Abstract
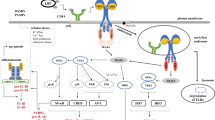
The aim of the study was to provide a theoretical foundation for understanding the relationship between periodontal diseases and systemic diseases by examining the inflammatory effect of Porphyromonas gingivalis lipopolysaccharide (LPS) on monocytes/macrophages isolated from tissues distinct from the oral cavity in normal and hyperlipidemic New Zealand white rabbits. Macrophages were isolated from four separate tissues (mononuclear cells from blood, alveolar macrophages, peritoneal macrophages, and Kupffer cells) from both normal and hyperlipidemic New Zealand white rabbits. Cells were either stimulated for 24 h in vitro with P. gingivalis–LPS or Escherichia coli–LPS, or were pre-treated with IL-10 before P. gingivalis–LPS treatment. RNA was isolated and the expression of SR-A, TLR4, CD14, and MHC-II measured by RT-PCR. For MHC-II, the suppression effects of P. gingivalis–LPS were similar to the effects of E. coli–LPS in all macrophages examined. In general, the magnitude of the effects of P. gingivalis–LPS on gene expression was lower than that of E. coli–LPS, and there were differences in the relative membrane receptors between the two, implying that the two LPSs stimulate different responses. IL-10 increased the expression of the defensive receptor SR-A and decreased the expression of CD14, TLR4, and the antigen-presenting molecule MHC-II in all types of macrophages examined, regardless of hyperlipidemic state. These data are consistent with an anti-inflammatory effect of IL-10. P. gingivalis–LPS is an activator of gene expression in macrophages isolated from tissues distinct from the oral cavity.




Similar content being viewed by others
References
Panteghini, M., R. Bonora, and F. Pagani. 1997. Rapid and specific immunoassay for cardiac troponin I in the diagnosis of myocardial damage. International Journal of Clinical and Laboratory Research 27 (1): 60–64.
Tsukamoto, H., K. Fukudome, S. Takao, N. Tsuneyoshi, and M. Kimoto. 2010. Lipopolysaccharide-binding protein-mediated Toll-like receptor 4 dimerization enables rapid signal transduction against lipopolysaccharide stimulation on membrane-associated CD14-expressing cells. International Immunology 22 (4): 271–280.
Hozumi, H., Y. Adachi, T. Murakami, N.N. Miura, and N. Ohno. 2006. Increment of plasma soluble CD14 level in carrageenan-primed endotoxin shock model mice. Biological and Pharmaceutical Bulletin 29 (5): 1015–1021.
Akira, S., and K. Takeda. 2004. Toll-like receptor signaling. Nature Reviews Immunology 4: 499–511.
Underhill, D.M., and A. Ozinsky. 2002. Toll-like receptors: key mediators of microbe detection. Current Opinion in Immunology 14 (1): 103–110.
Nagai, Y., S. Akashi, M. Nagafuku, M. Ogata, Y. Iwakura, S. Akira, et al. 2002. Essential role of MD-2 in LPS responsiveness and TLR4 distribution. Nature Immunology 3: 667–672.
Cotena, A., S. Gordon, and N. Platt. 2004. The class A macrophage scavenger receptor attenuates CXC chemokine production and the early infiltration of neutrophils in sterile peritonitis. The Journal of Immunology 173 (10): 6427–6432.
Wenzel, J., J.L. Ouderkirk, M. Krendel, and R. Lang. 2015. Class I myosin Myo1e regulates TLR4-triggered macrophage spreading, chemokine release, and antigen presentation via MHC class II. European Journal of Immunology 45 (1): 225–237.
Holt, S.C., L. Kesavalu, S. Walker, and C.A. Genco. 1999. Virulence factors of Porphyromonas gingivalis. Periodontology 2000 (20): 168–238.
Giacona, M.B., P.N. Papapanou, I.B. Lamster, L.L. Rong, V.D. D'Agati, A.M. Schmidt, et al. 2004. Porphyromonas gingivalis induces its uptake by human macrophages and promotes foam cell formation in vitro. FEMS Microbiology Letters 241 (1): 95–101.
Sadeghi, K., A. Berger, M. Langgartner, A.R. Prusa, M. Hayde, K. Herkner, et al. 2007. Immaturity of infection control in preterm and term newborns is associated with impaired Toll-like receptor signaling. The Journal of Infectious Diseases 195 (2): 296–302.
