Abstract
Introduction
The impact of antithrombotic treatment on the findings of small-bowel capsule endoscopy for patients with obscure gastrointestinal bleeding remains contentious. We aimed to determine the effect of these agents on small-bowel video capsule endoscopy positive findings.
Methods
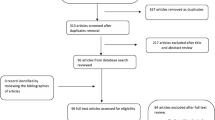
MEDLINE, Cochrane Library, and Google Scholar were searched for studies reporting on patients receiving concurrent antithrombotic treatment, while undergoing capsule endoscopy for obscure gastrointestinal bleeding (OGIB). Outcomes were the effect of antithrombotic therapy—overall and per type of antithrombotic agent—on the examination’s positive findings and re-bleeding risk. The effect size of study outcomes is presented as odds ratio (OR) with 95% confidence interval (CI).
Results
Fourteen studies with 1023 patients were included. We detected significant heterogeneity with no evidence of publication bias. Compared to antithrombotic drug nonusers, antithrombotic treatment was associated with an increased prevalence of positive findings [OR 1.98 (95% CI 1.34–2.93); P = 0.0006]. This effect did not differ between antiplatelet and anticoagulant treatments [OR 2.22 (95% CI 1.28–3.84); P = 0.005 and 2.53 (95% CI 1.66–3.87); P < 0.0001, respectively]. Antithrombotic use over no use was not associated either with overt [OR 1.17 (95% CI 0.51–2.66); P = 0.71] or with occult [OR 0.86 (95% CI 0.38–1.95); P = 0.71] bleeding pattern. However, concurrent antithrombotic treatment was associated with higher odds for re-bleeding compared to no treatment [OR 2.53 (95% CI 1.46–4.37); P = 0.0009].
Conclusions
Antithrombotic treatment is associated with more positive findings in small-bowel video capsule endoscopy in OGIB as well as higher odds of re-bleeding.




Similar content being viewed by others
References
Pennazio M, Spada C, Eliakim R, et al. Small-bowel capsule endoscopy and device-assisted enteroscopy for diagnosis and treatment of small-bowel disorders: European Society of Gastrointestinal Endoscopy (ESGE) clinical guideline. Endoscopy. 2015;47:352–376.
Tziatzios G, Gkolfakis P, Dimitriadis GD, Triantafyllou K. Long-term effects of video capsule endoscopy in the management of obscure gastrointestinal bleeding. Ann Transl Med. 2017;5:196.
Maiden L, Thjodleifsson B, Seigal A, et al. Long-term effects of nonsteroidal anti-inflammatory drugs and cyclooxygenase-2 selective agents on the small bowel: a cross-sectional capsule enteroscopy study. Clin Gastroenterol Hepatol. 2007;5:1040–1045.
Nagata N, Niikura R, Yamada A, et al. Acute middle gastrointestinal bleeding risk associated with NSAIDs, antithrombotic drugs, and PPIs: a multicenter case-control study. PLoS ONE. 2016;11:e0151332.
Lepileur L, Dray X, Antonietti M, et al. Factors associated with diagnosis of obscure gastrointestinal bleeding by video capsule enteroscopy. Clin Gastroenterol Hepatol. 2012;10:1376–1380.
Shiotani A, Honda K, Murao T, et al. Combination of low-dose aspirin and thienopyridine exacerbates small bowel injury. Scand J Gastroenterol. 2011;46:281–286.
Curdia Goncalves T, Arieira C, Monteiro S, Rosa B, Moreira MJ, Cotter J. ORBIT score: an useful predictor of small bowel rebleeding in patients under chronic anticoagulation. Scand J Gastroenterol. 2018;53:179–184.
Moher D, Shamseer L, Clarke M, et al. Preferred reporting items for systematic review and meta-analysis protocols (PRISMA-P) 2015 statement. Syst Rev. 2015;4:1.
