Abstract
Background
Previous studies have shown that several factors such as hemodynamic instability at admission are risk factors for rebleeding of peptic ulcer bleeding. However, whether steroid use increases the risk of rebleeding remains elusive.
Aims
This study aimed to clarify the risk factors for rebleeding after endoscopic hemostasis for peptic ulcer bleeding.
Methods
A total of 185 patients who underwent endoscopic hemostasis for peptic ulcer bleeding at our institution between 2005 and 2017 were retrospectively analyzed. We evaluated factors, including comorbid conditions, in-hospital onset, and steroid use, associated with rebleeding by logistic regression analysis. In addition, we investigated the association between the dose of steroids and rebleeding.
Results
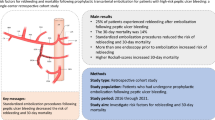
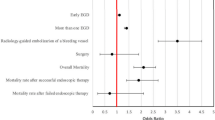
The rebleeding rate after endoscopic hemostasis for peptic ulcer bleeding was 14.6%. In the multivariate analysis, the independent risk factors for rebleeding were steroid use (odds ratio 4.56, p = 0.015), multiple ulcers (4.43, p = 0.005), number of comorbidities ≥ 3 3.18, p = 0.026), hemodynamic instability (3.06, p = 0.039), and number of comorbidities ≥ 3 (2.93, p = 0.047). Furthermore, the use of higher dose steroids (≥ 20 mg per day in prednisolone; 10.55, p = 0.002), but not lower dose (< 20 mg per day in prednisolone), was an independent risk factor for rebleeding in the multivariate analysis. The relationship between steroid use and rebleeding was observed in a dose-dependent manner (p for trend = 0.002).
Conclusions
This study first revealed that using higher dose steroids was an independent risk factor for rebleeding after endoscopic hemostasis for peptic ulcer bleeding, with a dose-response relation.



Similar content being viewed by others
Abbreviations
- PUB:
-
Peptic ulcer bleeding
- NSAIDs:
-
Nonsteroid antiinflammatory drugs
- GI:
-
Gastrointestinal
- PPI:
-
Proton pump inhibitor
- ASA:
-
American Society of Anesthesiologists
- PSL:
-
Prednisolone
- IQR:
-
Interquartile range
- ORs:
-
Odds ratios
- PEG:
-
Percutaneous endoscopic gastrostomy
- ENBD:
-
Endoscopic naso-biliary drainage
- CI:
-
Confidence interval
References
Longstreth GF. Epidemiology of hospitalization for acute upper gastrointestinal hemorrhage: a population-based study. Am J Gastroenterol. 1995;90:206–210.
Gralnek IM, Jensen DM, Gornbein J, et al. Clinical and economic outcomes of individuals with severe peptic ulcer hemorrhage and nonbleeding visible vessel: an analysis of two prospective clinical trials. Am J Gastroenterol. 1998;93:2047–2056.
Cook DJ, Guyatt GH, Salena BJ, Laine LA. Endoscopic therapy for acute nonvariceal upper gastrointestinal hemorrhage: a meta-analysis. Gastroenterology. 1992;102:139–148.
Lau JY, Sung JJ, Lee KK, et al. Effect of intravenous omeprazole on recurrent bleeding after endoscopic treatment of bleeding peptic ulcers. N Engl J Med. 2000;343:310–316.
Kim SB, Lee SH, Kim KO, et al. Risk factors associated with rebleeding in patients with high risk peptic ulcer bleeding: focusing on the role of second look endoscopy. Dig Dis Sci. 2016;61:517–522. https://doi.org/10.1007/s10620-015-3846-y.
Jensen DM, Pace SC, Soffer E, Comer GM, Study G. Continuous infusion of pantoprazole versus ranitidine for prevention of ulcer rebleeding: a U.S. multicenter randomized, double-blind study. Am J Gastroenterol. 2006;101:1991–1999. (quiz 2170).
Barkun A, Sabbah S, Enns R, et al. The Canadian Registry on Nonvariceal Upper Gastrointestinal Bleeding and Endoscopy (RUGBE): endoscopic hemostasis and proton pump inhibition are associated with improved outcomes in a real-life setting. Am J Gastroenterol. 2004;99:1238–1246.
Ramsoekh D, van Leerdam ME, Rauws EA, Tytgat GN. Outcome of peptic ulcer bleeding, nonsteroidal anti-inflammatory drug use, and Helicobacter pylori infection. Clin Gastroenterol Hepatol. 2005;3:859–864.
Rockall TA, Logan RF, Devlin HB, Northfield TC. Selection of patients for early discharge or outpatient care after acute upper gastrointestinal haemorrhage. National Audit of Acute Upper Gastrointestinal Haemorrhage. Lancet. 1996;347:1138–1140.
Simoens M, Rutgeerts P. Non-variceal upper gastrointestinal bleeding. Best Pract Res Clin Gastroenterol. 2001;15:121–133.
Chiu PW, Ng EK, Cheung FK, et al. Predicting mortality in patients with bleeding peptic ulcers after therapeutic endoscopy. Clin Gastroenterol Hepatol. 2009;7:311–316. (quiz 253).
Marmo R, Koch M, Cipolletta L, et al. Predicting mortality in non-variceal upper gastrointestinal bleeders: validation of the Italian PNED Score and Prospective Comparison with the Rockall Score. Am J Gastroenterol. 2010;105:1284–1291.
