Abstract
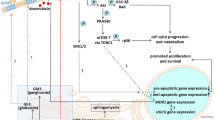
Functions of glycosphingolipids on the eukaryotic cell membranes during the onset of oncogenic processes and cell death are not well understood. Inhibitors of glycosphingolipid biosynthesis were recently found to trigger apoptosis in many carcinoma including breast cancer SKBR-3, MCF-7, and MDA-468 cells through either intrinsic or extrinsic apoptotic pathways as we previously reported. These anti-cancer inhibitors could increase ceramide concentration by blocking functions of glycolipid glycosyltransferases (GLTs). In this study, using a novel fluorescent dye (ASK-0) revealed the damage of cell organelle membranes by an inhibitor of glucosylceramide biosynthesis (L-PPMP). A highly drug- and cell-dependent regulation of MAPKs was also found by cis-platin and L-PPMP when inducing apoptosis in SKBR-3, MCF-7, and MDA-468 cells. A dose and time-dependent regulation of GLTs were investigated by enzymatic assay and DNA microarray analyses. These GLTs are involved in biosynthesis of LeX and sialosyl-LeX (neolactosyl-ceramide series) such as GalT-4 (UDP-Gal: LcOse3cer β−galactosyltransferase, GalT-5 (UDP-Gal: nLcOse4Cer α1, 3galactosyltransferase, FucT-3 (GDP-Fucose: LM1 α1, 4fucosyltransferase). A similar effect was observed with the GLTs involved in the biosyntheses of Gg-series gangliosides, such as SAT-4 (CMP-NeuAc: GgOse4Cer α2, 3sialyltransferase, and SAT-2 (CMP-NeuAc: GM3 α2, 8sialyltransferase). The glycol-related gene DNA-microarrays also suggested the transcriptional regulation of several GLTs involved in the biosynthesis of neolactosylceramide containing cell-surface antigens in these apoptotic breast carcinoma cells. In the early apoptotic stages (2 to 6 h after L-PPMP treatment) in addition to GlcT-1 gene, several genes (βGalTs and βGlcNAcTs) in the SA-Lea pathway were stimulated.












Similar content being viewed by others
Abbreviations
- GSLs:
-
Glycosphingolipids
- GLTs:
-
glycolipid glycosyltransferases
- GalT:
-
galactosyltransferases
- SAT:
-
sialyltransferases
- FucT:
-
fucosyltransferases
- GlcT:
-
glycosyltransferase
- l-PPMP:
-
l-threo-1-phenyl-2-palmitoylamino-3-morpholino-1-propanol
- d-PDMP:
-
d-threo-1-phenyl-2-decanoylamino-3-morpholino-1-propanol
- SA-LeX :
-
sialyl-fucosyl-neolactotetraosyl-ceramide
- cis-Platin:
-
cis-diamino-dichloro platinum
References
Basu, M., De, T., Das, K.K., Kyle, J.W., Chon, H.C., Schaeper, R.J., Basu, S.: Glycosyltransferases involved in glycolipid biosynthesis. In: Ginsburg, V. (ed.) Methods in Enzymology, pp. 575–607. Academic, New York (1987)
Basu, M., Basu, S.: Enzymatic synthesis of a tetraglycosylceramide by a galactosyltransferase from rabbit bone marrow. J. Biol. Chem. 247(5), 1489–1495 (1972)
Basu, M., Basu, S.: Enzymatic synthesis of a blood group B-related pentaglycosylceramide by an alpha-galactosyltransferase from rabbit bone marrow. J. Biol. Chem. 248(5), 1700–1706 (1973)
Basu, M., Hawes, J.W., Li, Z., Ghosh, S., Khan, F.A., Zhang, B.J., Basu, S.: Biosynthesis in vitro of SA-Lex and SA-diLex by alpha 1-3 fucosyltransferases from colon carcinoma cells and embryonic brain tissues. Glycobiology 1(5), 527–535 (1991). doi:10.1093/glycob/1.5.527
Basu, S., Kaufman, B., Roseman, S.: Enzymatic synthesis of glucocerebroside by a glucosyltransferase from embryonic chicken brain. J. Biol. Chem. 248(4), 1388–1394 (1973)
Basu, S.C.: The serendipity of ganglioside biosynthesis: pathway to CARS and HY-CARS glycosyltransferases. Glycobiology 1(5), 469–475 (1991). doi:10.1093/glycob/1.5.469