Brodala, N., E.P. Merricks, and D.A. Bellinger. 2005. Porphyromonas gingivalis bacteremia induces coronary and aortic atherosclerosis in normocholesterolemic and hypercholesterolemic pigs. Arteriosclerosis Thrombosis and Vascular Biology 25 (7): 1446–1451.
Zhou, Q., and S. Amar. 2007. Identification of signaling pathways in macrophage exposed to Porphyromonas gingivalis or to its purified cell wall components. Journal of Immunology 179 (11): 7777–7790.
Giacona, M.B., P.N. Papapanou, I.B. Lamster, L.R. Ling, V.D. D’Agati, A.M. Schmidt, et al. 2004. Porphyromonas gingivalis induces its uptake by human macrophages and promotes foam cell formation in vitro. FEMS Microbiology Letters 241 (1): 95–101.
Gibson, F.C., H. Yumoto, Y. Takahashi, H.H. Chou, and C.A. Genco. 2006. Innate immune signaling and Porphyromonas gingivalis-accelerated atherosclerosis. Journal of Dental Research 85 (2): 106–121.
Behrens, E.M. 2008. Macrophage activation syndrome in rheumatic disease: what is the role of the antigen presenting cell? Autoimmunity Reviews 7 (4): 305–308.
Agarwal, S., N.P. Piesco, L.P. Johns, and A.E. Riccelli. 1995. Differential expression of IL-1β,TNF-α,IL-6 and IL-8 in human monocytes in response to lipopolysaccharides from different microbes. Journal of Dental Research 74 (4): 1057–1065.
Bainbridge, B.W., and R.P. Darveau. 2001. Porphyromonas gingivalis lipopolysaccharide: an unusual pattern recognition receptor ligand for the innate host defense system. Acta Odontologica Scandinavica 59 (3): 131–138.
Inaba, H., and A. Amano. 2010. Roles of oral bacteria in cardiovascular diseases from molecular mechanisms to clinical cases: implication of periodontal diseases in development of systemic diseases. Journal of Pharmacological Sciences 113 (2): 103–109.
Rigante, D., G. Emmi, M. Fastiggi, E. Silvestri, and L. Cantarini. 2015. Macrophage activation syndrome in the course of monogenic autoinflammatory disorders. Clinical Rheumatology 34 (8): 1333–1339.
Filho, W.S.E.S., R.C.V. Casarin, E.L.N. Junior, H.M. Passos, A.W. Sallum, and R.B. Gonçalves. 2014. Microbial diversity similarities in periodontal pockets and atheromatous plaques of cardiovascular disease patients. PLoS One 9 (10): e109761.
Valledor, A.F., E. Sanchez-Tillo, L. Arpa, J.M. Park, C. Caelles, J. Lloberas, et al. 2008. Selective roles of MAPKs during the macrophage response to IFN-α. The Journal of Immunology 180 (7): 4523–4529.
Bähr, I.N., P. Tretter, J. Krüger, R.G. Stark, J. Schimkus, T. Unger, et al. 2011. High-dose treatment with telmisartan induces monocytic peroxisome proliferator-activated receptor-γ target genes in patients with the metabolic syndrome. Hypertension 58 (4): 725–732.
Zhou, H., A. Imrich, and L. Kobzik. 2008. Characterization of immortalized marco and sr-ai/ii-deficient murine alveolar macrophage cell lines. Particle & Fibre Toxicology 5 (1): 7.
Takeda, Y., V.N. Bui, K. Iwasaki, T. Kobayashi, H. Ogawa, and K. Imai. 2014. Influence of olive-derived hydroxytyrosol on the toll-like receptor 4-dependent inflammatory response of mouse peritoneal macrophages. Biochemical & Biophysical Research Communications 446 (4): 1225–1230.
Zhang, X., W.P. Yu, L. Gao, K.B. Wei, J.L. Ju, and J.Z. Xu. 2004. Effects of lipopolysaccharides stimulated Kupffer cells on activation of rat hepatic stellate cells. World Journal of Gastroenterology 10 (4): 610–613.
Cazalis, J., C. Bodet, G. Gagnon, and D. Grenier. 2008. Doxycycline reduces lipopolysaccharide-induced inflammatory mediator secretion in macrophage and ex vivo human whole blood models. Journal of Periodontology 79 (9): 1762–1768.
Zhang, D., L. Chen, S. Li, Z. Gu, and J. Yan. 2008. Lipopolysaccharide (LPS) of Porphyromonas gingivalis induces IL-1, TNF-α and IL-6 production by THP-1 cells in a way different from that of Escherichia coli LPS. Innate Immunity 14 (2): 99–107.
