Abstract
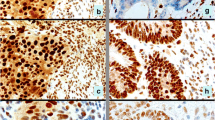
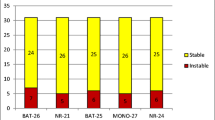
In 1997 Bethesda Guidelines (BG) were established and in 2004 those criteria were revised (RBG), with the main goal of selecting colorectal cancers (CRC) that should be subjected to microsatellite instability (MSI) testing. High microsatellite instability (MSI-H) is an intermediate marker for mutational analysis of the mismatch repair (MMR) genes involved in the genesis of Lynch Syndrome (LS). We aimed to evaluate and compare BG/RBG in the detection of MSI-H and subsequent identification of pathogenic MMR genes mutations. We included 174 patients with CRC and indication for MSI analysis according to BG or RBG. MSI testing was performed with the Bethesda markers and mutational analysis of MLH1, MSH2 and MSH6 genes undertaken with DGGE, MLPA and direct sequencing. One hundred fourteen of 174 patients (65.5 %) fulfilled BG and all of them RBG. With the BG, MSI-H was detected in 37/114 (32.5 %) CRCs and mutational analysis was positive in 14/37 (37.8 %) patients. The RBG led to detection of MSI-H in 49/174 (28.2 %) of the CRCs, having the mutational analysis been positive in 16/49 (32.7 %) patients. We could identify 14/114 (12.3 %) new cases of LS, through BG and 16/174 (9.2 %) via RBG. BG presented a similar overall percentage for the detection of MSI-H and mutations when compared with RBG. RBG implicated the analysis of more patients, though they gave rise to detection of two additional LS cases. This difference has a significant impact on the establishment of preventive measures, mainly for CRC, in all the mutation-carriers belonging to these families.

Similar content being viewed by others
References
Aaltonen LA, Salovaara R, Kristo P, Canzian F, Hemminki A, Peltomäki P et al (1998) Incidence of hereditary nonpolyposis colorectal cancer and the feasibility of molecular screening for the disease. N Engl J Med 338(21):1481–1487
Hampel H, Frankel WL, Martin E, Arnold M, Khanduja K, Kuebler P et al (2008) Feasibility of screening for Lynch syndrome among patients with colorectal cancer. J Clin Oncol 26:5783–5788
Lynch HT, de la Chapelle A (2003) Hereditary colorectal cancer. N Engl J Med 348:919–932
Vasen HF, Wijnen JT, Menko FH, Kleibeuker JH, Taal BG, Griffioen G et al (1996) Cancer risk in families with hereditary nonpolyposis colorectal cancer diagnosed by mutation analysis. Gastroenterology 110:1020–1027
Stoffel E, Mukherjee B, Raymond VM, Tayob N, Kastrinos F, Sparr J et al (2009) Calculation of risk of colorectal and endometrial cancer among patients with Lynch syndrome. Gastroenterology 137:1621–1627
Hendriks YM, Wagner A, Morreau H, Menko F, Stormorken A, Quehenberger F et al (2004) Cancer risk in hereditary nonpolyposis colorectal cancer due to MSH6 mutations: impact on counseling and surveillance. Gastroenterology 127:17–25
Quehenberger F, Vasen HF, van Houwelingen HC (2005) Risk of colorectal and endometrial cancer for carriers of mutations of the hMLH1 and hMSH2 gene: correction for ascertainment. J Med Genet 42:491–496
Peltomäki P, Vasen H (2004) Mutations associated with HNPCC predisposition—update of ICG-HNPCC/INSiGHT mutation database. Dis Markers 20:269–276
Rustgi AK (2007) The genetics of hereditary colon cancer. Genes Dev 21:2525–2538
Boland CR, Goel A (2010) Microsatellite instability in colorectal cancer. Gastroenterology 138:2073–2087
Aaltonen LA, Peltomäki P, Mecklin JP, Järvinen H, Jass JR, Green JS et al (1994) Replication errors in benign and malignant tumors from hereditary nonpolyposis colorectal cancer patients. Cancer Res 54:1645–1648
Kane MF, Loda M, Gaida GM, Lipman J, Mishra R, Goldman H et al (1997) Methylation of the hMLH1 promoter correlates with lack of expression of hMLH1 in sporadic colon tumors and mismatch repair-defective human tumor cell lines. Cancer Res 57:808–811
