not increase the risk of embryonic aneuploidy or diminish the implantation potential of blastocysts created after intracytoplasmic sperm injection: a novel, paired randomized controlled trial using DNA fingerprinting. Fertil Steril. 2012;98:644–9.
New York Times. First baby of a frozen embryo. NY Times Web. 1984;11:A16.
Chen C. Pregnancy after human oocyte cryopreservation. Lancet. 1986;1:884–6.
Oktay K, Cil AP, Bang H. Efficiency of oocyte cryopreservation: a meta-analysis. Fertil Steril. 2006;86:70–80.
Cobo A, Domingo J, Pérez S, Crespo J, Remohí J, Pellicer A. Vitrification: an effective new approach to oocyte banking and preserving fertility in cancer patients. Clin Transl Oncol. 2008;10:268–73.
Smith GD, Serafini PC, Fioaravanti J, Yadid I, Coslovsky M, Hassun P, et al. Prospective randomized comparison of human oocyte cryopreservation with slow-rate freezing or vitrification. Fertil Steril. 2010;94:2088–95.
Levi Setti PE, Porcu E, Patrizio P, Vigliano V, de Luca R, d’Alicia P, et al. Human oocyte cryopreservation with slow freezing versus vitrification. Results from the National Italian Registry data, 2007-2011. Fertil Steril. 2014 Jul;102(1):90–5.
Doyle JO, Richter KS, Lim J, Stillman RJ, Graham JR, Tucker MJ. Successful elective and medically indicated oocyte vitrification and warming for autologous in vitro fertilization, with predicted birth probabilities for fertility preservation according to number of cryopreserved oocytes and age at retrieval. Fertil Steril. 2016;105(2):459–66.
Solé M, Santaló J, Boada M, Clua E, Rodríguez I, Martínez F, et al. How does vitrification affect oocyte viability in oocyte donation cycles? A prospective study to compare outcomes achieved with fresh versus vitrified sibling oocytes. Hum Reprod. 2013;28(8):2087–92.
Trokoudes KM, Pavlides C, Zhang X. Comparison outcome of fresh and vitrified donor oocytes in an egg-sharing donation program. Fertil Steril. 2011;95(6):1996–2000.
Chang C, Elliot TA, Wright G, Shapiro DB, Toledo AA, Nagy ZP. Prospective controlled study to evaluate laboratory and clinical outcomes of oocyte vitrification obtained in in vitro fertilization patients aged 30 to 39 years. Fertil Steril. 2013;99(7):1891–7.
Rienzi L, Romano S, Albricci L, Magguilli R, Capalbo A, Baroni E, et al. Embryo development of fresh ‘versus’ vitrified metaphase II oocytes after ICSI: a prospective randomized sibling-oocyte study. Hum Reprod. 2010;25(1):66–73.
Druckenmiller S, Goldman KN, Labella PA, Fino ME, Bazzocchi A, Noyes N. Successful oocyte cryopreservation in reproductive-aged cancer survivors. Obstet Gynecol. 2016;127(3):474–80.
Devine K, Mumford SL, Goldman KN, Hodes-Wertz B, Druckenmiller S, Propst AM, et al. Baby budgeting: oocyte cryopreservation in women delaying reproduction can reduce cost per live birth. Fertil Steril. 2015;103(6):1446–53.
Li Z, Wang YA, Ledger W, Edgar DH, Sullivan EA. Clinical outcomes following cryopreservation of blastocysts by vitrification or slow freezing: a population-based cohort study. Hum Reprod. 2014;29(12):2794–801.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Ethical approval
This study was approved by the institutional review board at the University of Southern California (HS-15-00628). Written informed consent was not required from participants for this retrospective study.
Funding
No external funding was received for this study.
Conflict of interest
The authors declare that they have no conflict of interest.
Electronic supplementary material
ESM 1
(DOCX 15 kb)
Rights and permissions
About this article
Cite this article
Ho, J.R., Woo, I., Louie, K. et al. A comparison of live birth rates and perinatal outcomes between cryopreserved oocytes and cryopreserved embryos. J Assist Reprod Genet 34, 1359–1366 (2017). https://doi.org/10.1007/s10815-017-0995-2
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s10815-017-0995-2