Basu, S., Basu, M., Dastgheib, S., Hawes, J.W.: Biosynthesis and regulation of glycosphingolipids. In: Meth-Cohn, O., Pinto, B.M., Barton, D.H.R., Nakanishi, K. (eds.) Comprehensive Natural Products Chemistry, pp. 107–128. Pergamon, New York (1999)
Basu, S., Das, K., Basu, M.: Glycosyltransferase in glycosphingolipid biosynthesis. In: Ernst, B., Sinay, P., Hart, G. (eds.) Oligosaccharides in Chemistry and Biology—A Comprehensive Handbook, pp. 329–347. Wiley-VCH Verlag Gmbh, Germany (2000)
Roseman, S.: The synthesis of complex carbohydrates by multiglycosyltransferase systems and their potential function in intercellular adhesion. Chem. Phys. Lipids 5(1), 270–297 (1970). doi:10.1016/0009-3084(70)90024-1
Siskind, L.J.: Mitochondrial ceramide and the induction of apoptosis. J. Bioenerg. Biomembr. 37(3), 143–153 (2005). doi:10.1007/s10863-005-6567-7
Inokuchi, J., Radin, N.S.: Preparation of the active isomer of 1-phenyl-2-decanoylamino-3-morpholino-1-propanol, inhibitor of murine glucocerebroside synthetase. J. Lipid Res. 28(5), 565–571 (1987)
Radin, N.S.: Chemotherapy by slowing glucosphingolipid synthesis. Biochem. Pharmacol. 57(6), 589–595 (1999). doi:10.1016/S0006-2952(98)00274-3
Manning, L.S., Radin, N.S.: Effects of the glucolipid synthase inhibitor, P4, on functional and phenotypic parameters of murine myeloma cells. Br. J. Cancer 81(6), 952–958 (1999). doi:10.1038/sj.bjc.6690792
Chatterjee, S., Cleveland, T., Shi, W.Y., Inokuchi, J., Radin, N.S.: Studies of the action of ceramide-like substances (D- and L-PDMP) on sphingolipid glycosyltransferases and purified lactosylceramide synthase. Glycoconj. J. 13(3), 481–486 (1996). doi:10.1007/BF00731481
Basu, S., Ma, R., Mikulla, B., Bradley, M., Moulton, C., Basu, M., Banerjee, S., Inokuchi, J.: Apoptosis of human carcinoma cells in the presence of inhibitors of glycosphingolipid biosynthesis: I. Treatment of Colo-205 and SKBR3 cells with isomers of PDMP and PPMP. Glycoconj. J. 20(3), 157–168 (2004). doi:10.1023/B:GLYC.0000024254.64450.8b
Ma, R., Koulov, A., Moulton, C., Basu, M., Banerjee, S., Goodson, H., Basu, S.: Apoptosis of human breast carcinoma cells in the presence of disialosyl gangliosides: II. Treatment of SKBR3 cells with GD3 and GD1b gangliosides. Glycoconj. J. 20(5), 319–330 (2004). doi:10.1023/B:GLYC.0000033628.39302.ae
Basu, S., Ma, R., Boyle, P.J., Mikulla, B., Bradley, M., Smith, B., Basu, M., Banerjee, S.: Apoptosis of human carcinoma cells in the presence of potential anti-cancer drugs: III. Treatment of Colo-205 and SKBR3 cells with: cis -platin, Tamoxifen, Melphalan, Betulinic acid, L-PDMP, L-PPMP, and GD3 ganglioside. Glycoconj. J. 20(9), 563–577 (2004). doi:10.1023/B:GLYC.0000043293.46845.07
Boyle, P.J., Ma, R., Tuteja, N., Banerjee, S., Basu, S.: Apoptosis of human breast carcinoma cells in the presence of cis-platin and L-/D-PPMP: IV. Modulation of replication complexes and glycolipid: glycosyltransferases. Glycoconj. J. 23(3–4), 175–187 (2006). doi:10.1007/s10719-006-7923-5
Basu, S., Ma, R., Basu, M., Goodson, H., Smith, B., Banerjee, S.: Glycosphingolipid metabolism and signaling in apoptotic cancer cells, lipids: sphingolipid metabolizing enzymes, In: Haldar, D., Das, S.K. (eds.) Research Signpost, p. 81–100. India (2004)
Ma, R., Hopp, E.A., Decker, M.N., Loucks, A.J., Johnson, J.R., Moskal, J.R., Basu, M., Banerjee, S., Basu, S.: Regulation of glycosyltransferase genes in apoptotic breast cancer cells induced by L-PPMP and cis-Platin. In Proceedings of the Molecular Immunology Cancer Congress. Kluwer, Boston (in press) (2009)
