Abstract
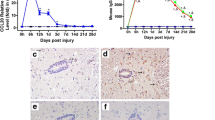
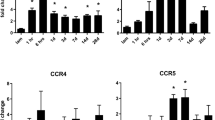
Spinal cord injury (SCI) is considered to be primarily associated with loss of motor function and leads to activate diverse cellular mechanisms in the central nervous system to attempt to repair the damaged spinal cord tissue. Chemokine Receptor 5 (CCR5), a major co-receptor for macrophage-tropic human immunodeficiency viruses, is expressed on the surface of monocytes/macrophages, dendritic cells, activated T cells, and NK cells. Recent papers have indicated the important role of CCR5 in SCI, but the mechanism is still unknown. In our current study, CCR5 blockade displayed increased myelin sparring and enhanced SC repair process. The number of CD4+ T cells, CD8+ T cells, Ly6G+ neutrophils and CD11b+ macrophages were all significantly lower in the anti-CCR5 group than that in the control group after SCI. The IL-4 and IL-13 levels in anti-CCR5 group were markedly higher than that in control group after SCI. Correspondingly, the anti-CCR5-treated group showed increased numbers of Arg1- or CD206-expressing macrophages compared with the control IgG group. Furthermore, CCR5 blockade promoted PPARγ activation, and the increased numbers of M2 macrophages induced by CCR5 blockade were both reversed with additional PPARγ antagonist treatment. In conclusion, our present work provides evidence to support the concept that CCR5 blockade promotes M2 macrophage activation and improves locomotor recovery after SCI in mice.





Similar content being viewed by others
References
Scott, J.M., D.E. Warburton, D. Williams, S. Whelan, and A. Krassioukov. 2011. Challenges, concerns and common problems: physiological consequences of spinal cord injury and microgravity. Spinal Cord 49: 4–16.
Thuret, S., L.D. Moon, and F.H. Gage. 2006. Therapeutic interventions after spinal cord injury. Nature Review Neuroscience 7: 628–643.
Nakahara, S., K. Yone, T. Sakou, et al. 1999. Induction of apoptosis signal regulating kinase 1 (ASK1) after spinal cord injury in rats: possible involvement of ASK1-JNK and -p38 pathways in neuronal apoptosis. Journal of Neuropathology and Experimental Neurology 58: 442–450.
Liu, S., G.L. Ruenes, and R.P. Yezierski. 1997. NMDA and non-NMDA receptor antagonists protect against excitotoxic injury in the rat spinal cord. Brain Research 756: 160–167.
Kato, H., G.K. Kanellopoulos, S. Matsuo, et al. 1997. Neuronal apoptosis and necrosis following spinal cord ischemia in the rat. Experimental Neurology 148: 464–474.
Crowe, M.J., J.C. Bresnahan, S.L. Shuman, J.N. Masters, and M.S. Beattie. 1997. Apoptosis and delayed degeneration after spinal cord injury in rats and monkeys. Nature Medicine 3: 73–76.
Taoka, Y., K. Okajima, M. Uchiba, et al. 1997. Role of neutrophils in spinal cord injury in the rat. Neuroscience 79: 1177–1182.
Popovich, P.G., Z. Guan, V. McGaughy, L. Fisher, W.F. Hickey, and D.M. Basso. 2002. The neuropathological and behavioral consequences of intraspinal microglial/macrophage activation. Journal of Neuropathology and Experimental Neurology 61: 623–633.
Pineau, I., and S. Lacroix. 2007. Proinflammatory cytokine synthesis in the injured mouse spinal cord: multiphasic expression pattern and identification of the cell types involved. Journal of Comparative Neurology 500: 267–285.
Carlson, S.L., M.E. Parrish, J.E. Springer, K. Doty, and L. Dossett. 1998. Acute inflammatory response in spinal cord following impact injury. Experimental Neurology 151: 77–88.
Blight, A.R. 2002. Miracles and molecules—progress in spinal cord repair. Nature Neuroscience 5(Suppl): 1051–1054.
Hausmann, O.N. 2003. Post-traumatic inflammation following spinal cord injury. Spinal Cord 41: 369–378.
Springer, T.A. 1995. Traffic signals on endothelium for lymphocyte recirculation and leukocyte emigration. Annual Review of Physiology 57: 827–872.
Flach, R., N. Speidel, S. Flohe, et al. 1998. Analysis of intragraft cytokine expression during early reperfusion after liver transplantation using semi-quantitative RT-PCR. Cytokine 10: 445–451.
Gu, L., S. Tseng, R.M. Horner, C. Tam, M. Loda, and B.J. Rollins. 2000. Control of TH2 polarization by the chemokine monocyte chemoattractant protein-1. Nature 404: 407–411.
Murphy, P.M., M. Baggiolini, I.F. Charo, et al. 2000. International Union of Pharmacology. XXII. Nomenclature for chemokine receptors. Pharmacological Reviews 52: 145–176.
Luster, A.D. 1998. Chemokines—chemotactic cytokines that mediate inflammation. New England Journal of Medicine 338: 436–445.
