Abstract
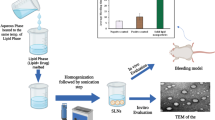
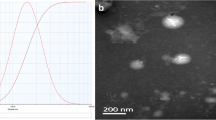
The sanguinarine (SG) was studied for its pharmacokinetic and anti-inflammatory activities with prepared solid lipid nanoparticles (SLNs). The sanguinarine solid lipid nanoparticles (SG-SLNs) were prepared by film-ultrasonic dispersion method and the entrapment efficiency of SG was higher at 75.6 %. The drug release profile of SG was examined in pH 7.4 PBS and 85 % of the SG loaded in SLNs was gradually released during 24 h. We used mice endotoxin shock model which was induced by lipopolysaccharide (1 mg/kg) to examine the anti-inflammatory function of SG-SLNs. Healthy Kunming mice were administered orally with saline, SG (10 mg/kg), and SG-SLNs (10 mg/kg), respectively, at 12 and 1 h before lipopolysaccharide (LPS) injection. Mice were sacrificed at 1 and 6 h, respectively, and blood was collect through the venous sinus to access inflammatory mediators. Pharmacokinetic studies proved that the AUC0→24 and C max of SG-SLNs were significantly increased compared that of SG. SG-SLNs revealed significant anti-inflammatory effects through inhibition of LPS-induced tumor necrosis factor-alpha level, interleukin 6 level, and nitric oxide production in serum. Therefore, it can be concluded that SG-SLNs led to a better oral bioavailability.




Similar content being viewed by others
References
Niu, X., T. Fan, W. Li, W. Xing, and H. Huang. 2012. The anti-inflammatory effects of sanguinarine and its modulation of inflammatory mediators from peritoneal macrophages. Eur J Pharmacol 689: 262–269.
Mazzanti, G., A. DiSotto, A. Franchitto, C.L. Mammola, P. Mariani, S. Mastrangelo, and A. Vitalone. 2009. Chelidonium majus is not hepatotoxic in Wistar rats, in a 4 weeks feeding experiment. J Ethnopharmacol 126: 518–524.
Mitscher, L.A., S. Drake, S.R. Gollapudi, and S.K. Okwute. 1987. A modern look at folkloric use of anti-infective agents. Journal of natural products 50: 1025–1040.
Walterová, D., J. Ulrichová, I. Valka, J. Vicar, C. Vavreckova, E. Taborska, and V. Simanek. 1994. Benzo[c]phenanthridine alkaloids sanguinarine and chelerythrine: biological activities and dental care applications. Acta universitatis palackianae olomucensis Facultatis Medicae 139: 7–16.
Agarwal, S., M.A. Reynolds, S. Pou, D.E. Peterson, J.A. Charon, and J.B. Suzuki. 1991. The effect of sanguinarine on human peripheral blood neutrophil viability and functions. Oral microbiology and immunology 6: 51–61.
Mehnert, W., and K. Mäder. 2001. Solid lipid nanoparticles: production, characterization and applications. Advanced drug delivery reviews 47: 165–196.
Müller, R.H., K. Mäder, and S. Gohla. 2000. Solid lipid nanoparticles (SLN) for controlled drug delivery—a review of the state of the art. European journal of pharmaceutics and biopharmaceutics 50: 161–177.
Zur Mühlen, A., C. Schwarz, and W. Mehnert. 1998. Solid lipid nanoparticles (SLN) for controlled drug delivery—drug release and release mechanism. European journal of pharmaceutics and biopharmaceutics 45: 149–155.
Joshi, M.D., and R.H. Müller. 2009. Lipid nanoparticles for parenteral delivery of actives. European journal of pharmaceutics and biopharmaceutics 71: 161–172.
Shahgaldian, P., E. Da Silva, A.W. Coleman, B. Rather, and M.J. Zaworotko. 2003. Para-acyl-calix-arene based solid lipid nanoparticles (SLNs): a detailed study of preparation and stability parameters. Int J Pharm 253: 23–38.
