Abstract
Purpose
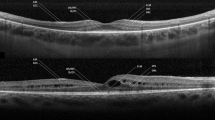
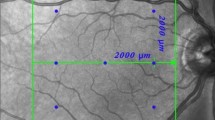
To evaluate spectral domain optical coherence tomography (SD-OCT) findings of 42 eyes with pars planitis and to identify risk factors affecting visual acuity.
Methods
Medical records and SD-OCT findings were retrospectively reviewed.
Results
Mean best-corrected visual acuity (BCVA) was 0.248 ± 0.3 on the logMAR scale at baseline. SD-OCT findings included epiretinal membrane (ERM) in 16 (38.1%) eyes, loss of normal foveal contour appearance in 8 (19.0%), ellipsoid zone (EZ) damage in 5 (11.9%), external limiting membrane (ELM) damage in 3 (7.1%), disruption of retinal pigment epithelium (RPE) in 2 (4.8%), and macular atrophy in 1 (2.4%). There was macular edema in 10 (23.8%) eyes [cystoid macular edema (CME) in 8 (19.0%), diffuse macular edema (DME) in 6 (14.3%), and serous retinal detachment in 2 (4.8%)]. The mean central macular thickness (CMT) was 272.1 ± 319.5 μm. Patients were followed up for a mean of 50.6 ± 36.7 months. Mean BCVA was 0.210 ± 0.3 at the final evaluation. SD-OCT findings included ERM in 28 (66.7%) eyes, EZ damage in 6 (14.3%), ELM damage in 3 (7.1%), disruption of RPE in 4 (9.5%), loss of normal foveal contour appearance in 12 (28.6%), and macular atrophy in 2 (4.8%). There was CME and/or DME in 6 (14.3%) eyes. The mean CMT was 238 ± 220.9 μm and was significantly lower than the baseline (p < 0.001). According to multivariate linear regression analysis, the presence of DME, and loss of normal foveal contour appearance at baseline were the independent factors associated with BCVA at the final examination (B = 0.726, p < 0.001; B = 0.766, p < 0.001, respectively).
Conclusions
DME and loss of normal foveal contour appearance were more likely to have adverse effects on visual acuity.


Similar content being viewed by others
References
Jabs DA, Nussenblatt RB, Rosenbaum JT, Standardization of Uveitis Nomenclature (SUN) Working Group (2005) Standardization of uveitis nomenclature for reporting clinical data. Results of the first ınternational workshop. Am J Ophthalmol 140(3):509–516. https://doi.org/10.1016/j.ajo.2005.03.057
Guest S, Funkhouser E, Lightman S (2001) Pars planitis: a comparison of childhood onset and adult onset disease. Clin Exp Ophthalmol 29(2):81–84. https://doi.org/10.1046/j.1442-9071.2001.d01-7.x
Ozdal PC, Sen E, Yazici A, Ozturk F (2012) Patterns of childhood-onset uveitis in a referral center in Turkey. J Ophthalmic Inflamm Infect 2(1):13–19. https://doi.org/10.1007/s12348-011-0044-8
Paroli MP, Spinucci G, Liverani M, Monte R, Pezzi PP (2009) Uveitis in childhood: an Italian clinical and epidemiological study. Ocul Immunol Inflamm 17(4):238–242. https://doi.org/10.1080/09273940802702561
Smith JA, Mackensen F, Sen HN et al (2009) Epidemiology and course of disease in childhood uveitis. Ophthalmology 116(8):1544–1551. https://doi.org/10.1016/j.ophtha.2009.05.002
Yalçındağ FN, Özdal PC, Özyazgan Y, Batıoğlu F, Tugal-Tutkun I, BUST Study Group (2018) Demographic and clinical characteristics of Uveitis in Turkey: the first national registry report. Ocul Immunol Inflamm 26(1):17–26. https://doi.org/10.1080/09273948.2016.1196714
Paroli MP, Spinucci G, Monte R, Pesci FR, Abicca I, Pezzi PP (2011) Intermediate uveitis in a pediatric Italian population. Ocul Immunol Inflamm 19(5):321–326. https://doi.org/10.3109/09273948.2011.603878
