Abstract
Purpose
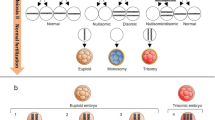
Preimplantation Genetic Diagnosis (PGD) has proven to be a useful reproductive option for carriers of some chromosome rearrangements. The data presented in this study compares the impact of one versus two blastomere biopsy on the likelihood of achieving a PGD result, as well as the effect on subsequent embryo development and clinical outcomes.
Methods
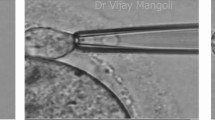
IVF-PGD couples had either one or two blastomeres biopsied from all embryos with ≥7 blastomeres on day 3 post oocyte collection. These blastomeres were assessed for the specific chromosome rearrangement using Fluorescent In-situ Hybridisation (FISH). Further embryo development was monitored on days 4 and 5. Clinical outcomes were assessed retrospectively.
Results
The data shows that statistically more embryos achieved a PGD result following two blastomere biopsy, compared with one blastomere biopsy (92 % versus 88 %, respectively). Furthermore it was found that embryo development and clinical outcomes were similar between the two biopsy groups.
Conclusions
Based on this analysis it appears that the biopsy of two blastomeres from embryos with ≥7 blastomeres on day 3 is a valid and successful approach for couples presenting for IVF-PGD for a chromosome rearrangement.

Similar content being viewed by others
References
Baart EB, Van Opstal D, Los FJ, Fauser BCJM, Martini E. Fluorescence in situ hybridization analysis of two blastomeres from day 3 frozen-thawed embryos followed by analysis of the remaining embryo on day 5. Hum Reprod. 2004;19:685–93.
Beyer CE, Osianlis T, Boekel K, Osborne E, Rombauts L, Catt J, Kralevski V, Aali BS, Gras L. Preimplantation genetic screening outcomes are associated with culture conditions. Hum Reprod. 2009;24:1212–20.
Cohen J, Wells D, Munne S. Removal of 2 cells from cleavage stage embryos is likely to reduce the efficacy of chromosomal tests that are used to enhance implantation rates. Fertil Steril. 2007;87:496–503.
De Vos A, Staessen C, De Rycke M, Verpoest W, Haentjens P, Devroey P, Liebaers I, Van de Velde H. Impact of cleavage-stage embryo biopsy in view of PGD on human blastocyst implantation: a prospective cohort of single embryo transfers. Hum Reprod. 2009;24:2988–96.
Emiliani S, Gonzalez-Merino E, Van den Bergh M, Delneste D, Englert Y, Abramowicz M. Correlation between fluorescence in-situ hybridization analyses and in-vitro development to blastocyst stage of embryos from Robertsonian translocation (13;14) carriers. Hum Reprod. 2002;17:2957–62.
Goossens V, De Rycke M, De Vos A, Staessen C, Michiels A, Verpoest W, Van Steirteghem A, Bertrand C, Liebaers I, Devroey P, Sermon K. Diagnostic efficiency, embryo development and clinical outcome after the biopsy of one or two blastomeres for preimplantation genetic diagnosis. Hum Reprod. 2007;23:481–92.
Harper JC, Coonen E, De Rycke M, Harton G, Moutou C, Pehlivan T, Traeger-Synodinos J, Van Rij M, Goossens V. ESHRE PGD consortium data collection X: cycles from January to December 2007 with pregnancy follow-up to October 2008. Hum Reprod. 2010;25:2685–707.
Harton GL, Magli MC, Lundin K, Montag M, Lemmen J, Harper JC. ESHRE PGD Consortium/Embryology Special Interest Group – best practice guidelines for polar body and embryo biopsy for preimplanation genetic diagnosis/screening (PGD/PGS). Hum Reprod. 2010;0:1–6.
Michiels A, Van Assche E, Liebaers I, Van Steirteghem A, Staessen C. The analysis of one or two blastomeres for PGD using fluorescence in-situ hybridisatiion. Hum Reprod. 2006;21:2396–402.
Munne S, Marquez C, Magli C, Morton P, Morrison L. Scoring criteria for preimplantation genetic diagnosis of numerical abnormalities for chromosomes X, Y, 13, 16, 18 and 21. Mol Hum Reprod. 1998;4:863–70.
Sandalinas M, Sadowy S, Alikani M, Calderon G, Cohen J, Munne S. Developmental ability of chromosomally abnormal human embryos to develop to the blastocyst stage. Hum Reprod. 2001;16:1954–8.
The Preimplantation Genetic Diagnosis International Society (PGDIS). Guidelines for good practice in PGD: programme requirements and laboratory quality assurance. RBM Online. 2008;16:134–47.
Van de Velde H, De Vos A, Sermon K, Staessen C, De Rycke M, Van Assche E, Lissens W, Vandervorst M, Van Ranst H, Liebaers I, Van Steirteghem A. Embryo implantation after biopsy of one or two cells from cleavage-stage embryos with a view to preimplantation genetic diagnosis. Prenat Diagn. 2000;20:1030–7.
Velilla E, Escudero T, Munne S. Blastomere fixation techniques and risk of misdiagnosis for preimplantation genetic diagnosis of aneuploidy. Reprod BioMed Online. 2002;4:210–7.
Acknowledgments
The authors wish to thank the following IVF clinics who participate in transport PGD through Monash IVF, for kindly agreeing to provide requested data on embryo development and clinical outcomes: Concept Fertility Centre, Hollywood Fertility Centre, Fertility Associates, Fertility Plus, Fertility Specialists of Western Australia, Monash IVF, Next Generation Fertility, Pivet and Repromed.
Author information
Authors and Affiliations
Corresponding author
Additional information
Capsule
The number of blastomeres biopsied from an embryo must be a careful balance between obtaining highly accuracy PGD results without compromising embryo quality and clinical outcomes.
Rights and permissions
About this article
Cite this article
Brodie, D., Beyer, C.E., Osborne, E. et al. Preimplantation genetic diagnosis for chromosome rearrangements – one blastomere biopsy versus two blastomere biopsy. J Assist Reprod Genet 29, 821–827 (2012). https://doi.org/10.1007/s10815-012-9782-2
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s10815-012-9782-2