Abstract
Background
Prior to withdrawing the EUS-FNA needle from the lesion, the stopcock of the suction syringe is closed to reduce contamination. Residual negative pressure (RNP) may persist in the needle despite closing the stopcock.
Aims
To determine whether neutralizing RNP before withdrawing the needle will improve the cytology yield.
Methods
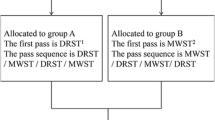
Bench-top testing was done to confirm the presence of RNP followed by a prospective, randomized, cross-over study on patients with pancreas mass. Ten milliliters of suction was applied to the FNA needle. Before withdrawing the needle from the lesion, the stopcock was closed. Based on randomization, the first pass was done with the stopcock either attached to the needle (S+) or disconnected (S−) to allow air to enter and neutralize RNP and accordingly the second pass was crossed over to S+ or S−. On-site cytopathologist was blinded to S+/S−.
Results
Bench tests confirmed the presence of RNP which was successfully neutralized by disconnecting the syringe (S−) from the needle. Sixty patients were enrolled, 120 samples analyzed. S+ samples showed significantly greater GI tract contamination compared to S− samples (16.7 vs. 6.7 %, p = 0.03). Of the 53 patients confirmed to have pancreas adenocarcinoma, FNA using S− approach was positive in 49 (93 %) compared to 40 using the S+ approach (76 %, p = 0.02).
Conclusions
Despite closing the stopcock of the suction syringe, RNP is present in the FNA needle. Neutralizing RNP prior to withdrawing the needle from the target lesion significantly decreased GI tract contamination of the sample thereby improving the FNA cytology yield.
Clinical Trials Registration Number
NCT01995474.




Similar content being viewed by others
Abbreviations
- EUS:
-
Endoscopic ultrasound
- FNA:
-
Fine needle aspiration
- S+:
-
Syringe-on; the suction syringe with its stopcock closed still attached to the needle handle
- S−:
-
Syringe-off; the suction syringe with its stopcock closed disconnected from the needle handle
- −:
-
Minus (negative pressure)
References
Dumonceau J-M, Polkowski M, Larghi A, et al. Indications, results, and clinical impact of endoscopic ultrasound (EUS)-guided sampling in gastroenterology: European Society of Gastrointestinal Endoscopy (ESGE) Clinical Guideline. Endoscopy. 2011;43:897–912.
Hewitt MJM, McPhail MJWM, Possamai LL, Dhar AA, Vlavianos PP, Monahan KJK. EUS-guided FNA for diagnosis of solid pancreatic neoplasms: a meta-analysis. Gastrointest Endosc. 2012;75:319–331.
Mertz H, Gautam S. The learning curve for EUS-guided FNA of pancreatic cancer. Gastrointest Endosc. 2004;59:33–37.
Yusuf TET, Ho SS, Pavey DAD, Michael HH, Gress FGF. Retrospective analysis of the utility of endoscopic ultrasound-guided fine-needle aspiration (EUS-FNA) in pancreatic masses, using a 22-gauge or 25-gauge needle system: a multicenter experience. Endoscopy. 2009;41:445–448.
Song TJ, Kim JH, Lee SS, et al. The prospective randomized, controlled trial of endoscopic ultrasound-guided fine-needle aspiration using 22G and 19G aspiration needles for solid pancreatic or peripancreatic masses. Am J Gastroenterol. 2010;105:1739–1745.
Klapman Logrono, Dye Waxman. Clinical impact of on-site cytopathology interpretation on endoscopic ultrasound-guided fine needle aspiration. Am J Gastroenterol. 2003;98:1289–1294.
Wani S, Early D, Kunkel J, et al. Diagnostic yield of malignancy during EUS-guided FNA of solid lesions with and without a stylet: a prospective, single blind, randomized, controlled trial. Gastrointest Endosc. 2012;76:328–335.
Puri RR, Vilmann PP, Săftoiu AA, et al. Randomized controlled trial of endoscopic ultrasound-guided fine-needle sampling with or without suction for better cytological diagnosis. Scand J Gastroenterol. 2009;44:499–504.
Lee JK, Choi JH, Lee KH, et al. A prospective, comparative trial to optimize sampling techniques in EUS-guided FNA of solid pancreatic masses. Gastrointest Endosc. 2013 Feb 21.
Savides TJ. Tricks for improving EUS-FNA accuracy and maximizing cellular yield. Gastrointest Endosc. 2009;69:S130–S133.
Mitsuhashi T, Ghafari S, Chang CY, Gu M. Endoscopic ultrasound-guided fine needle aspiration of the pancreas: cytomorphological evaluation with emphasis on adequacy assessment, diagnostic criteria and contamination from the gastrointestinal tract. Cytopathology. 2006;17:34–41.
