Abstract
Purpose
Comparing the effects of metformin or orlistat on hormone, lipid profile and ovulation status in obese women with polycystic ovary syndrome.
Methods
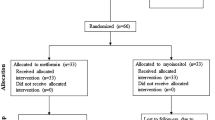
A total of 80 women were prospectively recruited to receive either metformin (n = 40) or orlistat (n = 40). Weight, BMI, waist, serum LH, total serum testosterone and lipid profile were assessed at baseline and after 3 months. The subjects’ ovulatory status was assessed after 3 months.
Results
There was no significant difference in ovulation between the two treatment groups (30% vs 15%). Treatment with either drug showed a significant decline in body weight, BMI (Body Mass Index), and waist circumference, but the degree of decline in both groups was the same. Patients who were treated with orlistat, showed a significant reduction in total testosterone and serum lipid. Women in metformin group showed a significant reduction in serum LH.
Conclusions
Both metformin and orlistat showed a similar effect on weight loss and ovulation rates.
Similar content being viewed by others
References
Adams H, Polson DW, Franks S. Prevalence of polycystic ovaries in women with anovulation and idiopathic hirsutism. Br Med J. 1986;293:355–9.
Hull MG. Epidemiology of infertility and polycystic ovarian disease: endocrinological and demographic studies. Gynaecol Endocrinol. 1987;1:235–45.
Azziz R, Woods KS, Reyna R, Key TJ, Knochenhauer ES, Yildiz BO. The prevalence and features of the polycystic ovary syndrome in an unselected population. J Clin Endocrinol Metab. 2004;89:2745–9.
Strowitzki T, Capp E, von Eye Corleta H. The degree of cycle irregularity correlates with the grade of endocrine and metabolic disorders in PCOS patients. Eur J Obstet Gynecol Reprod Biol. 2010;149:178–81.
Hahn S, Tan S, Elsenbruch S, Quadbeck B, Herrmann BL, Mann K, et al. Clinical and biochemical characterization of women with polycystic ovary syndrome in North Rhine-Westphalia. Horm Metab Res. 2005;37:438–44.
Azziz R, Carmina E, Dewailly D, Diamanti-Kandarakis E, Escobar-Morreale HF, Futterweit W, et al. The Androgen Excess and PCOS Society criteria for the polycystic ovary syndrome: the complete task force report. Fertil Steril. 2009;91:456–88.
Adams J, Franks S, Polson DW, Mason HD, Abdulwahid N, Tucker M, et al. Multi follicular ovaries: clinical and endocrine features and response to pulsatile gonadotrophin releasing hormone. Lancet. 1985;2:1375–9.
Azziz R, Carmina E, Dewailly D, Diamanti-Kandarakis E, Escobar-Morreale HF, Futterweit W, et al. Criteria for defining polycystic ovary syndrome as a predominantly hyperandrogenic syndrome: an Androgen Exess Society guidline. J Clin Endocrinol Metab. 2006;91:4237–45.
Dunaif A, Segal K, Futterweit W, Dobrjanky A. Profound peripheral resistance independent of obesity in polycystic ovary syndrome. Diabetes. 1989;38:1165–74.
Diamanti-Kandarakis E. Insulin resistance in PCOS. Endocr. 2006;30:13–7.
Azziz R, Marin C, Hoq L, Badamgarav E, Song P. Health care-related economic burden of the polycystic ovary syndrome during the reproductive life span. J Clin Endocrinol Metab. 2005;90:4650–8.
Chang RJ. A practical approach to the diagnosis of polycysticovary syndrome. Am J Obstet Gynecol. 2004;191:713–7.
Richardson MR. Current perspectives in polycystic ovary syndrome. Am Fam Physician. 2003;68:697–704.
Nestler JE, Jakubowicz DJ, de Vargas AF, Brik C, Quintero N, Medina F. Insulin stimulates testosterone biosynthesis by human thecal cells from women with polycystic ovary syndrome by activating its own receptor and using inositolglycan mediators as the signal transduction system. J Clin Endocrinol Metab. 1998;83:2001–5.
Azziz R, Ehrmann DA, Legro RS, Fereshetian AG, O’Keefe M, Ghazzi MN. PCOS/Troglitazone Study Group. Troglitazone decreases adrenal androgen levels in women with polycystic ovary syndrome. Fertil Steril. 2003;79:932–7.
Caballero B. The global epidemic of obesity: an overview. Epidemiol Rev. 2007;29:1–5.
Sturm R. Increases in morbid obesity in the USA: 2000–2005. Public Health. 2007;121:492–6.
Legro RS, Finegood D, Dunaif A. A fasting glucose to insulin ratio is a useful measure of insulin sensitivity in women with polycystic ovary syndrome. J Clin Endocrinol Metab. 1998;83:2694–8.