Romero R, Peralta J, Sendagorta E, Abelairas J (2007) Pars planitis in children: epidemiologic, clinical, and therapeutic characteristics. J Pediatr Ophthalmol Strabismus 44(5):288–293. https://doi.org/10.3928/01913913-20070901-03
Tugal-Tutkun I (2011) Pediatric uveitis. J Ophthalmic Vis Res 6(4):259–269
Donaldson MJ, Pulido JS, Herman DC, Diehl N, Hodge D (2007) Pars planitis: a 20-year study of incidence, clinical features, and outcomes. Am J Ophthalmol 144(6):812–817. https://doi.org/10.1016/j.ajo.2007.08.023
Nikkhah H, Ramezani A, Ahmadieh H et al (2011) Childhood pars planitis; clinical features and outcomes. J Ophthalmic Vis Res 6(4):249–254
Rosenberg KD, Feuer WJ, Davis JL (2004) Ocular complications of pediatric uveitis. Ophthalmology 111(12):2299–2306. https://doi.org/10.1016/j.ophtha.2004.06.014
de Boer J, Steijaert A, van den Bor R, Stellato R, Norel JO (2015) Development of macular edema and impact on visual acuity in uveitis associated with juvenile idiopathic arthritis. Ocul Immunol Inflamm 23(1):67–73. https://doi.org/10.3109/09273948.2013.871566
Salcedo-Villanueva G, Arellanes-Garcia L, Fromow-Guerra J, Hernández-Quintela E (2014) Association of epiretinal membranes with macular edema in pars planitis. Arch Soc Esp Oftalmol 89(1):22–26. https://doi.org/10.1016/j.oftal.2013.09.008
Grajewski RS, Boelke AC, Adler W, Meyer S, Caramoy A, Kirchhof B, Cursiefen C, Heindl LM (2016) Spectral-domain optical coherence tomography findings of the macula in 500 consecutive patients with uveitis. Eye (Lond) 30(11):1415–1423. https://doi.org/10.1038/eye.2016.133
Roesel M, Henschel A, Heinz C, Spital G, Heiligenhaus A (2008) Time-domain and spectral-domain optical coherence tomography in uveitic macular edema. Am J Ophthalmol 146(4):626–627. https://doi.org/10.1016/j.ajo.2008.06.023
Lehpamer B, Moshier E, Pahk P, Goldberg N, Ackert J, Godbold J, Jabs DA (2014) Epiretinal membranes in uveitic macular edema: effect on vision and response to therapy. Am J Ophthalmol 157(5):1048–1055. https://doi.org/10.1016/j.ajo.2014.01.020
Hee MR, Puliafito CA, Wong C, Duker JS, Reichel E, Rutledge B, Schuman JS, Swanson EA, Fujimoto JG (1995) Quantitative assessment of macular edema with optical coherence tomography. Arch Ophthalmol 113(8):1019–2029. https://doi.org/10.1001/archopht.1995.01100080071031
Cunningham ET Jr, van Velthoven ME, Zierhut M (2014) Spectral-domain-optical coherence tomography in uveitis. Ocul Immunol Inflamm 22(6):425–428. https://doi.org/10.3109/09273948.2014.982060
de Boer J, Berendschot TT, van der Does P, Rothova A (2006) Long-term follow-up of intermediate uveitis in children. Am J Ophthalmol 141(4):616–621. https://doi.org/10.1016/j.ajo.2005.09.035
Prieto JF, Dios E, Gutierrez JM, Mayo A, Calonge M, Herreras JM (2001) Pars planitis: epidemiology, treatment, and association with multiple sclerosis. Ocul Immunol Inflamm 9(2):93–102. https://doi.org/10.1076/ocii.9.2.93.3975
Arellanes-García L, Navarro-López L, Recillas-Gispert C (2003) Pars planitis in the Mexican Mestizo population: ocular findings, treatment, and visual outcome. Ocul Immunol Inflamm 11(1):53–60. https://doi.org/10.1076/ocii.11.1.53.15583
Sancho L, Kramer M, Koriat A, Eiger-Moscovich M, Sharon Y, Amer R (2019) Complications in intermediate uveitis: prevalence, time of onset, and effects on vision in short-term and long-term follow-up. Ocul Immunol Inflamm 27(3):447–455. https://doi.org/10.1080/09273948.2017.1420203
