Abstract
Purpose
The goal of this study was to determine whether high E2 levels after controlled ovarian hyperstimulation affect TSH.
Methods
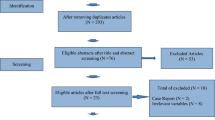
Patients completing ART cycles between April-October 2010 were eligible for this cohort study. 180 patients were recruited however those with known thyroid disease were excluded. The final analysis included 154 subjects. Blood was collected at each visit during the ART cycle as well as at the pregnancy test. Samples were frozen at −20 °C and analyzed together for E2 and TSH using the same assay kit once all patients had completed their cycles. All participants were treated at the McGill University Health Center. A paired t-test was used to study the difference in TSH levels recorded at maximal and minimal Estradiol levels during ovarian stimulation. Multiple regression analysis was then used to determine if factors such as anti-thyroid antibodies and ovarian reserve measures affect this change in TSH. We used multiple imputation methods to account for missing data.
Results
As E2 levels rose from low to supra-physiologic levels during treatment, TSH levels also rose significantly. This increase was clinically significant by the time of pregnancy test. The factors that potentially affected the change in TSH were: male factor/tubal factor infertility, type of protocol used as well as the presence of thyroid antibodies.
Conclusions
Although TSH increases during ART, this change only becomes clinically significant on the day of pregnancy test. Future studies should examine TSH changes specifically in certain “at-risk” sub-groups such as those with antibodies and known thyroid disease.
Similar content being viewed by others
References
Abalovich M, Gutierrez S, et al. Overt and subclinical hypothyroidism complicating pregnancy. Thyroid. 2002;12(1):63–8.
Alexander EK, Marqusee E, et al. Timing and magnitude of increases in levothyroxine requirements during pregnancy in women with hypothyroidism. N Engl J Med. 2004;351(3):241–9.
Arafah BM. Increased need for thyroxine in women with hypothyroidism during estrogen therapy. N Engl J Med. 2001;344(23):1743–9.
Baker V, Rone H, et al. Correlation of thyroid stimulating hormone (TSH) level with pregnancy outcome in women undergoing in vitro fertilization. Am J Obstet Gynecol. 2006;194(6):1668–74. discussion 1674–1665.
Bussen S, Steck T, et al. Increased prevalence of thyroid antibodies in euthyroid women with a history of recurrent in-vitro fertilization failure. Hum Reprod. 2000;15(3):545–8.
Canaris G, Manowitz N, et al. The Colorado thyroid disease prevalence study. Arch Intern Med. 2000;160(4):526–34.
Davis LB, Lathi RB, et al. The effect of infertility medication on thyroid function in hypothyroid women who conceive. Thyroid. 2007;17(8):773–7.
De Groot L, Abalovich M, et al. Management of thyroid dysfunction during pregnancy and postpartum: an Endocrine Society clinical practice guideline. J Clin Endocrinol Metab. 2012;97(8):2543–65.
Effraimidis G, Strieder TG, et al. Natural history of the transition from euthyroidism to overt autoimmune hypo- or hyperthyroidism: a prospective study. Eur J Endocrinol. 2011;164(1):107–13.
Escudero F, Gonzales GF, et al. Hormone profile during the menstrual cycle at high altitude. Int J Gynaecol Obstet. 1996;55(1):49–58.
Glinoer D. The regulation of thyroid function in pregnancy: pathways of endocrine adaptation from physiology to pathology. Endocr Rev. 1997;18(3):404–33.
Glinoer D, de Nayer P, et al. Regulation of maternal thyroid during pregnancy. J Clin Endocrinol Metab. 1990;71(2):276–87.
Goldsmith RE, Sturgis SH, et al. The menstrual pattern in thyroid disease. J Clin Endocrinol Metab. 1952;12(7):846–55.
Gracia CR, Morse CB, et al. Thyroid function during controlled ovarian hyperstimulation as part of in vitro fertilization. Fertil Steril. 2012;97(3):585–91.