Carmina E, Lobo RA. Polycystic ovary syndrome: arguably the most common endocrinopathy is associated with significant morbidity in women. J Clin Endocrinol Metab. 1999;84:1897–9.
Kiddy DS, Hamilton-Fairley D, Bush A, Anyaoku V, Reed MJ, Franks S. Improvement in endocrine and ovarian function during dietary treatment of obese women with polycystic ovary syndrome. Clin Endocrinol. 1992;36:1105–11.
Clark AM, Ledger W, Galletly C, Tomlinson L, Blaney F, Wang X, et al. Weight loss results in significant improvement in pregnancy and ovulation rates in anovulatory obese women. Hum Reprod. 1995;10:2705–12.
Lord JM, Flight IH, Norman RJ. Insulin-sensitising drugs (metformin, troglitazone, rosiglitazone, pioglitazone, D-chiroinositol) for polycystic ovary syndrome. Cochrane Database Syst Rev. 2003;(3):CD003053.
Dixon JB. Weight loss medications—where do they fit in? Aust Fam Physician. 2006;35:576–9.
Padwal RS, Majumdar SR. Drug treatments for obesity: orlistst, sibutramine, and rimonabant. Lancet. 2007;369:71–7.
Unluhizarci K, Kelestimur F, Bayram F, Sahin Y, Tutus A. The effects of metformin on insulin resistance and ovarian steroidogenesis in women with polycystic ovary syndrome. Clin Endocinol (Oxf). 1999;51:231–6.
Hanjalic-beck A, Gabriel B, Schaefer W, Zahradnik HP, Schories M, Tempfer C. Metformin versus acarbose therapy in patients with polycystic ovary syndrome: a prospective randomized double—blind study. Gynecol Endocrinol. 2010;26:690–7.
Palomba S, Orio F, Falbo A, Manguso F, Russo T, Cascella T. Prospective parallel randomized, double—blind, double—dummy controlled clinical trial comparing clomiphene citrate and metformin as the first line treatment for ovulation induction in nonobese anovulatory women with poycystic ovary syndrome. J Clin Endocrinol Metab. 2005;90:4068–74.
Palomba S, Orio F, Falbo A, Russo T, Tolino A. Clomiphene citrate versus metformin as first line approach for the treatment of anovulation in infertile patients with polycystic ovary syndrome. J Clin Endocrinol Metab. 2007;92:3498–503.
Cho LW, Kilpatrick ES, Keevil BG, Coady AM, Atkin SL. Effect of metformin, orlistat and pioglitazone treatment on mean insulin resistance and its biological variability in polycystic ovary syndrome. Clin Endocrinol (Oxf). 2009;70:233–7.
Jayagopal V, Kilpatric ES, Holding S, Jennings PE, Atkin SL. Orlistat is as beneficial as metformin in the treatment of polycystic ovary syndrome. J Clin Endocrinol Metab. 2005;90:729–33.
Metwally M, Amer S, Li TC, Ledger WL. An RCT of metformin versus orlistat for the management of obese anovulatory women. Hum Reprod. 2009;24:966–75.
Lord JM, Flight IH, Norman RJ. Metformin in polycystic ovary syndrome: systematic review and metaanalysis. BMJ. 2003;327:951–3.
De Sloover Koch Y, Ernst ME. Use of metformin in polycystic ovary syndrome. Ann Pharmacother. 2001;35:1644–7.
English PJ, Ashcroft A, Patterson M, Dovey TM, Halford JC, Harrison J, et al. Metformin Prolongs the postprandial fall in plasma ghrelin concentrations in type 2 diabetes. Diab Metab Res Rev. 2007;23:299–303.
Yasuda N, Inoue T, Nagakura T, Yamazaki K, Kira K, Saeki T, et al. Metformin causes reduction of food intake and body weight gain and improvement of glucose intolerance in combination with dipeptidyl peptidase IV inhibitor in Zucker fa/fa rats. J Pharmacol Exp Ther. 2004;310:614–9.
Huber-Buchholz MM, Carey DG, Norman RJ. Restoration of reproductive potential by lifestyle modification in obese polycystic ovary syndrome: role of insulin sensitivity and luteinizing hormone. J Clin Endocrinol Metab. 1999;84:1470–4.
Clark AM, Thirnley B, Tomlinson L, Galletley C, Norman RJ. Weight loss in obese infertile women results in improvement in reproductive outcome for all forms of fertility treatment. Hum Reprod. 1998;13:1502–5.
Pasquali R, Antenucci D, Casmirri F, Venturoli S, Paradisi R, Fabbri Rm, et al. Clinical and hormonal characteristics of obese amenorrheic hyperandrogenic women before and after weight loss. J Clin Endocrinol Metab. 1989;68:173–9.
