Abstract
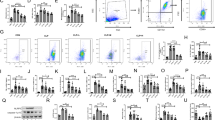
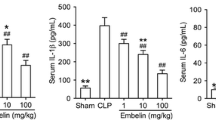
Heparin, a potent blood anticoagulant, is known to possess anti-inflammatory activity. In this work, we investigated whether heparin can ameliorate acute lung injury and lethal response in lipopolysaccharide (LPS)-induced mouse model of sepsis. We found that heparin effectively rescued lethality, improved lung pathological changes, inhibited myeloperoxidase (MPO) activity, and reduced malondialdehyde (MDA) level, lung wet/dry weight ratio and Evans blue values in LPS-induced septic mice. In addition, heparin also inhibited the release of tumor necrosis factor (TNF)-α, interleukin-6 (IL-6) and IL-1β in serum and decreased the expression of p-p38, nuclear factor κB (NF-κB) and p-c-SRC kinase in lungs of septic mice. Our findings suggest that heparin is capable of suppressing the lethal response and acute lung injury associated with sepsis, and support the notion that heparin may be a potential therapeutic agent for the conditions associated with septic shock.





Similar content being viewed by others
References
Russell, J.A. 2006. Management of sepsis. The New England Journal of Medicine 355(16): 1699–1713. doi:10.1056/NEJMra043632.
Fry, D.E. 2012. Sepsis, systemic inflammatory response, and multiple organ dysfunction: The mystery continues. The American Surgeon 78(1): 1–8.
Dombrovskiy, V.Y., A.A. Martin, J. Sunderram, and H.L. Paz. 2007. Rapid increase in hospitalization and mortality rates for severe sepsis in the United States: A trend analysis from 1993 to 2003. Critical Care Medicine 35(5): 1244–1250. doi:10.1097/01.CCM.0000261890.41311.E9.
Netea, M.G., J.W. van der Meer, M. van Deuren, and B.J. Kullberg. 2003. Proinflammatory cytokines and sepsis syndrome: Not enough, or too much of a good thing? Trends in Immunology 24(5): 254–258.
Abraham, E., A. Carmody, R. Shenkar, and J. Arcaroli. 2000. Neutrophils as early immunologic effectors in hemorrhage- or endotoxemia-induced acute lung injury. American Journal of Physiology. Lung Cellular and Molecular Physiology 279(6): L1137–L1145.
Silva, E., J. Arcaroli, Q. He, D. Svetkauskaite, C. Coldren, J.A. Nick, K. Poch, J.S. Park, A. Banerjee, and E. Abraham. 2007. HMGB1 and LPS induce distinct patterns of gene expression and activation in neutrophils from patients with sepsis-induced acute lung injury. Intensive Care Medicine 33(10): 1829–1839. doi:10.1007/s00134-007-0748-2.
Lever, R., and C.P. Page. 2002. Novel drug development opportunities for heparin. Nature Reviews. Drug Discovery 1(2): 140–148. doi:10.1038/nrd724.
Hirsh, J., S.S. Anand, J.L. Halperin, and V. Fuster. 2001. Guide to anticoagulant therapy: Heparin: A statement for healthcare professionals from the American Heart Association. Circulation 103(24): 2994–3018.
Baglin, T., T.W. Barrowcliffe, A. Cohen, and M. Greaves. 2006. Guidelines on the use and monitoring of heparin. British Journal of Haematology 133(1): 19–34. doi:10.1111/j.1365-2141.2005.05953.x.
Young, E. 2008. The anti-inflammatory effects of heparin and related compounds. Thrombosis Research 122(6): 743–752. doi:10.1016/j.thromres.2006.10.026.
Wang, M., J. He, B. Mei, X. Ma, and Z. Huo. 2008. Therapeutic effects and anti-inflammatory mechanisms of heparin on acute lung injury in rabbits. Academic Emergency Medicine 15(7): 656–663.
Mu, E., R. Ding, X. An, X. Li, S. Chen, and X. Ma. 2012. Heparin attenuates lipopolysaccharide-induced acute lung injury by inhibiting nitric oxide synthase and TGF-beta/Smad signaling pathway. Thrombosis Research 129(4): 479–485. doi:10.1016/j.thromres.2011.10.003.
Weng, T.I., H.Y. Wu, C.W. Kuo, and S.H. Liu. 2011. Honokiol rescues sepsis-associated acute lung injury and lethality via the inhibition of oxidative stress and inflammation. Intensive Care Medicine 37(3): 533–541. doi:10.1007/s00134-010-2104-1.
