Abstract
Puerose: To demonstrate our hypothesis that a correlation exists between oocyte maturity and a decrease in intraovarian blood flow resistance in assisted reproductive technology (ART) treatment cycles, oocyte maturity and total antioxidant status (TAOS) in follicular fluid was examined.
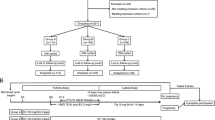
Methods: A total of 59 cycles involving 51 infertile patients undergoing ART treatment in our hospital were recruited in this study. The ART cycles were divided into two groups: deeply decreased (DD) group and not-deeply decreased (NDD) group, according to the pulsatility index (PI) values for perifollicular arterial blood flow before and after hCG administration. The PI values that showed a decrease in their PI after hCG administration of 10% or more were defined “deeply decreased” and showed a decrease of less than 10% were considered “not-deeply decreased.” The recovery rates of mature and immature oocytes and TAOS in follicular fluid were compared between the two groups.
Results: Mature and immature oocyte recovery rates in the DD group (62.5% and 17.2%) were significantly higher and lower, respectively, than those in the NDD group (41.7% and 38.3%, p < 0.05). The TAOS (1.55 ± 0.44 mmol/L) of the DD group was significantly lower than that in the NDD group (1.68 ± 0.47 mmol/L, p < 0.05).
Conclusions: The decrease in intraovarian arterial blood flow resistance measured after hCG administration may be a good indicator of retrieving mature oocyte.

Similar content being viewed by others
References
Nakahara K, Saito H, Saito H, Ito M, Ohta N, Sakai N, Tezuka N, Hiroi M, Watanabe H. Incidence of apoptotic bodies in membrane granulosa of the patients participating in an in vitro fertilization program. Fertil Steril 1997;67:302–3088
Seino T, Saito H, Kaneko T, Takahashi T, Kawachiya S, Kurachi H. Eight-hydroxy-2′-deoxyguanosine in granulosa cells is correlated with the quality of oocytes and embryos in an in vitro fertilization-embryo transfer program. Fertil Steril 2002;77:1184–90
Toya M, Saito H, Ohta N, Saito T, Kaneko T, Hiroi M. Moderate and severe endometriosis is associated with alterations in the cell cycle of granulosa cells in patients undergoing in vitro fertilization and embryo transfer. Fertil Steril 2000;73:344–50
Saito H, Kaneko T, Takahashi T, Kawachiya S, Saito T, Hiroi M. Hyaluronan in follicular fluids and fertilization of oocytes. Fertil Steril 2000;74:1148–52
Campbell S, Bourne TH, Waterstone J, Reynolds KM, Crayford TJB, Jurkovic D, Okokon EV, Collins WP. Transvaginal color blood flow imaging of the periovulatory follicle. Fertile Steril 1993;60:433–8
Collins W, Jurkovic D, Bourne T, Kurjak A, Campbell S. Ovarian morphology, endocrine function and follicular blood flow during the peri-ovulatory period. Hum Reprod 1991;6:319–24
Sladkevicius P, Valentin L, Marsal K. Blood flow in the uterine and ovarian arteries during the normal menstrual cycle. Ultrasound Obstet Gynecol 1993;3:199–208
Tan SL, Zaidi J, Campbell S, Doyle P, Collins W. Blood flow changes in the ovarian and uterine arteries during the normal menstrual cycle. Am J Obstet Gynecol 1996;175:625–31
Van Blerkom J, Antczak M, Schrader R. The developmental potential of the human oocyte is related to the dissolved oxygen content of follicular fluid: association with vascular endothelial growth factor levels and perifollicular blood flow characteristics. Hum Reprod 1997;12:1047–55
Van Blerkom J. Epigenetic influences on oocyte developmental competence: perifollicular vascularity and intrafollicular oxygen. J Assist Reprod Genet 1998;15:226–34
Coulam CB, Goodman C, Rinehart JS. Colour Doppler indices of follicular blood flow as predictors of pregnancy after in-vitro fertilization and embryo transfer. Hum Reprod 1999;14:1979–82
Nakagawa K, Ozawa N, Takamatsu K, Takahashi Y, Irahara M, Yoshimura Y, Saito H. A reduction in intraovarian arterial blood flow resistance after ovulation is necessary to achieve pregnancy in natural cycle. J Assist Reprod Genet 2005;22:9–14
Nakagawa K, Takahashi Y, Ito M, Horikawa T, Ohgi S, Irahara M, Saito H. Intraovarian arterial blod flow resistance in oligomenorrheal infertile women. J Assist Reprod Genet 2006;23:105–10
Baynes JW. Role of oxidative stress in development of complications in diabetes. Diabetes 1991;40:405–12
Giugliano D, Ceriello A, Paolisso G. Oxidative stress and diabetic vascular complications. Diabetes Care 1996;19:257–67
Tarin JJ, Vendrell Fj, ten J, Cano A. Antioxidant therapy counteracts the disturbring effects of diamide and maternal aging on meiotic division and chromosomal segregation in mouse oocytes. Mol Hum Reprod 1998;4:281–2
Betteridge DJ. What is the oxidative stress?a Metabolism 2000;49(suppl 1):3–8
Fenkci V, Fenksi S, Yilmazer M, Serteser M. Decreased total antioxidant state and increased oxidative stress in women with polycystic ovary syndrome may contribute to the risk of cardiovascular disease. Fertil Steril 2003;80:123–7
Saito H, Takakazu S, Kaneko T, Sasagawa I, Kuramoto T, Hiroi M. Relatively poor oocyte quality is an indication for intracytoplasmic injection. Fertil Steril 2000, 73:465–9
Saito H, Hiroi M. Corelation between the follicular gonadotropin inhibitor and the maturity of the ovum-corona cumulus complex. Fertil Steril 1986;46:66–672
Agarwal A, Gupta S, Sharma RK. Role of oxidative stress in female reproduction. Reprod Biol Endcrinol 2005;3:28
Espey LL. Ovulation as an inflammatory reaction—a hypothesis. Biol Reprod 1980;23:73–106
Fujii J, Iuchi Y, Okada F. Fundamental roles of reactive oxygen species and protective mechanism in the female reproductive system. Reprod Biol Endocrinol 2005;3:43
Yoshimura Y, Espey LL, Hosoi Y, Adachi T, Atlas SJ, Ghodgaonkar RB, Dubin NH, Wallach EE. The effects of bradikinin on ovulation and prostaglandin production by the perfused rabbit ovary. Endocrinology 1988;122:2540–6
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
About this article
Cite this article
Nakagawa, K., Ohgi, S., Kojima, R. et al. Reduction of perifollicular arterial blood flow resistance after hCG administration is a good indicator of the recovery of mature oocytes in ART treatment. J Assist Reprod Genet 23, 433–438 (2006). https://doi.org/10.1007/s10815-006-9087-4
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s10815-006-9087-4