Abstract
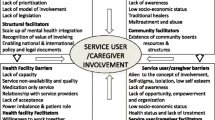
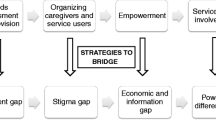
The diverse needs associated with mental illness warrant for the provision of mental health care by various sources. The South African government recognises the involvement of stakeholders as a potential means of narrowing the gaps in mental health service delivery. This study explored the views of different stakeholders about their roles as support systems for people with mental illness and their families at Mashashane, a rural setting in Limpopo Province, South Africa. Seven focus group discussions were conducted with various stakeholders. This qualitative study employed content analysis to allow for comparison of stakeholders’ views. Stakeholders understanding of mental illness was based on reaction towards people with mental illness, causes of mental illness and the behaviour displayed by the ill individual. The identified formal and informal systems were seen as ineffective with regards to provision of support. Collaboration was recommended as a mechanism to improve mental health services. The findings contributed in the formulation of guidelines to improve support.
Similar content being viewed by others
References
Ama, N. O., & Seloilwe, E. S. (2010). Estimating the cost of care giving on caregivers for people living with HIV and AIDS in Botswana: A cross-sectional study. Journal of the International AIDS Society, 13(14), 1–8.
Ama, N. O., & Seloilwe, E. S. (2011). Analysis of the burdens of caregivers providing care to people living with HIV/AIDS in Botswana. South African Family Practice, 53(1), 56–62.
Angermeyer, M. C., & Dietrich, S. (2006). Public beliefs about and attitudes towards people with mental illness: A review of population studies. Acta Psychiatrica Scandinavica, 113, 163–179.
Babbie, E., & Mouton, J. (2012). The practice of social research. Cape Town: Oxford University Press.
Byaruhanga, E., Cantor-Graae, E., Maling, S., & Kabakyenga, J. (2008). Pioneering work in mental health outreaches in rural, south-western Uganda. Journal of Mental Health and Psychosocial Support in Conflict Affected Areas, 6(2), 117–131.
Campbell-Hall, V., Petersen, I., Bhana, A., Mjadu, S., Hosegood, V., Flisher, A. J., et al. (2010). Collaboration between traditional practitioners and primary health care staff in South Africa: Developing a workable partnership for community mental health services. Transcultural Psychiatry, 47(4), 610–628.
Crawford, T. A., & Lipsedge, M. (2004). Seeking help for psychological distress: The interface of Zulu traditional healing and Western biomedicine. Mental Health, Religion & Culture, 7(2), 131–148.
Creswell, J. W., & Clark, V. L. P. (2007). Designing and conducting mixed method research. Thousand Oaks, CA: Sage Publications, Inc.
Danaher, A. (2011). Reducing health inequities: Enablers and barriers to inter-sectoral collaboration. Toronto: Wellesley Institute.
Dogar, I. M. (2007). Biopsychosocial model. Annals of Punjab Medical College, 1(1), 11–14.
Faull, E. (2012). Christian religion and wellbeing. Ekklesiastikos Pharos, 94, 169–187.
Friedman, I. (2005). Community health workers (CHWs). In P. Ijumba & P. Barron (Eds.), South African health review (pp. 176–189). Durban: Health Systems Trust
Ganasen, K. A., Parker, S., Hugo, C. J., Stein, D. J., Emsley, R. A., & Seedat, S. (2008). Mental health literacy: Focus on developing countries. African Journal of Psychiatry, 11, 23–28.
Greenwood, N., Ellmers, T., & Holley, J. (2014). The influence of ethnic group composition on focus group discussions. Medical Research Methodology, 14, 107–119.
Grifitths, J., Maggs, H., & George, E. (2008). Stakeholder involvement. Geneva: World Health Organization.
Knoetze, E. (2014). Legislative regulation of the developmental functions of traditional leadership—in conflict or cohesion with Municipal Councils? Speculum Juris, 1, 161–195.
Livingston, J. D., Desmarais, S. L., Greaves, C., Parent, R., Verdun-Jones, S., & Brink, J. (2014). What influences perceptions of procedural justice among people with mental illness regarding their interactions with the police? Community Mental Health Journal, 50, 281–287.
Magadla, N. I. N., & Kolwapi, X. X. (2013). Knowledge and skills police officers need to manage mental health care users. African Journal for Physical, Health Education, Recreation and Dance Supplement, 1, 167–176.
Magezi, V. (2010). From periphery to the centre: Towards repositioning churches for a meaningful contribution to public health care. HTS. Teologiese Studies/Theological Studies, 68(2), 1–8.