Gordon, S., and A. Plüddemann. 2017. Tissue macrophages: heterogeneity and functions. BMC Biology 15 (1): 53.
Agarwal, S., N.P. Piesco, L.P. Johns, and A.E. Riccelli. 1995. Differential expression of IL-1 beta, TNF-alpha, IL-6, and IL-8 in human monocytes in response to lipopolysaccharides from different microbes. Journal of Dental Research 74 (4): 1057–1065.
Wick, M.J., C.V. Harding, S.J. Normark, and J.D. Pfeifer. 1994. Parameters that influence the efficiency of processing antigenic epitopes expressed in Salmonella typhimurium. Infection & Immunity 62 (10): 4542–4548.
Tobian, A.A., N.S. Potter, L. Ramachandra, R.K. Pai, M. Convery, W.H. Boom, et al. 2003. Alternate class I MHC antigen processing is inhibited by Toll-like receptor signaling pathogen-associated molecular patterns: Mycobacterium tuberculosis 19-kDa lipoprotein, CpG DNA, and lipopolysaccharide. Journal of Immunology 171 (3): 1413–1422.
Scannapieco, F.A., and A.J.M. Mylotte. 1996. Relationships between periodontal disease and bacterial pneumonia. Journal of Periodontology 67 (10 Suppl): 1114–1122.
Scannapieco, F.A., and M.P. Rethman. 2003. The relationship between periodontal diseases and respiratory diseases. Dentistry Today 22 (8): 79–83.
Muthu, J., S. Muthanandam, and J. Mahendra. 2016. Mouth the mirror of lungs: where does the connection lie? Frontiers of Medicine 10 (4): 405–409.
Brass, D.M., J.W. Hollingsworth, E. Mcelvania-Tekippe, S. Garantziotis, I. Hossain, and D.A. Schwartz. 2007. CD14 is an essential mediator of LPS-induced airway disease. American Journal of Physiology Lung Cellular & Molecular Physiology 293 (1): 77–83.
Dagvadorj, J., K. Shimada, S. Chen, H.D. Jones, G. Tumurkhuu, W. Zhang, et al. 2015. Lipopolysaccharide induces alveolar macrophage necrosis via CD14 and the P2x7 receptor leading to interleukin-1α release. Immunity 42 (4): 640–653.
Maris, N.A., M.C. Dessing, A.F. de Vos, P. Bresser, V.D.Z. Js, H.M. Jansen, et al. 2006. Toll-like receptor mRNA levels in alveolar macrophages after inhalation of endotoxin. European Respiratory Journal 28 (3): 622–626.
Saito, T., T. Yamamoto, T. Kazawa, H. Gejyo, and M. Naito. 2005. Expression of toll-like receptor 2 and 4 in lipopolysaccharide-induced lung injury in mouse. Cell & Tissue Research 321 (1): 75–88.
Ganesan, S., A.N. Faris, A.T. Comstock, J. Sonstein, J.L. Curtis, and U.S. Sajjan. 2012. Elastase/LPS-exposed mice exhibit impaired innate immune responses to bacterial challenge: role of scavenger receptor A. American Journal of Pathology 180 (1): 61–72.
Yamamoto, T., Y. Ebe, G. Hasegawa, M. Kataoka, S. Yamamoto, and M. Naito. 1999. Expression of scavenger receptor class A and CD14 in lipopolysaccharide-induced lung injury. Pathology International 49 (11): 983–992.
Czerkies, M., K. Borzęcka, M.I. Zdioruk, A. Płóciennikowska, A. Sobota, and K. Kwiatkowska. 2013. An interplay between scavenger receptor A and CD14 during activation of J774 cells by high concentrations of LPS. Immunobiology 218 (10): 1217–1226.
Fitzgerald, M.L., K.J. Moore, M.W. Freeman, and G.L. Reed. 2000. Lipopolysaccharide induces scavenger receptor A expression in mouse macrophages: a divergent response relative to human THP-1 monocyte/macrophages. Journal of Immunology 164 (5): 2692–2700.
Tomofuji, T., D. Ekuni, R. Yamanaka, H. Kusano, T. Azuma, T. Sanbe, et al. 2007. Chronic administration of lipopolysaccharide and proteases induces periodontal inflammation and hepatic steatosis in rats. Journal of Periodontology 78 (10): 1999–2006.
Tomofuji, T., D. Ekuni, T. Sanbe, T. Azuma, N. Tamaki, K. Irie, et al. 2009. Effects of improvement in periodontal inflammation by toothbrushing on serum lipopolysaccharide concentration and liver injury in rats. Acta Odontologica Scandinavica 67 (4): 200–205.