Chung IK, Kim EJ, Lee MS, et al. Endoscopic factors predisposing to rebleeding following endoscopic hemostasis in bleeding peptic ulcers. Endoscopy. 2001;33:969–975.
Guglielmi A, Ruzzenente A, Sandri M, et al. Risk assessment and prediction of rebleeding in bleeding gastroduodenal ulcer. Endoscopy. 2002;34:778–786.
Muller T, Barkun AN, Martel M. Non-variceal upper GI bleeding in patients already hospitalized for another condition. Am J Gastroenterol. 2009;104:330–339.
Garcia-Iglesias P, Villoria A, Suarez D, et al. Meta-analysis: predictors of rebleeding after endoscopic treatment for bleeding peptic ulcer. Aliment Pharmacol Ther. 2011;34:888–900.
Elmunzer BJ, Young SD, Inadomi JM, Schoenfeld P, Laine L. Systematic review of the predictors of recurrent hemorrhage after endoscopic hemostatic therapy for bleeding peptic ulcers. Am J Gastroenterol. 2008;103:2625–2632. (quiz 33).
Sakamoto C, Sugano K, Ota S, et al. Case-control study on the association of upper gastrointestinal bleeding and nonsteroidal anti-inflammatory drugs in Japan. Eur J Clin Pharmacol. 2006;62:765–772.
Weisman SM, Graham DY. Evaluation of the benefits and risks of low-dose aspirin in the secondary prevention of cardiovascular and cerebrovascular events. Arch Intern Med. 2002;162:2197–2202.
Lanas A, Wu P, Medin J, Mills EJ. Low doses of acetylsalicylic acid increase risk of gastrointestinal bleeding in a meta-analysis. Clin Gastroenterol Hepatol. 2011;9:e6.
Messer J, Reitman D, Sacks HS, Smith H Jr, Chalmers TC. Association of adrenocorticosteroid therapy and peptic-ulcer disease. N Engl J Med. 1983;309:21–24.
Narum S, Westergren T, Klemp M. Corticosteroids and risk of gastrointestinal bleeding: a systematic review and meta-analysis. BMJ Open. 2014;4:e004587.
Conn HO, Blitzer BL. Nonassociation of adrenocorticosteroid therapy and peptic ulcer. N Engl J Med. 1976;294:473–479.
Conn HO, Poynard T. Corticosteroids and peptic ulcer: meta-analysis of adverse events during steroid therapy. J Intern Med. 1994;236:619–632.
Park SJ, Park H, Lee YC, et al. Effect of scheduled second-look endoscopy on peptic ulcer bleeding: a prospective randomized multicenter trial. Gastrointest Endosc. 2018;87:457–465.
Forrest JA, Finlayson ND, Shearman DJ. Endoscopy in gastrointestinal bleeding. Lancet. 1974;2:394–397.
Lu Y, Chen YI, Barkun A. Endoscopic management of acute peptic ulcer bleeding. Gastroenterol Clin North Am. 2014;43:677–705.
Wong SK, Yu LM, Lau JY, et al. Prediction of therapeutic failure after adrenaline injection plus heater probe treatment in patients with bleeding peptic ulcer. Gut. 2002;50:322–325.
Oken MM, Creech RH, Tormey DC, et al. Toxicity and response criteria of the Eastern Cooperative Oncology Group. Am J Clin Oncol. 1982;5:649–655.
American Society of Anesthesiologists Task Force on S, Analgesia by N-A. Practice guidelines for sedation and analgesia by non-anesthesiologists. Anesthesiology. 2002;96:1004–1017.
Cheng HC, Wu CT, Chen WY, Yang EH, Chen PJ, Sheu BS. Risk factors determining the need for second-look endoscopy for peptic ulcer bleeding after endoscopic hemostasis and proton pump inhibitor infusion. Endosc Int Open. 2016;4:E255–E262.
Luo JC, Shin VY, Liu ES, et al. Dexamethasone delays ulcer healing by inhibition of angiogenesis in rat stomachs. Eur J Pharmacol. 2004;485:275–281.
Carpani de Kaski M, Rentsch R, Levi S, Hodgson HJ. Corticosteroids reduce regenerative repair of epithelium in experimental gastric ulcers. Gut. 1995;37:613–616.
Asayama N, Oka S, Tanaka S. Polyglycolic acid sheet application for intractable acute hemorrhagic rectal ulcer. Dig Endosc. 2016;28:689.
Dorff TB, Crawford ED. Management and challenges of corticosteroid therapy in men with metastatic castrate-resistant prostate cancer. Ann Oncol. 2013;24:31–38.
Auchus RJ, Yu MK, Nguyen S, Mundle SD. Use of prednisone with abiraterone acetate in metastatic castration-resistant prostate cancer. Oncologist. 2014;19:1231–1240.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflict of interest
All authors have no conflicts to declare.
Rights and permissions
About this article
Cite this article
Kondo, Y., Hatta, W., Koike, T. et al. The Use of Higher Dose Steroids Increases the Risk of Rebleeding After Endoscopic Hemostasis for Peptic Ulcer Bleeding. Dig Dis Sci 63, 3033–3040 (2018). https://doi.org/10.1007/s10620-018-5209-y
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s10620-018-5209-y