Ma, R.: Apoptosis of breast and colon carcinoma cells by inhibitors of glycolipid and DNA biosynthesis. In Chemistry and Biochemistry, p. 272. University of Notre Dame, Notre Dame (2007)
Kroes, R.A., Panksepp, J., Burgdorf, J., Otto, N.J., Moskal, J.R.: Modeling depression: social dominance-submission gene expression patterns in rat neocortex. Neuroscience 137(1), 37–49 (2006). doi:10.1016/j.neuroscience.2005.08.076
Ritter, G., Livingston, P.O.: Ganglioside antigens expressed by human cancer cells. Semin. Cancer Biol. 2(6), 401–409 (1991)
Hakomori, S.: Tumor-associated carbohydrate antigens defining tumor malignancy: basis for development of anti-cancer vaccines. Adv. Exp. Med. Biol. 491, 369–402 (2001)
Nohara, K., Wang, F., Spiegel, S.: Glycosphingolipid composition of MDA-MB-231 and MCF-7 human breast cancer cell lines. Breast Cancer Res. Treat. 48(2), 149–157 (1998). doi:10.1023/A:1005986606010
Ugorski, M., Laskowska, A.: Sialyl Lewis(a): a tumor-associated carbohydrate antigen involved in adhesion and metastatic potential of cancer cells. Acta Biochim. Pol. 49(2), 303–311 (2002)
Kikuchi, N., Narimatsu, H.: Bioinformatics for comprehensive finding and analysis of glycosyltransferases. Biochim. Biophys. Acta 1760(4), 578–583 (2006)
Higashi, H., Basu, M., Basu, S.: Biosynthesis in vitro of disialosylneolactotetraosylceramide by a solubilized sialyltransferase from embryonic chicken brain. J. Biol. Chem. 260(2), 824–828 (1985)
Das, K.K., Basu, M., Basu, S.: A rapid preparative method for isolation of neutral and acidic glycosphingolipids by radial thin-layer chromatography. Anal. Biochem. 143(1), 125–134 (1984). doi:10.1016/0003-2697(84)90566-9
Tusher, V.G., Tibshirani, R., Chu, G.: Significance analysis of microarrays applied to the ionizing radiation response. Proc. Natl. Acad. Sci. U.S.A. 98(9), 5116–5121 (2001). doi:10.1073/pnas.091062498
Johnson, J.R.: Targeted delivery of molecular cargo and fluorescent bioimaging agents. In Chemistry and Biochemistry. University of Notre Dame: Notre Dame (2008).
Arunkumar, E., Fu, N., Smith, B.D.: Squaraine-derived rotaxanes: highly stable, fluorescent near-IR dyes. Chemistry (Easton) 12(17), 4684–4690 (2006)
Yamamoto, H., Oviedo, A., Sweeley, C., Saito, T., Moskal, J.R.: Alpha2,6-sialylation of cell-surface N-glycans inhibits glioma formation in vivo. Cancer Res. 61(18), 6822–6829 (2001)
Moskal, J.R., Kroes, R.A.: The development of glycobiology-based therapeutics for the treatment of brain tumors. Curr. Drug Targets (in press)
Siddik, Z.H.: Cisplatin: mode of cytotoxic action and molecular basis of resistance. Oncogene 22(47), 7265–7279 (2003). doi:10.1038/sj.onc.1206933
Rosenberg, B., VanCamp, L., Trosko, J.E., Mansour, V.H.: Platinum compounds: a new class of potent antitumour agents. Nature 222(5191), 385–386 (1969). doi:10.1038/222385a0
Jamieson, E.R., Lippard, S.J.: Structure, Recognition, and Processing of Cisplatin-DNA Adducts. Chem. Rev. 99(9), 2467–2498 (1999). doi:10.1021/cr980421n
Koulov, A.V., Stucker, K.A., Lakshmi, C., Robinson, J.P., Smith, B.D.: Detection of apoptotic cells using a synthetic fluorescent sensor for membrane surfaces that contain phosphatidylserine. Cell Death Differ. 10(12), 1357–1359 (2003). doi:10.1038/sj.cdd.4401315
Hanshaw, R.G., Smith, B.D.: New reagents for phosphatidylserine recognition and detection of apoptosis. Bioorg. Med. Chem. 13(17), 5035–5042 (2005). doi:10.1016/j.bmc.2005.04.071