Agarwal N, Rice SP, Bolusani H, Luzio SD, Dunseath M, Rees DA. Metformin reduces arterial stiffness and improves endothelial function in young women with polycystic ovary syndrome: a randomized, placebo—controlled, crossover trial. J Clin Endocrinol Metab. 2010;95:722–30.
Nestler JE, Jakubowics DJ, Evans WS, Pasquali R. Effects of metformin on spontaneous and clomiphene induced ovulation in the polycystic ovary syndrome. N Engl J Med. 1998;338:1876–80.
Moghetti P, Castello R, Negri C, Tosi F, Perrone F. Metformin effects on clinical features, endocrine and metabolic profiles, and insulin sensitivity in polycystic ovary syndrome: a randomized double-blind, placebo—controlled 6 month trial, followed by open long-term clinical evaluation. J Clin Endocrinol Metab. 2000;85:139–46.
Velazquez EM, Mendoza S, Hamer T, Sosa F. Metformin therapy in polycystic ovary syndrome reduces hyperinsulinemia, insulin resistance, hyperandrogenemia and systolic blood pressure, while facilitating normal menses and pregnancy. Metabolism. 1994;43:647–54.
Eisenhardt S, Schwarzmann N, Henschel V, Germeyer A. Early effects of metformin in women with polycystic ovary syndrome: a prospective randomized, double—blind, placebo—controlled trial. J Clin Endocrinol Metab. 2006;91:946–52.
Morin-papunem LC, Koivunem RM, Ruokonen A. Metformin therapy improves the menstrual pattern with minimal endocrine and metabolic effects in women with polycystic ovary syndrome. Fertil Steril. 1998;69:691–6.
Velazquez EM, Acosta A, Mendoza SG. Menstrual cyclicity after metformin therapy in polycystic ovary syndrome. Obstet Gynecol. 1997;90:392–5.
Nestler JE, Stovall D, Akhter N, Iuorno MJ, Jacubwicz DJ. Strategies for the use of insulin-sensitizing drugs to treat infertility in women with polycystic ovary syndrome. Fertil Steril. 2002;77:209–15.
Andersen P, Seljeflot I, Abdelnoor M, Arnesen H, Dale PO, Lovik A, et al. Increased insulin sensitivity and fibrinolytic capacity after dietary intervention in obese women with polycystic ovary syndrome. Metabolism. 1995;44:611–6.
Hamilton-Fairley D, Kiddy D, Anyaoku V, Koistinen R, Seppala M, Franks S. Response of sex hormone binding globulin and insulin- like growth factor binding protein −1 to an oral glucose tolerance test in obese women with polycystic ovary syndrome before and after calorie restriction. Clin Endocrinol (Oxf). 1993;39:363–7.
Kiddy DS, Hamilton-Fairley D, Seppala M, Koistinen R, James VH, Reed MJ, et al. Diet-induced changes in sex hormone binding globulin and free testosterone in women with normal or polycystic ovaries: correlation with serum insulin and insulin- like growth factor. J Clin Endocrinol (Oxf). 1989;31:757–63.
Poretsky L, Cataldo NA, Rosenwaks Z, Giudice LA. The insulin—related ovarian regulatory system in health and disease. Endocr Rev. 1999;20:535–82.
Soldani R, Cagnacci A, Yen SS. Insulin, insulin-like growth factor I (IGF-I) and IGF-II enhance basal and gonadotrophin-releasing hormone-stimulated luteinizing hormone release from rat anterior pituitary cells in vitro. Eur J Endocrinol. 1994;131:641–5.
Soldani R, Cagnacci A, Paoletti AM, Yen SS, Melis GB. Modulation of anterior pituitary luteinizing hormone response to gonadotropin-releasing hormone by insulin-like growth factor I in vitro. Fertil Steril. 1995;64:634–7.
Acknowledgements
The authors especially thank Dr Hossein Fallahzadeh for his assistance in statistical analysis of the data. This study was supported by a grant from the Research and Clinical Center for Infertility, Shahid Sadoughi University of Medical Sciences and Sabzevar University of Medical Sciences, Sabzevar, Iran.
Author information
Authors and Affiliations
Corresponding author
Additional information
Capsule
Metformin and orlistat show a similar effect on weight loss and ovulation rates in obese PCOS patients.
Rights and permissions
About this article
Cite this article
Ghandi, S., Aflatoonian, A., Tabibnejad, N. et al. The effects of metformin or orlistat on obese women with polycystic ovary syndrome: a prospective randomized open-label study. J Assist Reprod Genet 28, 591–596 (2011). https://doi.org/10.1007/s10815-011-9564-2
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s10815-011-9564-2