Raju GS, Gerson L, Das A, Lewis B, American Gastroenterological A. American Gastroenterological Association (AGA) Institute technical review on obscure gastrointestinal bleeding. Gastroenterology. 2007;133:1697–1717.
Stang A. Critical evaluation of the Newcastle–Ottawa scale for the assessment of the quality of nonrandomized studies in meta-analyses. Eur J Epidemiol. 2010;25:603–605.
Gerson LB, Fidler JL, Cave DR, Leighton JA. ACG clinical guideline: diagnosis and management of small bowel bleeding. Am J Gastroenterol. 2015;110:1265–1287.
Saurin JC, Delvaux M, Gaudin JL, et al. Diagnostic value of endoscopic capsule in patients with obscure digestive bleeding: blinded comparison with video push-enteroscopy. Endoscopy. 2003;35:576–584.
Veitch AM, Vanbiervliet G, Gershlick AH, et al. Endoscopy in patients on antiplatelet or anticoagulant therapy, including direct oral anticoagulants: British Society of Gastroenterology (BSG) and European Society of Gastrointestinal Endoscopy (ESGE) guidelines. Endoscopy. 2016;48:385–402.
Tziatzios G, Gkolfakis P, Hassan C, et al. Meta-analysis shows similar re-bleeding rates among Western and Eastern populations after index video capsule endoscopy. Dig Liver Dis. 2018;50:226–239.
Egger M, Davey Smith G, Schneider M, Minder C. Bias in meta-analysis detected by a simple, graphical test. BMJ. 1997;315:629–634.
Sterne JA, Sutton AJ, Ioannidis JP, et al. Recommendations for examining and interpreting funnel plot asymmetry in meta-analyses of randomised controlled trials. BMJ. 2011;343:d4002.
Macdonald J, Porter V, McNamara D. Negative capsule endoscopy in patients with obscure GI bleeding predicts low rebleeding rates. Gastrointest Endosc. 2008;68:1122–1127.
Sidhu R, Sanders DS, Kapur K, Leeds JS, McAlindon ME. Factors predicting the diagnostic yield and intervention in obscure gastrointestinal bleeding investigated using capsule endoscopy. J Gastroint Liver Dis. 2009;18:273–278.
Esaki M, Matsumoto T, Yada S, et al. Factors associated with the clinical impact of capsule endoscopy in patients with overt obscure gastrointestinal bleeding. Dig Dise Sci. 2010;55:2294–2301. https://doi.org/10.1007/s10620-009-1036-5.
Shahidi NC, Ou G, Svarta S, et al. Factors associated with positive findings from capsule endoscopy in patients with obscure gastrointestinal bleeding. Clin Gastroenterol Hepatol. 2012;10:1381–1385.
Kim JB, Ye BD, Song Y, et al. Frequency of rebleeding events in obscure gastrointestinal bleeding with negative capsule endoscopy. J Gastroenterol Hepatol. 2013;28:834–840.
Boal Carvalho P, Rosa B, Moreira MJ, Cotter J. New evidence on the impact of antithrombotics in patients submitted to small bowel capsule endoscopy for the evaluation of obscure gastrointestinal bleeding. Gastroenterol Res Pract. 2013;2014:709217.
Matsumura T, Arai M, Saito K, et al. Predictive factor of re-bleeding after negative capsule endoscopy for obscure gastrointestinal bleeding: over 1-year follow-up study. Dig Endosc. 2014;26:650–658.
Ribeiro I, Pinho R, Rodrigues A, Marques J, Fernandes C, Carvalho J. Obscure gastrointestinal bleeding: which factors are associated with positive capsule endoscopy findings? Rev Esp Enferm Dig. 2015;107:334–339.
Katsinelos P, Kountouras J, Chatzimavroudis G, et al. Factors predicting a positive capsule endoscopy in past overt obscure gastrointestinal bleeding: a multicenter retrospective study. Hippokratia. 2016;20:127–132.
