Abstract
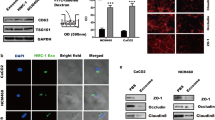
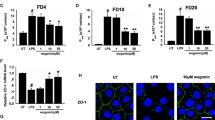
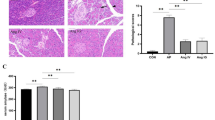
To explore the correlation between altered expression of mast cells and PAR-2 and impaired mucosal barrier in NSAIDs enteropathy through animal and cell experiments, and to elucidate the role of mast cells and PAR-2 in the pathogenesis of NSAIDs enteropathy and the regulatory mechanism of the tight junction of intestinal epithelium. Animal experiments: the NSAIDs-related small intestine injury model was established by intragastric administration of diclofenac sodium, and mast cells were detected by toluidine blue staining. Cell experiments: Intestinal epithelial cell line (IEC-6) was applied with diclofenac sodium and its activity was detected by CCK-8.IEC-6 and RBL-2H3 were co-cultured to evaluate the permeability of intestinal epithelial cells by detecting the concentration of potassium ion and LDH. The expressions of tight junction proteins (zo-1, claudin-1, occludin), cytoskeletal components (actin, tubulin, keratin) and par-2 were analyzed by Western Blot. In animal experiments, the number of mast cells was significantly increased after 24 h of action of diclofenac sodium. In cell experiments, the survival rate of IEC-6 cells decreased significantly when the concentration of diclofenac sodium is more than 50 μg/mL; after 24 h of co-culture, the potassium and LDH concentration in the co-culture group were significantly higher, and the expression of ZO-1, claudin-1, occludin, tubulin, and keratin was decreased. Mast cells activate PAR-2 in intestinal epithelial cells, downregulate the related proteins of cell tight junctions and cytoskeletal proteins, and increase the permeability of intestinal epithelial cells.






Similar content being viewed by others
Data Availability
The datasets used and/or analyzed during the current study are available from the corresponding author on reasonable request.
References
Sugimori, S., T. Watanabe, M. Tabuchi, N. Kameda, H. Machida, H. Okazaki, T. Tanigawa, H. Yamagami, M. Shiba, K. Watanabe, K. Tominaga, Y. Fujiwara, N. Oshitani, T. Koike, K. Higuchi, and T. Arakawa. 2008. Evaluation of small bowel injury in patients with rheumatoid arthritis by capsule endoscopy: effects of anti-rheumatoid arthritis drugs. Digestion 78 (4): 208–213.
Otani, K., T. Tanigawa, T. Watanabe, S. Shimada, Y. Nadatani, Y. Nagami, F. Tanaka, N. Kamata, H. Yamagami, M. Shiba, K. Tominaga, Y. Fujiwara, and T. Arakawa. 2017. Microbiota Plays a Key Role in Non-Steroidal Anti-Inflammatory Drug-Induced Small Intestinal Damage. Digestion 95 (1): 22–28.
Theoharides TC, Tsilioni I, Conti P (2019) Mast Cells May Regulate The Anti-Inflammatory Activity of IL-37. Int J Mol Sci 20 (15): 3701.
Kodani, M., H. Fukui, T. Tomita, T. Oshima, J. Watari, and H. Miwa. 2018. Association between gastrointestinal motility and macrophage/mast cell distribution in mice during the healing stage after DSS-induced colitis. Molecular Medicine Reports 17 (6): 8167–8172.
Pohl CS, Medland JE, Mackey E, Edwards LL, Bagley KD, DeWilde MP,et al (2017) Early weaning stress induces chronic functional diarrhea, intestinal barrier defects, and increased mast cell activity in a porcine model of early life adversity. Neurogastroenterol Motil 29 (11). https://doi.org/10.1111/nmo.13118.
Tai, F.W.D. 2018. McAlindon ME.NSAIDs and the small bowel. Current Opinion in Gastroenterology 34 (3): 175–182.
Sato, H., L.S. Zhang, K. Martinez, E.B. Chang, Q. Yang, F. Wang, P.N. Howles, R. Hokari, S. Miura, and P. Tso. 2016. Antibiotics suppress activation of intestinal mucosal mast cells and reduce dietary lipid absorption in Sprague-Dawley rats. Gastroenterology. 151 (5): 923–932.
Utzeri, E., and P. Usai. 2017. Role of non-steroidal anti-inflammatory drugs on intestinal permeability and nonalcoholic fatty liver disease. World Journal of Gastroenterology 23 (22): 3954–3963.
Adebayo, D., and I. Bjarnason. 2006. Is non-steroidal anti-inflammatory drug (NSAID) enteropathy clinically more important than NSAID gastropathy? Postgraduate Medical Journal 82 (965): 186–191.
Graham, D.Y., A.R. Opekun, F.F. Willingham, and W.A. Qureshi. 2005. Visible small-intestinal mucosal injury in chronic NSAID users. Clinical Gastroenterology and Hepatology 3 (1): 55–59.
Lanas, A., and F. Sopeña. 2009. Nonsteroidal anti-inflammatory drugs and lower gastrointestinal complications. Gastroenterology Clinics of North America 38 (2): 333–352.
