Abstract
Background
Prospective studies on bleeding risk during/after gastrointestinal endoscopic procedures are rare.
Aim
We investigated the risk of endoscopic procedure-related bleeding in patients with biopsy and/or cold snare polypectomy (CSP) in relation to antithrombotic therapy.
Methods
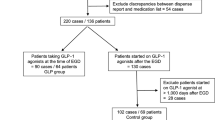
This prospective, observational single-center cohort study (NCT02594813) enrolled consecutive patients who underwent diagnostic esophagogastroduodenoscopy (EGD) or colonoscopy. The primary outcome measure was delayed bleeding in patients with biopsy and/or CSP who required endoscopic treatment within 2 weeks post-procedure. The secondary outcomes were immediate bleeding and the number of hemostatic clips used during the procedure.
Results
From November 2015 to October 2018 at our institution, 3069 (mean age, 66 years) and 37,887 (57 years) patients underwent EGD with and without antithrombotic therapy, respectively. In addition, 1116 (72 years) and 11,901 (65 years) patients had colonoscopy with and without antithrombotic therapy, respectively. In the 3069 EGD patients receiving antithrombotic therapy, no delayed bleeding occurred, whereas immediate bleeding occurred in 9 of 141 patients (6.4%) with biopsy. Of the 1116 colonoscopy patients receiving antithrombotic therapy, delayed bleeding occurred in three of 228 (1.3%) following CSP. Immediate bleeding occurred in nine of 225 (4%) following biopsy and in 32 of 228 (14%) following CSP. Multivariate analysis following univariate analysis identified chronic kidney disease and CSP as factors significantly associated with procedure-related bleeding in patients taking antithrombotic agents.
Conclusion
The risk of delayed bleeding in diagnostic EGD with biopsy or in colonoscopy with biopsy and/or CSP was low despite continuation of antithrombotic therapy.
Similar content being viewed by others
Abbreviations
- EGD:
-
Esophagogastroduodenoscopy
- CSP:
-
Cold snare polypectomy
References
Zhu J, Alexander GC, Nazarian S, et al. Trends and variation in oral anticoagulant choice in patients with atrial fibrillation, 2010-2017. Pharmacotherapy 2018; 38: 907–20.
Fujimoto K, Fujishiro M, Kato M, et al. Guidelines for gastroenterological endoscopy in patients undergoing antithrombotic treatment. Digestive Endoscopy. 2014;26:1–14.
Acosta RD, Abraham NS, Chandrasekhara V, et al. The management of antithrombotic agents for patients undergoing GI endoscopy. Gastrointest Endosc. 2016;83:3–16.
Horiuchi A, Nakayama Y, Kajiyama M, et al. Removal of small colorectal polyps in anticoagulated patients: a prospective randomized comparison of cold snare and conventional polypectomy. Gastrointest Endosc. 2014;79:417–423.
Makino T, Horiuchi A, Kajiyama M, et al. Delayed bleeding following cold snare polypectomy for small colorectal polyps in patients taking antithrombotic agents. J Clin Gastroenterol. 2018;52:502–507.
Horiuchi A, Nakayama Y, Hidaka N, et al. Low-dose propofol sedation for diagnostic esophagogastroduodenoscopy: results in 10,662 adults. Am J Gastroenterol. 2009;104:1650–1655.
Horiuchi A, Nakayama Y, Fujii H, et al. Psychomotor recovery and blood propofol level in colonoscopy when using propofol sedation. Gastrointest Endosc. 2012;75:506–512.
Sato M, Horiuchi A, Tamaki M, et al. Safety and effectiveness of nurse-administered propofol sedation in outpatients undergoing gastrointestinal endoscopy. Clin Gastroenterol Hepatol. 2019;17:1098–1104.
Cancer Registry and Statistics. Cancer Information Service, National Cancer Center, Japan.
Siegel R, Desantis C, Jemal A. Colorectal cancer statistics, 2014. CA Cancer J Clin. 2014;64:104–117.
Zauber AG, Winawer SJ, O’Brien MJ, et al. Colonoscopic polypectomy and long-term prevention of colorectal-cancer deaths. N Engl J Med. 2012;366:687–696.
Repici A, Hassan C, Vitetta E, et al. Safety of cold polypectomy for < 10 mm polyps at colonoscopy: a prospective multicenter study. Endoscopy. 2012;44:27–31.
Gatto NM, Frucht H, Sundararajan V, et al. Risk of perforation after colonoscopy and sigmoidoscopy: a population-based study. J Natl Cancer Inst. 2003;95:230–236.
Heldwein W, Dollhopf M, Rosch T, et al. The munich polypectomy study (MUPS): prospective analysis of complications and risk factors in 4000 colonic snare polypectomies. Endoscopy. 2005;37:1116–1122.
Shioji K, Suzuki Y, Kobayashi M, et al. Prophylactic clip application does not decrease delayed bleeding after colonoscopic polypectomy. Gastrointest Endosc. 2003;57:691–694.
Robbins R, Tian C, Singal A, et al. Periprocedural management of aspirin during colonoscopy: a survey of practice patterns in the United States. Gastrointest Endosc. 2015;82:895–900.
Lin D, Soetikno RM, McQuaid K, et al. Risk factors for postpolypectomy bleeding in patients receiving anticoagulation or antiplatelet medications. Gastrointest Endosc. 2018;87:1106–1113.
Acknowledgments
The authors thank Prof. David Y. Graham for his editorial assistance and assistance with English.
Author information
Authors and Affiliations
Corresponding author
Additional information
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
About this article
Cite this article
Yabe, K., Horiuchi, A., Kudo, T. et al. Risk of Gastrointestinal Endoscopic Procedure-Related Bleeding in Patients With or Without Continued Antithrombotic Therapy. Dig Dis Sci 66, 1548–1555 (2021). https://doi.org/10.1007/s10620-020-06393-1
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s10620-020-06393-1