Järvinen HJ, Aarnio M, Mustonen H, Aktan-Collan K, Aaltonen LA, Peltomäki P et al (2000) Controlled 15-year trial on screening for colorectal cancer in families with hereditary nonpolyposis colorectal cancer. Gastroenterology 118:829–834
Vasen HF, Mecklin JP, Khan PM, Lynch HT (1991) The international collaborative group on hereditary non-polyposis colorectal cancer (ICG-HNPCC). Dis Colon Rectum 34:424–425
Vasen HF, Watson P, Mecklin JP, Lynch HT (1999) New clinical criteria for hereditary nonpolyposis colorectal cancer (HNPCC, Lynch syndrome) proposed by the International Collaborative group on HNPCC. Gastroenterology 116:1453–1456
Rodriguez-Bigas MA, Boland CR, Hamilton SR, Henson DE, Jass JR, Khan PM et al (1997) A National Cancer Institute workshop on hereditary nonpolyposis colorectal cancer syndrome: meeting highlights and Bethesda guidelines. J Natl Cancer Inst 89:1758–1762
Umar A, Boland CR, Terdiman JP, Syngal S, de la Chapelle A, Rüschoff J et al (2004) Revised Bethesda guidelines for hereditary nonpolyposis colorectal cancer (Lynch syndrome) and microsatellite instability. J Natl Cancer Inst 96:261–268
Jasperson KW, Tuohy TM, Neklason DW, Burt RW (2010) Hereditary and familial colon cancer. Gastroenterology 138:2044–2058
Ramsey SD, Clarke L, Etzioni R, Higashi M, Berry K, Urban N (2001) Cost-effectiveness of microsatellite instability screening as a method for detecting hereditary nonpolyposis colorectal cancer. Ann Intern Med 135:577–588
Reyes CM, Allen BA, Terdiman JP, Wilson LS (2002) Comparison of selection strategies for genetic testing of patients with hereditary nonpolyposis colorectal carcinoma: effectiveness and cost-effectiveness. Cancer 95:1848–1856
Piñol V, Castells A, Andreu M, Castellví-Bel S, Alenda C, Llor X et al (2005) Accuracy of revised Bethesda guidelines, microsatellite instability, and immunohistochemistry for the identification of patients with hereditary nonpolyposis colorectal cancer. JAMA 293:1986–1994
de Jong AE, van Puijenbroek M, Hendriks Y, Tops C, Wijnen J, Ausems MG et al (2004) Microsatellite instability, immunohistochemistry, and additional PMS2 staining in suspected hereditary nonpolyposis colorectal cancer. Clin Cancer Res 10:972–980
Barnetson RA, Tenesa A, Farrington SM, Nicholl ID, Cetnarskyj R, Porteous ME et al (2006) Identification and survival of carriers of mutations in DNA mismatch-repair genes in colon cancer. N Engl J Med 354:2751–2763
Balmaña J, Stockwell DH, Steyerberg EW, Stoffel EM, Deffenbaugh AM, Reid JE et al (2006) Prediction of MLH1 and MSH2 mutations in Lynch syndrome. JAMA 296:1469–1478
Chen S, Wang W, Lee S, Nafa K, Lee J, Romans K et al (2006) Prediction of germline mutations and cancer risk in the Lynch syndrome. JAMA 296:1479–1487
Tresallet C, Brouquet A, Julié C, Beauchet A, Vallot C, Ménégaux F et al (2011) Evaluation of predictive models in daily practice for the identification of patients with Lynch syndrome. Int J Cancer doi. doi:10.1002/ijc.26144
Ferreira S, Claro I, Lage P, Filipe B, Fonseca R, Sousa R et al (2008) Colorectal adenomas in young patients: microsatellite instability is not a useful marker to detect new cases of Lynch syndrome. Dis Colon Rectum 51:909–915
Nyström-Lahti M, Wu Y, Moisio AL, Hofstra RM, Osinga J, Mecklin JP et al (1996) DNA mismatch repair gene mutations in 55 kindreds with verified or putative hereditary non-polyposis colorectal cancer. Hum Mol Genet 5:763–769
Wu Y, Nyström-Lahti M, Osinga J, Looman MW, Peltomäki P, Aaltonen LA et al (1997) MSH2 and MLH1 mutations in sporadic replication error-positive colorectal carcinoma as assessed by two-dimensional DNA electrophoresis. Genes Chromosomes Cancer 18:269–278