Song, X., Y. Zhao, S. Hou, F. Xu, R. Zhao, J. He, and Q. Chen. 2008. Dual agents loaded PLGA nanoparticles: systematic study of particle size and drug entrapment efficiency. European journal of pharmaceutics and biopharmaceutics 69: 445–453.
Zhang, X., S. Lu, J. Han, S. Sun, L. Wang, and Y. Li. 2011. Preparation, characterization and in vivo distribution of solid lipid nanoparticles loaded with syringopicroside. Die Pharmazie-An International Journal of Pharmaceutical Sciences 66: 404–407.
Gao, S., G. Fan, Z. Hong, X. Yin, S. Yang, and Y. Wu. 2006. HPLC determination of polydatin in rat biological matrices: application to pharmacokinetic studies. Journal of pharmaceutical and biomedical analysis 41: 240–245.
Riddick, T. 1968. Control of colloid stability through zeta potential: with a closing chapter on its relationship to cardiovascular disease. Wynnewood, PA: Zeta-Meter. Inc.
Suresh, G., K. Manjunath, V. Venkateswarlu, and V. Satyanarayana. 2007. Preparation, characterization, and in vitro and in vivo evaluation of lovastatin solid lipid nanoparticles. AAPS PharmSciTech 8: 162–170.
Wissing, S., O. Kayser, and R. Müller. 2004. Solid lipid nanoparticles for parenteral drug delivery. Advanced drug delivery reviews 56: 1257–1272.
Li, W., W. Xing, X. Niu, P. Zhou, and T. Fan. 2013. The pharmacokinetics of chelerythrine solution and chelerythrine liposomes after oral administration to rats. Planta medica 79: 654–660.
Heinzel, F.P., R.M. Rerko, P. Ling, J. Hakimi, and D.S. Schoenhaut. 1994. Interleukin 12 is produced in vivo during endotoxemia and stimulates synthesis of gamma interferon. Infection and immunity 62: 4244–4249.
Suzuki, K., K. Tateda, T. Matsumoto, F. Gondaira, S. Tsujimoto, and K. Yamaguchi. 2000. Effects of interaction between Escherichia coli verotoxin and lipopolysaccharide on cytokine induction and lethality in mice. Journal of medical microbiology 49: 905–910.
Leone, A., S. Moncada, P. Vallance, A. Calver, and J. Collier. 1992. Accumulation of an endogenous inhibitor of nitric oxide synthesis in chronic renal failure. The Lancet 339: 572–575.
Nkeh, B.C.-A., D. Njamen, J. Wandji, Z.T. Fomum, A. Dongmo, T.B. Nguelefack, and A. Kamanyi. 2003. Anti-inflammatory and analgesic effects of drypemolundein A, a sesquiterpene lactone from Drypetes molunduana. Pharmaceutical biology 41: 26–30.
Stoclet, J.C., B. Muller, R. Andriantsitohaina, and A. Kleschyov. 1998. Overproduction of nitric oxide in pathophysiology of blood vessels. Biochemistry. Biokhimiya 63: 826.
Li, W., T. Fan, Y. Zhang, X. Niu, and W. Xing. 2012. Effect of Chelerythrine against endotoxic shock in mice and its modulation of inflammatory mediators in peritoneal macrophages through the modulation of mitogen-activated protein kinase (MAPK) pathway. Inflammation 35: 1814–1824.
Acknowledgments
This work was supported by a research grant from Xi’an Jiaotong University.
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
About this article
Cite this article
Li, W., Li, H., Yao, H. et al. Pharmacokinetic and Anti-inflammatory Effects of Sanguinarine Solid Lipid Nanoparticles. Inflammation 37, 632–638 (2014). https://doi.org/10.1007/s10753-013-9779-8
Published:
Issue Date:
DOI: https://doi.org/10.1007/s10753-013-9779-8