Ormeci A, Akyuz F, Baran B, et al. What is the impact of capsule endoscopy in the long term period? World J Gastrointest Endosc. 2016;8:344–348.
Shimada S, Watanabe T, Nadatani Y, et al. Clinical factors associated with positive capsule endoscopy findings in patients with obscure gastrointestinal bleeding: a single-center study. Scand J Gastroenterol. 2017;52:1219–1223.
Gravito-Soares E, Gravito-Soares M, Almeida N, Lopes S, Figueiredo P. Clinical impact of small bowel capsule endoscopy in the era of antithrombotic therapy. Clin Rese Hepatol Gastroenterol. 2018;42:e41–e44.
Kono Y, Kawano S, Okamoto Y, et al. Clinical outcome of patients with obscure gastrointestinal bleeding during antithrombotic drug therapy. Ther Adv Gastroenterol. 2018;11:1–10. https://doi.org/10.1177/1756283X17746930
Nakamura S, Watanabe T, Shimada S, et al. Does discontinuation of antithrombotics affect the diagnostic yield of small bowel capsule endoscopy in patients demonstrating obscure gastrointestinal bleeding? J Clin Biochem Nutr. 2018;63:149–153.
Smecuol E, Pinto Sanchez MI, Suarez A, et al. Low-dose aspirin affects the small bowel mucosa: results of a pilot study with a multidimensional assessment. Clin Gastroenterol Hepatol. 2009;7:524–529.
Ehrhard F, Nazeyrollas P, Brixi H, Heurgue-Berlot A, Thiefin G. Proximal predominance of small bowel injury associated with uncoated low-dose aspirin therapy: a video capsule study in chronic users. Eur J Gastroenterol Hepatol. 2013;25:1265–1272.
Min YW, Kim JS, Jeon SW, et al. Long-term outcome of capsule endoscopy in obscure gastrointestinal bleeding: a nationwide analysis. Endoscopy. 2014;46:59–65.
Yung DE, Rondonotti E, Giannakou A, et al. Capsule endoscopy in young patients with iron deficiency anaemia and negative bidirectional gastrointestinal endoscopy. U Eur Gastroenterol J. 2017;5:974–981.
Tan W, Ge ZZ, Gao YJ, et al. Long-term outcome in patients with obscure gastrointestinal bleeding after capsule endoscopy. J Dig Dis. 2015;16:125–134.
Samaha E, Rahmi G, Landi B, et al. Long-term outcome of patients treated with double balloon enteroscopy for small bowel vascular lesions. Am J Gastroenterol. 2012;107:240–246.
Triantafyllou K, Gkolfakis P, Viazis N, et al. A 13-year time trend analysis of 3724 small bowel video capsule endoscopies and a forecast model during the financial crisis in Greece. Eur J Gastroenterol Hepatol. 2017;29:185–191.
Acknowledgments
We acknowledge the contribution of Prof. Dr. Filiz Akyuz who kindly provided raw data of his study.
Author information
Authors and Affiliations
Contributions
G Tziatzios and P Gkolfakis acquired the data, performed the meta-analysis, drafted, and finally approved the manuscript; Ioannis S. Papanikolaou revised the draft critically for important intellectual content and finally approved the manuscript; K Triantafyllou conceived the idea, revised the draft critically for important intellectual content, and finally approved the manuscript.
Corresponding author
Ethics declarations
Conflict interest
All authors declare that they have no conflict of interests
Electronic supplementary material
Below is the link to the electronic supplementary material.
Rights and permissions
About this article
Cite this article
Tziatzios, G., Gkolfakis, P., Papanikolaou, I.S. et al. Antithrombotic Treatment Is Associated with Small-Bowel Video Capsule Endoscopy Positive Findings in Obscure Gastrointestinal Bleeding: A Systematic Review and Meta-Analysis. Dig Dis Sci 64, 15–24 (2019). https://doi.org/10.1007/s10620-018-5292-0
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s10620-018-5292-0