Strasser, A., O'Connor, L., Dixit, V.M.: Apoptosis signaling. Annu. Rev. Biochem. 69, 217–245 (2000). doi:10.1146/annurev.biochem.69.1.217
Fulda, S., Debatin, K.M.: Extrinsic versus intrinsic apoptosis pathways in anticancer chemotherapy. Oncogene 25(34), 4798–4811 (2006). doi:10.1038/sj.onc.1209608
Xia, Z., Dickens, M., Raingeaud, J., Davis, R.J., Greenberg, M.E.: Opposing effects of ERK and JNK-p38 MAP kinases on apoptosis. Science 270(5240), 1326–1331 (1995). doi:10.1126/science.270.5240.1326
Qasba, P.K., Ramakrishnan, B., Boeggeman, E.: Structure and function of beta -1,4-galactosyltransferase. Curr. Drug Targets 9(4), 292–309 (2008). doi:10.2174/138945008783954943
Sen, R., Baltimore, D.: Multiple nuclear factors interact with the immunoglobulin enhancer sequences. Cell 46(5), 705–716 (1986). doi:10.1016/0092-8674(86)90346-6
Lewis, T.S., Shapiro, P.S., Ahn, N.G.: Signal transduction through MAP kinase cascades. Adv. Cancer Res. 74, 49–139 (1998). doi:10.1016/S0065-230X(08)60765-4
Zarubin, T., Han, J.: Activation and signaling of the p38 MAP kinase pathway. Cell Res. 15(1), 11–18 (2005). doi:10.1038/sj.cr.7290257
Kelley, T.J., Moghaddas, S., Bose, R., Basu, S.: Inhibition of immunopurified DNA polymerase-alpha from PA-3 prostate tumor cells by platinum (II) antitumor drugs. Cancer Biochem. Biophys. 13(3), 135–146 (1993)
Boyle, P.J.: Characterization of DNA helicase-III in replication complexes isolated from embryonic chicken brains and breast carcinoma cells. In Chemistry and Biochemistry, p. 188. University of Notre Dame: Notre Dame. (2005)
Bose, R.N., Li, D., Kennedy, M., Basu, S. (1995) Facile Formation of cis-platin nanopeptide complex of human DNA polymerase-a origin. J. Chem. Soc. Commun. Royal Soc. Chem., 1731–1732.
Bose, R.N., Li, D., Yang, W.W., Basu, S.: NMR structures of a nonapeptide from DNA binding domain of human polymerase-alpha determined by iterative complete-relaxation-matrix approach. J. Biomol. Struct. Dyn. 16(5), 1075–1085 (1999)
Acknowledgments
This article was written based on research supported by grants NS-18005 (NIMDS), CA-14764 (NCI) and grants-in-aid from the Bayer Corporation Elkhart, Indiana, and Coleman Foundation, Chicago, IL. to S. Basu. We are grateful to Dr. Surendra Gupta of American Radiolabeled Corporation, St. Louis and Sudip Basu of Moraveck Chemicals Corporation, Brea, CA, for providing us radioactive precursor chemicals need for this project. We are thankful to Professor Bradley Smith of the University of Notre Dame for his newly synthesized PSS-380 and AKS-0 dyes used for phosphatidylserine-binding and mitochondrial and Golgi-membrane scrambling studies. Our special thanks to Professor Jen-ichi Inokuchi of Hokkaido. University, Hokkaido, Japan, for providing us gift samples of chemically synthesized L-/D-PPMP and L-/D-PDMP used as apoptotic agents. We gratefully acknowledge the editorial help of Ms. Dorisanne Nielsen, and Christopher Thomas during preparation of this manuscript.
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
About this article
Cite this article
Ma, R., Matthew Decker, N., Anilus, V. et al. Post-translational and transcriptional regulation of glycolipid glycosyltransferase genes in apoptotic breast carcinoma cells: VII. Studied by DNA-microarray after treatment with l-PPMP. Glycoconj J 26, 647–661 (2009). https://doi.org/10.1007/s10719-008-9219-4
Received:
Revised:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s10719-008-9219-4