Parikh, S.M., T. Mammoto, A. Schultz, H.T. Yuan, D. Christiani, S.A. Karumanchi, and V.P. Sukhatme. 2006. Excess circulating angiopoietin-2 may contribute to pulmonary vascular leak in sepsis in humans. PLoS Medicine 3(3): e46. doi:10.1371/journal.pmed.0030046.
Cannon, J.G., R.G. Tompkins, J.A. Gelfand, H.R. Michie, G.G. Stanford, J.W. van der Meer, S. Endres, G. Lonnemann, J. Corsetti, B. Chernow, et al. 1990. Circulating interleukin-1 and tumor necrosis factor in septic shock and experimental endotoxin fever. The Journal of Infectious Diseases 161(1): 79–84.
Minamino, T., and I. Komuro. 2006. Regeneration of the endothelium as a novel therapeutic strategy for acute lung injury. The Journal of Clinical Investigation 116(9): 2316–2319. doi:10.1172/JCI29637.
Ogawa, T., S. Shimizu, I. Tojima, H. Kouzaki, and T. Shimizu. 2011. Heparin inhibits mucus hypersecretion in airway epithelial cells. American Journal of Rhinology & Allergy 25(2): 69–74. doi:10.2500/ajra.2011.25.3562.
Blackwell, T.S., T.R. Blackwell, E.P. Holden, B.W. Christman, and J.W. Christman. 1996. In vivo antioxidant treatment suppresses nuclear factor-kappa B activation and neutrophilic lung inflammation. The Journal of Immunology 157(4): 1630–1637.
Liu, S.F., X. Ye, and A.B. Malik. 1999. Inhibition of NF-kappaB activation by pyrrolidine dithiocarbamate prevents In vivo expression of proinflammatory genes. Circulation 100(12): 1330–1337.
Lee, H.S., H.J. Kim, C.S. Moon, Y.H. Chong, and J.L. Kang. 2004. Inhibition of c-Jun NH2-terminal kinase or extracellular signal-regulated kinase improves lung injury. Respiratory Research 5: 23. doi:10.1186/1465-9921-5-23.
Abu-Amer, Y., F.P. Ross, K.P. McHugh, A. Livolsi, J.F. Peyron, and S.L. Teitelbaum. 1998. Tumor necrosis factor-alpha activation of nuclear transcription factor-kappaB in marrow macrophages is mediated by c-Src tyrosine phosphorylation of Ikappa Balpha. The Journal of Biological Chemistry 273(45): 29417–29423.
Fan, C., Q. Li, D. Ross, and J.F. Engelhardt. 2003. Tyrosine phosphorylation of I kappa B alpha activates NF kappa B through a redox-regulated and c-Src-dependent mechanism following hypoxia/reoxygenation. The Journal of Biological Chemistry 278(3): 2072–2080. doi:10.1074/jbc.M206718200M206718200.
Kang, J.L., H.J. Jung, K. Lee, and H.R. Kim. 2006. Src tyrosine kinases mediate crystalline silica-induced NF-kappaB activation through tyrosine phosphorylation of IkappaB-alpha and p65 NF-kappaB in RAW 264.7 macrophages. Toxicological Sciences 90(2): 470–477. doi:10.1093/toxsci/kfj096.
Kang, J.L., H.W. Lee, H.J. Kim, H.S. Lee, V. Castranova, C.M. Lim, and Y. Koh. 2005. Inhibition of SRC tyrosine kinases suppresses activation of nuclear factor-kappaB, and serine and tyrosine phosphorylation of IkappaB-alpha in lipopolysaccharide-stimulated raw 264.7 macrophages. Journal of Toxicology and Environmental Health. Part A 68(19): 1643–1662. doi:10.1080/15287390500192114.
Lee, H.S., C. Moon, H.W. Lee, E.M. Park, M.S. Cho, and J.L. Kang. 2007. Src tyrosine kinases mediate activations of NF-kappaB and integrin signal during lipopolysaccharide-induced acute lung injury. The Journal of Immunology 179(10): 7001–7011.
Kim, H.J., H.S. Lee, Y.H. Chong, and J.L. Kang. 2006. p38 Mitogen-activated protein kinase up-regulates LPS-induced NF-kappaB activation in the development of lung injury and RAW 264.7 macrophages. Toxicology 225(1): 36–47. doi:10.1016/j.tox.2006.04.053.
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
About this article
Cite this article
Zhao, D., Ding, R., Mao, Y. et al. Heparin Rescues Sepsis-Associated Acute Lung Injury and Lethality Through the Suppression of Inflammatory Responses. Inflammation 35, 1825–1832 (2012). https://doi.org/10.1007/s10753-012-9503-0
Published:
Issue Date:
DOI: https://doi.org/10.1007/s10753-012-9503-0