Kiguchi, N., Y. Kobayashi, T. Maeda, F. Saika, and S. Kishioka. 2010. CC-chemokine MIP-1alpha in the spinal cord contributes to nerve injury-induced neuropathic pain. Neuroscience Letters 484: 17–21.
Ma, M., T. Wei, L. Boring, I.F. Charo, R.M. Ransohoff, and L.B. Jakeman. 2002. Monocyte recruitment and myelin removal are delayed following spinal cord injury in mice with CCR2 chemokine receptor deletion. Journal of Neuroscience Research 68: 691–702.
Scheff, S.W., A.G. Rabchevsky, I. Fugaccia, J.A. Main, and J.J. Lumpp. 2003. Experimental modeling of spinal cord injury: characterization of a force-defined injury device. Journal of Neurotrauma 20: 179–193.
Chawla, A., Y. Barak, L. Nagy, D. Liao, P. Tontonoz, and R.M. Evans. 2001. PPAR-gamma dependent and independent effects on macrophage-gene expression in lipid metabolism and inflammation. Nature Medicine 7: 48–52.
Basso, D.M., L.C. Fisher, A.J. Anderson, L.B. Jakeman, D.M. McTigue, and P.G. Popovich. 2006. Basso Mouse Scale for locomotion detects differences in recovery after spinal cord injury in five common mouse strains. Journal of Neurotrauma 23: 635–659.
Chen, K.B., K. Uchida, H. Nakajima, et al. 2011. Tumor necrosis factor-alpha antagonist reduces apoptosis of neurons and oligodendroglia in rat spinal cord injury. Spine (Phila Pa 1976) 36: 1350–1358.
Uchida, K., H. Baba, Y. Maezawa, and C. Kubota. 2002. Progressive changes in neurofilament proteins and growth-associated protein-43 immunoreactivities at the site of cervical spinal cord compression in spinal hyperostotic mice. Spine (Phila Pa 1976) 27: 480–486.
Saiwai, H., Y. Ohkawa, H. Yamada, et al. 2010. The LTB4-BLT1 axis mediates neutrophil infiltration and secondary injury in experimental spinal cord injury. American Journal of Pathology 176: 2352–2366.
Stirling, D.P., and V.W. Yong. 2008. Dynamics of the inflammatory response after murine spinal cord injury revealed by flow cytometry. Journal of Neuroscience Research 86: 1944–1958.
Goerdt, S., and C.E. Orfanos. 1999. Other functions, other genes: alternative activation of antigen-presenting cells. Immunity 10: 137–142.
Odegaard, J.I., R.R. Ricardo-Gonzalez, M.H. Goforth, et al. 2007. Macrophage-specific PPARgamma controls alternative activation and improves insulin resistance. Nature 447: 1116–1120.
Suzuki, Y., J. Claflin, X. Wang, A. Lengi, and T. Kikuchi. 2005. Microglia and macrophages as innate producers of interferon-gamma in the brain following infection with Toxoplasma gondii. International Journal of Parasitology 35: 83–90.
Makela, J., R. Koivuniemi, L. Korhonen, and D. Lindholm. 2010. Interferon-gamma produced by microglia and the neuropeptide PACAP have opposite effects on the viability of neural progenitor cells. PloS One 5: e11091.
Pouliot, P., V. Turmel, E. Gelinas, M. Laviolette, and E.Y. Bissonnette. 2005. Interleukin-4 production by human alveolar macrophages. Clinical and Experimental Allergy 35: 804–810.
Shin, W.H., D.Y. Lee, K.W. Park, et al. 2004. Microglia expressing interleukin-13 undergo cell death and contribute to neuronal survival in vivo. Glia 46: 142–152.
Popovich, P.G., P. Wei, and B.T. Stokes. 1997. Cellular inflammatory response after spinal cord injury in Sprague–Dawley and Lewis rats. Journal of Comparative Neurology 377: 443–464.
Stout, R.D., C. Jiang, B. Matta, I. Tietzel, S.K. Watkins, and J. Suttles. 2005. Macrophages sequentially change their functional phenotype in response to changes in microenvironmental influences. Journal of Immunology 175: 342–349.
Martinez, F.O., L. Helming, and S. Gordon. 2009. Alternative activation of macrophages: an immunologic functional perspective. Annual Review of Immunology 27: 451–483.
Bouhlel, M.A., B. Derudas, E. Rigamonti, et al. 2007. PPARgamma activation primes human monocytes into alternative M2 macrophages with anti-inflammatory properties. Cell Metabolism 6: 137–143.
Kigerl, K.A., J.C. Gensel, D.P. Ankeny, J.K. Alexander, D.J. Donnelly, and P.G. Popovich. 2009. Identification of two distinct macrophage subsets with divergent effects causing either neurotoxicity or regeneration in the injured mouse spinal cord. Journal of Neuroscience 29: 13435–13444.
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
About this article
Cite this article
Li, F., Cheng, B., Cheng, J. et al. CCR5 Blockade Promotes M2 Macrophage Activation and Improves Locomotor Recovery After Spinal Cord Injury in Mice. Inflammation 38, 126–133 (2015). https://doi.org/10.1007/s10753-014-0014-z
Published:
Issue Date:
DOI: https://doi.org/10.1007/s10753-014-0014-z