Mahilall, R. (2009). Motivations and expectations of a locally specific group of volunteer home based carers serving people with HIV/AIDS in the Mariannhill region. Published Master’s Thesis. University of South Africa (Online).
Mamba, S. T., & Ntuli, B. E. (2014). Activities and challenges in caring for chronically ill patients: Experiences of home-based carers in Soweto, South Africa. African Journal for Physical, Health Education, Recreation and Dance, 1(2), 409–419.
Mavundla, T. R., Toth, F., & Mphelane, M. L. (2009). Caregiver experience in mental illness: A perspective from a rural community in South Africa. International Journal of Mental Health Nursing, 18, 357–367.
Mokgobi, M. G. (2014). Western-trained health care practitioners’ knowledge of and experiences with traditional healing. African Journal for Physical, Health Education, Recreation and Dance Supplement, 2, 1–13.
Munikwa, J., Mutopa, S., & Maphosa, C. (2012). The nature and causes of para-suicide cases handled by traditional leaders in Hurungwe District in Zimbabwe. Journal of Human Ecology, 37(2), 93–102.
Ndetei, D. M., Khasakhala, L. I., Kingori, J., Going, A., & Raja, S. (2008). The complementary role of traditional and faith healers and potential liaisons with Western-style mental health services in Kenya. Retrieved from http://www.utsouthwestern.edu/psychiatryandfreedom.
Ndetei, D. M., Mbwayo, A. W., Mutiso, V. N., Khasakhala, L. I., & Chege, P. M. (2013). Traditional healers and their provision of mental health services in Cosmopolitan Informal Settlements in Nairobi. Kenya African Technology Policy Studies ATPS, Working paper 67.
Nsereko, J. R., Kizza, D., Kigozi, F., Ssebunya, J., Ndyanabangi, S., Flisher, A. J., et al. (2011). Stakeholder’s perceptions of help-seeking behaviour among people with mental health problems in Uganda. International Journal of Mental Health Systems, 5(5), 1–9.
Petersen, I., & Lund, C. (2011). Mental health service delivery in South Africa from 2000 to 2010: One step forward, one step backward. South African Medical Journal, 101(10), 751–757.
Pierce, R. (2009). Research methods in politics. Thousand Oaks: Sage Publications Inc.
Ross, E. (2010). Inaugural lecture: African spirituality, ethics and traditional healing—Implications for indigenous South African social work education and practice. South African Journal of Bioethics and Law, 3(1), 44–51.
Schmidt, L., & Monaghan, J. (2012). Intensive family support services: A consultative model of education and support. American Journal of Psychiatric Rehabilitation, 15, 26–43.
Skeen, S., Kleintjies, S., Lund, C., Petersen, I., Bhana, A., Flisher, A. J., et al. (2010). Mental Health is everybody’s businesses: Roles for an inter-sectoral approach in South Africa. Health Policy and Planning, 22(6), 611–623.
Sorsdahl, K., Stein, D. J., Grimsrud, A., Seedat, S., Flisher, A. J., Williams, D. R., et al. (2009). Traditional healers in the treatment of common mental disorders in South Africa. The Journal of Nervous and Mental Disease, 197(6)), 434–441.
Sorsdahl, K. R., Flisher, A. J., Wilson, Z., & Stein, D. J. (2010). Explanatory models of mental disorders and treatment practices among traditional healers in Mpumalanga, South Africa. African Journal of Psychiatry, 13, 284–290.
Taljaard, L. (2012). Clarifying the role of the SAPS in mental healthcare. African Journal of Psychiatry, 374–376.
Watson, A. C., Morabito, M. S., Draine, J., & Ottati, V. (2008). Improving police response to persons with mental illness: A multi-level conceptualization CIT. International Journal of Law and Psychiatry, 31, 359–368.
World Health Organization. (2013). Mental health action plan 2013–2020. Geneva: World Health Organization.
Yin, R. Y. (2003). Case study research: Design and methods (3rd ed.). Thousand Oaks: Sage Publications.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflict of interest
Authors declare that there are no known conflicts of interest.
Ethical Approval
The study was approved by the Ethics Committee of the North-West University, Potchefstroom with reference number NWU-00125-11-A1.
Informed Consent
Informed consent was obtained from all individual participants. Participants were reimbursed for transportation.
Rights and permissions
About this article
Cite this article
Matsea, T., Ryke, E. & Weyers, M. Stakeholders’ Views Regarding Their Role as Support System for People with Mental Illness and Their Families in Rural South Africa. Community Ment Health J 55, 672–679 (2019). https://doi.org/10.1007/s10597-018-0337-6
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s10597-018-0337-6