Abstract
Background
Hospital readmissions have received increased scrutiny as a marker for excessive resource utilization and also quality care.
Aim
To identify the rate of and risk factors for hospital readmission after major surgery at academic medical centers.
Methods
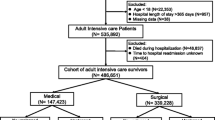
Using the University Health Consortium Clinical Database, 30-day readmission rates in all adult patients undergoing colectomy (n = 103,129), lung resection (n = 73,558), gastric bypass (n = 62,010) or abdominal aortic surgery (n = 17,997) from 2009 to 2012 were identified. Logistic regression was performed to examine risks for readmission.
Results
Overall readmission rates ranged from 8.9 % after gastric bypass to 15.8 % after colectomy. Black race was associated with increased likelihood for readmission after three of the four procedures with odds ratios ranging from 1.13 after colectomy to 1.44 after gastric bypass. For all procedures, moderate, severe, or extreme severity of illness (SOI) and need for transitional care were associated with increased odds for hospital readmission. Lower center volume was an independent predictor of readmission after gastric bypass surgery and aortic surgery.
Conclusion
Readmission rates after major elective surgery are high across national academic centers. Center volume, SOI, and need for transitional care after discharge are factors associated with readmission and may be used to identify patients at high risk of readmission and hospital utilization after major surgery.
Similar content being viewed by others
References
Readmissions Reduction Program. 2012. http://www.cms.gov/Medicare/Medicare-Fee-for-Service-Payment/AcuteInpatientPPS/Readmissions-Reduction-Program.html.
Gorodeski EZ, Starling RC, Blackstone EH. Are all readmissions bad readmissions? N Engl J Med. 2010;363:297–298.
Ahmad SA, Edwards MJ, Sutton JM, et al. Factors influencing readmission after pancreaticoduodenectomy: a multi-institutional study of 1302 patients. Ann Surg. 2012;256:529–537.
Kassin MT, Owen RM, Perez SD, et al. Risk factors for 30-day hospital readmission among general surgery patients. J Am Coll Surg. 2012;215:322–330.
About UHC. 2013. http://www.uhc.edu/12443.htm.
Sutton JM, Hayes AJ, Wilson GC, et al. Validation of the University HealthSystem Consortium administrative dataset: concordance and discordance with patient-level institutional data. J Surg Res. 2014;190:484–490. doi:10.1016/j.jss.2014.03.044.
M APR DRG Software—Account for severity and risk among all patients. 2013. http://solutions.3m.com/wps/portal/3M/en_US/Health-Information-Systems/HIS/Products-and-Services/Products-List-A-Z/APR-DRG-Software/.
Birkmeyer JD, Siewers AE, Finlayson EV, et al. Hospital volume and surgical mortality in the United States. N Engl J Med. 2002;346:1128–1137.
Singla A, Simons J, Li Y, et al. Admission volume determines outcome for patients with acute pancreatitis. Gastroenterology. 2009;137:1995–2001.
Macomber CW, Shaw JJ, Santry H, et al. Centre volume and resource consumption in liver transplantation. HPB (Oxf). 2012;14:554–559.
Lucas DJ, Haider A, Haut E, et al. Assessing readmission after general, vascular, and thoracic surgery using ACS-NSQIP. Ann Surg. 2013;258:430–439.
Martin RC, Brown R, Puffer L, et al. Readmission rates after abdominal surgery: the role of surgeon, primary caregiver, home health, and subacute rehab. Ann Surg. 2011;254:591–597.
Mudge AM, Kasper K, Clair A, et al. Recurrent readmissions in medical patients: a prospective study. J Hosp Med. 2011;6:61–67.
Jencks SF, Williams MV, Coleman EA. Rehospitalizations among patients in the Medicare fee-for-service program. N Engl J Med. 2009;360:1418–1428.
Goodney PP, Stukel TA, Lucas FL, Finlayson EV, Birkmeyer JD. Hospital volume, length of stay, and readmission rates in high-risk surgery. Ann Surg. 2003;238:161–167.
Hong B, Stanley E, Reinhardt S, Panther K, Garren MJ, Gould JC. Factors associated with readmission after laparoscopic gastric bypass surgery. Surg Obes Relat Dis. 2012;8:691–695.
Tsai TC, Joynt KE, Orav EJ, Gawande AA, Jha AK. Variation in surgical-readmission rates and quality of hospital care. N Engl J Med. 2013;369:1134–1142.
Li LT, Barden GM, Balentine CJ, et al. Postoperative transitional care needs in the elderly: an outcome of recovery associated with worse long-term survival. Ann Surg. 2014. doi:10.1097/SLA.0000000000000673.
Arbaje AI, Wolff JL, Yu Q, Powe NR, Anderson GF, Boult C. Postdischarge environmental and socioeconomic factors and the likelihood of early hospital readmission among community-dwelling Medicare beneficiaries. Gerontologist. 2008;48:495–504.
Kind AJ, Smith MA, Frytak JR, Finch MD. Bouncing back: patterns and predictors of complicated transitions 30 days after hospitalization for acute ischemic stroke. J Am Geriatr Soc. 2007;55:365–373.
van Walraven C, Bennett C, Jennings A, Austin PC, Forster AJ. Proportion of hospital readmissions deemed avoidable: a systematic review. CMAJ. 2011;183:E391–E402.
Lucas FL, Stukel TA, Morris AM, Siewers AE, Birkmeyer JD. Race and surgical mortality in the United States. Ann Surg. 2006;243:281–286.
Conflict of interest
None.
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
About this article
Cite this article
Wilson, G.C., Cutler Quillin, R., Sutton, J.M. et al. Factors Related to Readmission After Major Elective Surgery. Dig Dis Sci 60, 47–53 (2015). https://doi.org/10.1007/s10620-014-3306-0
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s10620-014-3306-0