Fujii LL, Levy MJ. Pitfalls in EUS FNA. Gastrointest Endosc Clin N Am. 2014;24:125–142.
Gleeson FC, Kipp BR, Caudill JL, et al. False positive endoscopic ultrasound fine needle aspiration cytology: incidence and risk factors. Gut. 2010;59:586–593.
Eloubeidi MA, Jhala D, Chhieng DC, et al. Yield of endoscopic ultrasound-guided fine-needle aspiration biopsy in patients with suspected pancreatic carcinoma. Cancer. 2003;99:285–292.
Kliment M, Urban O, Cegan M, et al. Endoscopic ultrasound-guided fine needle aspiration of pancreatic masses: the utility and impact on management of patients. Scand J Gastroenterol. 2010;45:1372–1379.
Woolf KMW, Liang H, Sletten ZJ, Russell DK, Bonfiglio TA, Zhou Z. False-negative rate of endoscopic ultrasound-guided fine-needle aspiration for pancreatic solid and cystic lesions with matched surgical resections as the gold standard: one institution’s experience. Cancer Cytopathol. 2013;121:449–458.
Wallace MB, Kennedy T, Durkalski V, et al. Randomized controlled trial of EUS-guided fine needle aspiration techniques for the detection of malignant lymphadenopathy. Gastrointest Endosc. 2001;54:441–447.
Storch IM, Sussman DA, Jorda M, Ribeiro A. Evaluation of fine needle aspiration vs. fine needle capillary sampling on specimen quality and diagnostic accuracy in endoscopic ultrasound-guided biopsy. Acta Cytol. 2007;51:837–842.
Bang JY, Ramesh J, Trevino J, Eloubeidi MA, Varadarajulu S. Objective assessment of an algorithmic approach to EUS-guided FNA and interventions. Gastrointest Endosc. 2013;77:739–744.
Nakai Y, Isayama H, Chang KJ, et al. Slow pull versus suction in endoscopic ultrasound-guided fine-needle aspiration of pancreatic solid masses. Dig Dis Sci. 2014;59:1578–1585.
Polkowski M, Larghi A, Weynand B, et al. Learning, techniques, and complications of endoscopic ultrasound (EUS)-guided sampling in gastroenterology: European Society of Gastrointestinal Endoscopy (ESGE) Technical Guideline. Endoscopy. 2012;44:190–206.
Wani S, Muthusamy VR, Komanduri S. EUS-guided tissue acquisition: an evidence-based approach (with videos). Gastrointest Endosc. 2014;80:939–959.e7.
Rastogi A, Wani S, Gupta N, et al. A prospective, single-blind, randomized, controlled trial of EUS-guided FNA with and without a stylet. Gastrointest Endosc. 2011;74:58–64.
Kudo T, Kawakami H, Hayashi T, et al. High and low negative pressure suction techniques in EUS-guided fine-needle tissue acquisition by using 25-gauge needles: a multicenter, prospective, randomized, controlled trial. Gastrointest Endosc. 2014;80:1030–1031.
Iglesias-Garcia J, Dominguez-Munoz JE, Abdulkader I, et al. Influence of on-site cytopathology evaluation on the diagnostic accuracy of endoscopic ultrasound-guided fine needle aspiration (EUS-FNA) of solid pancreatic masses. Am J Gastroenterol. 2011;106:1705–1710.
Hayashi T, Ishiwatari H, Yoshida M, et al. Rapid on-site evaluation by endosonographer during endoscopic ultrasound-guided fine needle aspiration for pancreatic solid masses. J Gastroenterol Hepatol. 2013;28:656–663.
Wani S, Mullady D, Early DS, Rastogi A, Collins B. Clinical impact of immediate on-site cytopathology (CyP) evaluation during endoscopic ultrasound-guided fine needle aspiration (EUS-FNA) of pancreatic mass: Interim analysis of a multicenter randomized con- trolled trial. Gastrointest Endosc. 2013;77:2. (Abstract supplement).
Acknowledgments
This publication was supported by the National Center for Advancing Translational Sciences, National Institutes of Health, through Grant Number 8UL1TR000055. Its contents are solely the responsibility of the authors and do not necessarily represent the official views of the NIH.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflict of interest
The authors declare that they have no conflict of interest.
Electronic supplementary material
Below is the link to the electronic supplementary material.
Supplementary material 1 (WMV 49176 kb)
Supplementary material 2 (WMV 26989 kb)
Rights and permissions
About this article
Cite this article
Aadam, A.A., Oh, Y.S., Shidham, V.B. et al. Eliminating the Residual Negative Pressure in the Endoscopic Ultrasound Aspirating Needle Enhances Cytology Yield of Pancreas Masses. Dig Dis Sci 61, 890–899 (2016). https://doi.org/10.1007/s10620-015-3860-0
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s10620-015-3860-0