Yamamoto, T., T. Tomofuji, N. Tamaki, D. Ekuni, T. Azuma, and T. Sanbe. 2010. Effects of topical application of lipopolysaccharide and proteases on hepatic injury induced by high-cholesterol diet in rats. Journal of Periodontal Research 45 (1): 129–135.
Peng, Y., Z.J. Liu, J.P. Gong, H.Z. Liu, L. Gan, and S.B. Li. 2005. Expression of CD14 and Toll-like receptor 4 on Kupffer cells and its role in ischemia-reperfusion injury on rat liver graft. Zhonghua Wai Ke Za Zhi 43 (5): 274–276.
Choda, Y., Y. Morimoto, H. Miyaso, S. Shinoura, S. Saito, T. Yagi, et al. 2004. Failure of the gut barrier system enhances liver injury in rats: protection of hepatocytes by gut-derived hepatocyte growth factor. European Journal of Gastroenterology & Hepatology 6 (10): 1017–1025.
Imajo, K., K. Fujita, M. Yoneda, Y. Nozaki, Y. Ogawa, Y. Shinohara, et al. 2012. Hyperresponsivity to low-dose endotoxin during progression to nonalcoholic steatohepatitis is regulated by leptin-mediated signaling. Cell Metabolism 16 (1): 44–54.
Ono, K., C. Nishitani, H. Mitsuzawa, T. Shimizu, H. Sano, H. Suzuki, et al. 2006. Mannose-binding lectin augments the uptake of lipid A, Staphylococcus aureus, and Escherichia coli by Kupffer cells through increased cell surface expression of scavenger receptor A. Journal of Immunology 177 (8): 5517–5523.
Van, O.M., E.S. van Amersfoort, T.J. van Berkel, and J. Kuiper. 2001. Scavenger receptor-like receptors for the binding of lipopolysaccharide and lipoteichoic acid to liver endothelial and Kupffer cells. Journal of Endotoxin Research 7 (5): 381–384.
Jiang, Q., S. Akashi, K. Miyake, and H.R. Petty. 2000. Lipopolysaccharide induces physical proximity between CD14 and toll-like receptor 4 (TLR4) prior to nuclear translocation of NF-kappa B. Journal of Immunology 165 (7): 3541–3544.
Mirlashari, M.R., and T. Lyberg. 2003. Expression and involvement of toll-like receptors (TLR)2, TLR4, and CD14 in monocyte TNF-alpha production induced by lipopolysaccharides from Neisseria meningitidis. Medical Science Monitor International Medical Journal of Experimental & Clinical Research 9 (8): BR316–BR324.
Zhou, J., G. Tai, H. Liu, J. Ge, Y. Feng, F. Chen, et al. 2009. Activin A down-regulates the phagocytosis of lipopolysaccharide-activated mouse peritoneal macrophages in vitro, and in vivo. Cellular Immunology 255 (1–2): 69–75.
Acknowledgements
The authors gratefully acknowledge Li and Zheng Heping and their staff (Comparative Medicine Department, Fuzhou General Hospital of Nanjing Military Region of PLA) for the outstanding care given to the animals used in this study. We also acknowledge the staff of the Oral Medical Research Center of Fujian Medical University for their enthusiastic support and help in performing the experiments. We would like to thank Editage (www.editage.com) for English language editing and Publication Support.
Funding
This study was funded by the National Natural Science Foundation of China [grant numbers 81371152, 30973326] and Natural Science Foundation of Fujian Province, China [grant number 2017J01809]. The funding agency had no role in the study design, collection, analysis, or interpretation of data, the writing of the report, or the decision to submit the article for publication.
Author information
Authors and Affiliations
Corresponding authors
Ethics declarations
Conflict of Interest
The authors declare that they have no conflicts of interest.
Ethical Approval
This article does not contain any studies with human or animal subjects performed by any of the authors.
Informed Consent
Not applicable.
Rights and permissions
About this article
Cite this article
Wu, C., Liu, C., Luo, K. et al. Changes in Expression of the Membrane Receptors CD14, MHC-II, SR-A, and TLR4 in Tissue-Specific Monocytes/Macrophages Following Porphyromonas gingivalis–LPS Stimulation. Inflammation 41, 418–431 (2018). https://doi.org/10.1007/s10753-017-0698-y
Published:
Issue Date:
DOI: https://doi.org/10.1007/s10753-017-0698-y