Hofler M, Pfister H, et al. The use of weights to account for non-response and drop-out. Soc Psychiatry Psychiatr Epidemiol. 2005;40(4):291–9.
Hollowell JG, Staehling NW, et al. Serum TSH, T(4), and thyroid antibodies in the United States population (1988 to 1994): National Health and Nutrition Examination Survey (NHANES III). J Clin Endocrinol Metab. 2002;87(2):489–99.
Kilic S, Tasdemir N, et al. The effect of anti-thyroid antibodies on endometrial volume, embryo grade and IVF outcome. Gynecol Endocrinol. 2008;24(11):649–55.
Mandel SJ, Spencer CA, et al. Are detection and treatment of thyroid insufficiency in pregnancy feasible? Thyroid. 2005;15(1):44–53.
Mebis L, Van den Berghe G. Thyroid axis function and dysfunction in critical illness. Best Pract Res Clin Endocrinol Metab. 2011;25(5):745–57.
Mintziori G, Goulis DG, et al. “Thyroid function during ovarian stimulation: a systematic review.” Fertil Steril. 2011.
Muller AF, Verhoeff A, et al. Decrease of free thyroxine levels after controlled ovarian hyperstimulation. J Clin Endocrinol Metab. 2000;85(2):545–8.
Negro R, Formoso G, et al. Euthyroid women with autoimmune disease undergoing assisted reproduction technologies: the role of autoimmunity and thyroid function. J Endocrinol Invest. 2007;30(1):3–8.
Negro R, Mangieri T, et al. Levothyroxine treatment in thyroid peroxidase antibody-positive women undergoing assisted reproduction technologies: a prospective study. Hum Reprod. 2005;20(6):1529–33.
Poppe K, Glinoer D. Thyroid autoimmunity and hypothyroidism before and during pregnancy. Hum Reprod Update. 2003;9(2):149–61.
Poppe K, Unuane D, et al. Thyroid function after controlled ovarian hyperstimulation in women with and without the hyperstimulation syndrome. Fertil Steril. 2011;96(1):241–5.
Poppe K, Velkeniers B, et al. The role of thyroid autoimmunity in fertility and pregnancy. Nat Clin Pract Endocrinol Metab. 2008;4(7):394–405.
Reh A, Grifo J, et al. “What is a normal thyroid-stimulating hormone (TSH) level? Effects of stricter TSH thresholds on pregnancy outcomes after in vitro fertilization.” Fertil Steril. 2010.
Revelli A, Casano S, et al. A retrospective study on IVF outcome in euthyroid patients with anti-thyroid antibodies: effects of levothyroxine, acetyl-salicylic acid and prednisolone adjuvant treatments. Reprod Biol Endocrinol. 2009;7:137.
Rubin D. Multiple imputation for nonresponse in surveys. New York: Wiley; 1987.
Stuckey BG, Yeap D, et al. “Thyroxine replacement during super-ovulation for in vitro fertilization: a potential gap in management?” Fertil Steril. 2010 93(7): 2414 e2411–13.
Acknowledgments
The authors wish to thank Negin Zafar and Dr Fady Shehata for their contribution in data collection and database management. This study was funded in part by a research grant from the “Academic Enrichment Fund” of the Department of Obstetrics and Gynecology, McGill University, Montreal, Canada
Author disclosure statement
All authors declared they have no competing interests exist.
Author information
Authors and Affiliations
Corresponding author
Additional information
Capsule As estradiol levels rise during ART, TSH also rises. This rise may be affected by: cause of infertility, type of protocol used as well as the presence of anti-thyroid antibodies.
Rights and permissions
About this article
Cite this article
Reinblatt, S., Herrero, B., Correa, J.A. et al. Thyroid stimulating hormone levels rise after assisted reproductive technology. J Assist Reprod Genet 30, 1347–1352 (2013). https://doi.org/10.1007/s10815-013-0081-3
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s10815-013-0081-3