Navarrete A, Koriat A, Amer R (2020) Implications of pars planitis-associated cystoid macular edema on visual outcome and management in children. Graefes Arch Clin Exp Ophthalmol 258(8):1803–1811. https://doi.org/10.1007/s00417-020-04696-7
Jain R, Ferrante P, Reddy GT, Lightman S (2005) Clinical features and visual outcome of intermediate uveitis in children. Clin Exp Ophthalmol 33(1):22–25. https://doi.org/10.1111/j.1442-9071.2005.00938.x
Eser-Ozturk H, Sullu Y (2020) Pediatric uveitis in a referral center in north part of Turkey. Ocul Immunol Inflamm 28:1–5. https://doi.org/10.1080/09273948.2020.1758158
Malinowski SM, Pulido JS, Folk JC (1993) Long-term visual outcome and complications associated with pars planitis. Ophthalmology 100(6):818–824. https://doi.org/10.1016/s0161-6420(93)31567-8
Reiff A (2020) Clinical presentation, management, and long-term outcome of pars planitis, panuveitis, and Vogt-Koyanagi-Harada disease in children and adolescents. Arthritis Care Res (Hoboken) 72(11):1589–1596. https://doi.org/10.1002/acr.24056
Markomichelakis N, Halkiadakis I, Pantelia E et al (2004) Patterns of macular edema in patients with uveitis: qualitative and quantitative assessment using optical coherence tomography. Ophthalmology 111(5):946–952. https://doi.org/10.1016/j.ophtha.2003.08.037
Iannetti L, Tortorella P, D’Ambrosio E, Spena R, Zito R, Gharbiya M (2013) Epiretinal membranes in patients with uveitis: morphological and functional analysis with spectral domain optical coherence tomography. BioMed Res Int 2013:284821. https://doi.org/10.1155/2013/284821
Massamba N, Jennifer ML, Lehoang P, Sellam A, Bodaghi B (2017) Analysis of outer nuclear and external limiting membrane layers pattern on spectral-domain optical coherence tomography ın patients with posterior uveitis with or without cystoid macular edema. J Ophthalmol Clin Res 4:37. https://doi.org/10.24966/OCR-8887/100037
Gonzales CA, Ladas JG, Davis JL, Feuer WJ, Holland GN (2001) Relationships between laser flare photometry values and complications of uveitis. Arch Ophthalmol 119(12):1763–1769. https://doi.org/10.1001/archopht.119.12.1763
Davis JL, Dacanay LM, Holland GN, Berrocal AM, Giese MJ, Feuer WJ (2003) Laser flare photometry and complications of uveitis in children. Am J Ophthalmol 135(6):763–771. https://doi.org/10.1016/s0002-9394(03)00315-5
Eiger-Moscovich M, Tomkins-Netzer O, Amer R, Habot-Wilner Z, Kasb A, Friling R, Kramer M (2019) Visual and clinical outcome of macular edema complicating pediatric noninfectious uveitis. Am J Ophthalmol 202:72–78. https://doi.org/10.1016/j.ajo.2019.02.011
Funding
SD-OCT device was supported by the Ankara University Scientific Projects (Project number: 15A0230008).
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflict of interest
The authors declare that they have no conflict of interest.
Ethics approval
Our study was performed in adherence to the tenets of the Declaration of Helsinki. No institutional review board approval is required for chart review studies.
Informed consent
Informed consent was obtained from all individual participants included in the study.
Additional information
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
About this article
Cite this article
Yalçındağ, F.N., Temel, E. & Özgür, E.G. Spectral domain optical coherence tomography findings of patients with pars planitis and risk factors affecting visual acuity. Int Ophthalmol 41, 1753–1761 (2021). https://doi.org/10.1007/s10792-021-01734-z
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s10792-021-01734-z