Wu Y, Berends MJ, Mensink RG, Kempinga C, Sijmons RH, van Der Zee AG et al (1999) Association of hereditary nonpolyposis colorectal cancer-related tumors displaying low microsatellite instability with MSH6 germline mutations. Am J Hum Genet 65:1291–1298
Holinski-Feder E, Müller-Koch Y, Friedl W, Moeslein G, Keller G, Plaschke J et al (2001) DHPLC mutation analysis of the hereditary nonpolyposis colon cancer (HNPCC) genes hMLH1 and hMSH2. J Biochem Biophys Meth 47:21–32
Rodríguez-Moranta F, Castells A, Andreu M, Piñol V, Castellví-Bel S, Alenda C et al (2006) Clinical performance of original and revised Bethesda guidelines for the identification of MSH2/MLH1 gene carriers in patients with newly diagnosed colorectal cancer: proposal of a new and simpler set of recommendations. Am J Gastroenterol 101:1104–1111
Terdiman JP, Gum JR Jr, Conrad PG, Miller GA, Weinberg V, Crawley SC et al (2001) Efficient detection of hereditary nonpolyposis colorectal cancer gene carriers by screening for tumor microsatellite instability before germline genetic testing. Gastroenterology 120:21–30
Vasen HF (2007) Review article: the Lynch syndrome (hereditary nonpolyposis colorectal cancer). Aliment Pharmacol Ther 26(Suppl 2):113–126
Jang E, Chung D (2010) Hereditary colon cancer: Lynch syndrome. Gut Liver 4:151–160
Jass JR (2004) HNPCC and sporadic MSI-H colorectal cancer: a review of the morphological similarities and differences. Fam Cancer 3:93–100
Truta B, Chen YY, Blanco AM, Deng G, Conrad PG, Kim YH et al (2008) Tumor histology helps to identify Lynch syndrome among colorectal cancer patients. Fam Cancer 7:267–274
Pérez-Carbonell L, Ruiz-Ponte C, Guarinos C, Alenda C, Payá A, Brea A et al (2011) Comparison between universal molecular screening for Lynch syndrome and revised Bethesda guidelines in a large population-based cohort of patients with colorectal cancer. Gut. doi:gutjnl-2011-300041
Julié C, Trésallet C, Brouquet A, Vallot C, Zimmermann U, Mitry E et al (2008) Identification in daily practice of patients with Lynch syndrome (hereditary nonpolyposis colorectal cancer): revised Bethesda guidelines-based approach versus molecular screening. Am J Gastroenterol 103:2825–2835
Morrison J, Bronner M, Leach BH, Downs-Kelly E, Goldblum JR, Liu X (2011) Lynch syndrome screening in newly diagnosed colorectal cancer in general pathology practice: from the revised Bethesda guidelines to a universal approach. Scand J Gastroenterol 46:1340–1348
Canard G, Lefevre JH, Colas C, Coulet F, Svrcek M, Lascols O et al (2011) Screening for Lynch syndrome in colorectal cancer: are we doing enough? Ann Surg Oncol. doi:10.1245/s10434-011-2014-7
Gologan A, Krasinskas A, Hunt J, Thull DL, Farkas L, Sepulveda AR (2005) Performance of the revised Bethesda guidelines for identification of colorectal carcinomas with a high level of microsatellite instability. Arch Pathol Lab Med 129:1390–1397
Balmaña J, Balaguer F, Castellví-Bel S, Steyerberg EW, Andreu M, Llor X et al (2008) Comparison of predictive models, clinical criteria and molecular tumour screening for the identification of patients with Lynch syndrome in a population-based cohort of colorectal cancer patients. J Med Genet 45:557–563
Acknowledgments
The authors thank Isadora Rosa, MD, for her helpful comments on the manuscript and statistical advice.
Conflict of interest
The authors declare that they have no conflict of interest.
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
About this article
Cite this article
Serrano, M., Lage, P., Belga, S. et al. Bethesda criteria for microsatellite instability testing: impact on the detection of new cases of Lynch syndrome. Familial Cancer 11, 571–578 (2012). https://doi.org/10.1007/s10689-012-9550-6
Published:
Issue Date:
DOI: https://doi.org/10.1007/s10689-012-9550-6