Scarpignato, C., and R.H. Hunt. 2010. Nonsteroidal antiinflammatory drug-related injury to the gastrointestinal tract: clinical picture, pathogenesis, and prevention. Gastroenterology Clinics of North America 39 (3): 433–464.
Bjarnason, I., C. Scarpignato, E. Holmgren, M. Olszewski, K.D. Rainsford, and A. Lanas. 2018. Mechanisms of damage to the gastrointestinal tract from nonsteroidal anti-inflammatory drugs. Gastroenterology. 154 (3): 500–514.
Scarpignato, C. 2008. NSAID-induced intestinal damage: are luminal bacteria the therapeutic target? Gut 57 (2): 145–148.
Zhao, W., X. Huang, X. Han, D. Hu, X. Hu, Y. Li, et al. 2018. Resveratrol suppresses gut-derived NLRP3 inflammasome partly through stabilizing mast cells in a rat model. Mediators of Inflammation 2018: 6158671.
Söderholm, J.D., P.C. Yang, P. Ceponis, A. Vohra, R. Riddell, P.M. Sherman, et al. 2002. Chronic stress induces mast cell-dependent bacterial adherence and initiates mucosal inflammation in rat intestine. Gastroenterology. 123 (4): 1099–1108.
Xu, N., Z. Yu, X. Cao, Z. Wang, and M. Yan. 2017. Characteristics of nonsteroidal anti-inflammatory drugs (NSAIDs)-induced small bowel injury identified by single-balloon endoscopy or capsule endoscopy. Medical Science Monitor 23: 5237–5245.
Loganathan, A., J.E. Linley, I. Rajput, M. Hunter, J.P. Lodge, and G.I. Sandle. 2011. Basolateral potassium (IKCa) channel inhibition prevents increased colonic permeability induced by chemical hypoxia. American Journal of Physiology. Gastrointestinal and Liver Physiology 300 (1): G146–G153.
Kim, Y., G.A. West, G. Ray, S.P. Kessler, A.C. Petrey, C. Fiocchi, C. McDonald, M.S. Longworth, L.E. Nagy, and C.A. de la Motte. 2018. Layilin is critical for mediating hyaluronan 35kDa-induced intestinal epithelial tight junction protein ZO-1 in vitro and in vivo. Matrix Biology 66: 93–109.
Purohit, V., J.C. Bode, C. Bode, D.A. Brenner, M.A. Choudhry, F. Hamilton, Y.J. Kang, A. Keshavarzian, R. Rao, R.B. Sartor, C. Swanson, and J.R. Turner. 2008. Alcohol, intestinal bacterial growth, intestinal permeability to endotoxin, and medical consequences: summary of a symposium. Alcohol. 42 (5): 349–361.
Penissi, A.B., M.I. Rudolph, and R.S. Piezzi. 2003. Role of mast cells in gastrointestinal mucosal defense. Biocell. 27 (2): 163–172.
Nishida, Y., K. Murase, H. Isomoto, H. Furusu, Y. Mizuta, R.H. Riddell, and S. Kohno. 2002. Different distribution of mast cells and macrophages in colonic mucosa of patients with collagenous colitis and inflammatory bowel disease. Hepatogastroenterology. 49 (45): 678–682.
Coelho, A.M., N. Vergnolle, B. Guiard, J. Fioramonti, and L. Bueno. 2002. Proteinases and proteinase-activated receptor 2: a possible role to promote visceral hyperalgesia in rats. Gastroenterology 122 (4): 1035–1047.
McCoy, K.L., S.F. Traynelis, and J.R. Hepler. 2010. PAR1 and PAR2 couple to overlapping and distinct sets of G proteins and linked signaling pathways to differentially regulate cell physiology. Molecular Pharmacology 77 (6): 1005–1015.
Hyun, E., P. Andrade-Gordon, M. Steinhoff, P.L. Beck, and N. Vergnolle. 2010. Contribution of bone marrow-derived cells to the pro-inflammatory effects of protease-activatedreceptor-2 in colitis. Inflammation Research 59 (9): 699–709.
Funding
This research was supported by funding from the National Natural Science Foundation of China (82074214, 81973598,81573760); Zhejiang Provincial Natural Science Foundation of China under Grant No.LY18H030001; the Medicine and Health Science and Technology Plan Projects in Zhejiang province(2017KY413), Traditional Chinese Medicine Science and Technology Plan of Zhejiang Province(2017ZA089, 2016ZB071, 2015ZZ012, 2014ZA030); Medical Health Platform Plan Projects of Zhejiang Province (2015RCA020); Zhejiang Provincial Natural Science Foundation of China (LY16H030010).
Author information
Authors and Affiliations
Contributions
Guanqun Chao wrote the article. Xiaojie Hong did the experiment. Shuo Zhang guided.
Corresponding author
Ethics declarations
Ethics Approval and Consent to Participate
The study has been approved by the ethics committee of Zhejiang Chinese medical university.
Consent for Publication
Yes.
Competing Interests
The authors declare no competing interests.
Additional information
Publisher’s Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
About this article
Cite this article
Chao, G., Hong, X. & Zhang, S. Effects of Mast Cells Induced by NSAIDs Impair Intestinal Epithelial Barrier Function In Vivo and In Vitro. Inflammation 44, 1396–1404 (2021). https://doi.org/10.1007/s10753-021-01424-z
Received:
Revised:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s10753-021-01424-z